December 18, 2025
Defined contribution savings plans and 403(b) annuity plan sponsors, fiduciaries and vendors should use the “2025 Required Amendments List for Qualified and Section 403(b) Plans” to verify their programs are timely updated with all required amendments to avoid tax disqualification exposures.
Notice 2025-60 contains the Internal Revenue Service (“IRS”) 2025 Required Amendments List (“2025 RA List”) for individually designed plans qualified under section 401(a) of the Internal Revenue Code and individually designed plans that satisfy the requirements of section 403(b). The 2025 RA List also applies to pre-approved plans with respect to interim amendments.
Notice 2025-60 will be in IRB: 2025-52, dated: December 22, 2025.
If you have questions or need additional ion information or assistance, contact the author of this update, Cynthia Marcotte Stamer,
About the Author
Cynthia Marcotte Stamer is a Martindale-Hubble AV-Preeminent (highest/top 1%) practicing attorney recognized as a “Top Woman Lawyer,” “Top Rated Lawyer,” and “LEGAL LEADER™” in Health Care Law and Labor and Employment Law; among the “Best Lawyers In Dallas” in “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law recognized for her experience, scholarship, thought leadership and advocacy on health and other employee benefits, insurance, healthcare, workforce, HIPAA and other data and technology and other compliance in connection with her work with health care and life sciences, employee benefits, insurance, education, technology and other highly regulated and performance-dependent clients.
Board certified in labor and employment law by the Texas Board of Legal Specialization and a Fellow in the American College of Employee Benefits Counsel, Ms. Stamer is nationally recognized for her decades of leading edge experience on the design, sponsorship, administration and defense of health and other employee benefit, workforce, insurance, healthcare , data and technology and other operations to promote legal and operational compliance, reduce regulatory and other liability and promote other operational goals.
Along with her decades of legal and strategic consulting experience, Ms. Stamer also contributes her leadership and experience to many professional, civic and community organizations. She currently serves as Co-Chair of the ABA Real Property Trusts and Estates (“RPTE”) Section Welfare Plan Committee, Co-Chair of the ABA International Section International Employment Law Committee and its Annual Meeting Program Planning Committee, Chair Emeritus and Vice Chair of the ABA Tort Trial and Insurance (“TIPS”) Section Medicine and Law Committee, and Chair of the ABA Intellectual Property Section Law Practice Management Committee. She also has served as Scribe for the Joint Committee on Employee Benefits (“JCEB”) annual agency meetings with the Department of Health and Human Services and JCEB Council Representative, International Section Life Sciences Committee Chair, RPTE Section Employee Benefits Group Chair and a Substantive Groups Committee Member, Health Law Section Managed Care & Insurance Interest Group Chair, as TIPS Section Medicine and Law Committee Chair and Employee Benefits Committee and Workers Compensation Committee Vice Chair, Tax Section Fringe Benefit Committee Chair, and in various other ABA leadership capacities. Ms. Stamer also is a former Southwest Benefits Association Board Member and Continuing Education Chair, SHRM National Consultant Board Chair and Region IV Chair, Dallas Bar Association Employee Benefits Committee Chair, former Texas Association of Business State, Regional and Dallas Chapter Chair, a founding board member and Past President of the Alliance for Healthcare Excellence, as well as in the leadership of many other professional, civic and community organizations. She also is recognized for her contributions to strengthening health care policy and charitable and community service resolving health care challenges performed under PROJECT COPE Coalition For Patient Empowerment initiative and many other pro bono service involvements locally, nationally and internationally.
Ms. Stamer is the author of many highly regarded works published by leading professional and business publishers, the ABA, the American Health Lawyers Association, and others. Ms. Stamer also frequently speaks and serves on the faculty and steering committee for many ABA and other professional and industry conferences and conducts leadership and industry training for a wide range of organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see http://www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press™
Solutions Law Press™ provides health care, insurance, human resources and employee benefit, data and technology, regulatory and operational performance, and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education. These include extensive resources on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press™ resources or training.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by emailing it here.
NOTICE: These statements and materials are for general information and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation considering the specific facts and circumstances presented in their unique circumstances at the particular time. No comment or statement in this publication is to be construed as legal advice or admission. Solutions Law Press and its authors reserve the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law constantly and often evolves, subsequent developments that could impact the currency and completeness of this discussion are likely. Solutions Law Press and its authors disclaim and have no responsibility to provide any update or otherwise notify anyone of any fact or law-specific nuance, change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2025 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press.™ For information about licensing for republication, please contact the author directly. All other rights reserved.
 Comments Off on Confirm 2025 Required Defined Contribution & 403(b) Plan Amendments Timely Adopted |
Comments Off on Confirm 2025 Required Defined Contribution & 403(b) Plan Amendments Timely Adopted |  401(k), Corporate Compliance, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employers, enforcement, ERISA, Internal Revenue Code, Retirement Plans, Retirements |
401(k), Corporate Compliance, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employers, enforcement, ERISA, Internal Revenue Code, Retirement Plans, Retirements |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
February 24, 2023
The U.S. Department of Labor Employee Benefits Security Administration, the Internal Revenue Service (“IRS”) and the Pension Benefit Guaranty Corporation (“PBGC”) announcing changes to the 2023 Form 5500 Annual Return/Report of Employee Benefit Plan and Form 5500-SF Short Form in February 23.
The “Phase III” announcement released this week are set forth in the following:
The Phase III announcement implements the third and final phase of implementation of a September, 2021 regulatory proposal, which included changes related to provisions in the Setting Every Community Up for Retirement Enforcement Act, commonly known as the SECURE Act, which affected annual reporting requirements under the Employee Retirement Income Security Act and the Internal Revenue Code.
The first two phases of implementation included publication of Federal Register notices in December 2021 for Phase I and May 2022 for Phase II, respectively, to adopt changes for the 2021 and 2022 Form 5500 Returns/Reports.
The Phase III announcement features a Notice of Final Forms Revisions from the EBSA, IRS and PBGC for the 2023 plan year forms and instructions and a Notice of Final Rulemaking by the department that makes corresponding changes to annual reporting regulations under Title I of ERISA.
The 2023 plan year reports – which generally will be filed beginning in July 2024 for calendar year plans – include the following changes:
- A consolidated Form 5500 reporting option for certain groups of defined contribution retirement plans, improved reporting by pooled employer plans and other multiple employer plans.
- A change in the participant-counting methodology for determining eligibility for simplified reporting alternatives available to “small plans,” which are generally plans with fewer than 100 participants.
- A breakout of reporting on administrative expenses paid by the plan on the plan’s financial statements.
- Further improvements in financial and funding reporting by PBGC-covered defined benefit plans.
- The addition of selected Internal Revenue Code compliance questions to improve tax oversight and compliance of tax-qualified retirement plans.
- Technical and conforming changes as part of the annual rollover of forms and instructions.
Additionally, technical adjustments were made to the Federal Register notices to address certain provisions in SECURE Act 2.0 of 2022 on Code section 403(b) multiple employer plans, including pooled employer plans, minimum required distributions and audit requirements for plans in defined contribution group reporting arrangements.
The Federal Register notices, Document #2023-02653 for the Notice of Final Forms Revision and Document #2023-02652 for Notice of Final Rulemaking, also include appendices that describe the changes to the forms and instructions as well as a regulatory impact and paperwork burden analyses. A more detailed summary of the annual reporting changes is included in a fact sheet posted on the department’s website today. Mock-ups of the forms and instructions will be available at reginfo.gov as part of the Paperwork Reduction Act clearance process. The release of “for information-only” copies of the forms and instructions will happen later in 2023.
More Information
When investigating and responding to a violation, it is critically important to document the timing and details of the discovery of a potentially concern
We hope this update is helpful. For more information about the these or other health or other legal, management or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
Solutions Law Press, Inc. invites you receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 35+ years of workforce and other management work, public policy leadership and advocacy, coaching, teachings, scholarship and thought leadership.
A Fellow in the American College of Employee Benefit Counsel, Vice Chair of the American Bar Association (“ABA”) International Section Life Sciences and Health Committee, Past Chair of the ABA Managed Care & Insurance Interest Group, Scribe for the ABA JCEB Annual Agency Meeting with HHS-OCR, past chair of the ABA RPTE Employee Benefits & Other Compensation Group and current co-Chair of its Welfare Benefit Committee, Ms. Stamer’s work throughout her 35 year career has focused heavily on working with health care and managed care, health and other employee benefit plan, insurance and financial services and other public and private organizations and their technology, data, and other service providers and advisors domestically and internationally with legal and operational compliance and risk management, performance and workforce management, regulatory and public policy and other legal and operational concerns. As an ongoing component of this work, she regularly advises, represents and defends businesses on Guideline Program and other compliance, risk management and other internal and external controls in a wide range of areas and has published and spoken extensively on these concerns.
Ms. Stamer also is widely recognized for her decades of pragmatic, leading edge work, scholarship and thought leadership on workforce, compensation, and other operations, risk management, compliance and regulatory and public affairs concerns.
For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources available here.
IMPORTANT NOTICE ABOUT THIS COMMUNICATION
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advice or an admission. The author and Solutions Law Press, Inc.™ reserve the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving, and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The author and Solutions Law Press, Inc.™ disclaim, and have no responsibility to provide any update or otherwise notify anyone any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication. Readers acknowledge and agree to the conditions of this Notice as a condition of their access of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2023 Cynthia Marcotte Stamer. Limited non-exclusive right to republish granted to Solutions Law Press, Inc.™
 Comments Off on Updated Form 5500s and Instructions Released |
Comments Off on Updated Form 5500s and Instructions Released |  compliance, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, EBSA, Emploeyrs, employee, Employee Benefits, Employer, Employers, ERISA, ESOP, Form 5500, health plan, Health Plans, multiple employer plan (Meps), Retirement Plans, Retirements, third party administrators |
compliance, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, EBSA, Emploeyrs, employee, Employee Benefits, Employer, Employers, ERISA, ESOP, Form 5500, health plan, Health Plans, multiple employer plan (Meps), Retirement Plans, Retirements, third party administrators |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
June 26, 2020
Earlier this week, the Internal Revenue Service (“IRS”) announced that employee benefit plan participants that already took a required minimum distribution (RMD) in 2020 from certain retirement accounts now has the opportunity through August 31, 2020 to roll those funds back into a retirement account following the Coronavirus Aid, Relief, and Economic Security (CARES) Act RMD waiver for 2020. The announcement of this relief covers one of a long and growing list of special tax and other COVID-19 responsive special rules and requirements that may change requirements, provide special relief or both for businesses and individuals that every business leader and individual should carefully monitor and respond to appropriately.
Retirement Plan Rollover Relief
On July 23, 2020, the IRS announced its extension of the 60-day rollover period for any RMDs already taken this year to August 31, 2020 to give taxpayers time to take advantage of this opportunity in Notice 2020-51 (PDF). The Notice also answers questions regarding the waiver of RMDs for 2020 under the Coronavirus Aid, Relief, and Economic Security Act, known as the CARES Act.
The CARES Act enabled any taxpayer with an RMD due in 2020 from a defined-contribution retirement plan, including a 401(k) or 403(b) plan, or an IRA, to skip those RMDs this year. This includes anyone who turned age 70 1/2 in 2019 and would have had to take the first RMD by April 1, 2020. This waiver does not apply to defined-benefit plans.
In addition to the rollover opportunity, an IRA owner or beneficiary who has already received a distribution from an IRA of an amount that would have been an RMD in 2020 can repay the distribution to the IRA by August 31, 2020. The notice provides that this repayment is not subject to the one rollover per 12-month period limitation and the restriction on rollovers for inherited IRAs.
The notice provides two sample amendments that employers may adopt to give plan participants and beneficiaries whose RMDs are waived a choice as to whether or not to receive the waived RMD.
Other COVID-19 Tax Rules & Relief
The guidance and relief in Notice 2020-51 highlights only one of a long list of special COVID-19 associated tax rules and relief that could apply to a business, its employees or employee benefit plan participants or both including the following:
- IR-2020-127, IRS announces rollover relief for required minimum distributions from retirement accounts that were waived under the CARES Act
- IR-2020-126, IRS extends July 15, other upcoming deadlines for tornado victims in parts of the South; provides other relief
- IR-2020-124, Relief for taxpayers affected by COVID-19 who take distributions or loans from retirement plans
- IR-2020-122, IRS outlines changes to health care spending available under CARES Act
- IR-2020-121, IRS alert: Economic Impact Payments belong to recipient, not nursing homes or care facilities
- IR-2020-120, Treasury, IRS provide tax relief to investors and businesses affected by COVID-19 in new markets tax credit transactions
- IR-2020-119, IRS provides guidance on employer leave-based donation programs that aid victims of the COVID-19 pandemic
- IR-2020-118, IRS reminder: File now, choose direct deposit or schedule tax payments electronically before the July 15 deadline
- IR-2020-117, IRS reminder: Deadline postponed to July 15 for those who pay estimated taxes
- IR-2020-115, IRS warns against COVID-19 fraud; other financial schemes
- IR-2020-114, IRS provides answers about Coronavirus related tax relief for Qualified Opportunity Funds and investors
- IR-2020-111, 159 million Economic Impact Payments processed; Low-income people and others who aren’t required to file tax returns can quickly register for payment with IRS Non-Filers tool
- IR-2020-110, IRS provides relief to retirement plan participants to sign elections remotely
- IR-2020-109, IRS reminder: June 15 tax deadline postponed to July 15 for taxpayers who live and work abroad
- IR-2020-106, Treasury, IRS provide safe harbor for taxpayers that develop renewable energy projects
- IR-2020-105, Economic Impact Payments being sent by prepaid debit cards, arrive in plain envelope; IRS.gov answers frequently asked questions
- IR-2020-101, Treasury, IRS release latest state-by-state Economic Impact Payment figures for May 22, 2020
- IR-2020-99, IRS.gov helps taxpayers get tax information they need; find tools for filing, paying, checking accounts and answering questions
- Treasury News Release: Treasury is Delivering Millions of Economic Impact Payments by Prepaid Debit Card
- IR-2020-97, IRS adds phone operators to answer Economic Impact Payment questions
- IR-2020-96, IRS expands partner materials for Economic Impact Payments; continues sweeping effort to share details in multiple languages
- IR-2020-95, IRS provides tax relief through increased flexibility for taxpayers in section 125 cafeteria plans
- IR-2020-93, Why the Economic Impact Payment amount could be different than anticipated
- IR-2020-92, Act by Wednesday for chance to get quicker Economic Impact Payment; timeline for payments continues to accelerate
- IR-2020-91, Treasury, IRS release latest state-by-state Economic Impact Payment figures
- IR-2020-89, IRS: Three new credits are available to many businesses hit by COVID-19
- IR-2020-87, IRS retools Settlement Days program in response to COVID-19 pandemic; allows unrepresented taxpayers to settle their cases virtually and reach finality
- IR-2020-86, VA, SSI recipients with eligible children need to act by Tuesday, May 5 to quickly add money to their automatic Economic Impact Payment; ‘Plus $500 Push’ continues
- IR-2020-85, Economic Impact Payments continue to be sent, check IRS.gov for answers to common questions
- IR-2020-83, Use IRS Non-Filers: Enter Payment Info Here tool to get Economic Impact Payment; many low-income, homeless qualify
- IR-2020-82, IRS enhances Get My Payment online application to help taxpayers
- IR-2020-81, VA, SSI recipients with eligible children need to act by May 5 to quickly add money to their automatic Economic Impact Payment; ‘Plus $500 Push’ continues
- IR-2020-80, Treasury, IRS deliver 89.5 million Economic Impact Payments in first three weeks, release state-by-state Economic Impact Payment figures (Updated: April 28, 2020)
- IR-2020-77, Treasury, IRS announce cross-border tax guidance related to travel disruptions arising from the COVID-19 emergency
- IR-2020-76, SSA, RRB recipients with eligible children need to act by Wednesday to quickly add money to their automatic Economic Impact Payment; IRS asks for help in the “Plus $500 Push”
- IR-2020-75, Veterans Affairs recipients will receive automatic Economic Impact Payments; Step follows work between Treasury, IRS, VA
- IR-2020-74, IRS: Free File use soars; taxpayers still have time to do their taxes for free
- IR-2020-73, Supplemental Security Income recipients will receive automatic Economic Impact Payments; step follows work between Treasury, IRS, Social Security Administration
- IR-2020-72, Treasury, IRS unveil online application to help with Economic Impact Payments
- IR-2020-71, IRS, Security Summit partners warn tax professionals on scams, urge additional security measures to protect taxpayer data
- IR-2020-70, REMINDER: Schedule and pay federal taxes electronically due by July 15; only a few hours remaining for taxpayers to reschedule payments set for April 15
- IR-2020-69, Treasury, IRS launch new tool to help non-filers register for Economic Impact Payments
- IR-2020-68, IRS urges taxpayers to use electronic options; outlines online assistance
- IR-2020-67, IRS provides guidance under the CARES Act to taxpayers with net operating losses
- IR-2020-66, To help taxpayers, the Department of Treasury and the Internal Revenue Service announced today that Notice 2020-23 extends additional key tax deadlines for individuals and businesses
- IR-2020-65, Follow IRS on social media, sign up for e-news subscriptions for urgent updates on COVID-19, scams and economic impact payment information
- IR-2020-64, IRS issues warning about coronavirus-related scams; watch out for schemes tied to economic impact payments
- Treasury News Release: Social Security recipients will automatically receive Economic Impact Payments
- IR 2020-62, IRS: Employee Retention Credit available for many businesses financially impacted by COVID-19
- IR 2020-61, Economic impact payments: What you need to know
- IR-2020-59, IRS unveils new People First Initiative; COVID-19 effort temporarily adjusts, suspends key compliance program
- IR-2020-58, Tax Day now July 15: Treasury, IRS extend filing deadline and federal tax payments regardless of amount
- IR-2020-57, Treasury, IRS and Labor announce plan to implement coronavirus-related paid leave for workers and tax credits for small and midsize businesses to swiftly recover the cost of providing Coronavirus-related leave
- Treasury News Release: Treasury and IRS issue guidance on deferring tax payments due to COVID-19 outbreak
- IR-2020-54, IRS: High-deductible health plans can cover coronavirus costs
Along with these tax rules, businesses and their employees also may be impacted by a broad range of special federal and state labor and employment and other rules adopted in response to the continuing COVID-19 health care emergency and its fallout. Businesses and their leaders should carefully review and monitor these and other COVID-19 specific rules to ensure that their businesses don’t trigger unanticipated liability by failing to meet critical requirements or to ensure that they take full advantage of all available relief.
More Information
We hope this update is helpful. For more information about the these or other health or other legal, management or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
Solutions Law Press, Inc. invites you receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years legal and operational management work, coaching, public policy and regulatory affairs leadership and advocacy, training and public speaking and publications. As a significant part of her work, Ms. Stamer has worked extensively domestically and internationally on an demand, special project and ongoing basis with health industry, health plan and insurance and other businesses of all types, government and community organizations and their leaders, spoken and published extensively on workforce and other services, compensation and benefits, and related tax; insurance; workers’ compensation and occupational disease; business reengineering, disaster and distress; and many other management concerns.
Board Certified in Labor and Employment Law By the Texas Board of Legal Specialization, Scribe for the ABA JCEB Annual Agency Meeting with OCR, Vice Chair of the ABA International Section Life Sciences Committee, and the ABA RPTE Employee Benefits & Other Compensation Group and a former Council Representative, Past Chair of the ABA Managed Care & Insurance Interest Group, former Vice President and Executive Director of the North Texas Health Care Compliance Professionals Association, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer has extensive experience advising, representing, defending and training health care providers, health plans and insurers, employers, community organizations and others about HIPAA and other privacy concerns and has published and spoken extensively on these concerns.
Her involvement with HIPAA and other privacy and data concerns has taken place as part of her more than 30 years involvement working with with public and private health industry, health insurance and other employers and organizations of all sizes, employee benefit plans, insurance and financial services, health industry and a broad range of public and private domestic and international business, community and government organizations and leaders on pandemic and other health and safety, workforce and performance preparedness, risks and change management, disaster preparedness and response and other operational and tactical concerns throughout her adult life. A former lead advisor to the Government of Bolivia on its pension project, Ms. Stamer also has worked internationally and domestically as an advisor to business, community and government leaders on crisis preparedness and response, privacy and data security, workforce, health care and other policy and enforcement, as well as regularly advises and defends organizations about the design, administration and defense of their organizations workforce, employee benefit and compensation, safety, discipline and other management practices and actions.
Ms. Stamer also serves in leadership of a broad range of professional and civic organizations and shares insights and thought leadership through her extensive publications and public speaking. For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources available here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here. ©2020 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.
 Comments Off on Businesses Should Confirm Using Benefits, Meeting Mandates Of Special COVID-19 Tax Rules |
Comments Off on Businesses Should Confirm Using Benefits, Meeting Mandates Of Special COVID-19 Tax Rules |  401(k), Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act, retirement plan, Retirement Plans, Retirements, Unemployment Benefits, Unemployment Insurance |
401(k), Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act, retirement plan, Retirement Plans, Retirements, Unemployment Benefits, Unemployment Insurance |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 18, 2019
The Small Business Administration (“SBA”) Advocacy Office will is host an Employee Benefits Roundtable on Thursday, Nov. 21 from 10:00 AM until 12:00 noon at the SBA Headquarters in Washington, D.C. with the following agenda:
Welcome and Introductions (10:00 am – 10:15 am)
- Charles G. Jeane, Assistant Chief Counsel, SBA Office of Advocacy
Discussion of Small Business Use of Cafeteria Plans (10:15 am – 10:45 am)
- Gary Kushner, President and CEO of Kushner & Company
Discussion of MEPs and Open MEPs (10:45 am – 11:15 am)
- Sandra Turner, President of Retirement Plan Specialists, Inc.
Discussion of Adding Annuities as An Option for Plan Participants (11:15 am – 11:45 am)
- Chantel Sheaks, Executive Director, Retirement Policy, U.S. Chamber of Commerce
Open Discussion/Other Small Business Issues (11:45 am – 12:00 pm).
The purpose of these roundtable meetings is to exchange opinions, facts, and information and to obtain the attendees’ individual views and opinions regarding small business concerns. The meetings are not intended to communicate or achieve any consensus positions of the attendees.
Roundtable meetings are open to all interested persons, except the press. Press are excluded in order to facilitate an open and frank discussion about small business-related issues.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters.
Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies.
She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life.
In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations.
Ms. Stamer also is a highly popular public speaker, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on SBA Hosts Employee Benefits Roundtable 11/21 |
Comments Off on SBA Hosts Employee Benefits Roundtable 11/21 |  401(k), 4980D, 4980H, 6039D, Brokers, Cafeteria Plans, compensation, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, EBSA, Employee Benefits, Employers, Employment, ERISA, Fringe Benefit, Fringe Benefits, health Care, health care transparency, health insurance, Health Plans, Human Resources, multiple employer plan (Meps), Retirement Plans, Uncategorized |
401(k), 4980D, 4980H, 6039D, Brokers, Cafeteria Plans, compensation, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, EBSA, Employee Benefits, Employers, Employment, ERISA, Fringe Benefit, Fringe Benefits, health Care, health care transparency, health insurance, Health Plans, Human Resources, multiple employer plan (Meps), Retirement Plans, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 15, 2019
Tax exempt organizations and tax exempt employee benefit plans take note. The Internal Revenue Service (IRS) exempt organization determination procedures are changing.
Revenue Procedure 2019-5 updates the Exempt Organization determination letters procedures. Changes include:
Adding references to “new” Form 1024-A, Application for Recognition of Exemption Under Section 501(c)(4) of the Internal Revenue Code
Clarifying that the IRS won’t rule on a request under IRC Section 501(c)(6) for an organization whose purpose relates to a controlled substance that is illegal under federal law
Increasing user fees for certain miscellaneous determinations from $1,000 to $2,000
Changing the name of the Office of Associate Chief Counsel, Tax Exempt and Government Entities, to the Office of Associate Chief Counsel, Employee Benefits, Exempt Organizations and Employment Taxes.
These changes will impact processes for submitting approval applications and other exempt organization, VEBA, fraternal benefit association and qualified employee plan dealings with the IRS. Impacted organizations, their leaders and advisors will want to adjust accordingly.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on IRS Updates Plan Exemption & Exempt Organization Approval Procedures & Group Name |
Comments Off on IRS Updates Plan Exemption & Exempt Organization Approval Procedures & Group Name |  401(k), compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employer, Employers, Employment Tax, ESOP, Exempt, HR, Human Resources, MEWA, multiple employer plan (Meps), Patient Protection & Affordable Care Act, Plan Admistrator, Retirement Plans, Tax, tax exemption, Tax Qualification, third party administrators, Union |
401(k), compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employer, Employers, Employment Tax, ESOP, Exempt, HR, Human Resources, MEWA, multiple employer plan (Meps), Patient Protection & Affordable Care Act, Plan Admistrator, Retirement Plans, Tax, tax exemption, Tax Qualification, third party administrators, Union |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 14, 2019
Beginning April 1, 2019, applicants seeking to resolve employee benefit tax qualification issues via the Voluntary Compliance Resolution (VCR) program must submit applications electronically through Pay.gov. Any paper VCP submissions sent to the IRS with a postmark after March 31, 2019, will be returned to the applicant.
The IRS maintains a correction program that permits any size business or organization that sponsors a retirement plan (including SEP and SIMPLE IRA plans) to identify and correct problems they find. Where applicable, self correction program via the Employee Plans Compliance Resolution System (EPCRS), outlined in Revenue Procedure 2018-52 can solve manybpribkems
Under the Self-Correction Program (SCP), employer and other plan sponsors can correct many plan mistakes without contacting the IRS with many potential advantages including:
- Identify and correct mistakes using the procedures in EPCRS
- Do not notify the IRS
- Pay no fees to the IRS
- Your plan’s tax benefits are preserved
The Much more complicated Voluntary Correction Program (VCP) works for mistakes that are not eligible for self-correction or if the sponsor wants IRS assurance about how it corrected a mistake. Voluntary compliance resolution is much less flexible:
- You must make a written submission and pay a compliance fee to the IRS, prior to an IRS audit;
Disclose the self-identified problems along with a proposal to fix the problem
The IRS determines if the proposal is acceptable and issues a compliance statement documenting approval
- Your plan’s tax benefits are preserved.
The IRS also shares the following tips when making a VCP submission electronically through Pay.gov:
- A VCP application is not considered filed with the IRS until the VCP user fee has been paid and the Pay.gov website generates a payment confirmation receipt. If you don’t have a receipt with a Pay.gov Tracking ID #, you haven’t made a VCP submission to the IRS.
- Include all required VCP submission items in your PDF file that’s uploaded to the IRS. See Rev. Proc. 2018-52, section 11.04 and, if applicable, enclosure lists associated with the model VCP submission forms in the Form 14568-A through Form 14568-I series.
- The completed Form 8950 is uploaded automatically, so don’t include any copy of the Form 8950 as part of the uploaded PDF file containing the VCP submission documents.
- Place the VCP submission documents in the uploaded PDF in the order specified by Rev. Proc. 2018-52, section 11.11.
Prior to making a submission, review the electronic VCP submission process outlined in Revenue Procedure 2018-52. For more information, check out this IRS video and review Updated Retirement Plan Correction Procedures that discuss the VCP submission process.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on IRS Requires Electronic VCR Applications Beginning April 1. |
Comments Off on IRS Requires Electronic VCR Applications Beginning April 1. |  401(k), defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, ESOP, multiple employer plan (Meps), pension plan, Retirement Plans, Uncategorized |
401(k), defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, ESOP, multiple employer plan (Meps), pension plan, Retirement Plans, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 14, 2019
Employee benefit plan sponsors, fiduciaries, administrators and advisors should review and update their benefit and compensation plan designs and testing in response to the just released tables of covered compensation under § 401(l)(5)(E) of the Internal Revenue Code and related regulations for the 2019 plan year in new Revenue Ruling 2019-06.
The new tables are available in the advance release copy of Revenue Ruling 2019-06, scheduled for official publication in Internal Revenue Bulletin 2019-14 on April 1, 2019.
The Revenue Ruling provides tables of covered compensation under § 401(l)(5)(E) of the Internal Revenue Code and related regulations for the 2019 plan year.
For this purpose, covered compensation is average of the contribution and benefit bases in effect under section 230 of the Social Security Act for each year in the 35 year period ending with the year in which an employee attains social security retirement age.
As the change will impact plan contribution limits, discrimination testing and other plan and contribution design and administration, employer and other plan sponsors, fiduciaries, administrators and service providers should evaluate the effects of the adjustments so as to maximize their ability to anticipate and respond to the adjustments.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on IRS Updates 2019 Compensation Table |
Comments Off on IRS Updates 2019 Compensation Table |  105(h), 401(k), 4980H, ACA, board of directors, Brokers, church plan, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ESOP, FICA, Health Benefits, health insurance, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, multiple employer plan (Meps), pension plan, retirement plan, Retirement Plans, Retirements, Tax Qualification, Uncategorized |
105(h), 401(k), 4980H, ACA, board of directors, Brokers, church plan, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ESOP, FICA, Health Benefits, health insurance, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, multiple employer plan (Meps), pension plan, retirement plan, Retirement Plans, Retirements, Tax Qualification, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 13, 2018
Employers should invite employees to update their Form W-4 withholding and finalize other 2019 payroll and income tax withholding arrangements based on guidance for 2019 published by the IRS and Treasury Department in Notice 2018-92 on November 26, 2018.
Many U.S. employers had delayed making changes to their income and payroll tax withholding pending the anticipated release by the IRS and Treasury Department of a revised Form W-4 and related income and payroll tax guidance updated to reflect changes to the Internal Revenue Code enacted as part of the Tax Cut and Jobs Act (P.L. 115-97)(“Trump Tax”) at the end of 2017.
Following the enactment of Trump Tax, most businesses have operated in reliance upon interim guidance published by the agencies at the beginning of the year to carryout their 2018 withholding obligations.
Until recently, the IRS and Treasury Department were expected to complete for use in 2019 the major overhaul of the Form W-4 and related guidance in response to the Trump Tax amendments to Sections 3402, 3405 and other Code rules. When the revision of the Form W-4 proved more complex than anticipated, however, the IRS and Treasury Department in September, 2018 announced that release of the newly designed and updated Form W-4 would be delayed from 2019 to 2020.
In Notice 2018-92, IRS and the Treasury Department provides interim guidance to employers and their workers on income tax withholding for 2019 pending agencies issuance of regulations implementing the changes, as well as requests comments on certain withholding procedures from concerned parties. For the most part, Notice 2018-92 continues the interim guidance that IRS and Treasury previously published for 2018. Specifically, Notice 2018-92:
- Announces that the 2019 Form W-4 will be similar to the 2018 Form W-4,
- Addresses new TCJA “withholding allowance” terminology,
- Continues until April 30, 2019 Notice 2018-14’s temporary suspension of the requirement to furnish new Forms W-4 within 10 days for changes resulting solely from the TCJA,
- Provides that, for 2019, the default rule when an employee fails to furnish a Form W-4 will continue to be single with zero withholding allowances,
- Allows taxpayers to take into account the qualified business income deduction under section 199A to reduce withholding under section 3402(m),
- Announces that the IRS and Treasury intend to update the regulations under section 3402 to explicitly allow taxpayers to use the online withholding calculator or Publication 505, Tax Withholding and Estimated Tax, in lieu of the worksheets to Form W-4,
- Requests comments on alternative withholding methods under section 3402(h),
- Announces that the IRS and the Treasury Department intend to eliminate the combined income tax withholding and employee FICA tax withholding tables under Treas. Reg. § 31.3402(h)(4)-1(b),
- Modifies notification requirements for the withholding compliance program, and
- Provides that for 2019, withholding on annuities or similar periodic payments where no withholding certificate is in effect is based on treating the payee as a married individual claiming 3 withholding allowances under § 3405(a)(4).
The Code generally requires employees that experience a change that reduces the number of withholding exemptions that the employee qualifies to claim to notify their employer and complete a new Form W-4 within 10 days of a specified event date. Interim relief published by the IRS and Treasury Department provides relief to workers whether the change in withholding eligibility results solely due to a Code change enacted as part of Trump Tax. Otherwise, however, employees generally still remain obligated to keep their withholding up-to-date. Since employees often are unaware of or overlook this responsibility, employers generally should encourage workers to review and update their Form W-4 withholding elections in connection with annual enrollment periods and in conjunction with other life or other changes likely to affect the withholding eligibility of the worker.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on Finalize 2019 Withholding Prep In Light of Notice 2018-92 |
Comments Off on Finalize 2019 Withholding Prep In Light of Notice 2018-92 |  105(h), 401(k), 4980D, 4980H, 6039D, board of directors, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, EBSA, employee, Employee Benefits, Employer, Employment, Employment Tax, Excise Tax, Executive Compensation, Fringe Benefit, Health Benefits, health insurance, HR, HSA, Human Resources, Income Tax, Payroll Tax, Tax Credit, Tax Qualification, TCJA Tax Reform, Uncategorized | Tagged: Tax, Withholding |
105(h), 401(k), 4980D, 4980H, 6039D, board of directors, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, EBSA, employee, Employee Benefits, Employer, Employment, Employment Tax, Excise Tax, Executive Compensation, Fringe Benefit, Health Benefits, health insurance, HR, HSA, Human Resources, Income Tax, Payroll Tax, Tax Credit, Tax Qualification, TCJA Tax Reform, Uncategorized | Tagged: Tax, Withholding |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
September 12, 2018
On Thursday, August 13, the House Ways & Means Committee will hold hearings on retirement rule reforms intended to change multiemployer plan rules to make it easier for small businesses to offer and their employees and independent contractors to participate in retirement plans and provide retirement plan relief for participants proposed in the Family Savings Act of 2018, H.R. 6757.
Part of recently 3-bill tax package dubbed “Tax Reform 2.0” introduced on Monday, September 10, H.R. 6757 would remove certain regulatory barriers restricting the types of small-business employers who are permitted to band together to offer a retirement plan through a multiple employer plan (MEP).
H.R. 6757 also includes relief for certain plan participants. Among other things, it would:
- End required minimum distributions of funds from 401(k) plans and other retirement savings accounts for retirees with balances under $50,000; and
- Protect the ability of participants invested in lifetime income options through an employment-based retirement plan against losing these investment guarantees when their employer changes recordkeepers.
Sponsored by Rep. Mike Kelly (R-PA), and cosponsored by Rep. Paul Mitchell (R-MI), House Ways and Means Committee Chairman Kevin Brady (R-TX), and all other Ways and Means Committee Republicans, H.R. 6757, the bill enjoys strong support among House Republicans and President Trump.
House Ways and Means Committee Chair Kevin Brady expressed strong support for its reforms, saying: “We are creating financial security. The Family Savings Act focuses on helping families save more and earlier for the future by making it easier for businesses to offer retirement savings plans while ensuring workers can easily participate in these plans. This will help give our families the financial stability they need for whatever life throws their way.”
The Ways and Means Committee will address the H.R. 6757 proposals during its scheduled Tax Reform 2.0 markup on Thursday, September 13, 2018 at 10:00 a.m. in Room 1100 of the Longworth House Office Building. Use these links to read these bills:
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following
▪DOL Spending Reports Required As Taxpayer Tool Need Improvement
▪Check & Protect Health & Other Electronic Systems & Data Against New Security Threat
▪April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26
▪Arizona Proposal To Ban Sexual Harassment Confidentiality Agreements Sign Of Growing Employer Risks
▪$23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses
▪Take Care of Your Good People
▪Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source
▪Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning
▪IRS Prepares To Nail Employers Under Obamacare Mandate While Giving Some Individual Mandate Relief
▪Hiring & Retaining Workers Growing Business Challenge
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on House W&M Committee To Markup Retirement and Other “Tax Reform 2.0” Bills Thursday |
Comments Off on House W&M Committee To Markup Retirement and Other “Tax Reform 2.0” Bills Thursday |  401(k), Banking, Brokers, compensation, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, employee, Employee Benefits, Employer, Employers, Employment Policies, Employment Tax, ERISA, ESOP, Fiduciary Responsibility, Human Resources, Income Tax, multiple employer plan (Meps), Retirement Plans, Retirements, Tax, Tax Qualification, TCJA Tax Reform, Uncategorized |
401(k), Banking, Brokers, compensation, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, employee, Employee Benefits, Employer, Employers, Employment Policies, Employment Tax, ERISA, ESOP, Fiduciary Responsibility, Human Resources, Income Tax, multiple employer plan (Meps), Retirement Plans, Retirements, Tax, Tax Qualification, TCJA Tax Reform, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 18, 2018
Employers should consider inviting their workers to conduct a Paycheck Checkup to review their withholding elections to confirm they have the right amount of tax deducted from their paychecks in response to tax law changes enacted by the Tax Cuts and Jobs Act (Trump Tax) and other recent legislation. Helping workers properly to take into account tax relief or other changes reducing their income tax liability can help boost workers’ take home pay, helping them to see more benefit from the wages paid by the employer at payday.
The amount of withholding that an employer withholds from an employee’s pay generally depends upon two factors:
- The amount the employee can earn; and
- The accuracy of the personal information the employee uses to complete the Form W-4 to notify the employer of his withholding elections; and
- The tax rules that decide how much tax the employee ultimately will owe when their personal income tax returns become due on April 15, 2018.
Although most employees don’t think about the potential need to re-evaluate the withholding elections on their current Form W-4 unless reminded by an employer or professional advisor, it’s generally a good idea for workers to periodically review and update their withholding elections since these often change from time to time. Encouraging workers to periodically review and update their W-4 elections can help workers maximize their take home pay while minimizing the risk of being surprised with an unexpected income tax or even under withholding penalty when they file their annual income tax return.
A number of recent events make it particularly likely that employees will benefit from re-evaluating their W-4 withholding now. For one thing, the Tax Cuts and Jobs Act recently changed the way income tax is calculated for most individual taxpayers. As many of these changes were enacted to provide individual tax relief for many taxpayers, workers qualifying for this relief that do not review and update their withholding elections likely are having the employer withhold more tax than necessary from their paychecks. Beyond these tax rule changes, many workers also may need to update their withholding elections in response to changes in their income, marital or other family status or other changes in their personal situation that also can affect the income tax withholding of the individual worker.
The Internal Revenue Service recently updated the Withholding Calculator the IRS provides on its website to help individuals estimate their annual income tax for purposes of deciding the withholding they should enter on their Form W-4 in light of the Tax Cuts and Jobs Act changes. Individuals can use the Withholding Calculator to estimate their 2018 and to compare their current tax withholding to help the individual decide if the individual needs to change his withholding with an employer.
More details about the Withholding Calculator and the new 2018 withholding tables can be found using the following internet links on the IRS’ Frequently Asked Question pages:
Employers should consider sending a reminder to workers to review their Form W-4 using these tools to determine if they can increase their take home pay by changing their withholding to take into account any potential income tax and withholding reductions they qualify for, if any, as a result of the Tax Cuts and Jobs Act or other changes in factors that impact their withholding and income tax liability or if other changes are warranted. Because most employees just completed their annual tax returns and likely have not considered the potential need to change their elections for tax reform or other changes, employees are likely to be particularly receptive and responsive to these reminders now. Employers and benefit plan administrators also may wish to consider helping employees remember to review and update their Form W-4 withholding when sending benefit enrollment packages, processing benefit enrollment elections when announcing pay increases or bonuses, in employee handbooks or payroll stuffers, at annual enrollment times or in response to mid-year election or beneficiary change notifications and at other times when the employer or their benefit plans deal with life event or benefit election events that could impact an employee’s withholding.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
The author of the “Texas Payday Act,” and numerous other highly regarded publications on wage and hour and other human resources, employee benefits and compensation publications, Ms. Stamer is well-known for her 30 years of extensive wage and hour, compensation and other management advice and representation of restaurant and other hospitality, health, insurance, financial services, technology, energy, manufacturing, retail, governmental and other domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advice or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Remind Employees To Update Withholding |
Comments Off on Remind Employees To Update Withholding |  105(h), 401(k), 4980D, 4980H, 6039D, Cafeteria Plans, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, Employment Tax, Excise Tax, Excise Taxes, Executive Compensation, health benefit, Health Benefits, health plan, Health Plans, HR, Human Resources, Income Tax, Internal Revenue Code, Labor Management Relations, Management, Pay, Payroll Tax, Tax, Tax Qualification, Uncategorized |
105(h), 401(k), 4980D, 4980H, 6039D, Cafeteria Plans, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, Employment Tax, Excise Tax, Excise Taxes, Executive Compensation, health benefit, Health Benefits, health plan, Health Plans, HR, Human Resources, Income Tax, Internal Revenue Code, Labor Management Relations, Management, Pay, Payroll Tax, Tax, Tax Qualification, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 24, 2018
Department of Labor (DOL) and other agencies’ spending reports posted at USASpending.gov to comply withthe Digital Accountability and Transparency Act of 2014 (DATA Act) are intended to help taxpayers, government leaders and others monitor and evaluate agency spending. However a new report from the DOL Office of Inspector General (OIG) found data reporting and other issues have compromised the reliability of the data reported in DOL reports posed on USASpending.gov.
The Data Act requires federal agencies to report spending data in accordance with new government-wide data standards developed by the Office of Management and Budget (OMB) and the Department of Treasury (Treasury). The data reports are posted on so taxpayers and policy makers understand how the Department is spending its funds. The Act requires federal agencies to report spending data in accordance with new government-wide data standards developed by the Office of Management and Budget (OMB) and the Department of Treasury (Treasury). The Act also requires the Inspectors General of each federal agency to conduct a review of the agency’s DATA Act compliance every two years and report on the completeness, timeliness, accuracy, and quality of the agency’s data.
The new report reports OIG’s findings from a performance audit OIG performed to assess: (1) the completeness, timeliness, accuracy, and quality of data submitted by the Department; and (2) the Department’s implementation and use of the Government-wide data standards established by OMB and Treasury for the Fiscal Year 2017 second quarter. While OIG found DOL effectively implemented and used the Government-wide data standards established by OMB and Treasury to prepare the reports and timely submitted the DATA Act required reports, it found numerous issues with the overall quality of the spending data it submitted for publication on USAspending.gov. Among other things, OIG reports that DOL:
- Did not report all the required data elements for 19 percent of the transactions sampled. OIG found 77% of these errors occurred because the Department did not include Unique Record Identifiers for transactions when it was required to. This could cause issues when linking financial data with grant data on USAspending.gov.
- 74% of the transactions sampled contained an error in one or more data elements. OIG reports many of these errors resulted from issues in the Treasury’s DATA Act broker data extraction process.
- Excluding those errors, 52% of the transactions sampled contained inaccurate information.
- In addition to errors uncovered from OIG’s sampling audit, DOL also reported inaccurate program activity and object class codes for 5 and 7 percent of transactions, respectively, in its File B submission.
OIG attributes these errors in accuracy and completeness occurred because of data entry mistakes, data extraction issues, and weak data validation processes and concluded that these control deficiencies will have a negative impact on the quality of the data DOL reports until corrected.
Based on these findings, OIG has made eight recommendations to DOL’s Principal Deputy Chief Financial Officer to improve the quality of the data the DOL reports to USAspending.gov in the future and to strengthen internal controls over its data management processes.
While OIG reports DOL has concurred with these recommendations and has stated it has implemented additional controls, resulting in fewer errors with each submission, taxpayers and others using past reports need to consider the reported deficiencies in their evaluation and use of the data as well as assess the validity of future reported data for possible issues for future assessments. Even considering these issues, however, taxpayers and government leaders should consider consulting the data when investigating or evaluating DOL or other program activities or expenditures for policy, enforcement priority or other purposes.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on DOL Spending Reports Required As Taxpayer Tool Need Improvement |
Comments Off on DOL Spending Reports Required As Taxpayer Tool Need Improvement |  401(k), Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, Defined Contribution Plans, Discrimination, Disease Management, Drug & Alcohol, EBSA, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, ERISA, Executive Compensation, Fair Labor Standards Act, family leave, fiduciary duty, Fiduciary Responsibility, FLSA, Government Accountability, Government Contractors, h-2A Visa, Health Benefits, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, LEP, LGBT, Management, medical leave, Mental Health, MEWA, Military Leave, mine safety, MSHA, NLRA, Obamacare, occupational safety, officers, OSHA, Overtime, Patient Empowerment, Pay, pension plan, Plan Admistrator, Prescription Drugs, Public Policy, Reporting & Disclosure, Retirement Plans, Retirements, Sexual Harassment, Unfair Labor Practice, Union, VEVRAA, Wellness Programs |
401(k), Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, Defined Contribution Plans, Discrimination, Disease Management, Drug & Alcohol, EBSA, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, ERISA, Executive Compensation, Fair Labor Standards Act, family leave, fiduciary duty, Fiduciary Responsibility, FLSA, Government Accountability, Government Contractors, h-2A Visa, Health Benefits, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, LEP, LGBT, Management, medical leave, Mental Health, MEWA, Military Leave, mine safety, MSHA, NLRA, Obamacare, occupational safety, officers, OSHA, Overtime, Patient Empowerment, Pay, pension plan, Plan Admistrator, Prescription Drugs, Public Policy, Reporting & Disclosure, Retirement Plans, Retirements, Sexual Harassment, Unfair Labor Practice, Union, VEVRAA, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 10, 2018
Employer and sponsors, fiduciaries, administrators and insurers of employee benefitplansof any type covered by the Employee Retirement Income Security Act (ERISA) making any disability based determinations now have until April 1, 2018 to bring their plans’ claims and appeals procedures for disability-based decisions and related notices and communications into compliance with substantially more complicated requirements in new Department of Labor Employee Benefit Security Administration (EBSA) regulations.
The EBSA announced on January 5, 2018 the extension of the effective date of new requirements for benefit plan processing and providing notification about claims or appeals involving disability determinations from their originally scheduled effective date of January 1, 2018 to April 1, 2018.
While the extension gives employer and other sponsors, fiduciaries, administrators and insurers of employee benefit plans making disability-based benefit determinations a few extra months to review and update their plan documents, summary plan descriptions, procedures, processes and claims and appeals notices to meet tightened new federal rules on disability-based benefit determinations applicable to all post December 31, 2017 claims under the restated Final Rule on Claims Procedure for Plans Providing Disability Benefits (“Disability Claims Rule”), the nature and scope of these new requirements will require updates to virtually all ERISA-covered benefit plans with any disability dependent provisions. These updates are likely to include changes to plan documents, summary plan descriptions, notices, contracts, processes and procedures for a broad range of plans. Consequently, employer and other plan sponsors, fiduciaries, administrators, insurers and others responsible for any benefit plan not already reviewed and updated to comply should get moving to complete the necessary review and update to meet the April 1, 2018 deadline.
Cynthia Marcotte Stamer and others will lead a free telephone study group discussion of “Claims Regulations and Other Developments Affecting Plan Fiduciaries” on January 26, 2018 beginning at 1 PM (Eastern), Noon (Central), 11 AM (Mountain), and 10 AM (Pacific). For more details about the Study Group, see here.
New Disability Claims Rule Overview
Originally published in final form by the EBSA on December 16, 2016, the Disability Claims Rule generally require all ERISA-covered employee benefit plans making any disability benefit or other determination conditioned upon a finding of disability to comply with the new Disability Claims Rule for any claim received after March 31, 2018.
Based on EBSA’s previously adopted Patient Protection and Affordable Care Act (“ACA”) group health plan claims and appeals rules, the new Final Disability Claims Rule will apply to all disability determinations made under any ERISA-covered plan after March 31, 2018, regardless of how the plan characterizes the benefit or whether the plan is a health or other welfare, pension, 401(k) plan or other savings plan.
The new Disability Claims Rule will apply to a broad range of plans, most of which historically have not followed the detailed claims and appeals notification, independent and impartial decision-making, rescission, deemed exhaustion, “culturally and linguistically appropriate” and other procedural protections and safeguards that the Disability Claims Rule extends from the current group health plan rules to all ERISA-covered plans making benefit determinations based on disability. Consequently covered plans making disability-based benefit or other covered determinations are likely to require updates to plan documents, insurance or administrative services contracts, summary plan descriptions and other plan communications, claims and appeals notices, and other related processes, procedures and documentation to meet these new requirements. Since certain requirements of the Disability Claims Rules like the summary plan description advance disclosure requirements are required to be provided before the claim is received, plans and their sponsors, fiduciaries, insurers and administrators risk being accused of violating these requirements by waiting to update plans, their processes and materials until after claim involving a disability based determination arises.
Ensuring that impacted plans are updated before the April 1, 2018 deadline is important because the Disability Claims Rule, like the group health plan claims and appeals rules upon which it is based, also states that noncompliance with any of its requirements empowers a participant to immediately sue the plan for enforcement if his rights without further complying the the plan’s administrative procedures. Moreover, failing to comply with summary plan disclosure or claims or appeal adverse benefit determination notification requirements also may subject the plan administrator to administrative penalties under ERISA section 514(c); fiduciaries to ERISA fiduciary liability, and compromise the ability to defend otherwise defensible decisions. Consequently, employers and other plan sponsors, fiduciaries, administrators and insurers will want to act quickly to ensure that their plans, their summary plan descriptions and other communications, notices, processes, contracts and procedures are updated appropriately before April 1, 218.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |
Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |  401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |
401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 5, 2018
Continuing Fallout of 2015 Data Breach Provides Many Lessons For Other Businesses & Their Health Plans
Read the rest of this entry »
 Comments Off on $23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses |
Comments Off on $23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses |  ADA, Association Health Plan, Banking, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Claims Administration, compensation, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Excise Taxes, FACTA, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Breach, HIPAA, Identity Theft, Privacy, Technology |
ADA, Association Health Plan, Banking, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Claims Administration, compensation, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Excise Taxes, FACTA, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Breach, HIPAA, Identity Theft, Privacy, Technology |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 18, 2017
Want to know what tax changes are included in the Tax Cuts and Jobs Act (H.R. 1) (Act”) and expected to pass Congress tomorrow (December 20, 2017)? Check out the House Conference Committee Report, H. Rept. 115-466 (the “Conference Report”) released on Friday, December 15, 2017.
The House Conference Committee Report details the negotiated reconciliation of House Bill (H.R. 1) as passed by the House of Representatives on November 16, 2017 and the provisions of H.R. 1 with amendments passed by the Senate on December 2, 2017. Over the past few weeks, a joint committee made up of key representatives from the House and Senate have engaged in highly publicized negotiations to reconcile differences in the House and Senate versions of the Act. The House Conference Committee Report signed off by the Conference Committee and filed in the House of Representatives of December 15, 2017 documents the agreements reached by House and Senate Conferees reconciling the House and Senate versions of H.R. 1, which Congress will vote upon this week. Solutions Law Press, Inc. will publish analysis of various provisions of these reforms over the next few days. In the meantime, taxpayers interested in learning about the Act may use the links in this article to begin familiarizing themselves with its provisions.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses work with domestic and international businesses of all types and sizes as well as extensive work with Congress and U.S. federal and state regulatory agencies on workforce, compensation and benefits, and performance and operational compliance challenges. A primary drafter of the Bolivian Pension Privitization law who also has worked on workforce, tax, employee benefits, health care, insurance, safety, immigration, privacy and data security and other federal and state legal reforms domestically and internationally throughout her adult life, Ms. Stamer also has been extensively involved in various aspects of Congressional considerations of the current Act and other legislation considered by the current Congress.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations, for clients and others.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source |
Comments Off on Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source |  105(h), 401(k), 5000, Cafeteria Plans, church plan, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Agreement, Employment Tax, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Income Tax, Insurance, insurers, IRC, Management, Obamacare, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, pension plan, Premium Subsidies, retirement plan, Retirement Plans, Risk Management, Social Security, Tax, Tax Credit, Tax Qualification, Uncategorized | Tagged: tax reform, Taxes |
105(h), 401(k), 5000, Cafeteria Plans, church plan, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Agreement, Employment Tax, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Income Tax, Insurance, insurers, IRC, Management, Obamacare, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, pension plan, Premium Subsidies, retirement plan, Retirement Plans, Risk Management, Social Security, Tax, Tax Credit, Tax Qualification, Uncategorized | Tagged: tax reform, Taxes |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 18, 2017
Employers, employee benefit plan sponsors and administrators, vendors and their advisors and service providers should re-evaluate their existing payroll and other settings and elections, planning, testing and related strategies and assumptions in light of the 2018 annual cost-of-living adjustments (COLAs) to the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits announced by the Internal Revenue Service (IRS) in Notice 2017-64, IRB 2017-45 on November 6, 2017.
H.R. 1, Tax Cuts and Jobs Act (Tax Refirm Bill) reported out of the Conference Committee last week and scheduled for a vote before Congress tomorrow leaves these limits substantially unchanged.
Notice 2017-64 adjusts the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits. The Section 415 limitations COLAs are made and published annually to comply with Section 415(d)’s requirement that the Treasury Security annually adjust these limits for cost-of-living increases. Other limitations applicable to deferred compensation plans are also affected by these adjustments under § 415. Under § 415(d), the adjustments are to be made under adjustment procedures similar to those used to adjust benefit amounts under § 215(i)(2)(A) of the Social Security Act.
In addition to impacting contribution limits permitted to defined benefit, 401(k) and other defined contribution and other plans, the changes can impact the definition of highly compensated employees, discrimination testing, plan funding and a broad range of employee benefit, compensation, tax, payroll, union or other contracting and other concerns for employers, employee benefit plan sponsors, fiduciaries, administrators, payroll, plan and other vendors, participants and beneficiaries and others.
The following is a chart of the adjusted limits compared to the currently applicable 2017 limitations. (Download chart)
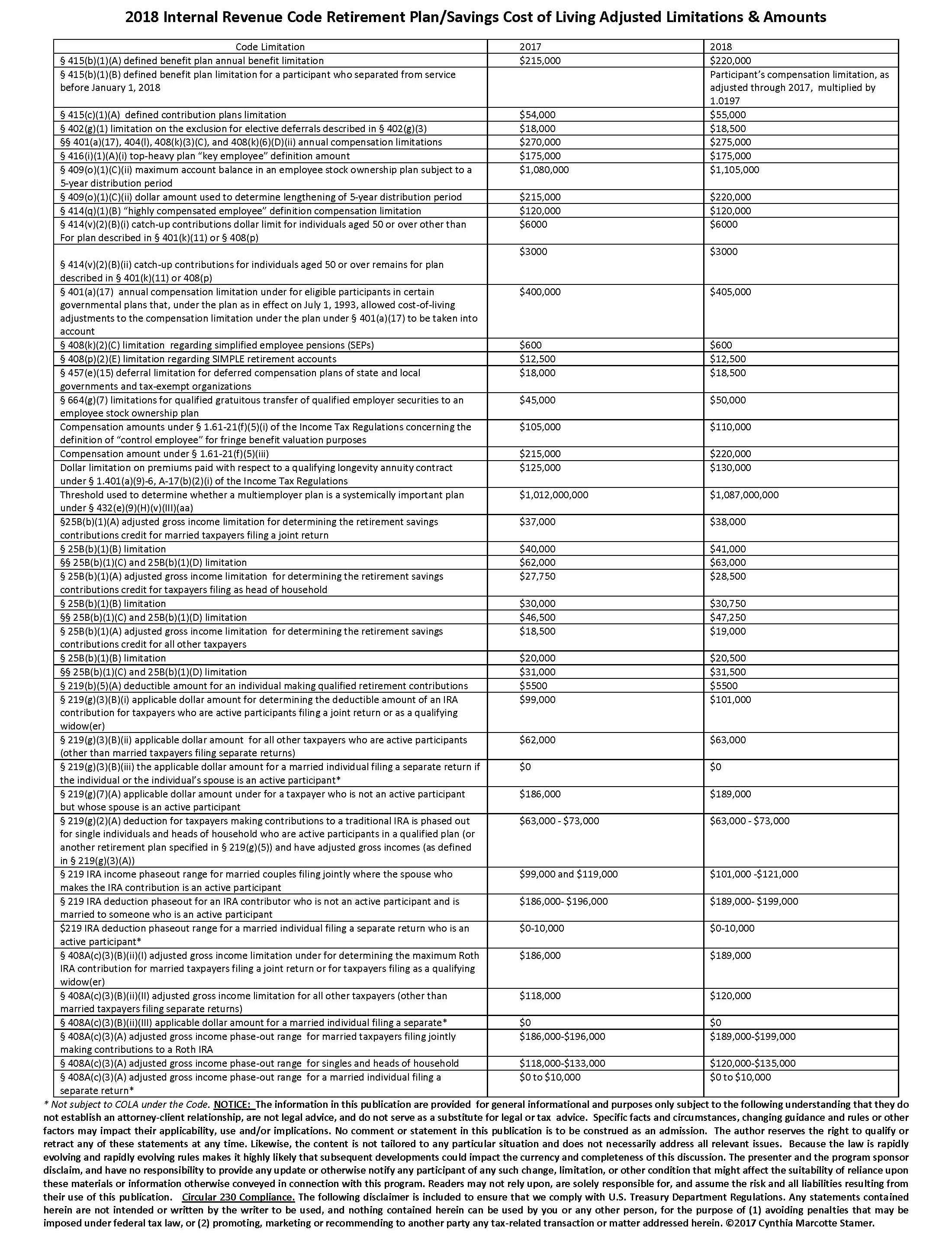
Employers, employee benefit plan sponsors, fiduciaries, administrators and other vendors, participants and beneficiaries and others working with employee benefit plans or compensation contributed to these arrangements should review these new 2018 COLA limitations to assess their potential impact and make appropriate adjustments to avoid compliance challenges or other unfortunate surprises in 2018. If they already have not already done so, reviewing the 2018 Social Security Act COLAs also would be wise. See 2018 Social Security COLAs Set.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |
Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |  401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |
401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 14, 2017
Employer and other sponsors, fiduciaries, administrators and insurers of the Employee Retirement Income Security Act (ERISA)-covered employee benefit plans making disability-based benefit determinations should confirm that their plan documents, summary plan descriptions, procedures and claims and appeals notices are updated and ready to meet tightened new federal rules on disability-based benefit determinations applicable to all post December 31, 2017 claims under the restated Final Rule on Claims Procedure for Plans Providing Disability Benefits (“Disability Claims Rule”). Given the nature and scope of these new requirements, most covered plans will require specific action be taken before the new rules take effect to update plan documents, summary plan descriptions, notices, contracts, processes and procedures to meet the January 1, 2018 deadline.
The Disability Claims Rule published by the Department of Labor Employee Benefit Security Administration (“EBSA”) on December 19, 2016 generally require all ERISA-covered employee benefit plans making any disability benefit or other determination conditioned upon a finding of disability to comply with the new Disability Claims Rule for any claim received after December 31, 2017.
The new Final Disability Claims Rule will apply to all disability determinations made under any ERISA-covered plan after December 31, 2017, regardless of how the plan characterizes the benefit or whether the plan is a health or other welfare, pension, 401(k) plan or other savings plan.
Significant affirmative action is likely required to prepare covered plans to meet these requirements since most plans historically have not followed the detailed claims and appeals notification, independent and impartial decision-making, rescission, deemed exhaustion, “culturally and linguistically appropriate” and other procedural protections and safeguards based on EBSA’s previously adopted Patient Protection and Affordable Care Act (“ACA”) group health plan claims and appeals rules, which the Disability Claims Rules extend and make applicable to all ERISA-covered plans making benefit determinations based on disability. Covered plans making disability-based benefit or other covered determinations are likely to require updates to plan documents, insurance or administrative services contracts, summary plan descriptions and other plan communications, claims and appeals notices, and other related processes, procedures and documentation to meet these new requirements. Since certain requirements of the Disability Claims Rules like the summary plan description advance disclosure requirements are required to be provided before the claim is received, plans and their sponsors risk being accused of violating these requirements by waiting to update plans, their processes and materials until after claim involving a disability based determination arises.
Ensuring that impacted plans are updated before the January 1, 2018 deadline is important because the Disability Claims Rule, like the group health plan claims and appeals rules upon which it is based, also states that noncompliance with any of its requirements empowers a participant to immediately sue the plan for enforcement if his rights without further complying the the plan’s administrative procedures. Moreover, failing to comply with summary plan disclosure or claims or appeal adverse benefit determination notification requirements also may subject the plan administrator to administrative penalties under ERISA section 514(c). Consequently, employers and other plan sponsors, fiduciaries, administrators and insurers will want to act quickly to ensure that their plans, their summary plan descriptions and other communications, notices, processes, contracts and procedures are updated appropriately before January 1, 2018.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediatepast RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, BenefitsMagazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Confirm Your Benefit Plans Ready For New Disability Determination Rules on 1/1/18 |
Comments Off on Confirm Your Benefit Plans Ready For New Disability Determination Rules on 1/1/18 |  401(k), ACA, ADA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Disability, Disability, Disability Plans, Drug & Alcohol, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, Leave, Management, medical leave, Mental Health, Mental Health Parity, Obamacare, Patient Protection & Affordable Care Act, Pay, pension plan, Plan Admistrator, Professional Liability, third party administrators, Uncategorized, Union, Worker | Tagged: Appeals, Claims, defined benefit plan, Disability, Disability Insurance, Disability Plan, EBSA, Employee Retirement Income Security act, ERISA, Fiduciary Responsibility, pension plan |
401(k), ACA, ADA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Disability, Disability, Disability Plans, Drug & Alcohol, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, Leave, Management, medical leave, Mental Health, Mental Health Parity, Obamacare, Patient Protection & Affordable Care Act, Pay, pension plan, Plan Admistrator, Professional Liability, third party administrators, Uncategorized, Union, Worker | Tagged: Appeals, Claims, defined benefit plan, Disability, Disability Insurance, Disability Plan, EBSA, Employee Retirement Income Security act, ERISA, Fiduciary Responsibility, pension plan |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 6, 2017
As businesses continue to struggle to comply with the growing plethora of federal and state laws mandating data security, the identity theft and cyber security epidemic keeps growing.
As human resources and other business leaders work to guard their own data and respond to employee demands for assistance in responding to breaches of their personal financial and other data, this weeks’ announcement that embattled credit monitoring giant Equifax has been awarded the exclusive contract to provide taxpayer identification and fraud prevention services to the Internal Revenue Service has many questioning whether these investments are futile.
The IRS’ announcement comes despite the September 7, 2017 announcement by Equifax of a data breach of its records impacting sensitive personal information of millions of consumers including:
- The names, Social Security numbers, birth dates, addresses and, in some instances, driver’s license numbers of an estimated 143 million U.S. consumers;
- Credit card numbers for approximately 209,000 U.S. consumers,
- Certain dispute documents with personal identifying information for approximately 182,000 U.S. consumers,and
- Personal information for certain U.K. and Canadian consumers.
The huge breach already was creating many headaches for many businesses and their human resources departments before the IRS announced the award of the contract to Equifax. Due to the massive size of the breach, mist companies have been required to respond to concerns of workers impacted directly by the breach as well as requests of employees and identity theft protection companies that the business consider offering cybersecurity protection for employees or customers.
Beyond helping their workforce understand and cope with the news, many businesses and employee benefit plans also face the added headache of needing to investigate and respond to concerns about their own potential responsibilities to provide breach notification or take other actions. This added headache arises due to their or their plans’ use of Equifax or vendors utilizing Equifax to run employee or vendor background checks or carry out internal employee or employee benefit plan, customer or other business activities. These involvements often give rise to duties to conduct investigations and potentially provide notification or other responses to employees, applicants, benefit plan members, contractors or customers whose data may have been impacted under the Fair and Accurate Credit Transactions Act (FACTA), the Health Insurance Portability and Accountability Act (HIPAA), the Employee Retirement Income Security Act (ERISA) Fiduciary Responsibility rules or various other federal and state laws and regulations, vendor contracts or their own data privacy or security policies.
When notification is recommended or required, human resources and other business leaders also have to consider if modifications should be considered to standard protocols recommended to data breach victims. Notification and registration as an identity theft victim with Equifax long has been a standard part of the federal and state government recommended protocol for recommended to consumers impacted by identity theft or other data breaches. See,e.g., IRS Taxpayer Guide To Identity Theft. Although government agencies as of yet have not changed this recommendation to remove Equifax reporting, many consumers and others view reporting to Equifax as akin to the fox watching the hen house. Consequently, employers and other parties helping consumers respond to the breach often receive push back or questions from consumers about the appropriateness and security reporting to Equifax in light of its breach.
Beyond evaluating and handling their own legal responsibilities to investigate and deal with any breach impacting their data, employers and other business leaders also likely are or should consider what claims against Equifax, other vendors and business partners involved with Equifax and their own liability insurers are available and warranted to help cover the costs and potential liabilities for the business arising from the breach and it’s fall out.
As employers and other businesses work through these issues, They should keep in mind that the fallout is likely to continue for years and be further complicated by past and subsequent breaches impacting other governmental and private organizations. Human resources, employee benefits and other businesses and their leaders can expect to experience challenges dealing with fraudulent uses of misappropriated information as well as demands that they tighten up their background check, data security and usage and other practices and documentation to mitigate risks from the compromised data.
Human resources, employee benefits and other business leaders need to secure the assistance of counsel experienced in guiding their organizations through these and other challenges.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes. Author of numerous works on privacy and data security, Ms. Stamer‘s experience includes involvement in cyber security and other data privacy and security matters for more than 20 years.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪RAISE Act Immigration Reforms Touted As “Giving Americans A Raise”
▪Health Clinic At Houston Convention Center, Other HHS Help For Hurricane Harvey Victims
▪IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties
▪DB Plan Sponsors Check Out New Bifurcated Distribution Model Amendmentsy
▪U.S. News Names 2017-2018 “Best” Hospitals; Patient Usefulness Starts With Metholodogy Understanding
▪Use Lessons Of Past Mistakes or Injustice To Build Better Future
▪Prepare For Turnover, Other Challenges From Rising Workforce Competition
▪Employers, Health Plans Should Brace For Tightened Federal Mental Health Coverage Mandate Disclosure And Enforcement
▪Withholding Calculator Tool Helps Workers Figure Withholding
▪Better Preparing U.S. Workers To Fill Your Jobs
▪SCOTUS Ruling Bars Many State Arbitration Agreement Restrictions
▪$2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Dealing With HR, Benefits & Other Headaches From Equifax and Other Data Breach |
Comments Off on Dealing With HR, Benefits & Other Headaches From Equifax and Other Data Breach |  Banking, board of directors, Brokers, Civil Monetary Penalties, Claims, Claims Administration, compliance, conflict of interest, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, E-Verify, EBSA, Educational Privacy, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Tax, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, Form 5500, GINA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, Hiring, HR, Human Resources, I-9, Identity Theft, Income Tax, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, Internet, IRC, Labor Management Relations, Leadership, Management, Managment, Patient Empowerment, Payroll Tax, pension plan, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Risk Management, Security, Tax, Tax Credit, Tax Qualification, Technology, third party administrators, visas, Workforce | Tagged: ADA, Corporate Compliance, Data Breach, Employee Benefits, Employer, Employers, employment law, Equifax, ERISA, Health Care, Health Insurance, HIPAA, Human Resources, Insurance, Insurer, Labor Department, Privacy, Retirement Plans, Risk Management, Tax, Technology, wage and hour, Worker Classification |
Banking, board of directors, Brokers, Civil Monetary Penalties, Claims, Claims Administration, compliance, conflict of interest, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, E-Verify, EBSA, Educational Privacy, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Tax, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, Form 5500, GINA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, Hiring, HR, Human Resources, I-9, Identity Theft, Income Tax, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, Internet, IRC, Labor Management Relations, Leadership, Management, Managment, Patient Empowerment, Payroll Tax, pension plan, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Risk Management, Security, Tax, Tax Credit, Tax Qualification, Technology, third party administrators, visas, Workforce | Tagged: ADA, Corporate Compliance, Data Breach, Employee Benefits, Employer, Employers, employment law, Equifax, ERISA, Health Care, Health Insurance, HIPAA, Human Resources, Insurance, Insurer, Labor Department, Privacy, Retirement Plans, Risk Management, Tax, Technology, wage and hour, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 1, 2017
Employers and employee benefit plan fiduciaries and administrators should consider sharing the free IRS Withholding Calculator resource offered in English, Spanish, and ASL formats with workers in annual employee benefit enrollment packages, new hire paperwork, bonus announcement and other wage related materials and other employee communications to help workers better understand and manage the tax and other effects of their annual employee benefit elections on their take-home pay. Including reminders to re-evaluate withholding and if necessary, change their W-4 withholding elections also helps employees and their families ensure that withholding elections that workers complete as part of new hire documentation are updated in response to changing taxable income and other relevant events.
Communicating the availability of these free government-resource tools to workers during the annual employee benefit plan enrollment period, year-end, raise or bonus time or other strategic times throughout the year could help employees better appreciate the tax-preferred benefit offerings provided by the employer as well as provide significant financial education benefits many workers need for little or no employer cost.
While enrollment packages typically tout the potential “tax savings” that employees can enjoy from participating in tax-favored, employer-sponsored health, group term life, qualified pension or profit-sharing, and other tax-preferred employee benefit or fringe benefit programs offered by their employers, few employees truly understand how to determine properly their necessary wage withholding on taxable wages, much less the specific effects of their employee benefit elections on their income or employment tax liability or withholding.
A better understanding of the relative tax benefits and savings of enrollment in tax-preferred benefits offered by an employer and their potential implications on the income tax withholding elected by the workers can benefit both employees and their employer. Aside from illustrating in real, meaningful terms specific to the worker the tax benefits of his election of employer-offered, tax preferred benefits, proper tax withholding helps employees avoid unnecessary over withholding that can reduce employees’ take-home pay as well as helps protect employees from unexpectedly higher year-end tax bills that often surprise workers when an employee sets his withholding too low.
While few employers or plans want to incur the potential financial costs or liability of estimating savings for individual workers, sharing information about free government-provided resources like the IRS calculator or using vendor-provided solutions that incorporate tools in employee enrollment and other communications can help employees appreciate the benefits of tax-preferred employee benefits and make more informed choices about their benefits and their withholding.
Educating employees about the availability of these free resources also is a low-cost way of providing valuable information to workers whether or not the employer or plan has a vendor offered solution that includes the same or similar tool. However, educating workers about the availability of the withholding calculator and other tools can be a particularly attractive option for an employer when the employer doesn’t have a vendor-provided option that includes that information or can only access the tool for added charges.
While many vendors offer similar tools and materials sold to employers and employee benefit plans, employers or benefit plan fiduciaries generally must pay fees, share promotional materials or meet at the requirements to deliver those resources as part of a vendor-supplied package. Utilizing these vendor supplied resources without fulfilling these preconditions could expose the employer or plan to potential copyright, trademark or other contractual or intellectual property claims from the vendor. In contrast, IRS withholding calculator and many other government tools can be used or shared freely without these concerns. Moreover, employers and plans are less likely to face challenges for sharing an unfiltered government resource than a similar tool packaged within a vendor communication package promoting other options.
Of course, regardless of whether these or other tools or information are shared as a free-standing tool or as part of a broader communication package, employers, plans and others sharing these government tools and other similar resources generally will want to ensure that the materials are distributed along with and subject to general tax advice and other disclaimers of reliance as well as statements encouraging users to consult with their own qualified tax or other qualified professionals about the users’ specific circumstance.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |
Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |  105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |
105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 1, 2017
Heads up tax-exempt and governmental entities, employer and other qualified employee benefit plan sponsor, fiduciaries, administrators, and recordkeepers and their management, accountants, attorneys, and other service providers and advisors. Changes to the procedures that Internal Revenue Service (IRS) Tax Exempt and Government Entities TE/GE examiners use to make and enforce Information Document Request (IDR) in connection with an audit or other examination make it more important than ever that taxpayers use special care to collect, organize and maintain all of the data and documentation that examiners are likely to request in IDR and take other steps to prepare in advance to respond to an IDR.
New procedures announced in the February 27, 2017 Memorandum For All TE/GE Examiners On New Process For All Information Document Requests and scheduled to take effect April 1 seek to expedite the examination process and reduce backlogs. To accomplish this, the new procedures impose specific, tightened timelines for responding to IDRs and IRS follow and enforcement of data and document productions demanded by an IDR. As part of these changes, the new procedures shorten the time that the examiners will issue early subpoena warnings and subpoenas to compel taxpayers to produce requested data.
Taxpayers unable to respond in a timely fashion risk of both triggering these perilous enforcement procedures and an enhanced risk that IRS examiners will view the delay as an indication that the taxpayer may not be using the internal controls and processes expected by the IRS rules. Accordingly, taxpayers should seek advise from experienced legal counsel about the policies, practices, data and information they might be expected to need to respond to a IDR or other government investigation, recommendations for conducting their operations to promote their ability to efficiently assemble and produce the necessary data, records and other information to respond to a IDR or other investigation, audit or enforcement action, and other appropriate steps to position their organizations timely to recognize and produce the often substantial data generally demanded by an IRD and minimize risks of liability likely to arise from an IRS examination or other governmental or private investigation or action.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 28 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other employee benefit, insurance, technology and other highly regulated organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps these and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, current American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Compliance Chair of the National Kidney Foundation of North Texas, and Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, Ms. Stamer’s includes nearly 30 years’ of work with a diverse range of health industry clients on an extensive range of matters.
Ms. Stamer has worked closely with health industry, managed care and insurance, employee benefit, financial services, technology, restructuring, retail, hospitality, manufacturing, consulting, sales, energy, import-export, staffing and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of staffing, human resources and workforce performance management, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; JCHO and other accreditation and quality organizations; private litigation and other federal and state health care industry investigation, enforcement including insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others, and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns.
Best known for her thoughleadership and experience on health benefit and other health and insurance industy matters, Ms. Stamer has worked throughout her career health care, health benefit and insurance and health information technology, data and related process and systems development, policy and operations design, management, product development, innovation, administration, public policy, regulatory compliance, enforcement, contracting, privacy and data security and related matter. Ms. Stamer continuously advises health and insurance industry clients about licensing, regulatory compliance and internal controls, workforce, agent and broker and medical staff performance, claims and reimbursement, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Scribe for ABA JCEB annual agency meeting with OCR for many years, Ms. Stamer also is widely recognized for her extensive work and leadership on HIPAA, FACTA, PCI, IRC and other tax, Social Security, GLB, rade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and concerns including policy design, drafting, administration and training; business associate and other contracting; risk assessments, audits and other risk prevention and mitigation; investigation, reporting, mitigation and resolution of known or suspected breaches, violations or other incidents; and defending investigations or other actions by plaintiffs, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others. Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks, insurers and other financial institutions, and others on trade secret confidentiality, privacy, data security and other risk management and compliance including the design, establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR, FTC and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and enforcement, and a host of other related concerns.
Her clients include public and private health care providers, health insurers, health plans, employers, payroll, staffing, recruitment, insurance and financial services, technology and other vendors, and others. In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others. Ms. Stamer also has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use published by BNA, the ABA and other premier legal industy publishers.
Ms. Stamer also has extensive experience with a diverse array of other human resources and other staffing, services, outsourcing and other workforce, qualified and nonqualified employee benefit, compensation, and related matters, their design, documentation, administration, modification, enforcement and defense and other related operational, compliance and risk management. Her experience includes advising andassisting employer and other plan sponsors, fiduciaries, administrators, vendors and others with and program design, documentation and ongoing administration administration for compliance and defensibility under IRS and other federal and state tax, OFCCP, CAS, SCA, Davis Bacon, SEC and other corporate, ERISA and other federal and state labor and employment, SEC and other corporate, Department of Insurance and other laws and regulations; advising and assisting buyers, sellers, investors, debtors, creditors, trustees, plan fiduciaries and service providers and others in relation to business transactions, restructurings, bankruptcies and other substantial corporate and business events and transactions including significant work involving amendment, termination, windup and restructuring of employee benefit plans and workforce concerns in highly publicized fiduciary, securities or other misconduct investigation and enforcement, bankruptcy, restructuring or other distress situations.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy and governmental and regulatory affairs experience, Ms. Stamer also is widely recognized for regulatory and policy work, advocacy and outreach on healthcare, education, aging, disability, savings and retirement, workforce, ethics, and other policies. Throughout her adult life and career, Ms. Stamer has provided thought leadership; policy and program design, statutory and regulatory development design and analysis; drafted legislation, proposed regulations and other guidance, position statements and briefs, comments and other critical policy documents; advised, assisted and represented health care providers, health plans and insurers, employers, professional. and trade associations, community and government leaders and others on health care, health, pension and retirement, workers’ compensation, Social Security and other benefit, insurance and financial services, tax, workforce, aging and disability, immigration, privacy and data security and a host of other international and domestic federal, state and local public policy and regulatory reforms through her involvement and participation in numerous client engagements, founder and Executive Director of the Coalition for Responsible Health Policy and its PROJECT COPE: the Coalition on Patient Empowerment, adviser to the National Physicians Congress for Healthcare Policy, leadership involvement with the US-Mexico Chamber of Commerce, the Texas Association of Business, the ABA JCEB, Health Law, RPTE, Tax, Labor, TIPS, International Life Sciences, and other Sections and Committees, SHRM Governmental Affairs Committee and a host of other involvements and activities.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns. Her insights on these and other related matters appear in the Health Care Compliance Association, Atlantic Information Service, Bureau of National Affairs, The Wall Street Journal, Business Insurance, the Dallas Morning News, Modern Health Care, Managed Healthcare, Health Leaders, and a many other national and local publications. In addition to her many years of service as a scrivener for the ABA JCEB’s meeting with OCR, for instance, she also serves as Chair the Southern California ISSA Health Care Privacy & Security Summit, and an editorial advisory board member, author, program chair or steering committee member, and faculties for a multitude of other programs and publications regarding privacy, data security, technology and other compliance, risk management and operational concerns in the health care, health and other insurance, employee benefits and human resources, retail, financial services and other arenas.Ms. Stamer also shares her thought leadership, experience and advocacy on HIPAA and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association, Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Board Compliance Chair and Board member of the National Kidney Foundation of North Texas, current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Employers, Benefit Plans & Exempt Org: Prepare For Shortened Deadlines & Other Changes To IRS Employee Plan & Exempt Organization Exam Documentation Request Procedures |
Comments Off on Employers, Benefit Plans & Exempt Org: Prepare For Shortened Deadlines & Other Changes To IRS Employee Plan & Exempt Organization Exam Documentation Request Procedures |  401(k), Attorney-Client Privilege, board of directors, church plan, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, Employee Benefits, Employer, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Form 5500, HR, Human Resources, Internal Revenue Code, IRC, Pay, pension plan, Plan Admistrator, Retirements, Tax, Tax Qualification, third party administrators, Workforce | Tagged: 401(k), 457 plan, Employee Benefits, Exempt Organizations, IRS, retirement plan, tax exempt, tax qualification, TEGE |
401(k), Attorney-Client Privilege, board of directors, church plan, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, Employee Benefits, Employer, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Form 5500, HR, Human Resources, Internal Revenue Code, IRC, Pay, pension plan, Plan Admistrator, Retirements, Tax, Tax Qualification, third party administrators, Workforce | Tagged: 401(k), 457 plan, Employee Benefits, Exempt Organizations, IRS, retirement plan, tax exempt, tax qualification, TEGE |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 21, 2016
Employee benefit plans and tax-exempt organizations facing Internal Revenue Service (IRS) audits or investigations after April, 2016, their leaders and advisors should prepare for some changes in the practices IRS agents will use to issue and enforce document requests (IDRs) after March 31.
The IRS Tax Exempt and Government Entities Division (TEGE) just issued updated internal guidance (Guidance) governing the procedures its agents will use to gather information for employee benefit plan and exempt organization examinations including information requests made in connection with:
- Employee Benefit Form 5500 Examination Procedures
- Exempt Organizations Pre-Audit Procedures
- On-Site Examinations
- Tax Exempt Bonds Examinations
- Indian Tribal Government Examinations and
- Federal, State and Local Governments (FSLG) Examinations
The new Guidance follows other recent announcements of changes of IRS employee plan or exempt organization procedures such as recently announced changes in IRS employee plan correction procedures. See, e.g., IRS Qualified Plan Correction Procedures Changing 1/1/17.
The new procedures defined in the Guidance apply more broadly and take effect April 1, 2017. The Guidance also requires that TEGE update the following IRMs to specifically reflect the new procedures within the next two years:
- IRM 4.71.1, Overview of Form 5500 Examination Procedures;
- IRM 4.75.10, Exempt Organizations Pre-Audit Procedures;
- IRM 4.75.11, On-Site Examination Guidelines;
- IRM 4.81.5, Tax Exempt Bonds Examination Program Procedures – Conducting the Examination;
- IRM 4.86.5, Conducting Indian Tribal Government Examinations; and
- IRM 4.90.9, Federal, State and Local Governments (FSLG) – Procedures, Workpapers and Report Writing.
Among other things, the new Guidance will require “active involvement” by managers of IRS examiners’ early in the process. The Guidance also calls for:
- Taxpayers to be involved in the IDR process.
- Examiners to discuss the issue being examined and the information needed with the taxpayer prior to issuing an IDR.
- Examiners to ensure that the IDR clearly states the issue and the relevant information they are requesting.
- If the taxpayer does not timely provide the information requested in the IDR by the agreed upon date, including extensions, examiners to issue a delinquency notice.
- If the taxpayer fails to respond to the delinquency notice or provides an incomplete response, for the examiner to issue a pre-summons notice to advise the taxpayer that the IRS will issue a summons unless the missing items are fully provided.
- For a summons to be issued if the taxpayer fails to provide a complete response to the pre-summons letter by its response due date.
According to TEGE the new procedures set forth in the Guidance are designed to “ensure” that IRS Counsel is prepared to enforce IDRs through the issuance of a summons when necessary while also reinforcing the IRS’ commitment to the respect of taxpayer rights under the Taxpayer Bill of Rights. TEGE says the updated procedures established in the Guidance will promote these goals by:
- Providing for open and meaningful communication between the IRS and taxpayers;
- Reducing taxpayer burdens
- Providing for consistent treatment of taxpayers;
- Allowing the IRS to secure more complete and timely responses to IDRs;
- Providing consistent timelines for IRS agents to review IDR responses; and
- Promoting timely issue resolution.
While it remains to be seen exactly how well the new procedures will promote these goals in operation, leaders, sponsors, administrators and tax advisors to employee benefit plans and exempt organizations tagged for audits after the Guidelines take effect will want to ensure that they review and fully understand the new procedures as soon as possible after receiving notice of the audit.
A clear understanding of the procedures can help the entities and their representatives to take advantage of all available options for mitigating exposures and liability from the audit as well as to avoid unfortunate missteps that could result in forfeiture of otherwise available tax-related rights and options or otherwise increase the tax and other associated risks and liabilities of the entities or others associated with them arising from the audit.
Along with responding to these tax-related risks, leaders and advisors of employee benefit plan and exempt organizations also need to keep in mind the often substantial non-tax related risks that may arise concurrently or evolve from a TEGE or other tax-related audit or investigation. The often substantial tax and non-tax exposures typically makes it desirable if not necessary to involve experienced legal counsel in the process as soon as possible.
To help respond to the audit and manage its tax and non-tax related risks and, leaders responsible for these entities generally not only will want to seek legal advice within the scope of attorney-client privilege from legal counsel immediately after receiving an IDR or other notice of an audit or investigation, as well as consider periodically consulting experienced legal counsel for assistance in conducting pre-audit assessment of compliance and other compliance and risk management planning.
Early involvement of legal counsel generally is necessary both to understand and manage both the tax and non-tax exposures associated with the audit, as well as to preserve and utilize the potential benefits of attorney-client privilege and other evidentiary privileges that could help to mitigate both the tax and non-tax related risks. While federal tax rules afford some evidentiary privileges to certain accounting professionals when providing tax representation or advice, the protective scope of such privileges generally are more limited than attorney-client privilege and work product evidentiary privileges and typically do not apply to non-tax matters. As a result, most entities and their leaders will want to consider involvement of legal counsel to maximize privilege protections and non-tax related exposures even if the parties plan for a qualified tax professional or other consultant to play a significant role in assisting them to prepare for and respond to the audit.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with health industry and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein
©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on IRS Changing Employee Plans & Exempt Organization Audit Procedures |
Comments Off on IRS Changing Employee Plans & Exempt Organization Audit Procedures |  105(h), 401(k), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, COBRA, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health reform, HR, Human Resources, Identity Theft, Income Tax, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Pay, Payroll Tax, pension plan, Plan Admistrator, Tax, Tax Credit, Tax Qualification, Uncategorized |
105(h), 401(k), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, COBRA, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health reform, HR, Human Resources, Identity Theft, Income Tax, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Pay, Payroll Tax, pension plan, Plan Admistrator, Tax, Tax Credit, Tax Qualification, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 13, 2016
Employers and other plan sponsors of tax-qualified 401(k) and other defined contribution or defined benefit plans (retirement plans) and others working to avoid plan disqualification by correcting plan documentation, administration or other problems that otherwise could disqualify their program for tax qualified treatment under the Internal Revenue Code (Code) under the Internal Revenue Service (IRS) Employee Plans Compliance Resolution System (EPCRS) or the Audit Closing Agreement Program (Audit CAP) modified rules beginning January 1, 2017, under changes announced by the IRS in Revenue Procedure 2016-51 on September 29, 2016.
The EPCRS and Audit CAP programs are two IRS correction programs commonly used to preserve the tax qualified status of a retirement plan affected by plan documentation, administration or other deficiencies that otherwise would result in the plan ceasing to qualify as a tax retirement plan under the Code. The EPCRS program generally is available to correct and resolve certain qualification concerns not eligible for self-correction that retirement plan sponsors or plans self-identify and disclose to the IRS in accordance with the EPCRS correction procedures, In contrast, the Audit CAP program provides an avenue that may provide a pathway for a plan sponsor of a retirement plan with significant problems in its compliance with the Code’s qualification requirements that are discovered by the IRS on audit or during the determination letter application process to preserve the tax benefits associated with maintaining a retirement plan in compliance with the Code’s tax qualification requirements by entering into a Closing Agreement pursuant to which the problems are corrected and paying a reasonable sanction to the IRS based directly on the amount of tax benefits preserved and the nature, extent and severity of the failure, taking into account the extent to which correction occurred before audit.
Key changes to the EPCRS correction procedures scheduled to take effect on January 1, 2017 under Revenue Procedure 2016-51 include the following:
- The IRS no longer will permit determination letter applications when applying the correction programs under EPCRS;
- The requirement for a plan sponsor to submit a determination letter application to the IRS when correcting qualification failures that include a plan amendment no longer will apply; and
- Fees associated with the Voluntary Correction Program (VCP) after December 31, 2017 will be user fees and no longer set forth in the EPCRS revenue procedure. For VCP submissions made in 2016, refer to Proc. 2016-8 and Rev. Proc. 2013-12 to determine the applicable user fee and after 2016, refer to the annual Employee Plans user fees revenue procedure to determine VCP user fees for that year. Availability of Self-Correction Program (SCP) for significant failures has been modified to provide that, for qualified individually designed plans, a determination letter need not be current to satisfy the Favorable Letter requirement
In addition to its announcements of changes to the EPCRS correction program Revenue Procedures 2016-51 also announces various modifications to the Audit CAP program, including:
- A revised approach to determining Audit CAP sanctions under which
- Sanctions, generally, will not be less than the fees associated with voluntary compliance under the EPCRS program;
- The required reasonable sanction will no longer be a negotiated percentage of the maximum payment amount (MPA). Instead, auditors will review facts and circumstances and the MPA amount is simply one factor to consider. In addition, there are revised, additional factors that IRS considers;
- New factors used in determining sanctions for late amender failures will apply;
- For late amender failures discovered by the IRS, while reviewing a determination letter application, a new approach to determining the applicable sanction will apply;
- The IRS will not provide partial refunds for certain Anonymous Submissions
Beyond specific modifications to the EPCRS and Audit CAP procedures, Revenue Procedures 2016-51 also:
- Updates citations and cross-references for several items previously contained in Rev. Proc. 2013-12; and
- Invites public comments on recovery of overpayments and on expanding EPCRS correction rules to provide additional guidance on the recovery or recoupment of overpayments.
Revenue Procedures 2016-51 is effective January 1, 2017. Plan sponsors may not elect to apply provisions before January 1, 2017. Rev. Proc. 2013-12, as modified by Rev. Proc. 2015-27 and Rev. Proc. 2015-28, are in effect for 2016. When Revenue Procedure 2016-51 takes effect on January 1, 2017:
- Proc. 2013-12 no longer applies as of January 1, 2017; and
- Provisions of Rev. Proc. 2015-27 and Rev. Proc. 2015-28 concerning EPCRS and other older revenue procedures will no longer apply.
About The Author
Cynthia Marcotte Stamer is a noted Texas-based management lawyer and consultant, author, lecture and policy advocate, recognized for her nearly 30-years of cutting edge management work as among the “Top Rated Labor & Employment Lawyers in Texas” by LexisNexis® Martindale-Hubbell® and as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,”“Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Group Chair and current Defined Contribution Plans Committee Co-Chair, Groups and Substantive Committee and Membership Committee Members, past Welfare Plans Committee Chair and Co-Chair, and former Fiduciary Responsibility Vice Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current ABA International Section Life Sciences Committee Vice Chair, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, former ABA Joint Committee on Employee Benefits Council Representative and Marketing Committee Chair and a prolific author and highly popular speaker and consultant, Ms. Stamer helps management manage.
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
For additional information about this topic or Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal control and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at http://www.Solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. ©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
 Comments Off on IRS Qualified Plan Correction Procedures Changing 1/1/17 |
Comments Off on IRS Qualified Plan Correction Procedures Changing 1/1/17 |  401(k), compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employer, Employers, Employment, ERISA, IRC, Retirement Plans, Uncategorized | Tagged: 401(k), Audits, Compensation, defined benefit plan, defined contribution plan, employee benefit plan, Employee Benefits, E{CRS, Plan Audits, plan qualification, Qualified Plan, Tax |
401(k), compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Employee Benefits, Employer, Employers, Employment, ERISA, IRC, Retirement Plans, Uncategorized | Tagged: 401(k), Audits, Compensation, defined benefit plan, defined contribution plan, employee benefit plan, Employee Benefits, E{CRS, Plan Audits, plan qualification, Qualified Plan, Tax |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 11, 2015
Health plans, insurers and other health plan industry service providers widespread use and reliance on internet applications to access and share protected health information when performing online enrollment, claims administration and payment, reporting, member and provider communications and a host of other key health plan functions makes it particularly important for health plans, their employer or other sponsors, fiduciaries, insurers and other vendors and their management to respond quickly to a warning from Department of Health & Human Services (HHS) Office of Civil Rights (OCR) warning to ensure applications and systems properly safeguard protected health information (PHI) as required by the Health Insurance Portability & Accountability (HIPAA) Privacy, Security & Breach Notification Rules (HIPAA Rules) and other laws made in its July 10, 2015 announcement of its latest HIPAA settlement.
The new Resolution Agreement with the Massachusetts based hospital system, St. Elizabeth’s Medical Center (SEMC) settles charges OCR made that SEMC reached HIPAA by failing to protect the security of PHI when using internet applications to access and share PHI. The Resolution Agreement also shows how complaints filed with OCR by workforce members can create additional compliance headaches for Covered Entities or their business associates while the “robust corrective action plan” imposed under the Resolution Agreement shares examples of ladder reporting and management oversight and documentation Covered Entities and business associates can expect to need to prove their organizations maintains the “culture of compliance” with HIPAA OCR expects in the event of an OCR audit or investigation.
With recent reports on massive health plan HIPAA and other data breaches fueling widespread participant and regulatory concern over identity theft and other data security, Covered Entities and their business associates should prepare to defend the adequacy of their own HIPAA and other data security practices in the event of an OCR breach investigation or audit. Accordingly, health plans and their employer or other sponsors, health plan fiduciaries, health plan vendors acting as business associates and others dealing with health plans and their management should contact legal counsel experienced in these matters for advice within the scope of attorney-client privilege about how to respond to the OCR warning and other developments to manage their HIPAA and other privacy and data security legal and operational risks and liabilities.
SEMC Resolution Agreement Overview
The SEMC Resolution Agreement settles OCR charges that SEMC violated HIPAA stemming from an OCR investigation of a November 16, 2012 complaint by SEMC workforce members and a separate data breach report SEMC separately made to OCR of a breach of unsecured electronic PHI (ePHI) stored on a former SEMC workforce member’s personal laptop and USB flash drive affecting 595 individuals. In their complaint, SEMC workers complained SEMC violated HIPAA by allowing workforce members to use an internet-based document sharing application to share and store documents containing electronic protected health information (ePHI) of at least 498 individuals without adequately analyzing the risks. OCR says its investigation of the complaint and breach report revealed among other things that:
- SEMC improperly disclosed the PHI of at least 1,093 individuals;
- SEMC failed to implement sufficient security measures regarding the transmission of and storage of ePHI to reduce risks and vulnerabilities to a reasonable and appropriate level; and
- SEMC failed to timely identify and respond to a known security incident, mitigate the harmful effects of the security incident, and document the security incident and its outcome.
To resolve OCR’s charges, SMCS agreed to pay $218,400 to OCR and implement a “robust corrective action plan” to correct these alleged HIPAA violations. While the required settlement payment is relatively small, the Resolution Agreement’s focus security requirements for internet application and data use and sharing activities engaged in by virtually every Covered Entity and business associate make the Resolution Agreement merit the immediate attention of all Covered Entities, their business associates and their management.
SEMC HIPAA Specific Compliance Lessons For Health Plans & Business Associates
In announcing the Resolution Agreement, OCR Director Jocelyn Samuels sent a clear warning to all Covered Entities and their business associates “to pay particular attention to HIPAA’s requirements when using internet-based document sharing applications,” stating “In order to reduce potential risks and vulnerabilities, all workforce members must follow all policies and procedures, and entities must ensure that incidents are reported and mitigated in a timely manner.”
The Resolution Agreement makes clear that OCR expects health plans and other Covered Entities and their business associates to be able to show both their timely investigation of reported or suspected HIPAA susceptibilities or violations as well as to self-audit and spot test HIPAA compliance in their operations. The SEMC corrective action plan also indicates Covered Entities and business associates must be able to produce documentation and other evidence needed to show the top to bottom dedication to HIPAA compliance necessary to prove a “culture of compliance” with HIPAA permeates their organizations.
In light of OCR’s warning and expectations, Covered Entities and business associates should start by considering the advisability for their own organization to take one or more of the steps outlined in the “robust corrective action plan” included in the Resolution Agreement, starting with the specific steps the corrective action plan requires SEMC to address its internet application security concerns such as:
- Conducting self-audits and spot checks of workforce members’ familiarity and compliance with HIPAA policies and procedures on transmitting ePHI using unauthorized networks; storing ePHI on unauthorized information systems, including unsecured networks and devices; removal of ePHI from SEMC; prohibition on sharing accounts and passwords for ePHI access or storage; encryption of portable devices that access or store ePHI; security incident reporting related to ePHI; and
- Inspecting laptops, smartphones, storage media and other portable devices, workstations and other devices containing ePHI and other data devices and systems and their use; and
- Conducting other tests and audits of security and compliance with policies, processes and procedures; and
- Documenting results, findings, and corrective actions including appropriate up the ladder reporting and management oversight of these and other HIPAA compliance expectations, training and other efforts.
Broader HIPAA Compliance & Risk Management Lessons
Beyond the specific internet applications and other security of ePHI lessons in the Resolution Agreement, Covered Entities and their business associates also should be mindful of other more subtle, but equally important broader HIPAA compliance and risk management lessons provided in the Resolution Agreement and other recent OCR guidance about their overall HIPAA compliance responsibilities.
One of the most significant of these lessons is the need for proper workforce training, oversight and management. The Resolution Agreement sends an undeniable message that OCR expects Covered Entities, business associates and their leaders to be able to show their effective oversight and management of the operational compliance of their systems and members of their workforce with HIPAA policies. The SEMC corrective action plan should prompt Covered Entities and business associates to weigh the adequacy of their existing workforce training, reporting, investigation and other management processes and documentation. Meanwhile, OCR’s report that an OCR complaint made by SEMC insiders to OCR prompted its investigation also should sensitize Covered Entities and their business associates of the need to ensure that their workforce training and management processes are appropriate to position their organization both to show their processes encourage proper internal reporting and investigation of compliance concerns, as well as manage the inevitable HIPAA and other human resources retaliation and whistleblower exposures that can arise out of such reports.
The Resolution Agreement also provides insights to the internal corporate processes and documentation of compliance efforts that Covered Entities and business associates may need to show their organization has the required “culture of compliance” needed to mitigate consequences of breaches or other compliance glitches. Particularly notable are Resolution Agreement’s terms on the documentation and up the ladder reporting to management and OCR of SEMC’s self-audit and self-correction activities and management oversight and management of these activities. Like tips shared by HHS in the recently released Practical Guidance for Health Care Governing Boards on Compliance Oversight, these details in the Resolution Agreement provide invaluable tips to Boards and other leaders of Covered Entities and business associates about steps they can take to promote their ability to demonstrate their organizations have the necessary culture of HIPAA compliance OCR expects.
Health Plan HIPAA Compliance Risks & Responsibilities of Employers & Their Leaders
While HIPAA places the primary duty for complying with HIPAA on Covered Entities and business associates, health plan sponsors and their management still need to make HIPAA compliance a priority for many practical and legal reasons.
As employers forced to cope with the deluge of fears and questions of employees and other health plan members impacted by recent massive PHI breach reports shared by Blue Cross association health insurance plan giants, Anthem and Premera can attest, HIPAA data breach or other compliance reports often trigger significant financial, administrative, workforce satisfaction and other operational costs employer health plan sponsors. Inevitable employee concern about health plan data breaches undermines employee value and satisfaction of the health benefit plan as an employee benefit. These concerns also usually require employers to expend significant management and financial resources to respond to these concerns and address other employer fallout from the breach.
The costs of investigation and redress of a known or suspected HIPAA data or other breach typically far exceed the actual damages to participants resulting from the breach. While HIPAA technically does not make sponsoring employers directly responsible for these duties or the costs of their performance, as a practical matter sponsoring employers typically can expect to pay costs and other expenses that its health plan incurs to investigate and redress a HIPAA breach. For one thing, except in the all too rare circumstances where employers as plan sponsors have specifically negotiated more favorable indemnification and liability provisions in their vendor contracts, employer and other health plan sponsors usually agree in their health plan vendor contracts to pay the expenses and to indemnify health plan insurers, third party administrators, and other vendors for costs and liabilities arising from HIPAA breaches or other events arising in the course of the administration of the health plan. Since employers typically are obligated to pay health plan costs in excess of participant contributions, employers also typically would be required to provide the funding their health plan needs to cover these costs even in the absence of such indemnification agreements.
Sponsoring employers and their management also should be aware the employer’s exception from direct liability for HIPAA Rule compliance does not fully insulate the employer or its management from legal risks in the event of a health plan data breach or other HIPAA violation.
While HIPAA generally limits direct responsibility for compliance with the HIPAA Rules to a health plan or other Covered Entity and their business associates, HIPAA hybrid entity and other organizational rules and criminal provisions of HIPAA, as well as various other federal laws arguably could create liability risks for the employer. See, e.g., Cyber Liability, Healthcare: Healthcare Breaches: How to Respond; Restated HIPAA Regulations Require Health Plans to Tighten Privacy Policies and Practices; Cybercrime and Identity Theft: Health Information Security Beyond. For example, hybrid entity and other organizational provisions in the HIPAA Rules generally require employers and their health plan to ensure that health plan operations are appropriately distinguished from other employer operations in order for otherwise non-covered human resources, accounting or other employer activities to avoid subjecting their otherwise non-covered employer operations and data to HIPAA Rules. To achieve this required designation and separation, the HIPAA rules typically also require that the health plan include specific HIPAA language and the employer and health plan take appropriate steps to designate and separate health plan records and data, workforces, and operations from the non-covered business operations and records of the sponsoring employer. Failure to fulfill these requirements could result in the unintended spread of HIPAA restrictions and liabilities to other aspects of the employer’s human resources or other operations. Sponsoring employers will want to confirm that health plan and other operations and workforces are properly designated, distinguished and separated to reduce this risk.
When putting these designations and separations in place, employers also generally will want to make arrangements to ensure that their health plan includes the necessary terms and the employer implements the policies necessary for the employer to provide the certifications to the health plan that HIPAA will require that the health plan receive before HIPAA will allow health plan PHI to disclosed to the employer or its representative for the limited underwriting and other specified plan administration purposes permitted by the HIPAA Rules.
Once these arrangements are in place, employers and their management also generally will want to take steps to minimize the risk that their organization or a member of the employer’s workforce honors these arrangements and does not improperly access or use health plan PHI, systems in violation of these conditions or other HIPAA Rules. This or other wrongful use or access of health plan PHI or systems could violate criminal provisions of HIPAA or other federal laws making it a crime for any person – including the employer or a member of its workforce – from wrongfully accessing health plan PHI, electronic records or systems. Since health plan PHI records also typically include personal tax, social security information that the Internal Revenue Code, the Social Security Act and other federal laws generally would require the employer to keep confidential and to protect against improper use, employers and their management also generally should be concern about potential exposures for their organization that could result from improper use or access of this information in violation of these other federal laws. Since HIPAA and some of these other laws under certain conditions make it a felony crime to violate these rules, employer and their management generally will want to treat compliance with these federal rules as critical elements of the employer’s Federal Sentencing Guideline and other compliance programs.
Beyond the already discussed concerns, employers or members of their management also may have an incentive to promote health plan compliance with HIPAA or other health plan privacy or data security requirements to many the exposure of the employer or management or other staff to statutory, regulatory, contractual or ethical liabilities arising under ERISA, Internal Revenue Code, the Fair & Accurate Credit Transaction Act (FACTA), trade secret, insurance, disability, identity theft, cybersecurity or other federal or state laws.
For instance, health plan sponsors and management involved in health plan decisions, administration or oversight could face personal fiduciary liability risks under ERISA for failing to act prudently to ensure that the health plan compliance with HIPAA and other federal privacy and data security requirements.. ERISA’s broad functional fiduciary definition encompasses both persons and entities appointed as “named” fiduciaries and others who functionally exercise discretion or control over a plan or its administration. Consequently, the sponsoring employer and certain members of its human resources or other executive management team who functionally possess or exercise responsibility or authority over the administration of the employer’s health plan or its data or other assets, the selection or oversight of plan fiduciaries, vendors, or other workforce members its administration, or other key health plan operations risk ERISA fiduciary liability for their own failures to act prudently in carrying out HIPAA compliance or other responsibilities or to take action when they know or should know that another fiduciary is or has breached these duties. This fiduciary status and risk can occur even if the entity or individual does not is not named a named fiduciary, expressly disclaims fiduciary responsibility or does not realize it bears fiduciary status or responsibility. Since fiduciaries generally bear personal liability for their own breaches of fiduciary duty as well as potential co-fiduciary liability for fiduciary breaches committed by others that they knew or prudently should have known, most employers and members of their management will make HIPAA health plan compliance a priority to avoid or minimize these potential ERISA fiduciary exposures.
Furthermore, most employers and their management also will appreciate the desirability of taking reasonable steps to manage potential exposures that the employer or members of its management could face if their health plan or the employer violates the anti-retaliation rules of HIPAA or other laws through the adoption and administration of appropriate human resources, internal investigation and reporting, risk management policies and practices. See Employee & Other Whistleblower Complaints Common Source of HIPAA Privacy & Other Complaints.
Act To Manage HIPAA & Other Related Risks
OCR’s release of the Resolution Agreement on the heels of widespread publicity about massive health plan and other data breaches at Blue Cross health care giants, Anthem and Premera and other U.S. businesses and the potential legal and financial exposures that a HIPAA data breach or other violation could create, health plans and their sponsors, insurers, business associates, and leaders should appreciate the advisability of acting promptly to ensure that their health plans and business associates are taking appropriate steps to comply with the HIPAA Rules and manage other associated risks and liabilities. At minimum, health plans and their business associates should move quickly to conduct a documented assessment of the adequacy of their health plan internet applications and other HIPAA compliance in in light of the Resolution Agreement and other developments. Given the scope and diversity of the legal responsibilities, risks and exposures associated with this analysis, most health plan sponsors, fiduciaries, business associates and their management also will want to consider taking other steps to mitigate various other legal and operational risks that lax protection or use of health plan PHI or systems could create for their health plan, its sponsors, fiduciaries, business associates and their management. Health plan fiduciaries, sponsors and business associates and their leaders also generally will want to explore options to use indemnification agreements, liability insurance or other risk management tools as a stop gap against the costs of investigation or defense of a HIPAA security or other data breach.
For Legal or Consulting Advice, Legal Representation, Training Or More Information
If you need help responding to these new or other workforce, benefits and compensation, performance and risk management, compliance, enforcement or management concerns, help updating or defending your workforce or employee benefit policies or practices, or other related assistance, the author of this update, attorney Cynthia Marcotte Stamer may be able to help.
A practicing attorney and Managing Shareholder of Cynthia Marcotte Stamer, P.C., a member of Stamer│Chadwick │Soefje PLLC, Ms. Stamer’s more than 27 years’ of leading edge work as an practicing attorney, author, lecturer and industry and policy thought leader have resulted in her recognition as a “Top” attorney in employee benefits, labor and employment and health care law.
Board certified in labor and employment law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, former Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, an ABA Joint Committee on Employee Benefits Council Representative and Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, Ms. Stamer is recognized nationally and internationally for her practical and creative insights and leadership on HIPAA and other health and other employee benefit, human resources, and related insurance, health care, privacy and data security and tax matters and policy.
Ms. Stamer’s legal and management consulting work throughout her 27 plus year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce management operations and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well known for her extensive work with health care, insurance and other highly regulated entities on corporate compliance, internal controls and risk management, her clients range from highly regulated entities like employers, contractors and their employee benefit plans, their sponsors, management, administrators, insurers, fiduciaries and advisors, technology and data service providers, health care, managed care and insurance, financial services, government contractors and government entities, as well as retail, manufacturing, construction, consulting and a host of other domestic and international businesses of all types and sizes.
As a key part of this work, Ms. Stamer uses her deep and highly specialized health, insurance, labor and employment and other knowledge and experience to help employers and other employee benefit plan sponsors; health, pension and other employee benefit plans, their fiduciaries, administrators and service providers, insurers, and others design legally compliant, effective compensation, health and other welfare benefit and insurance, severance, pension and deferred compensation, private exchanges, cafeteria plan and other employee benefit, fringe benefit, salary and hourly compensation, bonus and other incentive compensation and related programs, products and arrangements.
She is particularly recognized for her leading edge work, thought leadership and knowledgeable advice and representation on the design, documentation, administration, regulation and defense of a diverse range of self-insured and insured health and welfare benefit plans including private exchange and other health benefit choices, health care reimbursement and other “defined contribution” limited benefit, 24-hour and other occupational and non-occupational injury and accident, ex-patriate and medical tourism, onsite medical, wellness and other medical plans and insurance benefit programs as well as a diverse range of other qualified and nonqualified retirement and deferred compensation, severance and other employee benefits and compensation, insurance and savings plans, programs, products, services and activities. In these and other engagements, Ms. Stamer works closely with employer and other plan sponsors, insurance and financial services companies, plan fiduciaries, administrators, and vendors and others to design, administer and defend effective legally defensible employee benefits and compensation practices, programs, products and technology. She also continuously helps employers, insurers, administrative and other service providers, their officers, directors and others to manage fiduciary and other risks of sponsorship or involvement with these and other benefit and compensation arrangements and to defend and mitigate liability and other risks from benefit and liability claims including fiduciary, benefit and other claims, audits, and litigation brought by the Labor Department, IRS, HHS, participants and beneficiaries, service providers, and others. She also assists debtors, creditors, bankruptcy trustees and others assess, manage and resolve labor and employment, employee benefits and insurance, payroll and other compensation related concerns arising from reductions in force or other terminations, mergers, acquisitions, bankruptcies and other business transactions including extensive experience with multiple, high-profile large scale bankruptcies resulting in ERISA, tax, corporate and securities and other litigation or enforcement actions.
In the course of this work, Ms. Stamer has accumulated an impressive resume of experience advising and representing clients on HIPAA and other privacy and data security concerns. The scribe for the American Bar Association (ABA) Joint Committee on Employee Benefits annual agency meeting with the Department of Health & Human Services Office of Civil Rights for several years, Ms. Stamer has worked extensively with health plans, health care providers, health care clearinghouses, their business associates, employer and other sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA and other information privacy and data security rules, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and enforcement, and a host of other related concerns. Her clients include public and private health plans, health insurers, health care providers, banking, technology and other vendors, and others. Beyond advising these and other clients on privacy and data security compliance, risk management, investigations and data breach response and remediation, Ms. Stamer also advises and represents clients on OCR and other HHS, Department of Labor, IRS, FTC, DOD and other health care industry investigation, enforcement and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns. She also is the author of numerous highly acclaimed publications, workshops and tools for HIPAA or other compliance including training programs on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
Ms. Stamer also is deeply involved in helping to influence the Affordable Care Act and other health care, pension, social security, workforce, insurance and other policies critical to the workforce, benefits, and compensation practices and other key aspects of a broad range of businesses and their operations. She both helps her clients respond to and resolve emerging regulations and laws, government investigations and enforcement actions and helps them shape the rules through dealings with Congress and other legislatures, regulators and government officials domestically and internationally. A former lead consultant to the Government of Bolivia on its Social Security reform law and most recognized for her leadership on U.S. health and pension, wage and hour, tax, education and immigration policy reform, Ms. Stamer works with U.S. and foreign businesses, governments, trade associations, and others on workforce, social security and severance, health care, immigration, privacy and data security, tax, ethics and other laws and regulations. Founder and Executive Director of the Coalition for Responsible Healthcare Policy and its PROJECT COPE: the Coalition on Patient Empowerment and a Fellow in the American Bar Foundation and State Bar of Texas. She also works as a policy advisor and advocate to health plans, their sponsors, administrators, insurers and many other business, professional and civic organizations.
Author of the thousands of publications and workshops these and other employment, employee benefits, health care, insurance, workforce and other management matters, Ms. Stamer also is a highly sought out speaker and industry thought leader known for empowering audiences and readers. Ms. Stamer’s insights on employee benefits, insurance, health care and workforce matters in Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, Modern Healthcare, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications. Ms. Stamer also regularly serves on the faculty and planning committees for symposia of LexisNexis, the American Bar Association, ALIABA, the Society of Employee Benefits Administrators, the American Law Institute, ISSA, HIMMs, and many other prominent educational and training organizations and conducts training and speaks on these and other management, compliance and public policy concerns.
Ms. Stamer also is active in the leadership of a broad range of other professional and civic organizations. For instance, Ms. Stamer presently serves on an American Bar Association (ABA) Joint Committee on Employee Benefits Council representative; Vice President of the North Texas Healthcare Compliance Professionals Association; Immediate Past Chair of the ABA RPTE Employee Benefits & Other Compensation Committee, its current Welfare Benefit Plans Committee Co-Chair, on its Substantive Groups & Committee and its incoming Defined Contribution Plan Committee Chair and Practice Management Vice Chair; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; current Vice Chair of the ABA TIPS Employee Benefit Committee; the former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division; on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. She also previously served as a founding Board Member and President of the Alliance for Healthcare Excellence, as a Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; the Board President of the early childhood development intervention agency, The Richardson Development Center for Children; Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a member of the Board of Directors of the Southwest Benefits Association. For additional information about Ms. Stamer, see www.cynthiastamer.com, or http://www.stamerchadwicksoefje.com the member of contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also may be interested reviewing other Solutions Law Press, Inc.™ resources at www.solutionslawpress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile at here.
©2015 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on HIPAA Settlement Warns Health Plans, Sponsoring Employers & Business Associates To Manage HIPAA Risks |
Comments Off on HIPAA Settlement Warns Health Plans, Sponsoring Employers & Business Associates To Manage HIPAA Risks |  105(h), ADA, ARRA, Cafeteria Plans, Civil Rights, Claims Administration, Corporate Compliance, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, GINA, Government Contractors, Health Plans, HIPAA, Human Resources, Mental Health, MEWA, Retaliation, Risk Management | Tagged: Breach Notification, Data Breach, Employer, ERISA, Federal Sentencing Guidelines, Fiduciary Duties, Health Plans, HIPAA, Privacy, Risk Managemnet |
105(h), ADA, ARRA, Cafeteria Plans, Civil Rights, Claims Administration, Corporate Compliance, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, GINA, Government Contractors, Health Plans, HIPAA, Human Resources, Mental Health, MEWA, Retaliation, Risk Management | Tagged: Breach Notification, Data Breach, Employer, ERISA, Federal Sentencing Guidelines, Fiduciary Duties, Health Plans, HIPAA, Privacy, Risk Managemnet |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 10, 2014
Human resources and other management leaders are watching Washington to see if the change in Congressional control resulting from the November 4, 2014 mid-term election ushers in a more management friendly federal legal environment. Since President Obama took office, the Democrats aggressive pursuit of health care, minimum wage and other federal pro-labor legislation, regulations and enforcement has increased management responsibilities, costs and liabilities.
Nationally recognized management attorney, public policy advisor and advocate, author and lecturer Cynthia Marcotte Stamer will help human resources and other management leaders prepare for 2015 when she speaks on “2015 Federal Legislative, Regulatory & Enforcement Update: What HR & Benefit Leaders Should Expect & Do Now” at the 2015 Dallas HR monthly luncheon series kickoff meeting on January 13, 2014.
About The Program
While November 4, 2014 Republican election victories gave Republicans a narrow majority in both the House and Senate when the new Congress takes office January 3, 2015, the new Republican Majority may face significant challenges delivering on their promises to move quickly to enact more business-friendly health care, guest worker, tax and other key reforms Republicans say will boost the employment and the economy.
While President Obama and Democrat Congressional leaders say they plan to work with the new majority, President Obama already is threatening to use vetoes, regulations and executive orders to block Republicans from obstructing or rolling back his pro-labor policy and enforcement agenda. When the new Congress takes office, the narrowness of the Republican Majority in the Senate means Republicans can’t block a Democratic filibuster or override a Presidential veto without recruiting some Democratic support.
As the Democrats and Republicans head into battle again, Board Certified Labor & Employment attorney and public policy advocate Cynthia Marcotte Stamer will help human resources and other management leaders get oriented for the year ahead by sharing her insights and predictions on the legislative, regulatory and enforcement agendas that HR, benefit and other business leaders need to plan for and watch in 2015. Among other things, Ms. Stamer will:
- Discuss how management can benefit from monitoring and working to influence potential legislative, regulatory and enforcement developments when planning and administering HR and related workforce policies;
- Discuss the key workforce and other legislative, regulatory and enforcement priorities and proposals Democrats and Republicans plan to pursue during 2015;
- Share her insights and predictions about how the narrow Republican majority, Mr. Obama’s lame duck presidency and other factors could impact each Party’s ability to pursue its agenda
- Share tips management leaders can use to help monitor developments and to help shape legislation, regulation and enforcement through Dallas HR, SHRM and other organizations as well as individually;
- Learn tips for anticipating and maintaining flexibility to respond to legislative, regulatory and enforcement developments; and
- More
To register or get more details about the program, DallasHR, or both, see http://www.dallashr.org.
About Ms. Stamer
Board certified labor and employment attorney, public policy leader, author, speaker Cynthia Marcotte Stamer is nationally and internationally recognized and valued for her more than 25 years of work advising and representing employers, insurers, employee benefit plans, their fiduciaries and advisors, business and community leaders and governments about workforce, employee benefits, social security and pension, health and insurance, immigration and other performance and risk management, public policy and related regulatory and public policy, management and other operational concerns.
Throughout her career, Ms. Stamer continuously both has helped businesses and their management to monitor and respond to federal and state legislative, regulatory and enforcement concerns and to anticipate and shape federal, state and other laws, regulations, and enforcement in the United States and internationally.
Well known for her leadership on workforce, health and pension policy through her extensive work with clients as well as through her high profile involvements as the Founder and Executive Director of the Coalition for Responsible Healthcare Policy and its PROJECT COPE: the Coalition on Patient Empowerment, a founding Board member of the Alliance for Health Care Excellence, a Fellow in the American College of Employee Benefit Counsel, the American Bar Association (ABA), and the State Bar of Texas leadership and other involvements with the ABA including her annual service leading the annual agency meeting of Joint Committee on Employee Benefits (JCEB) representatives with the HHS Office of Civil Rights and participation in other JCEB agency meetings, past involvements with legislative affairs for the Texas Association of Business and Dallas HR and others, and many speeches, publications, and other educational outreach efforts, Ms. Stamer has worked closely with Congress and federal and state regulators on the Patient Protection & Affordable Care Act and other health care, pension, immigration, tax and other workforce-related legislative and regulatory reforms for more than 30 years. One of the primary drafters of the Bolivian Social Security reform law and a highly involved leader on U.S. workforce, benefits, immigration and health care policy reform, Ms. Stamer’s experience also includes working with U.S. and foreign government, trade association, private business and other organizations to help reform other countries’ and U.S. workforce, social security and severance, health care, immigration, privacy and data security, tax, ethics and other laws and regulations. Ms. Stamer also contributes her policy, regulatory and other leadership to many professional and civic organizations including as Vice President of the North Texas Healthcare Compliance Professionals Association; Immediate Past Chair of the American Bar Association RPTE Employee Benefits & Other Compensation Committee and its current Welfare Benefit Plans Committee Co-Chair, a Substantive Groups & Committee Member; a member of the leadership council of the ABA Joint Committee on Employee Benefits; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; the current Vice Chair of the ABA TIPS Employee Benefit Committee, and the past Coordinator of the Gulf Coast TEGE Council TE Division.
The publisher and editor of Solutions Law Press, Inc. who serves on the Editorial Advisory Boards of Employee Benefit News, HR.com, InsuranceThoughtLeadership.com and many other publications, Ms. Stamer also is a prolific and highly respected author and speaker, National Public Radio, CBS, NBC, and other national and regional news organization, Atlantic Information Services, The Bureau of National Affairs, HealthLeaders, Telemundo, Modern Healthcare, Business Insurance, Employee Benefit News, the Employee Benefits News, World At Work, Benefits Magazine, InsuranceThoughtLeadership.com, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, CEO Magazine, CFO Magazine, CIO Magazine, the Houston Business Journal, and many other prominent news and publications. She also serves as a planning faculty member and regularly conducts training and speaks on these and other management, compliance and public policy concerns for these and a diverse range of other organizations. For additional information about Ms. Stamer, see www.cynthiastamer.com.
For Added Information and Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For Help Or More Information
If you need assistance in auditing or assessing, updating or defending your organization’s compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 24 years of work helping employers and other management; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend union-management relations, wage and hour, discrimination and other labor and employment laws, privacy and data security, internal investigation and discipline and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on management, reengineering, investigations, human resources and workforce, employee benefits, compensation, internal controls and risk management, federal sentencing guideline and other enforcement resolution actions, and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters.Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see hereor contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2014 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Stamer Kicks Off Dallas HR 2015 Monthly Lunch Series With 2015 Federal Legislative, Regulatory & Enforcement Update |
Comments Off on Stamer Kicks Off Dallas HR 2015 Monthly Lunch Series With 2015 Federal Legislative, Regulatory & Enforcement Update |  105(h), ACA, ADA, Affirmative Action, Affordable Care Act, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Civil Rights, Claims Administration, COBRA, compensation transparency, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, ESOP, Excise Tax, Executive Compensation, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Mental Health, Mental Health Parity, MEWA, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Premium Subsidies, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Tax, Tax Credit, Telecommuting, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs | Tagged: Administrative Simplification, CMS, Health Benefits, Health Insurance, Health insurers, Health Plans, HHS, HPID, HPOES, out-of-pocket maximum, TPAs |
105(h), ACA, ADA, Affirmative Action, Affordable Care Act, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Civil Rights, Claims Administration, COBRA, compensation transparency, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, ESOP, Excise Tax, Executive Compensation, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Mental Health, Mental Health Parity, MEWA, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Premium Subsidies, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Tax, Tax Credit, Telecommuting, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs | Tagged: Administrative Simplification, CMS, Health Benefits, Health Insurance, Health insurers, Health Plans, HHS, HPID, HPOES, out-of-pocket maximum, TPAs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 2, 2014
A $6.48 million judgment against Direct TV satellite television installer, Bruister and Associates Inc.(BAI) its sole owner, Herbert Bruister, and other trustees of two BAI-sponsored employee stock ownership plans shows plan sponsors and trustees involved in stock purchase transactions where employee stock ownership plans commonly referred to as “ESOPs” and other employee benefit plan buy or hold investments in the stock of plan sponsors or other related businesses the risks of failing to conduct the transactions to ensure that the transactions are prudently performed and otherwise conducted in compliance with the Employee Retirement Income Security Act (ERISA) fiduciary responsibility requirements.
BAI Lawsuit & Judgment Highlights
The BAI judgment stems from a Department of Labor lawsuit that charged BAI, along with BAI board members and plan trustees Bruister and Amy Smith, and plan trustee Jonda Henry engaged in prohibited transactions and breached other fiduciary duties under ERISA by causing the plans to purchase 100 percent of BAI’s shares for $24 million in three sales transactions conducted between December 2002 to December 2005.
According to court documents, Bruister, Smith and Henry, as plan fiduciaries, engaged in prohibited transactions by causing the plans to pay excessive prices for BAI stock purchased from Bruister. For each purchase, the Labor Department charged the fiduciaries used flawed valuations prepared by Matthew Donnelly and his firm, Business Appraisal Institute.
The court also found that the three fiduciaries breached their duty of loyalty from start to finish. Additionally, Bruister and his attorney David Johanson went so far as to fire the initial attorney representing the plans because that attorney was too thorough. Moreover, the court found that Bruister and Johanson exercised undue influence over Donnelly’s valuations, and that as a result, Donnelly was not sufficiently independent to provide valuations for the plans.
The court concluded that Bruister, Henry and Smith, in their role as plan fiduciaries, failed to properly represent plan participants’ interests, and that they unreasonably relied on an appraiser who so obviously lacked independence. The court reasoned, “An informed trustee would not have remained idle while the seller communicated directly with the employee stock ownership trust’s independent appraiser and financial advisor to elevate the price at the participants’ expense.”
Although Johanson was not a fiduciary, the court found his conduct worthy of comment because he both was the attorney for the seller and structured each sale. The court noted that Johanson attempted to influence the valuations in Bruister’s favor, and the testimony Johanson gave at trial did not support his denials. The court even noted that Johanson coached Donnelly during a break in his deposition to retract his testimony that Johanson represented Bruister individually. “History rebuts Johanson’s suggestion that he did not interfere with Donnelly’s valuations and raises doubts as to each of the subject transactions,” the court said.
The order requires Bruister, Smith and Henry to jointly pay $4.5 million in restitution to the plans and requires Bruister to pay an additional $1.98 million in prejudgment interest. The order also held Bruister Family LLC liable with all defendants for $885,065 and jointly liable with Bruister for $390,604.
Company Stock Investments Carry Special ERISA Risks
Purchases of company stock by an ESOP or other employee benefit plan can create a wide range of risks under ERISA’s fiduciary responsibility rules. When making investment or other decisions under an employee benefit plan, the general fiduciary duty standards of ERISA § 404 generally require plan fiduciaries to act prudently and solely in the interest of participants and beneficiaries. Meanwhile, except in certain narrow circumstances and subject to fulfillment of ERISA § 404, the prohibited transaction rules of ERISA § 406 among other things prohibits plan fiduciaries from causing the plan to engage in a transaction, if he knows or should know that such transaction is a direct or indirect:
- Sale or exchange, or leasing, of any property between the plan and a party in interest;
- Furnishing of goods, services, or facilities between the plan and a party in interest;
- Transfer to, or use by or for the benefit of a party in interest, of any assets of the plan; or
- Acquisition, on behalf of the plan, of any employer security or employer real property in violation of section 1107 (a) of this title.
As for all plan investment transactions, detailed, unbiased valuation documentation showing the prudence of any decision to invest or hold the investments of the plan in company stock is critical when determining the initial purchase or sale prices for plan transactions involving company stock. Since the sponsoring company is a party-in-interest of the plan, holding, must less using plan assets to purchase company stock or other activities resulting in the inclusion of company stock among the plan assets held by the plan creates presumptions of impropriety that impose higher than usual burdens upon the plan, its sponsor and fiduciaries to prove the appropriateness of the transaction. See e.g., Pfeil v. State Street Bank & Trust Co., 671 F.3d 585 (6th Cir. 2012). As ESOP transactions to purchase company stock inherently require a host of complicated party-in-interest and other conflict of interest concerns, these risks are particularly heightened. Employee benefit plans, their fiduciaries and sponsors the need to continuously and prudently conduct documented monitoring and evaluations evaluate and monitor the investment of plan assets in company stock,the analysis and decisions about whether to continue to keep and offer this stock under the plan, as well as the qualifications, credentials and conduct of the fiduciaries and others empowered to influence these decisions. The Labor Department’s statement in announcing the Parrot litigation sums up the messages from these cases. “Plan officials are required by law to manage the ESOP in a careful, prudent manner and to act solely to benefit the plan’s participants,” said Jean Ackerman, director of the Employee Benefit Security Administration’s (EBSA’s) San Francisco Regional Office, which. “This action underscores the department’s commitment to protect the benefits that employers promise to their employees.”
In light of these exposures, plan fiduciaries, sponsors and their management, service providers and consultants participating in these activities need to both act with care and carefully document their actions to position to defend potential challenges.
Plans, their sponsors and fiduciaries also should ensure that appropriate steps are taken in selecting the fiduciaries, management and service providers responsible for administering or overseeing the administration of their plans, the selection of vendors, and other critical details. Appropriate background checks and other credentialing should be done both at commencement and periodically. Bonding and fiduciary liability insurance should be arranged and reviewed periodically along with their activities. Documentation of these and other steps should be carefully created and preserved.
When and if a change in stock value or other event that could compromise the investment occurs, consideration should be given as to the responsibilities that such events create under ERISA. As company leaders often have dual responsibilities to both the company and the plan, it is important that the company sponsoring the plan, its management and owners learn in advance how these responsibilities impact each other so that they are aware of the issues and have a good understanding of responsibilities and options as situations evolve.
Businesses and business leaders that fail to conduct and maintain the necessary evidence that these requirements are met when involving the plan in these transactions risk significant liability.
“Plan fiduciaries have an obligation to work solely in the interest of plan participants,” said Assistant Secretary of Labor for Employee Benefits Security Phyllis C. Borzi.in the Labor Department’s October 31, 2014 announcement of the judgment. “When they fail to do so, the retirement security of workers is put in jeopardy, and we will take action to make plan participants whole.”
For Help or More Information
If you need help reviewing and updating, administering or defending your employee benefit, human resources, insurance, health care matters or related documents or practices to monitor or respond to evolving laws and regulations, drafting or administering programs, resolving or defending audits, investigations or disputes or other employee benefit, human resources, safety, compliance or risk management concerns, please contact the author of this update, Cynthia Marcotte Stamer.
About Ms. Stamer
A Fellow in the American College of Employee Benefit Council, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 24 years of work, advocacy, education and publications on cutting edge health and managed care, employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials about regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns see here or contact Ms. Stamer via telephone at 469.767.8872 or via e-mail to cstamer@solutionslawyer.net.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2014 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Plan’s Purchase of Company Stock Triggers $6.48 Million Award Against ESOP Sponsor, Shareholder, Board Members & Trustees |
Comments Off on Plan’s Purchase of Company Stock Triggers $6.48 Million Award Against ESOP Sponsor, Shareholder, Board Members & Trustees |  ADA, Bankruptcy, Corporate Compliance, Defined Contribution Plans, Employee Benefits, Employers, ERISA, ESOP, Excise Tax, Fiduciary Responsibility, Human Resources, Internal Controls, Internal Investigations, Retirement Plans, Tax, Tax Qualification | Tagged: 404, 406, defined benefit plan, Employer, ERISA, ESOP, exclusive benefit, Fiduciary Responsibility, Human Resources, pension plan, plan qualification, profit sharing plan, prohibited transaction, Prudence, Retirement Plans, Tax |
ADA, Bankruptcy, Corporate Compliance, Defined Contribution Plans, Employee Benefits, Employers, ERISA, ESOP, Excise Tax, Fiduciary Responsibility, Human Resources, Internal Controls, Internal Investigations, Retirement Plans, Tax, Tax Qualification | Tagged: 404, 406, defined benefit plan, Employer, ERISA, ESOP, exclusive benefit, Fiduciary Responsibility, Human Resources, pension plan, plan qualification, profit sharing plan, prohibited transaction, Prudence, Retirement Plans, Tax |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 27, 2014
The Internal Revenue Service (IRS) has announced the cost-of-living adjustments (COLA) to the compensation and contribution limits affecting individual retirement account, qualified defined benefit plan, qualified 401(k) and other defined contribution and defined benefit plan contributions under the Internal Revenue Code (Code) for 2015. Meanwhile, the Pension Benefit Guarantee Corporation (PBGC) also released updated guaranteed benefit amounts that will apply under the pension benefit guarantee programs it administers for 2015.
Code COLAs for 2015
The 2015 COLA limits under the Code among other things determine what individuals are considered highly compensated and key employees for purposes of the Code’s rules for qualified retirement plans, health plans, cafeteria plans, and certain other employee benefit plans, the amounts that employers and employee can contribute on a tax preferred basis a qualified retirement plan, and various other issues relating to the tax treatment of employee benefit plans. The 2015 COLA amounts under the Code compared to those for 2014 and 2013 are as follows:
|
2015 |
2014 |
2013 |
|
IRAs
|
| IRA Contribution Limit |
$5,500 |
$5,500 |
$5,500 |
| IRA Catch-Up Contributions |
1,000 |
1,000 |
1,000 |
|
IRA AGI Deduction Phase-out Starting at
|
| Joint Return |
98,000 |
96,000 |
95,000 |
| Single or Head of Household |
61,000 |
60,000 |
59,000 |
|
SEP
|
| SEP Minimum Compensation |
600 |
550 |
550 |
| SEP Maximum Contribution |
53,000 |
52,000 |
51,000 |
| SEP Maximum Compensation |
265,000 |
260,000 |
255,000 |
|
SIMPLE Plans
|
| SIMPLE Maximum Contributions |
12,500 |
12,000 |
12,000 |
| Catch-up Contributions |
3,000 |
2,500 |
2,500 |
|
401(k), 403(b), Profit-Sharing Plans, etc.
|
| Annual Compensation |
265,000 |
260,000 |
255,000 |
| Elective Deferrals |
18,000 |
17,500 |
17,500 |
| Catch-up Contributions |
6,000 |
5,500 |
5,500 |
| Defined Contribution Limits |
53,000 |
52,000 |
51,000 |
| ESOP Limits |
1,070,000
210,000 |
1,050,000210,000 |
1,035,000205,000 |
|
Other
|
| HCE Threshold |
120,000 |
115,000 |
115,000 |
| Defined Benefit Limits |
210,000 |
210,000 |
205,000 |
| Key Employee |
170,000 |
170,000 |
165,000 |
| 457 Elective Deferrals |
18,000 |
17,500 |
17,500 |
| Control Employee (board member or officer) |
105,000 |
105,000 |
100,000 |
| Control Employee (compensation-based) |
215,000 |
210,000 |
205,000 |
| Taxable Wage Base |
118,500 |
117,000 |
113,700 |
Employer and other employee benefit plan sponsors, fiduciaries and administrators should update their plan documentation, enrollment and other communications, protocols for identifying and managing contributions for highly compensated and key employees, contribution and discrimination testing and other related programs and practices as well as notify employees and encourage them to take into account these adjusted limitations when making their upcoming benefit enrollment choices for the upcoming year.
2015 PBGC Maximum Insurance Benefit Level
The PBGC also updated its limits for 2015 today. It employer plan has increased to $60,136 for 2015, up from $59,318 for 2014. The increase is not retroactive. Payments to retirees whose plans terminated before 2015 will not change. The guarantee for multiemployer plans has not changed.
Single-Employer Plan Guarantee The PBGC maximum guarantee for participants in single-employer plans is determined using a formula prescribed by federal law that calls for annual increases. The formula provides lower amounts for people who begin getting benefits from PBGC before age 65, reflecting the fact that they will receive more monthly pension checks over their expected lifetime. Conversely, amounts are higher for benefits starting at ages above 65. The formula also calls for reducing the amount for retirees who choose a payment form that continues benefits to a beneficiary after the retiree’s death. The following table shows the maximum annual guarantee limits for 2015 for sample ages and payment forms. Amounts for other ages are posted on the Maximum Monthly Guarantees table on PBGC’s website.
| Age |
Annual Maximum Single Life Annuity |
Annual Maximum Joint & 50% Survivor Annuity* |
| 65 |
$60,136 |
$54,123 |
| 60 |
$39,098 |
$35,180 |
| 55 |
$27,061 |
$24,355 |
| *Assumes both spouses are the same age. Different amounts apply if that is not the case |
The limits shown above generally apply for participants whose plan terminates in 2015. However, if a plan terminates in 2015 as a result of a bankruptcy that began in an earlier year, the limits in effect for that earlier year apply. In most cases, the single-employer PBGC guarantee is larger than the pension earned by people in such plans. In fact, according to a 2006 study, almost 85% of retirees receiving PBGC benefits at that time received the full amount of their earned benefit.(For more information, see the entry “Making Sense of the Maximum Insurance Benefit” in PBGC blog, Retirement Matters.) The limits shown above represent the cap on what PBGC guarantees, not on what PBGC pays. In some cases, PBGC pays benefits above the guaranteed amount. Whether that happens depends on the retiree’s age and how much money was in the plan when it terminated. For more information about how the single-employer guarantee works, see Pension Guarantees on PBGC.gov.
Multiemployer Plan Guarantee Limit The PBGC maximum guarantee for participants in multiemployer plans is also based on a formula prescribed by federal law. Unlike the single-employer formula, the multiemployer guarantee is not indexed (i.e., it remains the same from year to year) and does not vary based on the retiree’s age or payment form. Unlike the single-employer formula, it varies based on the retiree’s length of service. In addition, the multiemployer guarantee structure has two tiers, providing 100% coverage up to a certain level and 75% coverage above that level. For a retiree with 30 years of service, the current annual limit is 100% of the first $3,960 and 75% of the next $11,760 for a total guarantee of $12,870. This limit has been in place since 2001.
About Author Cynthia Marcotte Stamer
If you need help reviewing or updating your health benefit program for compliance or with any other employment, employee benefit, compensation or internal controls matter, please contact the author of this article, attorney Cynthia Marcotte Stamer.
A Fellow in the American College of Employee Benefits Council, immediate past-Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPPT Employee Benefits & Other Compensation Arrangements, an ABA Joint Committee on Employee Benefits Council Representative, the ABA TIPS Employee Benefit Plan Committee Vice Chair, former ABA Health Law Section Managed Care & Insurance Interest Group Chair, past Southwest Benefits Association Board Member, Employee Benefit News Editorial Advisory Board Member, and a widely published speaker and author, Ms. Stamer has more than 24 years experience advising businesses, plans, fiduciaries, insurers. plan administrators and other services providers, and governments on health care, retirement, employment, insurance, and tax program design, administration, defense and policy. Nationally and internationally known for her creative and highly pragmatic knowledge and work on health benefit and insurance programs, Ms. Stamer’s experience includes extensive involvement in advising and representing these and other clients on ACA and other health care legislation, regulation, enforcement and administration.
Widely published on health benefit and other related matters, Ms. Stamer’s insights and articles have been published by the HealthLeaders, Modern Health Care, Managed Care Executive, the Bureau of National Affairs, Aspen Publishers, Business Insurance, Employee Benefit News, the Wall Street Journal, the American Bar Association, Aspen Publishers, World At Work, Spencer Publications, SHRM, the International Foundation, Solutions Law Press and many others.
For additional information about Ms. Stamer and her experience, see www.CynthiaStamer.com.
For Added Information and Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For Help Or More Information
If you need assistance in auditing or assessing, updating or defending your organization’s compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 24 years of work helping employers and other management; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend union-management relations, wage and hour, discrimination and other labor and employment laws, privacy and data security, internal investigation and discipline and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on management, reengineering, investigations, human resources and workforce, employee benefits, compensation, internal controls and risk management, federal sentencing guideline and other enforcement resolution actions, and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters.Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see hereor contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2014 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on IRS Announces Employee Plan Cost-Of-Living Adjustments |
Comments Off on IRS Announces Employee Plan Cost-Of-Living Adjustments |  105(h), Cafeteria Plans, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Health Plans, Human Resources, Reporting & Disclosure, Retirement Plans, Tax | Tagged: 401(k), Administrative Simplification, COLA, COLI, cost-of-living, Health Benefits, Health Plans, Retirement Plans |
105(h), Cafeteria Plans, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Health Plans, Human Resources, Reporting & Disclosure, Retirement Plans, Tax | Tagged: 401(k), Administrative Simplification, COLA, COLI, cost-of-living, Health Benefits, Health Plans, Retirement Plans |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 24, 2014
Revenue Procedure 2014-25 has the list of countries for tax year 2013 for which the minimum time requirements are waived for purposes of the foreign earned income exclusion. It will be formally published in Internal Revenue Bulletin 2014-15 on April 7, 2014.
For Representation, Training & Other Resources
If you need assistance monitoring or responding to these and other regulatory policy, enforcement, litigation or other developments, or to review or respond to these or other workforce, benefits and compensation, performance and risk management, compliance, enforcement or management concerns, the author of this update, attorney Cynthia Marcotte Stamer may be able to help.
Board Certified in Labor & Employment Law, Past Chair of the ABA RPTE Employee Benefit & Other Compensation Arrangements Group, Co-Chair and Past Chair of the ABA RPTE Welfare Plan Committee, Vice Chair of the ABA TIPS Employee Benefit Plans Committee, Vice President of the North Texas Health Care Compliance Professionals Association, Past Chair of the ABA Health Law Section Managed Care & Insurance Section and the former Board Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has more than 25 years’ experience advising health plan and employee benefit, insurance, financial services, employer and health industry clients about these and other matters. Ms. Stamer has extensive experience advising and assisting health care providers, health plans, their business associates and other health industry clients to establish and administer medical privacy and other compliance and risk management policies, to health care industry investigation, enforcement and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns. The scribe for the ABA JCEB Annual Agency Meeting with the Office of Civil Rights (OCR) for the past several years who has worked on medical and other privacy concerns throughout her career, she regularly designs and presents HIPAA and other risk management, compliance and other training for health plans, employers, health care providers, professional associations and others, defends covered entities and business associates against OCR, FTC and other privacy and data security investigations, serves as special counsel in litigation arising from these concerns and is the author of several highly regarded publications on HIPAA and other privacy and security concerns.
Ms. Stamer also regularly works with OCR, FTC, USSS, FBI and state and local law enforcement on privacy, data security, health care, benefits and insurance and other matters, publishes and speaks extensively on medical and other privacy and data security, health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns. Her publications and insights appear in the Health Care Compliance Association, Atlantic Information Service, Bureau of National Affairs, World At Work, The Wall Street Journal, Business Insurance, the Dallas Morning News, Modern Health Care, Managed Healthcare, Health Leaders, and a many other national and local publications. For instance, Ms. Stamer for the third year will serve as the appointed scribe for the ABA Joint Committee on Employee Benefits Agency meeting with OCR. Her insights on HIPAA risk management and compliance frequently appear in medical privacy related publications of a broad range of health care, health plan and other industry publications Among others, she has conducted privacy training for the Association of State & Territorial Health Plans (ASTHO), the Los Angeles Health Department, the American Bar Association, the Health Care Compliance Association, a multitude of health industry, health plan, insurance and financial services, education, employer employee benefit and other clients, trade and professional associations and others. You can get more information about her HIPAA and other experience here.
You can review other recent human resources, employee benefits and internal controls publications and resources and additional information about the employment, employee benefits and other experience of the Cynthia Marcotte Stamer, PC here. If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile www.cynthiastamer.com or by registering to participate in the distribution of these and other updates on our HR & Employee Benefits Update distributions here including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. For important information concerning this communication click here. ©2014 Cynthia Marcotte Stamer. Limited, non-exclusive right to republished granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on List of Countries Excluded From Foreign Earned Income Exclusion Minimum Time Requirements Published |
Comments Off on List of Countries Excluded From Foreign Earned Income Exclusion Minimum Time Requirements Published |  Defined Benefit Plans, Defined Contribution Plans, Employers, ERISA, Human Resources, Insurance, Retirement Plans | Tagged: cash balance plans, Cycle C, determination letter, Determination Letters, ex patriate, International, Qualified Plans, Retirement Plans |
Defined Benefit Plans, Defined Contribution Plans, Employers, ERISA, Human Resources, Insurance, Retirement Plans | Tagged: cash balance plans, Cycle C, determination letter, Determination Letters, ex patriate, International, Qualified Plans, Retirement Plans |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 19, 2014
Employer or other sponsors of individually-designed cash balance plans who have pending Cycle C determination letter applications pending before the Internal Revenue Service (IRA) seeking approval of the qualification of their individually-designed plan who now prefer instead to adopt a pre-approved cash balance plan should act quickly to withdraw their pending application. The IRS has announced that these parties can get a refund of the application fee paid for the individually-designed plan application by signing the Form 8905, Certification of Intent to Adopt a Pre-approved Plan , by March 31, 2014 and withdrawing their pending applications for individually designed cash balance plans by May 31, 2014 in accordance with the instructions set forth later in this article.
Background
Announcement 2014-4 extended the submission period for pre-approved defined benefit pension plans from January 31, 2014, to February 2, 2015, to allow time for the IRS to expand the pre-approved program to let plans with cash balance features. The announcement also allowed Cycle C plan sponsors who want to adopt a pre-approved cash balance plan to complete and sign a Form 8905, Certification of Intent to Adopt a Pre-approved Plan by March 31, 2014, instead of submitting determination letter applications for individually designed plans by the Cycle C deadline of January 31, 2014.
Withdrawals for Cycle C Applicants For Individually-Designed Cash Balance Plan Approval
Cycle C applicants who already submitted their applications for individually-designed cash balance plans during the second Cycle C remedial amendment cycle that ended January 31, 2014, and who instead wish to adopt a pre-approved cash balance plan, may sign the Form 8905, withdraw the application, and request a refund of the user fee by complying with the instructions below.
The IRS says that a request for return of A Cycle C determination letter application and a refund of the user fee must be made in writing and postmarked (or faxed) by May 31, 2014 to: Internal Revenue Service 550 Main Street Cincinnati, OH 45202 Attn: Joyce Heinbuch. Correspondence sent via Fax should be sent to the attention of Ms. Heinbuch at (513) 263-4699 (not a toll-free call).
The written request must include:
- the name of the plan sponsor
- plan number
- EIN
- the document locator number, if known (shown on your IRS acknowledgement letter)
- the following statement in bold letters: “Per Announcement 2014-4, we are withdrawing this application in order to submit under the pre-approved program.”
For additional information and resources, see Deadline Extended For Pre-Approved Defined Benefit Plans and FAQs on Withdrawing Cycle C Applications or contact your preferred employee benefit attorney.
For Representation, Training & Other Resources
If you need assistance monitoring or responding to these and other regulatory policy, enforcement, litigation or other developments, or to review or respond to these or other workforce, benefits and compensation, performance and risk management, compliance, enforcement or management concerns, the author of this update, attorney Cynthia Marcotte Stamer may be able to help.
Board Certified in Labor & Employment Law, Past Chair of the ABA RPTE Employee Benefit & Other Compensation Arrangements Group, Co-Chair and Past Chair of the ABA RPTE Welfare Plan Committee, Vice Chair of the ABA TIPS Employee Benefit Plans Committee, Vice President of the North Texas Health Care Compliance Professionals Association, Past Chair of the ABA Health Law Section Managed Care & Insurance Section and the former Board Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has more than 25 years’ experience advising health plan and employee benefit, insurance, financial services, employer and health industry clients about these and other matters. Ms. Stamer has extensive experience advising and assisting health care providers, health plans, their business associates and other health industry clients to establish and administer medical privacy and other compliance and risk management policies, to health care industry investigation, enforcement and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns. The scribe for the ABA JCEB Annual Agency Meeting with the Office of Civil Rights (OCR) for the past several years who has worked on medical and other privacy concerns throughout her career, she regularly designs and presents HIPAA and other risk management, compliance and other training for health plans, employers, health care providers, professional associations and others, defends covered entities and business associates against OCR, FTC and other privacy and data security investigations, serves as special counsel in litigation arising from these concerns and is the author of several highly regarded publications on HIPAA and other privacy and security concerns.
Ms. Stamer also regularly works with OCR, FTC, USSS, FBI and state and local law enforcement on privacy, data security, health care, benefits and insurance and other matters, publishes and speaks extensively on medical and other privacy and data security, health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns. Her publications and insights appear in the Health Care Compliance Association, Atlantic Information Service, Bureau of National Affairs, World At Work, The Wall Street Journal, Business Insurance, the Dallas Morning News, Modern Health Care, Managed Healthcare, Health Leaders, and a many other national and local publications. For instance, Ms. Stamer for the third year will serve as the appointed scribe for the ABA Joint Committee on Employee Benefits Agency meeting with OCR. Her insights on HIPAA risk management and compliance frequently appear in medical privacy related publications of a broad range of health care, health plan and other industry publications Among others, she has conducted privacy training for the Association of State & Territorial Health Plans (ASTHO), the Los Angeles Health Department, the American Bar Association, the Health Care Compliance Association, a multitude of health industry, health plan, insurance and financial services, education, employer employee benefit and other clients, trade and professional associations and others. You can get more information about her HIPAA and other experience here.
You can review other recent human resources, employee benefits and internal controls publications and resources and additional information about the employment, employee benefits and other experience of the Cynthia Marcotte Stamer, PC here. If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile www.cynthiastamer.com or by registering to participate in the distribution of these and other updates on our HR & Employee Benefits Update distributions here including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. For important information concerning this communication click here. ©2014 Cynthia Marcotte Stamer. Limited, non-exclusive right to republished granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Some Sponsors Should Act by 3/31 To Withdraw Individually-Designed Cash Balance Plan Approval Request |
Comments Off on Some Sponsors Should Act by 3/31 To Withdraw Individually-Designed Cash Balance Plan Approval Request |  Defined Benefit Plans, Defined Contribution Plans, Employers, ERISA, Human Resources, Insurance, Retirement Plans | Tagged: cash balance plans, Cycle C, determination letter, Determination Letters, Qualified Plans, Retirement Plans |
Defined Benefit Plans, Defined Contribution Plans, Employers, ERISA, Human Resources, Insurance, Retirement Plans | Tagged: cash balance plans, Cycle C, determination letter, Determination Letters, Qualified Plans, Retirement Plans |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 13, 2013
With 2013 rushing to the close, the Internal Revenue Service (IRS) has issued guidance providing nondiscrimination relief for certain defined benefit plans is providing temporary nondiscrimination relief for some defined benefit plans, its annual list of qualified plan changes, and guidance about in-plan Roth rollovers,.
DB Plan Discrimination Rule Relief
Notice 2014-05 provides temporary nondiscrimination relief for certain “closed” defined benefit pension plans (i.e., defined benefit plans that provide ongoing accruals but that have been amended to limit those accruals to some or all of the employees who participated in the plan on a specified date). The Notice allows some employers that sponsor a closed defined benefit plan and a defined contribution plan to demonstrate that the aggregated plans comply with the nondiscrimination requirements of § 401(a)(4) on the basis of equivalent benefits, even if the aggregated plans do not satisfy the current conditions for testing on that basis. The notice also requests comments on possible permanent changes to the nondiscrimination rules under § 401(a)(4).
Plan sponsors and administrators of plans that may benefit from this relief should consult with qualified legal or tax counsel for assistance in understanding the potential applicability and implications of the guidance.
In Plan Roth Rollover Guidance
Notice 2013-74 provides guidance on in-plan Roth rollovers, the practitioner community is looking forward to this guidance.
Notice 2013-84 contains the 2013 Cumulative List of Changes in Plan Qualification Requirements (2013 Cumulative List) described in section 4 of Rev. Proc. 2007-44, 2007-2 C.B. 54.
For Assistance or More Information
If you have questions or need help with these or employee benefit, human resources, insurance, health care matters or related documents or practices, please contact the author of this update, Cynthia Marcotte Stamer.
A Fellow in the American College of Employee Benefit Council, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 25 years of work, advocacy, education and publications on cutting edge health and managed care, employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials about regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, HR.com, Insurance Thought Leadership, Solutions Law Press, Inc. and other publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. Her widely respected publications and programs include more than 25 years of publications on health plan contracting, design, administration and risk management including a “Managed Care Contracting Guide” published by the American Health Lawyers Association and numerous other works on vendor contracting. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer here.
Other Helpful Resources & Other Information
We hope that this information is useful to you. If you found these updates of interest, you also be interested in one or more of the following other recent articles published on the Coalition for Responsible Health Care Reform electronic publication available here, our electronic Solutions Law Press Health Care Update publication available here, or our HR & Benefits Update electronic publication available here . You also can get access to information about how you can arrange for training on “Building Your Family’s Health Care Toolkit,” using the “PlayForLife” resources to organize low-cost wellness programs in your workplace, school, church or other communities, and other process improvement, compliance and other training and other resources for health care providers, employers, health plans, community leaders and others here. If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail by creating or updating your profile here. You can reach other recent updates and other informative publications and resources.
Recent examples of these publications include:
For important information about this communication click here.
©2013 Cynthia Marcotte Stamer. Nonexclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on IRS Provides Closed DB Plan Relief, Qualified Plan Changes List & In-Plan Roth Rollovers Guidance |
Comments Off on IRS Provides Closed DB Plan Relief, Qualified Plan Changes List & In-Plan Roth Rollovers Guidance |  Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Retirement Plans | Tagged: 401(a)(4), defined benefit plan, defined contribution plan, discrimination testing, plan qualification |
Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Retirement Plans | Tagged: 401(a)(4), defined benefit plan, defined contribution plan, discrimination testing, plan qualification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
June 5, 2013
The June 4, 2013 announcement of the Employee Benefit Security Administration (EBSA) provides a timely reminder to businesses sponsoring employee benefit plans, their owners and management, plan fiduciaries, banks, administrative service providers and other plan vendors, employee benefit plan and bankruptcy trustees, corporate receivers, creditors, and others looking to expedite the windup of abandoned 401(k), profit-sharing and other individual account pension plans of the challenges that can result when employee benefit plan responsibilities are mishandled when companies fail or experience other significant events, as well as the availability of tools to help mitigate or prevent these challenges through responsible proactive action.
Hidden Employee Benefit Exposures For Unwary Abound For Parties In Business Insolvency Or Other Transactions
A complex maze of ERISA, tax and other rules make, administration and termination of employee benefit plans a complicated matter. When the company sponsoring a plan experiences a significant workforce or other restructuring, becomes distressed, goes bankrupt or liquidates, merges, sells assets or engages in other significant business transaction impacting the plans or its workforce, the rules, as well as the circumstances, can create a liability and operational quagmire for everyone from the sponsoring business, its management, buyers, vendors, plan fiduciaries, plan participants and beneficiaries, related entities, asset purchasers and others. While tough economic times may tempt business leaders to cut corners, more than 3o years of litigation and enforcement precedent make clear that cutting corners on the assessment and handling of employee benefit and other workforce responsibilities amid business distress or in other business transactions or events presents risks for all parties involved. See e.g., Tough Times Are No Excuse For ERISA Shortcuts; Mishandling Employee Benefit Obligations Creates Big Liabilities For Distressed Businesses & Their Business Leaders. While many business leaders and plan fiduciaries lack a strong understanding of these rules and their implications in times of business or benefit plan distress or other significant business transactions, even those experienced with these concerns need to use caution to understand and respond to the series of ongoing changes in these rules, regulations and precedent that impact on the handling of plan related responsibilities in these and other special situations.
The Internal Revenue Code (Code) requires contains a maze of requirements that companies sponsoring pension, profit-sharing, health and other employee benefit plans, their plans, and plan administrators must follow when maintaining, administering, or terminating these plans including in many instances, special rules on the termination of the plans, distribution of assets, and the liabilities that attach to affiliated companies, successors, and assets resulting from transactions involving employee benefit plans or their sponsors.
In addition to the Code’s rules, companies and other individuals that in name or in function have or exercise discretionary responsibility or authority over the maintenance, administration or funding of employee benefit plans regulated by ERISA also generally must meet ERISA’s high standards for carrying out these duties based on their functional ability to exercise discretion over these matters, whether or not they have been named as fiduciaries formally. Under many circumstances these rules, or the handling of transactions can broaden the scope of responsibility or create exposures for a surprising range of parties dealing with the plan sponsor, related corporations or their stock, assets, benefit plans or workforce in corporate bankruptcies, mergers, asset or stock acquisitions, liquidations or other transactions.
Beyond these basic tax and fiduciary obligations, ERISA and the Internal Revenue Code (Code) create additional responsibilities and liabilities for when dealing with defined benefit or other pension plans subject to ERISA’s minimum funding and plan termination rules that when violated trigger a plethora of funding and notification obligations, penalties, liens on assets, and other obligations that can create significant traps for unwary plan fiduciaries and administrators, the sponsoring corporation, its management, affiliates and successors, as well as creditors or purchasers of stock or assets and others dealing with them.
Despite these well-documented responsibilities and a well-established pattern of enforcement by the Department of Labor, Pension Benefit Guarantee Corporation, Internal Revenue Service and private plaintiffs, many businesses and business leaders fail to appropriately understand these and other basic responsibilities and liabilities associated with the establishment, administration, termination and windup of employee benefit plans and other details about how their or others mishandling of employee benefit plan related responsibilities can undermine business goals and create unanticipated liability exposures.
Frequently, companies sponsoring their employee benefit plans and their executives mistakenly assume that they can rely upon vendors and advisors to ensure that their programs are appropriately established. The establishment and maintenance of these arrangements with limited review or oversight by the sponsoring company or its management team can be risky.
In other instances, businesses and their leaders do not realize that ERISA’s functional definition to determine fiduciary status means that individuals participating in discretionary decisions about the employee benefit plan, as well as the plan sponsor, may bear liability under many commonly occurring situations if appropriate care is not exercised to protect participants or beneficiaries in these plans.
In yet other instances, purchasers, related entities, bankruptcy trustees and creditors or others don’t appreciate the way their own or others mishandling of employee benefit plan obligations or exposures can impact their transactions and associated risks.
Proactive Action Can Mitigate Exposures & Costs
For this reason, companies providing employee benefits and their management, service providers, and related entities and the businesses dealing with them need a clear understanding of the rules and responsibilities Federal law imposes on the funding, administration and termination of these programs, how these rules can impact their responsibilities and goals, and the steps necessary to avoid or mitigate exposures likely to result if they or others mishandle employee benefit plan related responsibilities or assets and how to avoid or mitigate these concerns.
The challenges of winding up an abandoned plan discussed in the EBSA news release yesterday highlights just one of these complications, the problem of dealing with abandoned plans.
When companies and their management abandon plans, they leave their plans, participants and beneficiaries, service providers and others in limbo, without the authority or funds to wind up the plans. When employers abandon their individual account pension plans, custodians such as banks, insurers and mutual fund companies are left holding the assets of these abandoned plans but without the authority to terminate such plans and make benefit distributions even in response to participant demands. Service providers often find themselves in the legally awkward situation of having continuing plan responsibilities without necessary direction or compensation for performance. Meanwhile, participants and beneficiaries can’t manage, access or often even get information about their funds until the situation resolves. Dealing with these issues usually requires cumbersome, time-consuming and costly processes often requiring complex, lengthy, highly formalistic and expensive judicial and administrative procedures to resolve while fiduciary, tax and other liabilities mount. Meanwhile, participants and beneficiaries often lose access to their accounts or benefits or even see plan value decline as plan assets that could go to benefits are diverted to cover administrative costs of winding up the plan.
The EBSAs abandoned plan program is just one of many examples of tools that parties struggling with these issues can use to mitigate these challenges and exposures. EBSA uses its abandoned plan program to facilitate a voluntary efficient process for winding up the affairs of abandoned individual account plans so that benefit distributions are made to participants and beneficiaries when this occurs.
The EBSA Abandoned Plan News Release and the EBSA’s related response Response to ADP/JP Morgan published June 4, 2013 show an example of how EBSA used its abandoned plan program to give critical relief to JP Morgan Chase Bank NA and ADP Inc. to use to wind up certain abandoned plans without exhausting the 90-day waiting period that ordinarily applies before the termination of a retirement plan based on the best interest of participants pursuant to 29 CFR §2578.1. By exercising its discretion to waive the 90-day notice period, the EBSA allowed JP Morgan Chase Bank NA and ADP Inc. to terminate immediately and wind up approximately 180 defined contribution pension plans abandoned due to corporate crises or neglect.
Requesting relief from the EBSA like that granted to JP Morgan Chase Bank NA and ADP Inc. in the announcement made yesterday is just one of various types of relief that legal counsel experienced with dealing with workforce and employee benefit plan challenges that can arise when companies or their plans become inadequately funded, bankrupt, or experience other significant transactions or events, can use to help debtors, and other plan sponsors, their management, affiliates, successors, buyers, plan fiduciaries, vendors, bankruptcy creditors and trustees.
Experienced counsel can help companies understand and negotiate the complex rules of the EBSA, the Pension Benefit Guarantee Corporation and the Internal Revenue Service governing dealings with these plans and where appropriate and available by taking advantage of relief or other options to mitigate these challenges. Involving experienced counsel to explore and use these options early can help all parties get participants and beneficiaries their benefits while minimizing legal risks, time and expenses associated with the wind up of these troubled or abandoned plans. Even where special dispensation is not available, the early involvement of experienced legal counsel as early as possible after the possibility that a business or its plans or assets will be impacted by underfunding, insolvency, a bankruptcy or liquidation, workforce reduction, sale, merger or other significant event can help plan and administer the steps necessary to handle cost effectively employee benefit related responsibilities and impacts.
For Help or More Information
If you need help with assessing or handing employee benefit or workforce challenges arising from business or employee benefit plan insolvency, stock or asset sales, mergers, bankruptcy or liquidation, reductions or other workforce changes or other significant business transactions or events, or other employee benefit, human resources, insurance, health care matters or related documents or practices, please contact the author of this update, Cynthia Marcotte Stamer.
A Fellow in the American College of Employee Benefit Council, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 25 years of work, advocacy, education and publications on cutting edge health and managed care, employee benefit, human resources and related workforce, insurance and financial services, and health care matters including extensive experience handling workforce and employee benefit challenges arising from plan underfunding, company restructurings, workforce change, insolvencies, bankruptcies, mergers, stock or asset acquisitions, or other significant business or plan transactions.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, and insurers, bankruptcy trustees and receivers, asset purchasers, creditors and others dealing with plans and their sponsors, and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials about regulatory, investigatory or enforcement concerns. Her experience includes involvement in the planning, execution and resolution of workforce and employee benefit related details of a multitude of high and low profile restructurings, bankruptcies and other significant transactions throughout her more than 25 year career.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer here.
Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For important information about this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2013 Cynthia Marcotte Stamer, P.C. Nonexclusive license to republish granted to Solutions Law Press, Inc. All other rights reserved
 1 Comment |
1 Comment |  Affordable Care Act, Bankruptcy, Claims Administration, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Agreement, ERISA, Excise Tax, Executive Compensation, Fiduciary Responsibility, Health Care Reform, Health Plans, HIPAA, Human Resources, Income Tax, Insurance, MEWA, Patient Protection and Affordable Care Act, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Tax | Tagged: abandoned plans, bankkruptcy, employee benefit plans, ERISA, fiduciary responsibiltiies, illiquid, insolvancy, reductions in force, Reengineering |
Affordable Care Act, Bankruptcy, Claims Administration, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Agreement, ERISA, Excise Tax, Executive Compensation, Fiduciary Responsibility, Health Care Reform, Health Plans, HIPAA, Human Resources, Income Tax, Insurance, MEWA, Patient Protection and Affordable Care Act, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Tax | Tagged: abandoned plans, bankkruptcy, employee benefit plans, ERISA, fiduciary responsibiltiies, illiquid, insolvancy, reductions in force, Reengineering |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 23, 2012
USI Advisors Inc. (USI) will pay $1,265,608.70 to 13 pension plans to resolve charges it violated the Employee Retirement Income Security Act (ERISA) by failing to properly disclose 12b-1 fees it collected off of fund investments. The complaint behind the settlement reflects the commitment of the U.S Department of Labor Employee Benefit Security Administration (EBSA) to enforcing Employee Retirement Income Security Act (ERISA) fee disclosure and other requirements against service providers to employee benefit plans. With regulations tightening, the tough economy driving greater scrutiny of plan investments, expenditures and performance, and enforcement rising, plan vendors, and the employee benefit plan sponsors and fiduciaries responsible for their engagement, compensation and oversight need to ensure the adequacy of their processes for deciding and reporting compensation, as well as the qualification, selection and oversight of vendors and fiduciaries generally.
USI Settlement
An investigation by the U.S. Department of Labor’s Employee Benefits Security Administration (EBSA) USI, fiduciary investment adviser made investments in mutual funds on behalf of ERISA-covered defined benefit plan clients and received 12b-1 fees from those funds. A 12b-1 fee is paid by a mutual fund out of fund assets to cover certain expenses. USI Advisors failed to fully disclose the receipt of the 12b-1 fees, and to use those fees for the benefit of the plans either by directly crediting the amounts to the plans or by offsetting other fees the plans would be obligated to pay the company.
“If you, as an investment adviser, are a fiduciary under ERISA with respect to plan investments in mutual funds, you cannot use your fiduciary authority to receive an additional fee or to receive compensation from third parties for your own personal account in transactions involving plan assets. We are very pleased that this settlement addresses the problems we identified with USI’s practices and restores funds to the plans and their participants,” said Phyllis C. Borzi, assistant secretary of labor for employee benefits security. “We are also very pleased that recently finalized fee disclosure regulations issued by the Labor Department will require fiduciaries like USI to be more transparent about the fees they receive when dealing with their plan clients.”
Under the terms of the settlement, USI Advisors has agreed not to provide bundled investment advisory and actuarial services to any ERISA-covered defined benefit plan client without first entering into a written agreement, contract or letter of understanding that specifies the services provided and whether the company or its affiliates will act as a fiduciary to those plans. USI Advisors also will provide to clients a description of all compensation and fees received, in any form, from any source, involving any investment or transaction related to them.
The alleged violations in this case occurred between 2004 and 2010. USI Advisors is a wholly owned subsidiary of USI Consulting Group, a Goldman Sachs Capital Partners Co.
The investigation conducted by EBSA as part of the agency’s Consultant/Adviser Project, highlights the need for employee benefit plan fiduciaries and vendors alike to properly identify and report all vendor compensation received by employee benefit plan investment advisors and other service providers in compliance with ERISA’s fee disclosure and other requirements. The Consultant/Adviser Project targets vendors and advisors to employee benefit plans for review, and where applicable, enforcement action when service providers violate ERISA’s requirements. EBSA has made misconduct by consultants, advisors and other service providers a priority as part of its broader emphasis on enforcement of ERISA’s fiduciary responsibility and reporting requirements.
Tightening Rules, Enforcement & Tough Times Driving Risks
The EBSA’s announcement of the USI settlement comes as it continues to move forward to strengthen the transparency of vendor compensation and other fiduciary regulations and enforcement. Just shortly before today’s announcement, EBSA recently clarified its guidance about how its rules affect 401(k) plan brokerage window arrangements in response to public feedback. Field Assistance Bulletin No. 2012-02R published July 30, 2012, modifies and replaces Q&A 30 of Field Assistance Bulletin No. 2012-02 (issued May 7, 2012) with a new Q&A 39.
EBSA’s final fee disclosure regulation[i] published on requires plan administrators to make to disclose specified information about retirement plan fees and expenses to participants and beneficiaries. The regulation requires plan administrators to give participants and beneficiaries more informationm about administrative and investment fees and expenses in their 401(k) plans.
EBSA issued Field Assistance Bulletin No. 2012-02, which provided guidance to its field enforcement personnel in question and answer format on the obligations of plan administrators under the fee disclosure regulation on May 7, 2012. In response to questions and concerns about statements in Question 30 regarding brokerage windows and other arrangements that enable plan participants and beneficiaries to select investments beyond those designated by the plan, EBSA issued Field Assistance Bulletin No. 2012-02 which supersedes Field Assistance Bulletin 2012-02 by modifying its provisions about brokerage windows and inviting more public comments for EBSA to use to consider further clarification of this guidance.
As did its predecessor, Field Assistance Bulletin No. 2012-02R specifies that while the fee disclosure regulation covers “brokerage windows,” “self-directed brokerage accounts,” and other similar plan arrangements that enable participants and beneficiaries to select investments beyond those designated by the plan, its coverage of brokerage windows is limited to the disclosure requirements in paragraph (c) of the regulation relating to plan-related information. The disclosure requirements for investment-related information in paragraph (d) of the regulation do not apply to brokerage windows, self-directed brokerage accounts, and similar arrangements or to any investment selected by a participant or beneficiary that is not designated by the plan (i.e., any investments made through the window, account, or arrangement).
Beyond meeting the technicalities of the fee disclosure requirements, plan sponsors, fiduciaries and vendors should also ensure that their selection, oversight, determination of compensation and other dealings with plan vendors and consultants meet the general fiduciary responsibility, prohibited transaction, bonding and other requriements of ERISA, as well as any applicable securities and tax requirements.
Through its participant fee disclosure and other stepped up fiduciary regulations and enforcement, EBSA is sending clear signals that it stands ready to investigate and take action against service providers or others that charge excessive fees, failure to adequately justify or appropriately disclose fees or other compensation from plan transactions, or other fiduciary protections of ERISA. In the face of these requirements, plan fiduciaries, sponsors, advisors and vendors should carefully review the appropriateness of compensation received or promised to plan vendors, as well as the adequacy of practices for identifying and reporting that compensation and the selection and oversight of the vendors receiving that compensation.
For Help or More Information
If you need help reviewing and updating, administering or defending your group health or other employee benefit, human resources, insurance, health care matters or related documents or practices to respond to emerging regulations, monitoring or commenting on these rules, defending your health plan or its administration, or other health or employee benefit, human resources or risk management concerns, please contact the author of this update, Cynthia Marcotte Stamer.
A Fellow in the American College of Employee Benefit Council, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 24 years of work, advocacy, education and publications on cutting edge health and managed care, employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials concerning regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and registerto receive future updates about developments on these and other concerns from Ms. Stamer here.
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
[i]See 75 FR 64910 (Oct. 20, 2010).
©2012 Cynthia Marcotte Stamer. Non-Exclusive License To Republish Granted To Solutions Law Press, Inc. All Other Rights Reserved.
 1 Comment |
1 Comment |  Corporate Compliance, Defined Contribution Plans, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Human Resources, Income Tax, Reporting & Disclosure, Retirement Plans | Tagged: 401(k) plans, brokerage accounts, compliance, Employee Benefits, Employer, ERISA, fee disclosure regulation, Fiduciary Responsibility, Finance, Health Care Reform. Employer, Management, Plan Sponosr, Retirement Plans, Risk Managment |
Corporate Compliance, Defined Contribution Plans, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Human Resources, Income Tax, Reporting & Disclosure, Retirement Plans | Tagged: 401(k) plans, brokerage accounts, compliance, Employee Benefits, Employer, ERISA, fee disclosure regulation, Fiduciary Responsibility, Finance, Health Care Reform. Employer, Management, Plan Sponosr, Retirement Plans, Risk Managment |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 6, 2012
U.S. Department of Labor’s Employee Benefits Security Administration recently clarified its guidance about how its rules affect 401(k) plan brokerage window arrangements in response to public feedback. Field Assistance Bulletin No. 2012-02R published July 30, 2012, modifies and replaces Q&A 30 of Field Assistance Bulletin No. 2012-02 (issued May 7, 2012) with a new Q&A 39.
EBSA’s final fee disclosure regulation[i] published on requires plan administrators to make to disclose specified information about retirement plan fees and expenses to participants and beneficiaries. The regulation requires plan administrators to give participants and beneficiaries more informationm about administrative and investment fees and expenses in their 401(k) plans.
EBSA issued Field Assistance Bulletin No. 2012-02, which provided guidance to its field enforcement personnel in question and answer format on the obligations of plan administrators under the fee disclosure regulation on May 7, 2012. In response to questions and concerns about statements in Question 30 regarding brokerage windows and other arrangements that enable plan participants and beneficiaries to select investments beyond those designated by the plan, EBSA issued Field Assistance Bulletin No. 2012-02 which supersedes Field Assistance Bulletin 2012-02 by modifying its provisions about brokerage windows and inviting more public comments for EBSA to use to consider further clarification of this guidance.
As did its predecessor, Field Assistance Bulletin No. 2012-02R specifies that while the fee disclosure regulation covers “brokerage windows,” “self-directed brokerage accounts,” and other similar plan arrangements that enable participants and beneficiaries to select investments beyond those designated by the plan, its coverage of brokerage windows is limited to the disclosure requirements in paragraph (c) of the regulation relating to plan-related information. The disclosure requirements for investment-related information in paragraph (d) of the regulation do not apply to brokerage windows, self-directed brokerage accounts, and similar arrangements or to any investment selected by a participant or beneficiary that is not designated by the plan (i.e., any investments made through the window, account, or arrangement).
New Q-39 of Field Assistance Bulletin No. 2012-02R addresses when a plan offers an investment platform that includes a brokerage window, self-directed brokerage account, or similar plan arrangement but the fiduciary did not designate any of the funds on the platform or available through the brokerage window, self-directed brokerage account, or similar plan arrangement as “designated investment alternatives” under the plan, if the brokerage account platform or the brokerage window, self-directed brokerage account, or similar plan arrangement is a designated investment alternative for purposes of the regulation. According to Field Assistance Bulletin No. 2012-02R, it is not. According to the Field Assistance Bulletin, the regulation does not require that a plan have a particular number of “designated investment alternative” (DIA), and the Bulletin does not prohibit the use of a platform or a brokerage window, self-directed brokerage account, or similar plan arrangement in an individual account plan. Rather, whether an investment alternative is a DIA for purposes of the regulation depends on whether it is specifically identified as available under the plan.
However Question 39 also cautions plan administrators and fiduciaries about the need to ensure other applicable ERISA obligations are fulfilled. Field Assistance Bulletin 2012-02R notes it does not change the 404(c) regulation or the requirements for relief from fiduciary liability under section 404(c) of ERISA or address the application of ERISA’s general fiduciary requirements to SEPs or SIMPLE IRA plans. Also, fiduciaries of such plans with platforms or brokerage windows, self-directed brokerage accounts, or similar plan arrangements that enable participants and beneficiaries to select investments beyond those designated by the plan are still bound by ERISA section 404(a)’s statutory duties of prudence and loyalty to participants and beneficiaries who use the platform or the brokerage window, self-directed brokerage account, or similar plan arrangement, including taking into account the nature and quality of services provided in connection with the platform or the brokerage window, self-directed brokerage account, or similar plan arrangement. It also notes that that a 401(k) or other individual account plan fiduciary’s failure to designate investment alternatives to avoid investment disclosures under the regulation, raises questions under ERISA section 404(a)’s general statutory fiduciary duties of prudence and loyalty.
For Help or More Information
If you need help reviewing and updating, administering or defending your group health or other employee benefit, human resources, insurance, health care matters or related documents or practices to respond to emerging health plan regulations, monitoring or commenting on these rules, defending your health plan or its administration, or other health or employee benefit, human resources or risk management concerns, please contact the author of this update, Cynthia Marcotte Stamer.
A Fellow in the American College of Employee Benefit Council, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 24 years of work, advocacy, education and publications on cutting edge health and managed care, employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials concerning regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and registerto receive future updates about developments on these and other concerns from Ms. Stamer here.
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
[i]See 75 FR 64910 (Oct. 20, 2010).
©2012 Cynthia Marcotte Stamer. Non-Exclusive License To Republish Granted To Solutions Law Press, Inc. All Other Rights Reserved.
 1 Comment |
1 Comment |  Corporate Compliance, Defined Contribution Plans, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Human Resources, Income Tax, Reporting & Disclosure, Retirement Plans | Tagged: 401(k) plans, brokerage accounts, compliance, Employee Benefits, Employer, ERISA, fee disclosure regulation, Fiduciary Responsibility, Finance, Health Care Reform. Employer, Management, Plan Sponosr, Retirement Plans, Risk Managment |
Corporate Compliance, Defined Contribution Plans, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Human Resources, Income Tax, Reporting & Disclosure, Retirement Plans | Tagged: 401(k) plans, brokerage accounts, compliance, Employee Benefits, Employer, ERISA, fee disclosure regulation, Fiduciary Responsibility, Finance, Health Care Reform. Employer, Management, Plan Sponosr, Retirement Plans, Risk Managment |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 15, 2011
The Internal Revenue Service is reminding tax return preparers to renew their Preparer Tax Identification Numbers (PTINs) before year’s end. All 2011 PTINs will expire on Dececember 31 and must be renewed annually. Tax preparers can renew by loging in here. The fee to renew is $63.
According to the IRS, preparers who applied for PTINs using a paper Form W-12 last year are encouraged to renew online. An activation code and instructions were mailed to each paper applicant for this purpose. Individuals who prefer to renew their PTIN on paper must mail a Form W-12, IRS Paid Preparer Tax Identification Number Application and Renewal. The response time is 4 to 6 weeks.
Tips about dealing with password or other issues are available on the PTIN page here.
For Help or More Information
If you need help reviewing, updating, administering or defending your fringe benefit or other employee benefit, compensation or human resources practices, please contact the author of this update, Cynthia Marcotte Stamer.
Recently selected for induction as a Fellow in the American College of Employee Benefit Council and for extensive work and accomplishments in the employee benefits and human resources area, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 24 years of work, advocacy, education and publications on employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to watch legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials about regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer here.
Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at ww.solutionslawpress.com.
THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2011 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on IRS Urges Preparers to Renew PTINs for 2012 |
Comments Off on IRS Urges Preparers to Renew PTINs for 2012 |  Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Retirement Plans, Tax, Tax Qualification | Tagged: 401(k), accountant, Circular 230, CPA, Determination Letters, Employee Benefits, Fringe Benefits, investment advice, IRA, meal expense, plan qualification, Preparer Tax Identification Number, prohibited transactions, ptin, retirement plan, Retirement Plans, tax preparer, travel expense |
Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Retirement Plans, Tax, Tax Qualification | Tagged: 401(k), accountant, Circular 230, CPA, Determination Letters, Employee Benefits, Fringe Benefits, investment advice, IRA, meal expense, plan qualification, Preparer Tax Identification Number, prohibited transactions, ptin, retirement plan, Retirement Plans, tax preparer, travel expense |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 4, 2011
The Internal Revenue Service has announced that enrolled retirement plan agents will not be required to obtain a preparer tax identification number (PTIN)
Notice 2011-91 will provide that enrolled retirement plan agents are not required to get a preparer tax identification number. Notice 2011-91 is scheduled for publication in Internal Revenue Bulletin 2011-47 on November 21, 2011.
For Help or More Information
If you need help reviewing, updating, administering or defending your fringe benefit or other employee benefit, compensation or human resources practices, please contact the author of this update, Cynthia Marcotte Stamer.
Recently selected for induction as a Fellow in the American College of Employee Benefit Council and for extensive work and accomplishments in the employee benefits and human resources area, immediate past Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Group and current Co-Chair of its Welfare Benefit Committee, Vice-Chair of the ABA TIPS Employee Benefits Committee, a council member of the ABA Joint Committee on Employee Benefits, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer is recognized, internationally, nationally and locally for her more than 24 years of work, advocacy, education and publications on employee benefit, human resources and related workforce, insurance and financial services, and health care matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experienced with these and other employment, employee benefit and compensation matters, Ms. Stamer continuously advises and assists employers, employee benefit plans, their sponsoring employers, fiduciaries, insurers, administrators, service providers, insurers and others to monitor and respond to evolving legal and operational requirements and to design, administer, document and defend medical and other welfare benefit, qualified and non-qualified deferred compensation and retirement, severance and other employee benefit, compensation, and human resources, management and other programs and practices tailored to the client’s human resources, employee benefits or other management goals. A primary drafter of the Bolivian Social Security pension privatization law, Ms. Stamer also works extensively with management, service provider and other clients to monitor legislative and regulatory developments and to deal with Congressional and state legislators, regulators, and enforcement officials concerning regulatory, investigatory or enforcement concerns.
Recognized in Who’s Who In American Professionals and both an American Bar Association (ABA) and a State Bar of Texas Fellow, Ms. Stamer serves on the Editorial Advisory Board of Employee Benefits News, the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, and active in a multitude of other employee benefits, human resources and other professional and civic organizations. She also is a widely published author and highly regarded speaker on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, Modern and many other national and local publications. You can learn more about Ms. Stamer and her experience, review some of her other training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer here.
Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at www.solutionslawpress.com.
THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2011 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on IRS Exempts Enrolled Retirement Plan Agents From PTIN Requirement |
Comments Off on IRS Exempts Enrolled Retirement Plan Agents From PTIN Requirement |  Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Retirement Plans, Tax, Tax Qualification | Tagged: 401(k), accountant, Circular 230, CPA, Determination Letters, Employee Benefits, Fringe Benefits, investment advice, IRA, meal expense, plan qualification, Preparer Tax Identification Number, prohibited transactions, ptin, retirement plan, Retirement Plans, tax preparer, travel expense |
Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Retirement Plans, Tax, Tax Qualification | Tagged: 401(k), accountant, Circular 230, CPA, Determination Letters, Employee Benefits, Fringe Benefits, investment advice, IRA, meal expense, plan qualification, Preparer Tax Identification Number, prohibited transactions, ptin, retirement plan, Retirement Plans, tax preparer, travel expense |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 16, 2011
The American Bar Association Tort Trial & Insurance Practice Section recently appointed Solutions Law Press Managing Editor Cynthia Marcotte Stamer to serve as Vice-Chair Appointment of the Employee Benefits General Committee for the 2011-2012 fiscal year.
The TIPS Employee Benefits Committee concentrates on helping attorneys and others keep on top of and respond to developments in the constantly evolving practice area of employee benefits, with particular emphasis on litigation and regulatory compliance issues through programs, meetings, publications and other projects and activities. Additional information about involvement in the Employee Benefits Committee and its programs, publications and activities is available here.
A noted Texas-based employee benefits and employment lawyer with extensive involvement in the leadership of the ABA and other professional organizations involved in employee benefits, health care and workforce matters, is nationally and internationally known for her pioneering leadership and work as an attorney, consultant, policy advocate, speaker and author helping businesses, governments, and communities on health and other insurance and employee benefits, patient education and empowerment, wellness and disease management, and other programs, policies, and processes. For more than 24 years, Ms. Stamer’s legal practice has focused on advising and representing employers, insurers, health care providers, community leaders and governments about health care and employee benefits policy and process improvement, quality, performance management, education, compliance, communications, risk management, reimbursement and finance, and other related matters. In addition to her legal practice, Stamer also extensively consults and provides leadership to a broad range of clients, professional and civic organizations, and others on strategies for improving the health care system and the ability of health care providers, payers, employers, community organizations, government agencies to help patients and their families to access cost-effective, quality, affordable health care and other resource needs. She also has worked extensively with a broad range of business and government clients on health care, pension, social security, workforce, insurance and many other related policy matters.
In addition to her service with TIPS, Ms. Stamer also is active in the leadership of a broad range of other professional and civil organizations. For instance, Ms. Stamer presently serves as Executive Director of Project COPE, the Coalition on Patient Empowerment and the Coalition for Responsible Healthcare Policy; Vice President of the North Texas Healthcare Compliance Professionals Association; Immediate Past Chair of the American Bar Association RPTE Employee Benefits & Other Compensation Committee and its representative to the ABA Joint Committee on Employee Benefits and Vice Chair of its Welfare Benefits Committee; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; and as the Gulf Coast TEGE Council TE Committee Coordinator. She previously served as a founding Board Member and President of the Alliance for Healthcare Excellence, as a Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; the Board President of the early retirement intervention agency, The Richardson Development Center for Children; Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a member of the Board of Directors of the Southwest Benefits Association; on many seminar faculties and in many other professional and civic leadership and volunteer roles.
Author of the hundreds of publications and workshops these and other employment, employee benefits, health care, insurance, workforce and other management matters, Ms. Stamer’s insights on employee benefits, insurance, health care and workforce matters in Atlantic Information Services, The Bureau of National Affairs, HealthLeaders, Modern Healthcare, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other publications. She also regularly conducts training and speaks on these and other management, compliance and public policy concerns. Some recent publications and programs that may be of interest include:
For additional information about Ms. Stamer, upcoming training, publications or other materials or events, see here or contact Ms. Stamer directly via email here or (469) 767-8872.
IIf you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here. For important information concerning this communication click here. If you do not wish to receive these updates in the future, send an e-mail with the word “Remove” in the Subject to here.
©2011 Cynthia Marcotte Stamer, P.C. All rights reserved.
 Comments Off on ABA TIPS Section Appoints Cynthia Marcotte Stamer Vice Chair of Employee Benefits General Committee |
Comments Off on ABA TIPS Section Appoints Cynthia Marcotte Stamer Vice Chair of Employee Benefits General Committee |  Cafeteria Plans, COBRA, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, Fiduciary Responsibility, Health Plans, HIPAA, Human Resources, Insurance, Internal Controls, Malpractice, Medicare Part D, Mental Health, Mental Health Parity, Preemption, Prescription Drugs, Retirement Plans, Wellness, Wellness Programs |
Cafeteria Plans, COBRA, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, Fiduciary Responsibility, Health Plans, HIPAA, Human Resources, Insurance, Internal Controls, Malpractice, Medicare Part D, Mental Health, Mental Health Parity, Preemption, Prescription Drugs, Retirement Plans, Wellness, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 28, 2011
Assistant Secretary of Labor, Employee Benefits Security Administration (EBSA) Phyllis C. Borzi testified Tuesday, July 26, 2011 to the House Committee on Education and the Workforce Subcommitte on Health, Employment, Labor, and Pensions that EBSA a proposed fiduciary regulation that would update EBSA regulations defining when a person is considered a “fiduciary” by reason of giving investment advice for a fee with respect to assets of an employee benefit plan or IRA will help protect employee benefit plan participants by correcting “loopholes” in a “flawed 35-year-old rule” that allow many parties providing advice about the investment of retirement plan assets to escape coverage by ERISA’s fiduciary responsibility rules. The proposed regulations and other stepped up regulations and enforcement of ERISA’s fiduciary protections by the EBSA means that plan sponsors, fiduciaries, investment advisors and other plan service providers and others involved in the sponsorship, design, and administration of an employee benefit plan need to act to manage expanding fiduciary responsibilities and exposures.
- Borzi Says Loopholes & Other Flaws In Existing Regulations Hurt Plans & Their Participants
Borzi told the Committee that EBSA believes its rules about the types of advisory relationships that give rise to fiduciary status under the ERISA on the part of those providing investment advice services need to change because “technicalities” and “loopholes” in the current EBSA fiduciary regulations definition of “investment advisor” in effect since 1975 harms participants and beneficiaries by allowing many advisers to easily dodge fiduciary status.
Borzi testified that the five-part regulatory test used under the current regulations to determine when ERISA’s fiduciary requirements apply to “investment advice” and when the advisor is a “fiduciary” significantly narrowed the plain language of the ERISA statute so that much of what plainly is advice about plan investments is not treated as investment advice as fiduciary conduct under ERISA and the person paid to render that advice is not treated as an ERISA fiduciary.
Under current fiduciary regulation, an investment adviser is not treated as a fiduciary accountable for complying with ERISA’s prudence, exclusive benefit, prohibited transaction and other fiduciary responsibility safeguards if and when providing advice that meets each element of a five part test.
Under the current regulation, a person is a fiduciary under ERISA and/or the tax code with respect to their advice only if and when he or she:
- Make recommendations on investing in, purchasing or selling securities or other property, or give advice as to their value;
- On a regular basis;
- Pursuant to a mutual understanding that the advice;
- Will serve as a primary basis for investment decisions; and
- Will be individualized to the particular needs of the plan.
Borzi told members of Congress this narrow definition of investment advisor exempts a wide range of parties receiving compensation for providing advice about the investment of employee benefit funds from coverage by ERISA’s fiduciary responsibility requirements. Borzi testified that the narrowness of the existing regulation opened the door to serious problems, and changes in the market since the regulation was issued in 1975 have allowed these problems to proliferate and intensify. Borzi says the narrowness of the regulation has harmed some plans, participants, and IRA holders. Research has linked adviser conflicts with underperformance. SEC reviews of certain financial sales practices may also reflect these influences. Finally, EBSA’s own enforcement experience has demonstrated specific negative effects of conflicted investment advice.
- Borzi Says Proposed Regulation Would Strengthen Protections For Plans & Their Participants
Borzi said the proposed regulation published in the Federal Register on October 22, 2010 would change the rules defining a person is considered to be a “fiduciary” by reason of giving investment advice for a fee with respect to assets of an employee benefit plan or IRA by modifying the current regulation in effect since 1975 would replace the five-part test of “investment advisor” with a broader definition more in keeping with the statutory language while providing clear exceptions for conduct that should not result in fiduciary status.
According to Borzi, types of advice and recommendations that generally would trigger fiduciary status under the proposed regulations include: (1) appraisals or fairness opinions concerning the value of securities or other property; (2) recommendations as to the advisability of investing in, purchasing, holding or selling securities or other property; or (3) recommendations as to the management of securities or other property.
To be a fiduciary for performing these or other activities treated as fiduciary investment advice, Borzi explained that a person engaging in one of these activities must receive a fee and also meet at least one of the following four conditions:
- Represent to a plan, participant or beneficiary that the individual is acting as an ERISA fiduciary;
- Already be an ERISA fiduciary to the plan by virtue of having any control over the management or disposition of plan assets, or by having discretionary authority over the administration of the plan;
- Be an investment adviser under the Investment Advisers Act of 1940; or
- Provide the advice pursuant to an agreement or understanding that the advice may be considered in connection with investment or management decisions with respect to plan assets and will be individualized to the needs of the plan.
At the same time, Borzi testified that the proposed regulation recognizes that activities by certain persons should not result in fiduciary status. Specifically, these are:
- Persons who do not represent themselves to be ERISA fiduciaries, and who make it clear to the plan that they are acting for a purchaser/seller on the opposite side of the transaction from the plan rather than providing impartial advice;
- Persons who provide general financial/investment information, such as recommendations on asset allocation to 401(k) participants under existing Departmental guidance on investment education;
- Persons who market investment option platforms to 401(k) plan fiduciaries on a non-individualized basis and disclose in writing that they are not providing impartial advice; and
- Appraisers who provide investment values to plans to use only for reporting their assets to the DOL and IRS.
- EBSA Still Working To Address Expressed Concerns
The proposed regulation has prompted a large volume of comments and a vigorous debate. Borzi testified that the EBSA is working hard to hear and consider every stakeholder concern and shared some examples of how EBSA is considering addressing certain of these concerns. Borzi said EBSA is taking multiple steps in its effort to respond to these and other concerns in its efforts to finalize the regulation including:
Borzi told the Committee EBSA is working to better understand how specific compensation arrangements would be affected by the proposed rule and whether clarifications of existing prohibited transactions exemptions would be appropriate. Borzi said EBSA has already begun to issue subregulatory guidance describing some of these clarifications and will continue to do so as necessary as it completes its analysis.
Borzi also said that as EBSA further develops its thinking in this rulemaking, EBSA is paying special attention to the two primary exceptions to fiduciary status under the proposed rule: (1) clarifying the difference between investment education that does not give rise to fiduciary status and fiduciary investment advice; and (2) clarifying the scope of the so-called “sellers’ exception” under which sales activity is not fiduciary advice. In both cases, Borzi said EBSA intends to analyze and address the comments and concerns that were raised during our extensive public comment period.
Finally, Borzi said EBSA is exploring a range of appropriate regulatory options for moving forward, taking into consideration public comments submitted for the record, EBSA’s economic analysis, and relevant academic research. In so doing, Borzi told the Committee EBSA is aiming to address conflicted investment advice while not unnecessarily disrupting existing compensation practices or business models.
- Plan Sponsors, Fiduciaries, Service Providers Should Prepare For Tighter Rules While Continuing To Provide Input To EBSA
The proposed changes to the definition of investment advisor is one of many steps that EBSA is taking to tighten the regulations implementing ERISA’s fiduciary requirements and to enforce the protections of ERISA. The proposal to expand the conditions that providing investment advice regarding retirement plan assets will trigger the fiduciary protections of ERISA is designed to expand the reach of those regulations. Service providers involved in providing these or other related services generally will want to review and update their processes, documentation and training to manage new exposures likely to arise from these proposed regulations, while continuing to share feedback to EBSA and other rulemakers.
Service providers are not the only parties that need to update practices and provide input about these rules. Plan sponsors, fiduciaries, service providers, participants and beneficiaries also are impacted. Employers and other plan sponsors, fiduciaries and others need to anticipate and respond effectively to the inevitable efforts by providers of investment advice and other services to avoid or shift liability. Parties securing or relying on advice or services about investments or other responsibilities should:
- Carefully, prudently conduct a documented investigation and critical analysis of existing and proposed advisors and other service providers credentials, analysis, performance, contract, recommendations and other conduct;
- Carefully review contracts and other materials and secure appropriate constractual and other safeguards;
- Require indemnification, insurance and other protections;
- Ensure that appropriate action is taken to appoint parties intended to perform fiduciary advisory or other services to manage risks
- Secure and maintain appropriate fiduciary and other liability insurance coverage;
- Carefully conduct an appropriate, well-documented prudent review of performance, credentials and other relevant factors on a regular basis to preserve ongoing evidence of prudence; and
- Other appropriate safeguards to manage risks and liabilities.
To help guard and position themselves to defend against fiduciary exposures plan sponsors, fiduciaries, service providers and others involved in the administration of health or other employee benefit plans should seek the advice of legal counsel with appropriate experience with employee benefit and other related matters to develop an understanding of ERISA and other laws and the duties and liabilities that these rules may create for their organizations and themselves personally. For additional tips and information about managing these risks, see here.
For Help With These Or Other Risk Management Matters
If you need assistance in auditing or assessing, updating or defending your wage and hour or with other labor and employment, employee benefit, compensation or internal controls practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here. To unsubscribe, e-mail here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Borzi Tells House Committee Current Fiduciary Regs Flawed; Must Fix Loopholes In Investment Advisor Definition To Protect Plans |
Comments Off on Borzi Tells House Committee Current Fiduciary Regs Flawed; Must Fix Loopholes In Investment Advisor Definition To Protect Plans |  Bankruptcy, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Union | Tagged: 404, Director Liability, embezzlement, ERISA, Fiduciary, Fiduciary Responsibility, Officer Liability, Officers & Directors Liability, Owner Liability, Plan Sponsor Liability, Service Provider Liability, tpa |
Bankruptcy, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Union | Tagged: 404, Director Liability, embezzlement, ERISA, Fiduciary, Fiduciary Responsibility, Officer Liability, Officers & Directors Liability, Owner Liability, Plan Sponsor Liability, Service Provider Liability, tpa |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 20, 2011
The National Labor Regulations Board (NLRB)’s announcement of a settlement against a Connecticut nursing home operator this week in conjunction with a series of other enforcement actions highlight the need for businesses to tighten defenses and exercise other caution to minimize their organization’s exposure to potential NLRB charges or investigation. As reflected by many of these enforcement acts, the exposures arise both from active efforts by businesses to suppress union organizing or contracting activities, as well as the failure to identify and manage hidden labor law exposures in the design and administration of more ordinary human resources, compliance, business operations and other policies and practices.
On May 17, 2011, the NLRB announced here that Connecticut nursing home operator Spectrum Healthcare has agreed to settle a NLRB case involving multiple allegations of unlawful suspensions, discharges and unilateral changes in violation of the National Labor Relations Act and other federal labor laws by offering reinstatement and back pay to all discharged and striking workers and signing a new three-year collective bargaining agreement with its employees’ union, New England Health Care Employees Union District 1199, SEIU.
Along with the contract and reinstatement of all employees, the company agreed to pay $545,000 in back pay and pension benefits to employees who were harmed by the unfair labor practices, and to expunge any disciplinary records related to the case. As a result, all NLRB charges against the company have been withdrawn. Spectrum admits to no wrongdoing in the settlement.
The settlement, reached midway through a hearing before an NLRB administrative law judge in Connecticut and approved by the judge yesterday, ends a long-running dispute which grew into a strike by almost 400 employees at four nursing homes in Connecticut operated by Spectrum Healthcare, LLC. Complaints issued by the NLRB Regional Office in Hartford alleged that, beginning in the fall of 2009, several months after the prior collective bargaining agreement expired, Spectrum discharged seven employees and suspended three others to retaliate against their union activities and to discourage other employees from supporting the union. In addition, one employee was discharged and seven others were suspended after the employer unilaterally changed its tardiness discipline policy without first bargaining with the union.
The complaints further alleged that in April 2010, employees at the four nursing homes — in Derby, Ansonia, Winsted, and Hartford — went on strike to protest the unfair labor practices. When the strikers offered unconditionally to return to work in late August, the employer refused to take them back. Under federal labor law, if a strike is called because of an unfair labor practice, employees are entitled to reinstatement after an unconditional offer to return to work.
The reinstated employees are due to return to the facilities this week.
The Spectrum Healthcare settlement is reflective of the growing number of NLRB enforcement orders against employers generally and health care providers specifically under the Obama Administration. The Obama Administration has close ties and has expressed its strong and open support for union and union organizing activities. The adoption of a series of union friendly labor law reforms was one of the key campaign promises of President Obama during his election campaign. While other legislative priorities and the change in the leadership of the House of Representatives appears to have slowed efforts to push through this agenda, it has not slowed the Administration’s efforts to support unions with strong enforcement activities. Empowered by a difficult economic and job situation and an awareness of the Obama Administration’s strong support for union organizing and other activities, unions are stepping up organizing efforts and more aggressively challenging employers actions.
Over the past few months, public awareness of the Obama Administration’s aggressive enforcement agenda on behalf of unions has drawn new attention as a result of the widespread media coverage of NLRB actions challenging Boeings planned relocation of certain manufacturing jobs intervention in a planned relocation of certain manufacturing operations. See, e.g., Acting General Counsel Lafe Solomon releases statement on Boeing complaint; National Labor Relations Board issues complaint against Boeing Company for unlawfully transferring work to a non-union facility. However, the Boeing and Spectrum Healthcare actions represent only the tip of the iceberg of the rising number of NLRB enforcement activities, most of which take place with little media or public attention.
Along side the Spectrum Healthcare and Boeing actions, in recent weeks, the NLRB also has been busy with several other enforcement activities. For instance:
- On May 9 2011, the NLRB issued a complaint against Hispanics United of Buffalo (HUB), a nonprofit that provides social services to low-income clients, that alleges that HUB unlawfully discharged five employees after they took to Facebook to criticize working conditions, including work load and staffing issues. The case involves an employee who, in advance of a meeting with management about working conditions, posted to her Facebook ; and
- On May 17, the NLRB secured a temporary injunction from a U.S. District Court in San Jose California against San Jose area waste hauling company OS Transport LLC, charged with engaging in unfair labor practices including the termination of a lead organizer and another Union supporter, retaliation against Union efforts in the form of unfavorable assignments, threats to Union supporters, and promises of improved treatment of employees who disavow the Union for the alleged purpose of defeating a union. o offer reinstatement to two drivers and restore full assignments to other drivers who had expressed support for a union during an organizing campaign. More Details here.,
In addition, in recent weeks, the NLRB also has:
Amid this difficult enforcement environment, business leaders should exercise special care to prepare to defend their actions against both potential organizing efforts, to understand the types of actions and activities that may help fuel charges, and take steps to manage these and other union organization and other labor risks.
For Help With Labor & Employment, Employee Benefits Or Other Risk Management and Defense
If you need assistance in auditing or assessing, updating or defending your labor and employment, employee benefits, compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here .
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Spectrum Healthcare NLRB Charge Settlement Highlights Need To Defend Against Possible Unfair Labor Practices & Other Union Exposures |
Comments Off on Spectrum Healthcare NLRB Charge Settlement Highlights Need To Defend Against Possible Unfair Labor Practices & Other Union Exposures |  105(h), Absenteeism, ADA, Affirmative Action, Affordable Care Act, ARRA, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Claims Administration, COBRA, COBRA Subsidy, Corporate Compliance, Data Security, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, Excise Tax, Fair Labor Standards Act, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, H.R. 4872, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Malpractice, medical leave, Medicare Part D, Mental Health, Mental Health Parity, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Pandemic, Patient Empowerment, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Refunds, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Stimulus Bill, Swine Flu, Tax, Tax Credit, Tax Qualification, Telecommuting, Uncategorized, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs, Whistleblower | Tagged: ADAAA, Americans With Disabiltiies Act, Employer, employment discrimination, facebook, HR, Human Resources, NLRA, social medial, unfair labor practices, Union |
105(h), Absenteeism, ADA, Affirmative Action, Affordable Care Act, ARRA, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Claims Administration, COBRA, COBRA Subsidy, Corporate Compliance, Data Security, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, Excise Tax, Fair Labor Standards Act, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, H.R. 4872, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Malpractice, medical leave, Medicare Part D, Mental Health, Mental Health Parity, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Pandemic, Patient Empowerment, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Refunds, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Stimulus Bill, Swine Flu, Tax, Tax Credit, Tax Qualification, Telecommuting, Uncategorized, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs, Whistleblower | Tagged: ADAAA, Americans With Disabiltiies Act, Employer, employment discrimination, facebook, HR, Human Resources, NLRA, social medial, unfair labor practices, Union |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 10, 2011
Keeping on top of the employee plan guidance published by the Internal Revenue Service (IRS) and other relevant agencies can be critical to efforts of plan sponsors, fiduciaries, administrators and other service provider’s ability to anticipate plan design or other actions needed to maintain compliance or manage other concerns. The following is a recap of the more significant the IRS Employee Plan guidance published by the IRS between January 1 and March 31, 2011.
- Notice 2011-33, 2011-19 I.R.B.: Updates for the corporate bond weighted average interest rate for plan years beginning in April 2011; the 24-month average segment rates; the funding transitional segment rates applicable for April 2011; and the minimum present value transitional rates for March 2011.
- Notice 2011-22, 2011-12 I.R.B. 557: Updates for the corporate bond weighted average interest rate for plan years beginning in March 2011; the 24-month average segment rates; the funding transitional segment rates applicable for March 2011; and the minimum present value transitional rates for February 2011.
- Announcement 2011-21, 2011-12 I.R.B. 567: This announcement designates Form 8955-SSA, Annual Registration Statement Identifying Separated Participants With Deferred Vested Benefits, as the form to be used to satisfy the reporting requirements of §6057(a) of the Code for plan years beginning on or after January 1, 2009, and sets forth the due dates for filing the form for the 2009 plan year and subsequent plan years. .
- Notice 2011-19, 2011-11 I.R.B. 550: This notice provides guidance regarding when securities of the employer are readily tradable on an established securities market or readily tradable on an established market for purposes of certain provisions of the Internal Revenue Code relating to employer securities held by certain qualified retirement plans. .
- Announcement 2011-16, 2011-7 IRB 500: This announcement corrects a typographical error in Rev. Rul. 2011-3.
- Rev. Rul 2011-7, 2011-10 I.R.B.: This revenue ruling provides guidance clarifying how the section 403(b) plan termination provisions apply. .
- Announcement 2011-8, 2011-5 IRB 446: This announcement corrects an error in Rev. Proc. 2011-8 in the user fee schedule that applies to a non-mass submitter of a master or prototype (M&P) plan.
- Notice 2011-13, 2011-9 I.R.B. 529: Updates for the corporate bond weighted average interest rate for plan years beginning in February 2011; the 24-month average segment rates; the funding transitional segment rates applicable for February 2011; and the minimum present value transitional rates for January 2011.
- Notice 2011-7, 2011-5 I.R.B. 437: Updates for the corporate bond weighted average interest rate for plan years beginning in January 2011; the 24-month average segment rates; the funding transitional segment rates applicable for January 2011; and the minimum present value transitional rates for December 2010.
- Notice 2011-3, 2011-2 IRB 263: The notice provides guidance on the special rules relating to funding relief for single-employer defined benefit pension plans (including multiple employer defined benefit pension plans) under the Preservation of Access to Care for Medicare. Beneficiaries and Pension Relief Act of 2010 (PRA 2010), Pub. L. No. 111-192.
- Rev. Rul. 2011-3, 2011-4 I.R.B. 326: The covered compensation tables under Code §401 for the year 2011 are provided to determine contributions to defined benefit plans and permitted disparity.
- Rev. Proc. 2011-4, 2011-1 I.R.B. 123: Annual EP/EO revenue procedure on letter rulings.
- Rev. Proc. 2011-5, 2011-1 I.R.B. 167: Annual EP/EO revenue procedure on technical advice.
- Rev. Proc. 2011-6, 2011-1 I.R.B. 195: Annual EP determination letter revenue procedure.
- Rev. Proc. 2011-8, 2011-1 I.R.B. 237: Annual EP/EO revenue procedure on user fees.
For Help With These Or Other Risk Management Matters
If you need assistance in accessing, assessing or auditing, updating or defending your employee benefit or compensation arrangements and practices in response to this recent guidance or with other labor and employment, employee benefit, compensation or internal controls practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Recap of IRS Employee Plans 2011 1st Quarter Guidance |
Comments Off on Recap of IRS Employee Plans 2011 1st Quarter Guidance |  Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Tax, ERISA, Retirement Plans, Risk Management, Tax, Tax Qualification | Tagged: 401(k) Plan, 403(b) Plan, employee benefit plan, Employee Plan, IRS, plan qualification, Qualified Plan, retirement plan, Tax |
Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, Employment Tax, ERISA, Retirement Plans, Risk Management, Tax, Tax Qualification | Tagged: 401(k) Plan, 403(b) Plan, employee benefit plan, Employee Plan, IRS, plan qualification, Qualified Plan, retirement plan, Tax |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 4, 2011
Mitigate Risk With Appropriate Prevention, Monitoring & Response
Executives, board members, and other business leaders of companies providing health, 401(k) or other employee benefits under plans regulated by the Employee Retirement Income Security Act of 1974, as amended (ERISA) should heed a series of recent fiduciary liability settlement orders and lawsuits of the U.S. Department of Labor (Labor Department) as important reminders of the potential personal liability exposures executives can may face if their company’s benefit programs are not appropriately maintained and administered.
Recent Enforcement Actions, Changing Regulations Highlight Fiduciary Risks
On March 29, 2011, the Labor Department sued the owner of Eyeglass Factory, Inc. (EGF), Stephen Schaffer, for breach of fiduciary duties under ERISA by failing to ensure that EGF timely forwarded health plan contributions collected from employees to pay health plan contributions to the plan and failing to ensure that he and other plan fiduciaries and service providers were bonded in accordance with ERISA’s fidelity bond requirements.[i] The Labor Department suit charges that from July 1, 2000 to October 1, 2000, Schaffer and EGF withheld and failed to forward to the health plan contributions deducted from employee pay for health insurance coverage and contributions made to the flexible benefit plan sponsored by EGF from January 1, 2000 to December 4, 2000. The employees’ paycheck withholdings were commingled with the company’s general assets and used for its general operating expenses. The Labor Department is asking the court to order that Schaffer and other defendants make restitution to the plan for the misapplied contributions, including lost opportunity costs, to correct prohibited transactions and to appoint an independent fiduciary to oversee the plans once Schaffer is removed as the plan fiduciary.
The Schaffer suit follows the Labor Department’s successful prosecution of a breach of fiduciary duty action against Larry Lauterback, the president and former owner of a Minnesota Cement Company, for his role in allowing his construction company to commingle with company assets and divert to company use employee health and 401(k) contributions withheld from employee’s pay. In Solis v. Larry Lauterback, [ii] the District Court ordered Lauterback to restore $17,273.18 in unremitted employee contributions and lost opportunity costs to the company’s health and dental plan, and $747.20 in unremitted employee contributions to the company’s 401(k) plan and enjoins Lauterback from serving or acting as a fiduciary or service provider to any employee benefit plan for three years.. The order followed the entry of a consent judgment against Lauterback and the plan sponsor, Slate Cement, Inc., for failure to remit employee contributions, failure to forward employee contributions to medical and dental providers, co-mingling employee contributions of the general assets and using those assets for company operations.
The Schaffer and Lauterback actions taken in March, 2011 are only the most recent in a series of enforcement actions taken against business executives, board members, plan vendors and others for their role in committing or failing to take prudent steps to prevent or redress alleged misconduct relating to the maintenance, administration and funding of various employee benefit programs regulated by ERISA. In recent months and years, the Labor Department has filed several lawsuits against business executives and businesses for alleged breaches of fiduciary duties. While misuse of employee contributions by plan sponsors is a common focus of many of these actions, plan sponsors, plan service providers and members of their management with discretionary authority or responsibility over plan assets or administration or the election of those appointed to administer those responsibilities often arise out of the failure or these individuals to take prudent steps to prevent, monitor or address misconduct by other plan fiduciaries or service providers.[iii]
Plan sponsors, fiduciaries, service providers and their management should anticipate these risks and their attendant responsibilities will continue to rise as the Labor Department moves forward to adopt and implement revisions and enhancements to its fiduciary regulations such as those provided for in the new “Interim Final Regulation Relating to Improved Fee Disclosure for Pension Plans” scheduled to take effect in July, 2011 and the Proposed Regulation on the “Definition of the Term Fiduciary” published by the Labor Department in July and October, 2010 respectively.
Meanwhile, the Labor Department enforcement activities highlight the longstanding and ongoing policy of aggressive investigation and enforcement of alleged misconduct by companies, company officials, and service providers in connection with the maintenance, administration and funding of ERISA-regulated employee benefit plans. In its Fiscal Year 2010, the Labor Department closed 3,112 civil investigations, of which 2,301 (73.94%) resulted in monetary recoveries or other corrective action. The Labor Department referred 264 cases for civil litigation and filed 128 civil lawsuits. Meanwhile on the criminal side, the Labor Department closed 281 criminal investigations and obtained indictments against 96 people.
In addition to prosecutions brought by the Labor Department, companies and individuals that exercise discretion and control of the administration or funding of employee benefit plans regulated by ERISA also may be sued personally by participants and beneficiaries for breach of fiduciary under ERISA. A review of the Labor Department’s enforcement record and existing precedent makes clear that where the Labor Department perceives that a plan sponsor or its management fails to take appropriate steps to protect plan participants, the Labor Department will aggressively pursue enforcement regardless of the size of the plan sponsor or its plan, or the business hardships that the plan sponsor may be facing.
Plan Sponsors, Fiduciaries, Service Providers & Their Management Should Act To Manage Exposures
Given these exposures, businesses providing employee benefits to employees or dependents, as well as members of management participating in, or having responsibility to oversee or influence decisions concerning the establishment, maintenance, funding, and administration of their organization’s employee benefit programs need a clear understanding of their responsibilities with respect to such programs, the steps that they should take to demonstrate their fulfillment of these responsibilities, and their other options for preventing or mitigating their otherwise applicable fiduciary risks.
To help guard and position themselves to defend against these and other exposures, plan sponsors, fiduciaries, service providers and others involved in the administration of health or other employee benefit plans should seek the advice of legal counsel with appropriate experience with employee benefit and other related matters to develop an understanding of ERISA and other laws and the duties and liabilities that these rules may create for their organizations and themselves personally. For additional tips and information about managing these risks, see here.
For Help With These Or Other Risk Management Matters
If you need assistance in auditing or assessing, updating or defending your wage and hour or with other labor and employment, employee benefit, compensation or internal controls practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here. To unsubscribe, e-mail here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
[i] Chao v. Stephen Schaffer, the Eyeglass Factory, Inc., No O2-CV-60197, as announced in EBSA Release No. 11-341-CHI (March 29, 2011).
[ii] Solis v. Larry Lauterback, as announced in EBSA Release No 11-322-CHI (March 14, 2011).
[iii] See, e.g. Chao v. Associated Plan Administrators, as announced in EBSA Release No. 07-1265-BOS/BOS 2007-298 (October 16, 2007); Chao v. Starkey, as announced in EBSA Release No. 05-747-ATL (May 2, 2005); Chao v. Perry., as announced in EBSA Release BOS 2002-054 (March 21, 2002); Chao v. Mabry, as announced in EBSA Release No. 160 (March 20, 2002). See also, e.g., Baker v. Kingsley, 2006 WL 2027606 (N.D.Ill.2007); In Re Enron Corp Securities Derivative & “ERISA” Litigation, 284 F.Supp. 511 (S.D.Tex. 2003); Varity Corp. v. Howe, 516 U.S. 489 (1996); Brink v. DeLesio, 496 F. Supp. 1350 (D.Md. 1980).
 Comments Off on Plan Sponsors. Their Owners & Management & Others Risk Personal Liability If Others Defraud Plans or Mismanage Employee Benefit Plan Responsibilities |
Comments Off on Plan Sponsors. Their Owners & Management & Others Risk Personal Liability If Others Defraud Plans or Mismanage Employee Benefit Plan Responsibilities |  Bankruptcy, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Union | Tagged: 404, Director Liability, embezzlement, ERISA, Fiduciary, Fiduciary Responsibility, Officer Liability, Officers & Directors Liability, Owner Liability, Plan Sponsor Liability, Service Provider Liability, tpa |
Bankruptcy, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Professional Liability, Reporting & Disclosure, Restructuring, Retirement Plans, Risk Management, Union | Tagged: 404, Director Liability, embezzlement, ERISA, Fiduciary, Fiduciary Responsibility, Officer Liability, Officers & Directors Liability, Owner Liability, Plan Sponsor Liability, Service Provider Liability, tpa |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
February 25, 2011
TPA’s Embezzlement Guilty Plea Reminds Plan Sponsors, Fiduciaries & Service Providers To Ensure Fiduciaries, Administrators & Staff Prudently Selected, Monitored & Bonded
The guilty plea of an Ohio-based third-party administrator to embezzlement of $1 million in plan assets reminds employers and other employee benefit plan sponsors and members of their management participating in plan related activities, plan administrators and other plan fiduciaries and plan service providers (“plan decision-makers”) of the importance of ensuring appropriate, well-documented credentialing and selection, oversight, auditing and bonding the individuals and companies acting as fiduciaries and others participating in administration of plans or their assets (“plan workforce members”) to minimize their potential exposure to potential personal liability as a result of the fraud under the Employee Retirement Income Security Act (ERISA).
Cox Prosecution Reflective DOL Readiness To Prosecute Parties For Misuse of Plan Monies & Other Plan Fraud
According to a February 23, 2011 U.S. Department of Labor (DOL) announcement, Rhonda Sue Irvin Cox, owner of Irvin Administrative Solutions LLC (IAS), pleaded guilty to the embezzlement of $1 million of retirement plan assets from client plans administered by IAS. The DOL reports that between January 2003 and April 2007, Cox plead guilty to using used her position with ISC to embezzle the funds from 12 of 59 plans for which IAS served as a third party administrator. Cox also pleaded guilty to one count of making false statements in documents required under ERISA to be kept and certified by the plans’ administrator. Scheduled to be sentenced on June 1, 2011, Cox faces a maximum of five years in prison on each criminal count, a $250,000 fine and a special assessment. Cox is scheduled to be sentenced on June 1, 2011.
The DOL and Justice Department have a long-standing record of aggressive investigation and prosecution of embezzlement or other fraud impacting health and other employee benefit plans. Their criminal and civil enforcement and prosecution record makes clear this commitment remains strong.
Plan Sponsors, Fiduciaries & Service Providers May Face Civil Liability From When Others Defraud Their Plans
While plan decision-makers generally are aware that individuals defrauding health or other employee benefit plans risk criminal and civil prosecution, many fail to recognize their own potential civil liability exposures that may arise out of the fraudulent acts or other misconduct of another plan workforce member.
Embezzlement of plan assets is one of many acts of misconduct that can create potential fiduciary liability exposure for plan decision-makers under ERISA. Until confronted with potential fraud, misconduct or other misfeasance by a plan fiduciary, service provider or other plan workforce member, many plan decision-makers lack an adequate appreciation of the personal liability they may incur if they cannot demonstrate appropriate steps were taken to protect their health plan from this misconduct.
Under ERISA’s fiduciary responsibility rules, embezzlement or other misuse of employee contributions or other plan assets as well as certain other misconduct or misfeasance by a plan fiduciary, service provider or other plan workforce member can create personal liability exposures for plan decision-makers with responsibility or discretionary authority over the selection, retention, or management of plan workforce members if the plan decision-maker cannot demonstrate appropriate steps were taken to select, monitor and bond the plan workforce and other prudent action was taken to prevent and redress the fraud. Accordingly, health plans, their sponsors, fiduciaries, service providers, their management, and others serving as, or selecting, managing or retaining companies or individuals that participate in the handling of health plan assets or administration should act to strengthen their health plans and themselves against these exposures.
Risk Management Strategies & Tips
When embezzlement or other concern affecting their health plan arises, plan decision-makers concerned about protecting their health plans and themselves must act promptly in a carefully documented, prudent manner to investigate and respond to the concern. They should be prepared to present well-documented evidence of the scope and limits of their responsibility, authority, awareness, and potential for the selection, monitoring and oversight of the plan workforce member or others responsible for the performance of those actions, the adequacy of the bonding arrangements for the plan, and other efforts to prudently protect the plan before, during and after the discovery of the concern. While these and other steps can help strengthen the ability of a plan decision-maker to liability exposures that can result from the other plan workforce member’s embezzlement of plan assets or other misconduct, plan sponsors and plan decision-makers also should acquire suitable fiduciary and other liability insurance coverage and make other arrangements to help provide for the potential financial costs and other demands that are likely to arise in the event that it becomes necessary to investigate or redress fraud or other misconduct. Learn more here.
For Help With Investigations, Policy Review & Updates Or Other Needs
If you need help investigating or responding to fraud or other misconduct affection a health or other employee benefit plan, dealing with an employee benefit plan investigation or enforcement action by the Labor Department, private plaintiffs or another public or private party, reviewing current or proposed health plan processes or procedures, or responding to other employee benefit, labor and employment or other related controls and practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on HIPAA and other privacy and data security, health plan, health care and other human resources and workforce, employee benefits, compensation, internal controls and related matters.
For more than 23 years, Ms. Stamer has counseled, represented and trained employers and other employee benefit plan sponsors, plan administrators and fiduciaries, insurers and financial services providers, third party administrators, human resources and employee benefit information technology vendors and others privacy and data security, fiduciary responsibility, plan design and administration and other compliance, risk management and operations matters. In connection with this work, Ms. Stamer regularly counsels and helps clients to defend a broad range of clients about employee benefit plan fraud and other fiduciary responsibility concerns. Throughout her career, she has represented and served as special counsel to health and other employee benefit plans, plan sponsors, plan service providers, officers, directors and other management officials, bankruptcy trustees, debtors and creditors, and others in connection with health and other employee benefit plan fraud and other fiduciary responsibility and related investigations, prosecutions and other actions involving the Labor Department, IRS, HHS, Justice Department, state insurance and attorneys general, bankruptcy actions, and participant, beneficiary and vendor disputes. She also is recognized for her publications, industry leadership, workshops and presentations on these and other employee benefits, insurance and human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on health care, human resources, employee benefits, data security and privacy, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here. To unsubscribe, e-mail here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Avoiding Liability For Another’s Health Plan Fraud |
Comments Off on Avoiding Liability For Another’s Health Plan Fraud |  Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Malpractice, Professional Liability, Retirement Plans, Risk Management | Tagged: co-fiduciary liability, embezzlement, employee benefit, ERISA, Fiduciary Liability, fraud, Health Plan |
Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Malpractice, Professional Liability, Retirement Plans, Risk Management | Tagged: co-fiduciary liability, embezzlement, employee benefit, ERISA, Fiduciary Liability, fraud, Health Plan |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 21, 2010
The U.S. Department of Labor Employee Benefit Security Administration (EBSA) today published a Proposed Regulation that would expand the circumstances when individuals giving investment advice to an employee benefit or employee benefit plan or individual retirement account participant for purposes of the fiduciary definition of Employee Retirement Income Security Act (ERISA) § 3(21) and the prohibited transaction provisions of Internal Revenue Code (Code) § 4975(e)(3)(B).
If adopted as proposed, the Proposed Regulation would broaden the persons considered fiduciaries based on their provision of investment related advice or services to plans, participants or beneficiaries. Additionally, the restatement of these standards also likely will necessitate that both plan fiduciaries and providers of these services tighten agreements and other practices and procedures governing the engagement and delivery of services in order to maintain or protect desired allocations of fiduciary responsibility over these activities.
The deadline for individuals and organizations to comment on the proposed rule is January 19, 2011. Plan sponsors, fiduciaries, service providers and others concerned about the potential impact of the proposed changes should assess the potential implications of the rule and timely submit any comments or concern to the EBSA by this date.
To learn more about the Proposed Rule and its implications, see the more detailed article here.
If your organization needs assistance to evaluate or respond to the Proposed Regulation or reviewing, updating, administering or defending your employee benefit, human resources, compensation or internal control and risk management procedures, documentation, or policies or procedures, please contact the author of this update, Board Certified Labor & Employment attorney Cynthia Marcotte Stamer at (469) 767-8872 or via e-mail here.
Other Resources
If you found this information of interest, you also may be interested in reviewing other recent Solutions Law Press updates including:
About Ms. Stamer
Chair of the American Bar Association (ABA) RPTE Employee Benefit & Other Compensation Group, a Council Member of the ABA Joint Committee on Employee Benefits and Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Cynthia Marcotte Stamer is nationally recognized for her extensive work helping clients develop, implement and defend innovative, practical, legally defensible solutions to their particular health and other employee benefit, employment and insurance needs. Ms. Stamer has more than 23 years experience advising and representing employer, association and other plan sponsors, health and other employee benefit plans, their fiduciaries, plan administrators, consultants, vendors, outsourcers, insurers, governments and others about health plan and product design; administration, legal and operational risk management, vendor and fiduciary credentialing, managed care and vendor contracting, cost-containment, documentation, public policy, enforcement, privacy, technology, litigation and other concerns. Ms. Stamer also publishes, conducts client and other training, speaks and consults extensively on these and other health and managed care program concerns and practices for the ABA, American Health Lawyers Association, Institute of Internal Auditors, Society for Professional Benefits Administrators, HCCA, Southwest Benefits Association and many other organizations. Her insights on these and related topics have appeared in Atlantic Information Service, Bureau of National Affairs, World At Work, The Wall Street Journal, Business Insurance, Managed Healthcare, Health Leaders, various ABA publications and a many other national and local publications. To learn more about Ms. Stamer, her experience, involvements, programs and publications, see here or contact Ms. Stamer.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available for review here. If you or someone else you know would like to receive future updates and notices about other upcoming Solutions Law Press events, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here. For important information concerning this communication click here.
©2010 Cynthia Marcotte Stamer PC. Reprint Permission Granted To Solutions Law Press. All other rights reserved.
 Comments Off on DOL Proposes To Expand Investment Related Services Giving Rise to ERISA Fiduciary Status As Investment Fiduciary |
Comments Off on DOL Proposes To Expand Investment Related Services Giving Rise to ERISA Fiduciary Status As Investment Fiduciary |  Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Retirement Plans, Risk Management, Tax, Tax Qualification |
Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Retirement Plans, Risk Management, Tax, Tax Qualification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer



 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer 

You must be logged in to post a comment.