April 8, 2026
Human resources and other business leaders, using or allowing workforce members to CHAT-GPT or other artificial intelligence (“AI”) tools to research, make decisions or to support other activities should ensure that their organizations and their teams understand and manage the resulting evidentiary consequences and responsibilities these activities create.
In today’s AI age, Human Resources directors and other business leaders in increasingly are encouraged to turn to AI tools for a quick understanding of the law, drafting of documents, and a host of other human relations and business functions traditionally performed with the assistance of legal counsel. Although AI tools can be valuable under the right situations and properly used, the use of AI tools, along side of or as a substitute for legal advice obtained within the scope of attorney client privilege can carry a number of inherent risks and challenges. Human Resources and other leaders and their organization should carefully evaluate and manage these consequences before using AI.
AI Searches May Be And Create Evidence
AI prompts, outputs, and related metadata often qualify as discoverable electronically stored information (“ESI”) in litigation, regulatory audits, and enforcement proceedings.
Under the Federal Rules of Civil Procedure, discoverable information includes electronically stored information (ESI”) relevant to claims or defenses. See Fed. R. Civ. P. 26(b)(1); 34(a)(1)(A). Once litigation is reasonably anticipated, organizations must preserve relevant ESI under Federal Rules of Civil Procedure. See e.g.,Hoffer v. Tellone, 128 F.4th 433 (2d Cir. 2025).
AI searches and other interactions and the information and other outputs they produce generally qualify as ESI for purposes of the Federal Rules of Civil Procedure, Federal Rules of Evidence, (hereafter collectively the “Federal Rules”) and comparable federal and state litigation procedural rules.
Likewise, federal and state regulatory and enforcement agencies tend to consider AI and other ESI evidence covered by document retention and discovery rules.
Where applicable, these Federal Rules and agency rules generally include AI and other ESI evidence organizations must preserve, identify, and subject to discovery or other production like traditional evidence in litigation and agency audits and investigations.
ESI evidence generally includes any data stored in electronic form—such as emails, texts, spreadsheets, social media, and Internet of Things (“IoT”) data. As broadly construed by the courts, courts already long have admitted:
- Internet search histories;
- Internal chats and Slack messages;
- Draft documents; and
- Deleted files.
AI searches are simply the next evolution of this evidence category. AI records and information considered ESI can include;
- AI prompt histories;
- Generated outputs;
- Embedded AI-assisted drafts;
- Platform logs (if accessible); and
- Other records.
Organizations that fail to fulfill requirements for AI or other ESI early identification, data authentication and other requirements of Federal Rule of Evidence 902, the requirements of Federal Rule of Civil Procedure 37(e) regarding lost evidence, or other applicable requirements to preserve and produce ESI may result in sanctions, adverse inferences, and penalties under the Federal Rules. Similarly, organizations may incur evidentiary sanctions, regulator penalties, and other adverse consequences for failing to identify, retain and produce ESI from AI or other sources in government audits and investigations. Common sanctions include:
- Monetary sanctions;
- Evidence preclusion;
- Adverse inference jury instructions; and
- Other authorized sanctions.
See, e.g., Jones v. Riot Hosp. Grp. LLC, 95 F.4th 730 (9th Cir. 2024) (affirming dismissal as sanction for intentional destruction of ESI); Maziar v. City of Atlanta, No. 1:21-cv-02172, 2024 WL 197561 (N.D. Ga. June 10, 2024) (denying summary judgment and awarding fees based on loss of text messages); McBride v. Moore, No. 2:23-cv-02904, 2024 WL 1136429 (C.D. Cal. Feb. 23, 2024) (denying sanctions where ESI not shown lost or duty not triggered). Gregory v. State of Montana, No. 22-____ (9th Cir. 2024) (reversing sanctions imposed outside Rule 37(e); emphasizing Rule 37(e) as exclusive remedy for ESI spoliation); DR Distribs., LLC v. 21 Century Smoking, Inc., 513 F. Supp. 3d 839 (N.D. Ill. 2021) (recognizing financial prejudice from spoliation and awarding fees); Bistrian v. Levi, 448 F. Supp. 3d 454 (E.D. Pa. 2020) (Rule 37(e) provides exclusive framework for ESI spoliation); Fast v. GoDaddy.com LLC, 340 F.R.D. 326 (D. Ariz. 2022) (failure to preserve mobile device data warranted sanctions).
These and other related cases alert organizations that AI and other modern data sources are squarely within ESI. Courts treat AI, texts, mobile data, and app-based communications as discoverable ESI.
The precedent reflects that the best opportunity to position your organization to show the reasonability of the actions taken is through the existence and enforcement of policies before and during the use of the AI tool.ESI preservation obligations depend on foreseeability, control, and access to data. When deciding the consequences of the unavailability or failure to produce ESI, the determination regarding failure to take “reasonable steps” is fact-intensive. Of course, the failure to retain the documentation will be particularly likely to be found unreasonable where the party was under a statutory, regulatory, ethical, contractual, or other pre-existing obligation to preserve the evidence.
Also, courts require proof of intent to deprive before imposing the most severe adverse inference or dismissal sanctions, a lack of proof of intent to deprive the request requesting party of evidence does not mean there will not be consequences for the non-producing party. Negligent failure to retain and produce ESI and other evidence still carries consequences. Even without bad faith, courts may impose curative measures, fees, or evidentiary limitations.
Similarly, the U.S. Department of Justice Securities and Exchange CommissionDepartment of Health and Human Services Office for Civil Rights Equal Employment Opportunity Commission and other federal and state government agencies are increasingly sophisticated in digital evidence collection.
Among other things, organizations should be prepared to routine and produce documentation and data obtained, utilized, or otherwise interacting with AI tools and it’s associated meta-data and other components to respond to litigation and regulatory request for a broad range of data and information. Optimally the data captured and retained should include, but it’s not necessarily limited to:
- AI usage policies;
- Employee and other agent AI interaction records;
- Evidence of AI and other relevant governance and training; and
- Data protection controls.
Consequently, failure to govern, identify, preserve and produce AI-generated and AI-assisted records appropriately can expose organizations to spoliation sanctions, adverse inference instructions, regulatory penalties, loss of privilege protections, and expanded liability exposure.
In recognition of the possibility that AI tool interactions may give rise to obligations to retain and produce ESI evidence created as a consequence of that interaction, or organization should work with legal counsel to develop an administer appropriate practices to monitor, identify, retain, manage, and where necessary produce this ESI evidence.
AI Tools Create Evidence
Beyond considering and meeting documentation and other evidently protection, preservation, and production responsibilities, organizations and their human resources and other leaders need to recognize that the use of the tool itself and its outputs creates evidence that may give rise to legal opportunities, risks, and obligations for the organization.
Organizations should keep in mind that the use of AI tools creates legal evidently risks because AI tools typically generate synthesized responses (not just links) that often incorporate user inputs into outputs that may reflect user intent, knowledge, biases and opinions, and decision-making. This often makes AI interactions particularly valuable evidence for:
- Intent (e.g., “how to terminate employee without legal risk”) Knowledge (awareness of compliance obligations) State of mind (deliberate vs. negligent conduct);
- Knowledge (awareness of compliance obligations);
- State of mind (intentional, willful, or deliberate vs. negligent conduct)
The potential risks of this and other evidence is heightened by the fact that the evidence created may arise not only from the actions taken by the user of the AI tool, but also may be inherently built into the design of the AI tool itself or the databases or other reference materials that it accesses, not all of which may be transparent to the user or the organization that employs the user. These risks are further heightened when the AI tool use is not conducted internally within the organization by its employee, but rather is a tool utilized by a consultant or other third-party provider conducting activities of a sensitive nature on behalf of the organization, such as a recruiting company, investigation, company, or other service provider.
These unique characteristics of AI make it advisable that organizations recognize and manage potentially heightened exposures that employee or other agent use AI tools can produce for the organization in a wide range of sensitive areas.
Examples of queries that can become “smoking gun” evidence include but are not limited to:
- In employment or other workforce administration searches, AI queries such as “How to terminate employee with medical condition,” ‘How to avoid claims when, terminating older, disabled, complaining, injured or other employee with protected status, or the like can be evidence of discriminatory or other adverse intent;” or “How to beat a union organizing campaign;”
- Compliance & Regulatory searches such as “How to structure payments to avoid reporting requirements,” “HIPAA penalties for disclosure; searches about compliance or looking for compliance loophole; searches where company researched sanctions for noncompliance in areas involved in litigation or enforcement; or searches on risk management that could be evidence the organization saw but chose not to follow rules or standards or otherwise looked for or acted to circumvent compliance or disregarded interpretations less favorable to chosen challenged course of action;
- Litigation or Other Defense Strategy searches or tools such as “How to defeat a whistleblower claim,” “Ways to minimize damages in lawsuit” “Protecting your assets from IRS or in bankruptcy,” “How to conceal” or How to hide” orthe like can harm the organization’s interest by showing adverse intent, willfulness, or other motive or state of mind;
- Litigation case law, enforcement, argument drafting, or other actions that could reveal or provide insight on sensitive litigation strategies or their strengths or weaknesses;
- Financial & Tax searches such as “Aggressive tax strategies unlikely to be audited,” or “contract terms to reclassify employee to contractor,” “Structure transaction to avoid disclosure” or the like; and
- Other searches or tool uses that could reflect improper, intent, or document improper activities, such as how to hide evidence, how to create a bomb, how to poison somebody or that creates a record of conduct such as edits to revise data or documentation in reports or records, where the changes are tracked and retained.
Given these other risks, organizations should carefully consider and manage these and other risks when deciding whether, when, how and what AI tools their organizations allow their people to use, who gets to use what tools, designate and train those authorized to use these tools appropriately, and design and implement appropriate tools to track, capture, retain and manage these records of AI use and their implications. Optimally, the planning should identify and work to manage the creation and preservation of evidence and related AI ESI required or otherwise helpful to meet, applicable, regulatory, contractual, statutory, or other requirements in a manner that minimizes the creation of evidence that could call into question the compliance or other appropriateness of the organizations actors.
Privilege and Confidentiality Risks
Asking AI tools to answer legal questions or provide guidance in legal advice obtained within the scope of attorney. Client privilege also can enhance the exposure for the organization and it’s actors because of the implications of that Youts on the availability of attorney-client privilege for the activities and information obtained. Using AI tools and output also can have implications on the ability of an organization to protect legal advice and work product developed and shared within the scope of attorney privileges from discovery in judicial or regulatory actions. Organizations need to recognize risk to the confidentiality of legal advice or work product that entering sensitive legal questions or information into public AI tools not specifically designed and used outside the scope of the attorney-client relationship to avoid creating problematic evidence, disclosing discussions or work product that otherwise might qualify for protect against discovery in litigation or agency proceedings under the attorney-client privilege or attorney work product rules, or both.
Searches conducted by organization employees, consultants, or other agents or representatives about the law, strategies, or legal risks and consequences without or outside the scope of an attorney-client relationship generally can be discovered and used as evidence. Consequently, organizations should regulate the use by officers, directors, compliance officers, human resources directors, consultants, non-legal investigators and auditors and others of AI tools, internet or other searches to investigate the law or legal strategies independent of or outside the scope of attorney-client privilege.
Particularly risky scenarios include:
- In-house counsel, Human Resources, risk management or compliance staff using public AI tools;
- Employees seeking legal guidance outside approved channels;
- Consultants, contractors, and other vendors use of AI in performing tasks or tools;
- Embedded AI in software or other tools; or
- Uploading contracts, PHI, or proprietary data into AI systems.
Additionally, organizations and others communicating or working with legal counsel on behalf of the organization within the scope of attorney-client privilege to design strategies or investigate or defend actions generally should not use AI tools to conduct their own legal research or analysis without authorization and direction of the legal counsel to avoid forfeiting attorney-client privilege and work product protections.
If the required confidentiality is preserved, the attorney-client privilege and work product privileges rules can protect confidential communications between a client and its attorney and work product prepared for risk management, defense or other purposes of the legal engagement against disclosure in litigation or other proceedings in many circumstances. However these protections are lost if the communication or work product is disclosed to or discussed with third parties outside the attorney-client relationship. Entering factual information, conducting legal searches, or using AI tools outside the attorney-client relationship, not specifically designed to preserve confidentiality, or both to draft or evaluate legal documents, research, drafts, or strategies generally is considered a third party disclosure that can waiver or undermine the privilege for the specific information input to the AI tool as well as potentially related communications or work product.
For these and other reasons, organizations and individuals generally should resist the temptation to use AI tools to evaluate legal strategies, advice or work product.
Trade Secret, HIPAA and Other Data Privacy and Use Exposures
Human Resources and other leaders also must keep in mind their organization’s responsibilities to respect other organizations, intellectual property, to safeguard the confidentiality and security of data, and their organization’s need to protect its own intellectual property.
AI tool enthusiasts promote AI tools as substitutes for legal advice and other paid services. While asking AI to write a “free” policy or contract may seem a great way to save legal or other consulting, licensing or other costs, human resources and other leaders and their organizations must keep in mind that not all data, information and resources obtained through a ChatGPT or other AI search is shareware. Most nongovernmental data bases, contractual firms, tools, templates and other materials accessed through AI searches are or incorporate materials owned or subject to copyrights or other intellectual property protections of third parties. Unlicensed use of these resources can expose their organizations to copyright and other intellectual property infringement liability.
Furthermore, human resources and other executives choosing to use materials drafted using AI tools or otherwise acquired off of the Internet or other sources without legal advice to recognize that acquired materials and resources may not be currently compliant, appropriately tailored to their use, or contain other deficiencies for utilization in their organizations. These deficiencies can arise from a number of sources. For one thing, the queries input by the user may not be sufficiently tailored to adequately represent all of the material considerations necessary to tailor he organizations, questions, and the AI response to the needs of the organization. Also, because AI databases often times include a broad range of historical data, AI responses may rely upon outdated, legal or operational presumptions incorporated into these historical policies when they no longer are appropriate for use in your organization. Additionally, the response of AI may draw from a wide range of sources, including many of which may be sample policies not drafted by qualified individuals with adequate expertise to fully understand the legal and operational implications of the policy and properly draft a policy appropriate for use in the organization, acquiring the form or materials off of the Internet.
Beyond suitability of the information where tool obtained through the AI search itself, unlicensed use of the response, may expose your organization to liability for violating other organizations or authors, intellectual property rights. AI searches can and often do access and incorporate data and other resources protected by third party copyright,trade secrets, HIPAA or other confidentiality, or other safeguards. Accordingly, accessing or using data bases, sample language or forms, or other materials without proper licensing or attribution may trigger liability to individuals and organizations for breaches of these intellectual property rights.
A separate concern arising from the use of AI tools in HR and other business operations to evaluate, formate or otherwise process sensitive data also creates potentially serious risks when theof these tools involves allowing the AI tool to access or uploading the confidential or other sensitive information into the tool. Human resources and other leaders must exercise care not to share inappropriately and to help their organizations use policies and processes to prevent their people’s use of AI tools to avoid violating statutory, regulatory or contractual confidentiality requirements, compromising confidential information, their own or business partner’s trade secrets, proprietary information and other intellectual property, or both.
Furthermore, uploading or sharing trade secrets, Health Insurance Portability and Accountability (“HIPAA”) protected health information, confidential employee, tax or other regulated information, trade secrets or other confidential or sensitive data into AI tools or searches without proper controls may itself breach of HIPAA, trade secret, federal or state privacy laws (e.g., biometric, consumer data laws) or other statutory, regulatory, ethical or contractual data privacy or confidentiality obligations. Additionally, allowing AI tools to access and interact with electronic data or systems frequently triggers data and systems security obligations under HIPAA, the Fair and Accurate Credit Transactions Act, Equal Employment Opportunity and other Human Resources and benefits data, electronic crimes, federal and state government contract, and a broad range of international, federal and state cybersecurity laws and regulations, and other government and private contractual and program participation, statutes, and regulations.
Given these concerns, organizations should avoid using AI tools that require uploading customer, financial, sales, or other data or information that the organization considers its own trade secrets or proprietary information into AI data bases or tools that do not adequately safeguard the ownership and confidentiality of that information.
AI Tool Hallucinations and Other Output Deficiency Risks
AI tools and the output they produce are not always reliable. Among other things, certain AI tools are known to:
- Lack the ability to distinguish between more and less credible information sources;
- Create plausible-sounding but entirely fabricated facts, news articles, legal authorities, or academic citations;
- Create biased, false, incomplete, or inaccurate responses when models lack complete training data, are subjected to biased data, have limited context, ir under other circumstances;
- Create false positives such as I dentifying a threat (e.g., in fraud detection) that is not actually present.
- Fail to detect a real threat (e.g., in medical imagery) or report other false positives;
- Fabricate non-existent, fake information or other incorrect or inaccurate information; and
- Engage in hallucinations or other errors
The quality of the response, at best, often varies based on the quality and precision of the question asked. Lack of experience and careful structuring of the questions and inquiries made, lack of specialized knowledge necessary to structure the inquiry to be tailored to the specific needs at hand, and other limitations and concerns about the searches can undermine the accuracy, completeness and relevance of the AI tools output. Accordingly, response obtained by AI tools, often are unreliable and must be validated by a person experienced and skilled. The validation process should be conducted in such a matter that it preserves evidence that changes and responses are made based on thoughtful and reasonable determinations that the evidence obtained was not applicable or reliable, to minimize susceptibility to claims that decisions and actions were cherry picking based on improper intent rather than appropriate quality assurance processes. Organizations allowing the use of the tools and the individuals utilizing them need to understand and appropriately manage the very operational, legal in other risks of these deficiencies and error errors when utilizing AI tools.
Adopt And Enforce AI Policies To Manage AI Tool Use Responsibilities and Risks
Considering these and other responsibilities, human resources and other leaders and their organizations should use care to decide when, how, why, and by whom it allows AI tools to be used in or on behalf of its organization and provide appropriate steps to manage those uses in the resulting ESI to fill its legal obligations and manage its legal and operational risks. Because this process of itself could be evidence impacting, the organizations, legal exposures, organizations generally should work with qualified legal counsel within the scope of attorney-client privilege to work define and enforce policies and practices, to promote the organization’s legal and operational interests and manage the resulting legal obligations.
The author of this update, Cynthia Marcotte Stamer has decades of experience advising and representing governmental and private entities, AI and other technology, workforce and other legal and operational compliance, risk management and other operational and enforcement matters. If you have questions or need advice or help evaluating or addressing these or other compliance, risk management, or other concerns, contact her.
For More Information
We hope this update is helpful. For more information about these or other legal, contractual or operational compliance or risk management, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452-8297.
Solutions Law Press, Inc. invites you receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for her more than 35 years of health industry and other management work, public policy leadership and advocacy, coaching, teachings, and publications including leading edge work on workforce and other risk management and compliance.
Ms. Stamer’s work throughout her career has focused heavily on working with businesses domestically and internationally on employment, benefits, technology, data confidentiality, privacy, and security, and other Federal Sentencing Guidelines and other workforce management, regulatory and public policy and other legal and operational concerns.
Author of many highly regarded compliance, training and other resources on these and other operations, risk management, compliance and government affairs concerns, Ms. Stamer is widely recognized for her thought leadership and advocacy on these matters.
In addition, Ms. Stamer currently or previously served as the American Bar Association (“ABA”) Joint Committee on Employee Benefits OCR annual agency scribe and a Council Representative, International Section International Employment Law Committee Chair and International Life Sciences and Health Committee Chair, ABA TIPS Medicine and Law Committee Chair, ABA Health Law Section Managed Care & Insurance Interest Group Chair, former Vice President and Executive Director of the North Texas Health Care Compliance Professionals Association, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, and a host of other professional and civic leadership roles. She is a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her extensive publications and thought leadership as well as leadership involvement in a broad range of other professional and civic organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press™
Solutions Law Press™ provides health care, human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on health care, leadership, governance, human resources, employee benefits, data security and privacy, insurance, and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press™ resources.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general information and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation considering the specific facts and circumstances presented in their unique circumstance at the particular time. No comment or statement in this publication is to be construed as legal advice or admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law constantly and often evolves, subsequent developments that could impact the currency and completeness of this discussion are likely. The author and Solutions Law Press, Inc. disclaim and have no responsibility to provide any update or otherwise notify anyone of any fact or law specific nuance, change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2026 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Managing Evidentiary Consequences Of AI Use |
Comments Off on Managing Evidentiary Consequences Of AI Use |  Accommodation, ADA, adea, Age Discrimination, Antitrust, Attorney-Client Privilege, board of directors, Brokers, Civil Monetary Penalties, Civil Rights, Claims, Claims Administration, compliance, conflict of interest, Corporate Compliance, corporate governance, Cybercrime, Cybersecurity, Data Breach, Data breach, Data Security, defined benefit plan, defined contribution plan, Department of Defense, DFAR, directors, Disability, Disability Discrimination, Disability Plans, Discovery, Discrimination, Diversity, Drug Testing, EBSA, Education, EEOC, Electronic Medical Record, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Discrimination, Employment Policies, ERISA, Evidence, Executive Compensation, Fair Credit Reporting Act, Fair Labor Standards Act, Federal Sentencing Guidelines, FICA, Fiduciary Responsibility, FLSA, FMLA, GINA, Government Contractors, government employer, government plan, group health plan, health benefit, health Care, health insurance, HIPAA, HIPAA, Hiring, Human Resources, I-9, Identity Theft, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Licensing, Management, OFCCP, OFCCP, OSHA, Protected Health Information, Provider, provider contracting, Public Accommodation, Public Policy, Rehabilitation Act, Reporting & Disclosure, Retaliation, Risk Management, Safety, tpa, Union, Union certification, Worker Classification |
Accommodation, ADA, adea, Age Discrimination, Antitrust, Attorney-Client Privilege, board of directors, Brokers, Civil Monetary Penalties, Civil Rights, Claims, Claims Administration, compliance, conflict of interest, Corporate Compliance, corporate governance, Cybercrime, Cybersecurity, Data Breach, Data breach, Data Security, defined benefit plan, defined contribution plan, Department of Defense, DFAR, directors, Disability, Disability Discrimination, Disability Plans, Discovery, Discrimination, Diversity, Drug Testing, EBSA, Education, EEOC, Electronic Medical Record, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Discrimination, Employment Policies, ERISA, Evidence, Executive Compensation, Fair Credit Reporting Act, Fair Labor Standards Act, Federal Sentencing Guidelines, FICA, Fiduciary Responsibility, FLSA, FMLA, GINA, Government Contractors, government employer, government plan, group health plan, health benefit, health Care, health insurance, HIPAA, HIPAA, Hiring, Human Resources, I-9, Identity Theft, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Licensing, Management, OFCCP, OFCCP, OSHA, Protected Health Information, Provider, provider contracting, Public Accommodation, Public Policy, Rehabilitation Act, Reporting & Disclosure, Retaliation, Risk Management, Safety, tpa, Union, Union certification, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 14, 2025
Solutions Law Press publisher and attorney Cynthia Marcotte Stamer will discuss tobacco cessation class actions, health plan PBM, excessive fee, antitrust and other selected emerging health and disability plan litigation trends to watch in 2025 as part of the Welfare Plan Update at the American Bar Association Real Property, Probate and Trust Section Employee Plans and Executive Compensation Group will host during its free committee call on January 17, 2025, at 11:30 AM Central Time.
Along with Ms. Stamer’s comments, the Update also will include updates on the mental health partiy final rules and implications of the January 1, 2025 expiration of high deductible health plan telemedicine relief by her fellow Welfare Benefit Committee Co-Chair Jacquelyn M. Abbott and Committee Vice Chair Julia Mader.
Members interested in the meeting are invited to use the following Zoom credentials to connect to the meeting:
Join Zoom Meeting Link: https://americanbar.zoom.us/j/93409339280?pwd=aQcwUtePdkKni1943AJ4UjIaac6F5v.1
Meeting ID: 934 0933 9280, Passcode: 602434
One tap mobile
+13092053325,,93409339280# US
+13126266799,,93409339280# US (Chicago)
About Cynthia Marcotte Stamer
Board Certified in Labor and Employment Law by the Texas Board of Legal Specialization and a Fellow in the American College of Employee Benefits Counsel, Stamer is recognized for her decades of work on leading edge employee benefits, employment, health care and insurance concerns with recognition as a Martindale Hubble “Top Rated Lawyer” and “Legal Leader” in Health Care and Labor and Employment Law; as among the D Magazine “Best Lawyers In Dallas” in Labor & Employment, Tax: ERISA & Employee Benefits, Health Care and Business and Commercial Law.
Stamer has more than 35 years of experience guiding employers, health and other employee benefit and insurance programs and their fiduciaries, managed care, TPAs, PBMs, health care clearinghouses and their service providers; and other managed care and other health and health plan industry clients on program, product, systems and process design, administration, and defense; government and regulatory investigations and affairs; HIPAA and other data and systems privacy, cybersecurity and other integrity; workforce and other service provider credentialing, contracting, and management; government and private investigations, disputes, audits and enforcement; and other compliance, risk management and operations concerns in a wide range of contexts. Her work, and the interests of her clients are enhanced by her continuous involvement in federal and state legislative advocacy, regulatory affairs and government relations on these and other related concerns throughout her career.
In the course of this work, Stamer frequently advises and represents and defends health and other employee benefit plans, their fiduciaries, third party administrators, brokers, insurers, trustees and other plan service providers, debtor plan sponsors and their leaders, auditors, creditors and creditor committees, bankruptcy trustees, on prevention and mitigation of claims, fiduciary, licensing, prompt pay and other contractual, regulatory and other risks and liabilities arising from underfunded or distressed companies and employee benefit plans. She also advises employers, their boards, investors and management, third party administrators, preferred provider organizations, insurers and other plan service providers and others in fiduciary, claims and other audits, investigations and enforcement actions by private litigants, the Department of Labor, Department of Health & Human Services, Internal Revenue Service, Department of Justice, Federal Trade Commission, state insurance, attorneys’ general or other regulator, contractual arising out of workforce and staffing, employee benefit and insurance practices and programs in ongoing operations, corporate or credit transactions, bankruptcy or other situations and serves as special or consulting counsel for bankruptcy and other human resources, benefits, insurance, health care and regulatory compliance and investigation concerns. Stamer also counsels, represents and defends third party administrators, preferred provider and other managed care organizations, brokers and other regulated parties in state insurance and other regulators notice and reporting, investigations, audits, discipline and other enforcement actions.
Past Chair of the ABA RPTE Employee Benefit and Other Compensation Group, the Health Law Section Managed Care and Insurance Interest Group, and the Tort Trial and Insurance Section Medicine and Law Committee, Stamer also contributes her experience and knowledge by serving as Scribe for the American Bar Association (“ABA) Joint Committee on Employee Benefits (“JCEB”) annual agency meeting with the Department of Health and Human Services as well as a leader of employee benefits, human resources, health as an industry thought leader, Stamer also publishes and speaks extensively on health and other employee benefits, compensation, workforce, health care and related regulatory compliance and risk management matters.Her insights on these and other matters appear in publications of the American Bar Association, Bloomberg/BNA, Modern Healthcare, Aging In Place, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Stamer, her speaking, legal, consulting and other experience and services, or to access other publications by Stamer see CynthiaStamer.com or contact Stamer directly via e-mail or telephone (214) 452-8287.
For more details about the Real Property Probate and Trust Section Employee Benefits and Other Compensation Committee or other employee benefits related committees and activities of the American Bar Association, see the American Bar Association website here.
To receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here and connect with Stamer on Linkedin. For important information concerning this communication click here. If you do not wish to receive these updates in the future, unsubscribe by updating your profile here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides health care, insurance, human resources and employee benefit, data and technology, regulatory and operational performance, and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education. These include extensive resources on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general information and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation considering the specific facts and circumstances presented in their unique circumstances at the particular time. No comment or statement in this publication is to be construed as legal advice or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law constantly and often rapidly evolves, subsequent developments that could impact the currency and completeness of this discussion are likely. The author and Solutions Law Press, Inc. disclaim and have no responsibility to provide any update or otherwise notify anyone of any fact or law-specific nuance, change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2025 Cynthia Marcotte Stamer, P.C. Non-exclusive limited license to republish granted to Solutions Law Press, Inc.
 Comments Off on Stamer To Discuss Emerging Health and Disability Litigation Trends To Watch In January 17 Virtual Welfare Benefit Plan Update |
Comments Off on Stamer To Discuss Emerging Health and Disability Litigation Trends To Watch In January 17 Virtual Welfare Benefit Plan Update |  ACA, Claims Administration, Corporate Compliance, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, Fiduciary Responsibility, Fringe Benefits, health benefit, Health Benefits, health Care, health insurance, Health Plans, Managed Care | Tagged: business, Employment, Health, High Deductible Health PLan, Human Resources, news, Telemedicine |
ACA, Claims Administration, Corporate Compliance, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, Fiduciary Responsibility, Fringe Benefits, health benefit, Health Benefits, health Care, health insurance, Health Plans, Managed Care | Tagged: business, Employment, Health, High Deductible Health PLan, Human Resources, news, Telemedicine |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 27, 2024
With this week’s Thanksgiving celebrations kicking off the 2024 year-end holiday festivities, wise businesses will proactively act to reduce the risk that their business will start 2025 with a post-holiday workforce liability hangover.
Responsibly managed, company-sponsored and other social celebrations and activities can promote team building, morale, goodwill and other rewards. However, holiday celebrations, staffing disruptions, behaviors and their fallout also can often create attendance, discipline, compliance, safety and other legal and operational responsibilities, risks and costs. Wise business leaders act proactively to mitigate these risks as the nation enters holiday season begins.
Health & Safety
Gatherings, food, game playing, toasting with alcohol, travel and other aspects of company-sponsored and off-duty celebrations can enhance usual or create new accident and illness risks. Holiday socialization, presentism, distractions, staffing disruptions, operational changes and other factors can increase illness and accident risks. Injuries and illnesses suffered on or off the job can create added occupational health and safety and worker’s compensation responsibilities, costs and liabilities, disrupt staffing and productivity, and fuel health care, medical leave, disability, worker’s compensation and other responsibilities and expenses long after the holiday season ends. To help workers enjoy the Holidays safely and avoid these business costs and disruptions, businesses should confirm that their occupational health, safety and injury policies, practices, and staffing fulfill applicable occupational health and safety and workplace accident and injury laws, as well as consider encouraging workers to follow good health and safety practices on and off the job throughout the holiday season.
Employers generally have a duty of care under the Occupational Safety and Health Act (“OSH Act”) and other occupational health and safety laws to provide a safe work environment. The OSH Act requires businesses to recognize and take appropriate steps to keep their workplaces safe. The OSH Act, worker’s compensation, leave and other laws. OSH Act and other workplace safety laws generally require employers to promptly report and investigate workplace accidents and injuries, ensure workers receive timely treatment, and trigger occupational injury and other leave and other duties.
Workplace injuries resulting from unsafe workplace conditions generally trigger expensive penalties and damages, in addition to worker’s compensation or other occupational injury coverage liabilities. The holiday season often exacerbates or adds to the ongoing challenges employers face in maintaining workplace safety and responding to workplace injuries and accidents. Some common sources of additional risks associated with the holiday season include decreased oversight from management holiday absences, heightened worker fatigue and distraction, demand-driven, vacation or illness-related understaffing, expanded use of temporary or contract staffing, and holiday season-associated intoxication. See Holiday Workplace Safety. OSHA offers various recommendations to aid employers in recognizing and managing heightened workplace safety risks during the holiday season. Keeping Workers Safe This Holiday Season. To mitigate their risks from workplace injuries and accidents caused by safety violations and associated violations of investigation, reporting, benefit and other requirements, business leaders should ensure that their organizations identify and manage these additional risks, as well as ensure appropriate staffing and other arrangements are in place to ensure timely response, investigation and reporting of any workplace accidents or injuries during the holiday season.
With outbreaks of the flu, respiratory illnesses and other communicable or infectious diseases that spread from person to person common during the holidays, and holiday gatherings heightening the potential for transmission of the flu or other contagious diseases, businesses also should consider their responsibilities under the OSH Act or other laws to manage contagious disease exposures and spread. For instance, health care and certain other industries may be subject to laws or regulations that impose specific requirements for preventing and responding to contagious diseases, many of which may have been added or changed since the COVID-19 pandemic. Businesses should verify their policies meet or exceed current federal, state, local and contractual requirements as well as are designed to meet their business’ need to manage other contagious disease costs, absences and other disruptions.
Whether or not a business is subject to specific contagious disease management mandates, all businesses generally will benefit from reviewing and communicating their existing contagious disease and related leave and other workforce policies to workers and management to help protect their operations against the costs, operational disruptions and liabilities that often result from contagious disease outbreaks within their workplace. To enhance efforts to deter worker injuries and illnesses, businesses should consider using free resources like the Centers for Disease Control’s Healthy Habits to Prevent Flu and 8 Tips for a Safe and Healthy Holiday Season flyers, workplace posters, payroll stuffers and other communications to remind workers and their families to follow best safety and contagious disease prevention practices during the holidays.
Along with encouraging workers to stay healthy and safe during the Holidays, businesses should also consider providing documented reminders and take other steps to encourage workers to provide timely notice of illnesses and injuries and verify appropriate management coverage and arrangements to ensure that management team absences don’t disrupt the business’ timely delivery of Family and Medical Leave Act, occupational injury and other notifications, coverage for absences, provision of benefits, and other performance of other responsibilities in response to injury and illness reports despite holiday associated absences or hours of operation impacting the employing business or its responsible vendors.
Businesses also should verify their workplace safety, contagious disease and leave policies are designed and administered to prevent and mitigate exposure for unlawful OSH Act and worker’s compensation retaliation, disability discrimination against legally protected employees with chronic or other disabilities under the Americans with Disabilities Act (“ADA”), denial of leave or other violations of the Family and Medical Leave Act leave, notice and other requirements; and ADA and other privacy and confidentiality laws.
Alcohol & Other Conscious Altering Substance Consumption
The increased prevalence of holiday season celebrations and vacations often fuels an increase in consumption of alcohol, marijuana, and other consciousness-altering substances. This consumption can fuel a host of risks and headaches for businesses. Businesses concerned about these risks should act proactively to mitigate these risks.
When addressing business-related alcohol consumption, many businesses will want to consider not only alcohol and other conscious altering consumption at business-related events as well as potential costs that may arise from off-duty excess alcohol consumption. Whether resulting from on or off-duty consumption, excess alcohol, marijuana or other conscious altering consumption, whether on or off duty, can undermine productivity, create attendance and discipline issues, and fuel a host of other risks even when it does not result in a specific accident or injury.
Impaired judgment from alcohol or other intoxication in the workplace or at other events often fuels or contributes to employees or others exhibiting or subjecting employees to inappropriate sexual advances or other discriminatory statements, violent behavior, suicidal behavior or other problematic conduct requiring workplace investigations and discipline.
Most businesses also recognize that accidents caused by alcohol or other intoxication at work or work-related functions create substantial liability exposures for the company under the OSH Act and other occupational safety laws, as well as to workers and any third parties injured by a drunken employee, business associate, client or guest.
Businesses risk “dram shop” or other claims or other liability if employees or guests impaired by alcohol or other substances consumed at company-sponsored or associated events or operating company vehicles or equipment injure others.
Beyond this third-party liability, businesses also may incur significant worker’s compensation, health or disability benefit-related benefit costs if an employee is injured or injures another worker in an alcohol-related accident.
The potential headaches are even greater where the business is a health care, education, automobile sales, trucking and other transportation, or another business subject to or that has voluntarily adopted specific drug and alcohol-free, drug and alcohol testing and other related regulatory or contractual requirements. Businesses subject to these requirements should ensure appropriate arrangements for timely drug and alcohol testing, reporting, and other compliance with these requirements during the holiday season to avoid regulatory or contractual penalties for noncompliance. Companies administering substance abuse testing must comply with applicable mandates while also ensuring that their processes incorporate appropriate protocols to comply with disability discrimination, accommodation and confidentiality requirements of the Americans With Disabilities Act (“ADA”). See, e.g., ADA May Require Employers To Accommodate Employees Testing Positive For Legally Prescribed Medications
Also, because workers engaged in these industries generally risk loss of licensure, certification or other credentials required to perform their jobs for engaging in or failing to report certain alcohol or substance-related offenses or conduct, even off-duty consumption can create staffing headaches for an employer if a worker becomes temporarily or permanently disqualified to work as a result of a substance-related infraction. Consequently, businesses in industries affected by these heightened requirements have a heightened interest in educating and reminding workers to behave legally and responsibly when deciding if and when to consume alcohol or other conscious-altering substances.
Accordingly, virtually all businesses can benefit from encouraging employees to be responsible when consuming alcohol in both business and non-business functions and in planning and hosting holiday functions.
Businesses that serve alcohol at company functions or anticipate that employees will attend other business functions where alcohol will be served need to consider the potential liability risks that may result if the alcohol-impaired judgment of an employee or other guest causes him to injure himself or someone else. A company anticipates an employee or guest might consume alcohol at a company-sponsored or another business event and should adopt and enforce clear policies to prohibit and prevent individuals from over-imbibing and from driving under the influence. Many businesses also find it beneficial to suggest, require or offer at company expense alternate transportation for employees to use when leaving a company or business-related event where the employee consumed alcohol.
Businesses concerned with these liability exposures should take steps to manage the potential risks that commonly arise when employees, clients or other guests consume alcohol at company-sponsored events or while attending other business-associated festivities. To minimize these risks at company-sponsored events, many companies elect not to serve or limit alcohol consumed by workers and served to guests at company sponsored events and other business functions.
To help prevent intoxication from fueling inappropriate behavior at company celebrations where alcohol might be consumed or present, businesses, at a minimum, should remind employees that company policies prohibiting intoxication apply to company-sponsored social and business events. Some practical tips for hosting safe holiday gatherings include:
- Management and other leaders should communicate expectations and set a good example.
- Reduce opportunities for intoxication by prohibiting or restricting and monitoring the amount of alcohol available and served.
- Offer a plentiful supply of a variety of nonalcoholic drinks—water, juices, sparkling sodas. Nonalcoholic drinks provide guests with alternatives to alcohol. They also may help counteract the dehydrating effects of alcohol, slow the rate of alcohol absorption into the body and may reduce the peak alcohol concentration in the blood.
- Provide a variety of healthy foods and snacks. Food consumption can slow the absorption of alcohol and reduce the peak level of alcohol in the body by about one-third. Food can also minimize stomach irritation and gastrointestinal distress the following day.
- Encourage guests to help keep each other safe by monitoring and assign a team to monitor attendees for potential overconsumption or other signs of intoxication. With appropriate pre-consumption notification to attendees, some businesses even require or encourage attendees consuming alcohol to take a breathalyzer test before departure to minimize the risk that an intoxicated guest will be arrested or involved in an accident after departing the party.
- Help your guests get home safely by arranging reliable transportation by using designated drivers and taxis. Anyone getting behind the wheel of a car should not have ingested any alcohol.
Because holiday-associated alcohol consumption and other stresses also tend to fuel increased depression, domestic violence and other stress-associated behaviors, many businesses also find it beneficial to redistribute information about employee assistance programs (EAPs).
Businesses also may want to review the adequacy of existing health, disability, accident and dismemberment, group legal services and other benefit programs, liability insurance coverage and employment policies to protect and promote the company’s risk management and workforce coverage objectives. Businesses can experience unfortunate surprises if they don’t anticipate the implications of these provisions on their employment policies, leave and benefit, safety and other workplace programs and liability insurance and indemnification obligations and costs. Maintaining and reminding workers about policies regarding alcohol consumption or intoxication, accident and traffic offense notifications, privacy waivers, or other policies enhancing accident investigation and response, or other strategic policies can help deter and facilitate investigation and response to on and off-duty accidents or other risk-creating events.
Many employee assistance (“EAP”) health and disability programs incorporate special provisions affecting injuries arising from inappropriate alcohol use as well as offer coverage and benefits to aid employees and family members affected by mental health or substance abuse-related conditions. Changes in regulatory mandates and expanded enforcement of federal group health plan mental health and substance abuse coverage mandates make it important to ensure that employment-based health coverage complies with these requirements. Similarly, many businesses increasingly qualify for preferential rates or discounts on liability policies based upon representations that the business has in effect certain alcohol and drug use or other risk management policies and practices. Reviewing these policies now to become familiar with any of these requirements and conditions can also be invaluable in helping a business respond effectively if an employee or guest is injured in an alcohol-related accident.
Discrimination & Harassment Liability Risks
Businesses should also manage exposures to religious, sex and other discrimination risks linked with the holiday season.
Businesses should critically review their scheduling and other holiday season plans and practices for potential prohibited discrimination or other insensitivity. Businesses should use care to handle carefully requests for religious-based scheduling changes, particularly in light of changes in judicial precedent and regulations in recent years. Leave policies should disclose policies for scheduling and holiday leave clearly and include appropriate, updated policies and procedures for requesting religious accommodation. Companies also should consider seeking advice from legal counsel before denying a faith-based request for a schedule change in light of the latest guidance or recent court decisions precedent.
Business-sponsored or connected holiday or year-end parties, communications, gifts, and other December festivities and observances should be designed to reflect appropriate sensitivity to sexual harassment and religious and other cultural diversity risks. Businesses should exhibit sensitivity and alert their workforce to their expectation that members of their workplace exhibit respect and sensitivity to differences in religious practices and observances among their employees, business associates and friends. Management and other workers should use care to plan social gatherings to be inclusive and to accommodate differences in cultural, religious and other differences. Businesses also should be sensitive to the potential that workers of alternative faiths may feel discriminated against if holiday observances focus unduly on a particular religion to exclude their faith. Businesses also should use care to manage other discrimination exposures in the planning of holiday festivities, gift exchanges, and other activities. Businesses also should be vigilant in watching for signs of inappropriate patterns of discrimination in the selection of employees invited to participate in company-connected social events and off-duty holiday gatherings sponsored by managers and supervisors.
A good starting point is reminding employees, business partners and customers that the company expects employees, business partners and other guests to adhere to company rules against sexual harassment, religious and cultural and other inappropriate discrimination at company-sponsored and other gatherings involving other employees or business associates. Businesses also should remind employees that the company does not expect or require that employees submit to unwelcome sexual, religious, or other inappropriate harassment or discrimination when participating in parties or other social engagements with fellow employees, customers or other business partners and of the procedures to follow to report any concerning events. Even a simple e-mail reminder to employees that the company expects them to be familiar with and comply with these policies and can help promote compliance and provide helpful evidence if an employee or other celebrant steps over the line.
To enhance the effectiveness of these reminders, a business should consider adopting and sharing specific guidance to educate workers about its policies, including examples to illustrate company-sponsored and other off-duty holiday-associated activities of particular concern.
Businesses also should recognize that whether or not company-sponsored, the fraternization inherent in holiday parties and other celebrations where employees celebrate with other employees, clients, suppliers or other business associates can lower inhibitions and obscure the line between appropriate and inappropriate social and business behavior. With or without alcohol, some employees, clients or business associates may misinterpret the festive social atmosphere of holiday celebrations. Some employees, clients or business associates make unwelcome sexual advances, make sexually suggestive or other inappropriate statements, or engage in other actions that expose the business to sexual harassment or other employment discrimination, harassment or retaliation liability. To help deter inappropriate or risky conduct, businesses should consider providing reminders that company prohibitions and rules about sexual harassment, discrimination, fraternization and other inappropriate conduct remain in effect during the holiday season, including when planning or attending holiday celebrations or other events hosted by the business, business partners and clients, and even private management sponsored events and observances.
Gift Giving, Gratuities & Social Entertainment
The exchange of social invitations, gifts and gratuities during the holiday season or at other times throughout the year also can raise various concerns. Businesses should adopt and communicate clear policies and procedures governing both giving and receiving social invitations, gifts, and other benefits. Businesses should review applicable governmental regulations, contractual requirements, and customer and vendor policies for requirements that could impact the offering, receipt, reporting or other handling of gifts, social invitations or other activities. Businesses also should design policies to ensure that they collect and retain sufficient documentation from employees, officers, consultants, customers, and vendors to monitor compliance and other legal and operational risks associated with social entertainment, gifts, and other similar benefits, to report tax deductions and income arising from these activities appropriately, and to meet other compliance obligations. Businesses should review and update current business policies affecting social entertainment, gifting and other similar activities for opportunities to promote compliance and mitigate risks.
As with other holiday observances, all gifts, gratuities and social entertainment must adhere to applicable laws, regulations and company policies regarding bribery, conflict of interest or other inappropriate inducements or rewards. Companies should implement and enforce appropriate policies for the offering and provision of and recordkeeping and reporting of these perks.
Gifts, gratuities and entertainment practices also must not discriminate inappropriately based on sex, religion or other protected status and must reflect appropriate sensitivity to potential religious, sex, race, or other protected status. A business that anticipates workplace or work-connected private festivities might include white elephant or other gift exchanges may wish to specifically include a reminder to exercise care to avoid selecting a gift that may be sexually suggestive, insensitive to religious, cultural or other differences or otherwise offensive.
Businesses also should confirm that all applicable tax implications arising from the giving or receiving of gifts are appropriately characterized, documented and reported in accordance with applicable tax, referral, conflict of interest and other requirements.
In addition to ensuring proper tax documentation and reporting, businesses also need to ensure and retain documentation of the propriety of invitations, gifts and other benefits. Social entertainment and gift-giving activities intended to show appreciation or support marketing efforts can create significant legal or relationship risks if not properly tailored to avoid regulatory or contractual prohibitions or appearances of impropriety. Government contractors, government officials, health care providers, nonprofits, public companies and an amazingly broad range of other entities often must comply with specific statutory, regulatory, contractual or ethical requirements affecting the giving or receiving of invitations, gifts or other preferences. An ill-conceived social invitation, gift, or other benefit that violates these restrictions may expose both givers and recipients to legal prosecution, program disqualification and other serious legal risks.
In addition to these externally imposed legal mandates, many businesses have established their own conflict of interest, social entertainment, gift giving or other policies to minimize the risk that employee loyalty or judgment will be comprised by gifts offered or received from business partners or other outsiders. Employees, officers and contractors of businesses maintaining these policies may face termination or other significant discipline for violating these requirements. Accordingly, businesses offering social invitations, gifts and other benefits to valued vendor or customer relationships risk must be sensitive to these organizationally imposed requirements.
Timekeeping, Performance, Attendance & Time Off
Businesses also commonly face a range of year-end timekeeping, attendance and time off, pay, compensation and productivity concerns. The winter cold and flu season and other post-celebration illnesses, vacations, and winter weather inevitably combine to fuel a rise in absenteeism and competing requests for time off during the holiday season. Improperly designed or out-of-date timekeeping and reporting, leave and attendance, investigations, privacy and other workplace policies can exacerbate management of these challenges and their costs. Further complications can arise when dealing with employees suspected of mischaracterizing the reason for their absence or otherwise gaming the company’s time off policies. Meanwhile, performance and productivity concerns also become more prevalent as workers allow holiday shopping, personal holiday preparations, and other personal distractions to distract their performance.
Managing staffing needs and tracking and administering timekeeping, overtime and other pay, paid and unpaid time off and other attendance, compensation and absence administration while maintaining compliance with legally protected or other legitimate requests for excused time off by employees can present major headaches for businesses and their management. Recent changes in federal, state and local paid and other protected leave mandates add additional traps for the unprepared. Businesses concerned with these challenges ideally will review their policies and practices to ensure their organizations have in place well-designed policies and practices concerning timekeeping, overtime and other pay, attendance and time off, productivity and performance that comply with the Fair Labor Standards Act and other compensation, timekeeping, leave, reporting, investigations, privacy and other federal, state and local laws. Businesses should exercise care when addressing productivity and attendance concerns to investigate and document their investigation before imposing discipline. Businesses also should ensure that their policies are appropriately and even-handedly administered. They also should exercise care to follow company policies, to maintain time records for non-exempt workers, to avoid inappropriately docking exempt worker pay, and to provide all required notifications and other legally mandated rights to employees taking medical, military or other legally protected leaves. In the event it becomes necessary to terminate an employee during December, careful documentation can help the business to defend this decision. The increasing prevalence of worker classification challenges by federal and state agencies and plaintiff’s attorneys also makes it important for businesses to take steps to require and preserve access to documentation be able to demonstrate compliance with these and other applicable legal obligations by staffing and other contract labor suppliers.
Timely Investigation, Notification & Reporting
Businesses faced with allegations of discrimination, sexual harassment or other misconduct or potential business liabilities arising during holiday seasons should also take steps to ensure that appropriate staffing and other arrangements to ensure their organization’s ability to promptly investigate, if necessary, take appropriate corrective action to address complaints or other concerns arising during the holiday season around management or other time off.
Delay in investigation or redress of accidents, discrimination or other concerns can increase the liability exposure of a business presented with a valid complaint and complicate the ability to defend charges that may arise against the business. Additionally, delay also increases the likelihood that a complaining party will seek the assistance of governmental officials, plaintiff’s lawyers or others outside the corporation in the redress of his concern.
If a report of an accident, act of discrimination or sexual harassment or other liability related event arises, businesses should take steps to ensure that management responsible for responding to these and other occurrences are property trained or otherwise supported to carry out these responsibilities in an appropriate, defensible manner as well as to provide timely notification as needed to any government entities, contract partners, insurers, agencies or other parties. Injuries occurring at company related functions often qualify as occupational injuries subject to worker’s compensation and occupational safety laws. Data breaches and various other events may trigger notification or other disclosure obligations to meet statutory, contractual or other requirements. Likewise, automobile, cyber, employment practices and other liability policies often require covered parties to notify the carrier promptly upon receipt of notice of an event or claim that may give rise to coverage, even though the carrier at that time may not be obligated to tender a defense or coverage at that time. Ensuring appropriate, timely response can play a critical role in promoting defensibility, mitigating liability or preserving coverage or indemnification rights.
For Help With Investigations, Policy Updates Or Other Needs
If your organization would like to learn more about the concerns discussed in this update or seeks assistance auditing, updating, administering or defending its human resources, compensation, benefits, corporate ethics and compliance practices, or other performance-related concerns, please contact management attorney and consultant Cynthia Marcotte Stamer.
An attorney Board-Certified in Labor and Employment Law by the Texas Board of Legal Specialization, Ms. Stamer’s work focuses on helping management manage performance, legal compliance and operational risks.
For more than 35 years, Ms. Stamer’s work has advised businesses and business leaders about enhancing the effectiveness and defensibility of their operations using employment and other workforce and services management, employee benefits, compensation, performance management, contracting, Federal Sentencing Guideline and other compliance and risk management, investigations, and other legal and operational tools and solutions. While helping businesses define and manage the conduct and performance of their employees, contractors and vendors, she also assists employers and others with compliance with federal and state equal employment, compensation, health and other employee benefits, workplace safety, leave, and other labor and employment, privacy and data security, and other laws, advises and defends businesses against labor and employment, employee benefit, compensation, fraud and other regulatory compliance and IRS, Department of Labor, Department of Justice, SEC, Federal Trade Commission, HUD, HHS, DOD, Departments of Insurance, Department of Health, Department of Agriculture and other federal and state regulators.
Ms. Stamer also speaks, coaches management and publishes extensively on these and other related matters.
Her work, thought leadership and scholarship on helping organizations manage people, operations and risk have earned her recognition as a Fellow in the American College of Employee Benefit Counsel, a “Top Woman Lawyer,” “Top Rated Lawyer,” and “LEGAL LEADER™” in Labor and Employment Law and Health Care Law; a “Best Lawyers” in “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law.”
For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
Other Helpful Resources & Information
If you found this article of interest, you also may be interested in reviewing other Breaking News, articles and other resources like:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here. For important information concerning this communication, click here. If you do not wish to receive these updates in the future, unsubscribe by updating your profile here.
NOTICE: These materials are for general informational and educational purposes only. They do not establish an attorney-client relationship, are not legal advice, a substitute for legal advice, an offer or commitment to provide legal advice or an admission. The information and statements in these materials may not address all relevant issues or apply to any particular situation or circumstances. The author reserves the right to qualify or retract any of these statements at any time. and does not necessarily address all relevant issues. Because the law evolves, subsequent developments could impact the currency and completeness of this discussion. The author disclaims and has no responsibility to provide any update or otherwise notify anyone of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers are urged to engage competent legal counsel for consultation and representation at any time, considering the specific facts and circumstances presented in their unique circumstances. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from using this publication. Readers acknowledge and agree to the conditions of this Notice as a condition of their access to this publication. Circular 230 Compliance. The following disclaimer is included to comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein. ©2024 Cynthia Marcotte Stamer. All rights reserved.
 Comments Off on Workforce Strategies For Avoiding Holiday Liability Hangovers |
Comments Off on Workforce Strategies For Avoiding Holiday Liability Hangovers |  ADA, Civil Rights, compliance, Corporate Compliance, directors, Disability, Disability Discrimination, Disability Leave, Disability Plans, Discrimination, Drug & Alcohol, Drug Testign, Drug Testing, EEOC, Emergency, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, family leave, FLSA, FMLA, FMLA, Fringe Benefits, health benefit, Health Benefits, Health Plans, HR, Human Resources, Leave, medical leave, Overtime, religious accommodation, Religous Discrimination, Risk Management, Safety, Sex Discrimination, Sexual Harassment, Worker, Workers' Compensation, workfirce, Workforce, workplace violence | Tagged: ADA, Discrimination, Drug Testing, Employee Benefits, Employer, Employers, Employment, employment law, Health Insurance, Health Plan, Health Plans, holidays, Human Resources, Labor, OSHA, Safety, workers comp |
ADA, Civil Rights, compliance, Corporate Compliance, directors, Disability, Disability Discrimination, Disability Leave, Disability Plans, Discrimination, Drug & Alcohol, Drug Testign, Drug Testing, EEOC, Emergency, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, family leave, FLSA, FMLA, FMLA, Fringe Benefits, health benefit, Health Benefits, Health Plans, HR, Human Resources, Leave, medical leave, Overtime, religious accommodation, Religous Discrimination, Risk Management, Safety, Sex Discrimination, Sexual Harassment, Worker, Workers' Compensation, workfirce, Workforce, workplace violence | Tagged: ADA, Discrimination, Drug Testing, Employee Benefits, Employer, Employers, Employment, employment law, Health Insurance, Health Plan, Health Plans, holidays, Human Resources, Labor, OSHA, Safety, workers comp |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 17, 2023
Out-of-state employers, insurers, employee benefit plan vendors, and other businesses registered to do business in Pennsylvania, Georgia, Iowa, Kansas, Minnesota, or another state that requires that out-of-state businesses consent to jurisdiction as a condition of their registration to do business in the state face a heightened risk of getting hauled into court in the consent to jurisdiction state following last month’s Supreme Court decision in Mallory v. Norfolk Southern Railway Company, 600 U. S. ____ (2023) even if none of the events giving rise to the lawsuit took place in that state.
The Mallory ruling arose from a state lawsuit filed in Pennsylvania state court seeking damages by Robert Mallory (“Mallory”) to recover damages for cancer the argued was caused by the negligence of his former employer, Norfolk Southern Railroad (“Norfolk”) pursuant to the Federal Employers’ Liability Act workers’ compensation scheme that permits railroad employees to sue for injuries caused by employer negligence. Mallory filed the suit in Pennsylvania, a jurisdiction with no real connection to the claims but noted for its favorability to plaintiffs even though he never worked for Norfolk in Pennsylvania. Mallory only worked for Norfolk in Ohio and Virginia, was a Virginia resident at the time of the suit, and only briefly lived in Pennsylvania after leaving Norfolk’s employment before returning to live in Virginia. Given the lack of connection of Pennsylvania to the parties and events giving rise to the claim, Virginia-based Norfolk Southern moved for the dismissal of the Pennsylvania lawsuit for lack of the requisite “substantial minimum contacts” generally required to support personal jurisdiction.
While courts generally recognize and enforce contractual agreements by a party to consent to jurisdiction, mere registration of an out-of-state business to do business in a state historically has not been recognized as creating the necessary “substantial minimum contacts” that the Due Process clause of the United States Constitution generally requires exist to provide the general personal jurisdiction that must exist for a state court to possess jurisdiction to decide a lawsuit over the out-of-state business under the Supreme Court precedent first articulated in International Shoe Co. v. Washington, 326 U. S. 310 (1945)
Because Pennsylvania is one of five states that currently requires all out-of-state businesses registering to do business in the State to consent to be sued in the state as a condition of registration, however, Mallory argued and the Supreme Court agreed in Mallory that Norfolk waived its ability to object to personal jurisdiction when it registered to do business in the Commonwealth.
In Mallory, the Supreme Court Majority ruled that any corporation registered to do business in a state which requires out-of-state businesses to consent to general personal jurisdiction waives its right to assert a Due Process challenge to jurisdiction in that state. Accordingly, businesses registering to do business in a consent-to-jurisdiction registration state should anticipate that their mere registration with the state likely subjects the business to the jurisdiction of courts in that state even if the business has not entered into a contractual agreement to submit to that state’s jurisdiction or otherwise engage in other actions establishing the required substantial minimum contacts to satisfy the International Shoe Due Process standards even if none of the events underlying the lawsuit took place in that state.
Given the Supreme Court’s Mallory decision, businesses should take into account the potential risks of being subjected to out-of-state litigation and regulation anytime the business expands operations into, registers to do business as an out-of-state business or signs an agreement consenting to jurisdiction into a state other than their primary place of business. As evidenced by Mallory, businesses generally should consider and take steps to manage the risks of allowing the creation of jurisdiction against their business in states other than the primary location in which the business operates. Businesses subject to jurisdiction in a state generally become subject to laws, regulations, and lawsuits in that state. Aside from added obligations and costs associated with being subject to the laws of another state and conducting litigation in an unfamiliar state, businesses subject to the jurisdiction of laws in courts in multiple states open the door for opposing parties to strengthen their position by foreign shopping. Like Mallory, disgruntled current or former employees, plan members, or other opposing parties in disputes may choose to file their lawsuit in the state with the laws, rules, or precedent most favorable to their position even where the dispute does not arise out of events occurring in the chosen state. Along with assessing when their organization may be subject to liability in other states, businesses should review their insurance coverage and applications to ensure that their insurance and other risk management arrangements take into account the added risks and liabilities that could arise from the additional state law jurisdiction. Consequently, businesses choosing to operate, to register to do business in a consent-to-jurisdiction state, or contractually to agree to submit to jurisdiction in any states should be prepared for the possibility that their organization could subject themselves to regulations, lawsuits, investigations and enforcement actions in that state.
More Information
We hope this update is helpful. For more information about these or other health or other legal, management, or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
Solutions Law Press, Inc. invites you to receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 35+ years of health industry and other management work, public policy leadership and advocacy, coaching, teachings, and publications. As a significant part of her work, Ms. Stamer has worked extensively domestically and internationally with business, government, and community leaders to prepare for and deal with pregnancy, disability, and other discrimination, leave, health and safety, and other workforce, employee benefit, health care and other operations planning, preparedness and response for more than 35 years. As a part of this work, she regularly advises businesses and government leaders on an on-demand and ongoing basis about the preparation of workforce, health care, and other business and government policies and practices to deal with management in a wide range of contexts ranging from day-to-day operations, through times of crisis or change, and in response to complaints, investigations and enforcement.
Author of a multitude of other highly regarded publications and presentations on MHPAEA and other health and other benefits, workforce, compliance, workers’ compensation and occupational disease, business disaster and distress, and many other topics, Ms. Stamer has worked with health plans, employers, insurers, government leaders and others on these and other health benefit, workforce and performance and other operational and tactical concerns throughout her adult life.
A former lead advisor to the Government of Bolivia on its pension privatization project, Ms. Stamer also has worked domestically and internationally as an advisor to business, community, and government leaders on health, severance, disability, pension, and other workforce, health care and other reform, as well as regularly advises and defends organizations about the design, administration, and defense of their organization’s workforce, employee benefit and compensation, safety, discipline, and other management practices and actions.
Board Certified in Labor and Employment Law By the Texas Board of Legal Specialization, Scribe for the ABA JCEB Annual Agency Meeting with OCR, Chair-Elect of the ABA TIPS Medicine and Law Committee, Chair of the ABA International Section Life Sciences Committee, and Past Group Chair and current Welfare Plan Committee Chair of the ABA RPTE Employee Benefits & Other Compensation Group, former Vice President and Executive Director of the North Texas Health Care Compliance Professionals Association, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her extensive publications and thought leadership as well as leadership involvement in a broad range of other professional and civic organizations. For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training, and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls, and operational concerns. If you find this of interest, you also be interested in reviewing some of our other Solutions Law Press, Inc.™ resources available here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2023 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Businesses Risk Out-Of-State Lawsuits, Regulation From Registering In Consent To Jurisdiction States and Contractual Consents To Jurisdiction |
Comments Off on Businesses Risk Out-Of-State Lawsuits, Regulation From Registering In Consent To Jurisdiction States and Contractual Consents To Jurisdiction |  Age Discrimination, Antitrust, board of directors, Brokers, child labor, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, Disability, Disability Discrimination, Disability Plans, Discrimination, Drug Testing, Emploeyrs, employee, Employee Handbook, Employer, Employment, Employment Discrimination, Employment Termination, enforcement, Fair Labor Standards Act, Family Leave, FLSA, FMLA, Fringe Benefits, health benefit, health insurance, Health Plans, Human Resources, Identity Theft, insurers, Internal Controls, Internal Investigations, Joint Employer, LBGT, Leave, Management, noncompete, occupational safety, OSHA, Wage & Hour, Whistleblower | Tagged: Abortion, civil rights, Contraception, Employee Benefits, Employer, Health Plans, Insurance, LBGT, Reproductive Rights, Speach, Workforce |
Age Discrimination, Antitrust, board of directors, Brokers, child labor, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, Disability, Disability Discrimination, Disability Plans, Discrimination, Drug Testing, Emploeyrs, employee, Employee Handbook, Employer, Employment, Employment Discrimination, Employment Termination, enforcement, Fair Labor Standards Act, Family Leave, FLSA, FMLA, Fringe Benefits, health benefit, health insurance, Health Plans, Human Resources, Identity Theft, insurers, Internal Controls, Internal Investigations, Joint Employer, LBGT, Leave, Management, noncompete, occupational safety, OSHA, Wage & Hour, Whistleblower | Tagged: Abortion, civil rights, Contraception, Employee Benefits, Employer, Health Plans, Insurance, LBGT, Reproductive Rights, Speach, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 16, 2022
New Jersey McDonald’s franchisee JDKD Enterprises, L.P will pay $100,000 to settle a disability discrimination lawsuit arising from its termination of an autistic employee filed by the U.S. Equal Employment Opportunity Commission (“EEOC”). The lawsuit warns other employers against failing to reasonably accommodate or otherwise discriminating against individuals with autism or other disorders who can perform essential job functions with or without reasonable accommodation.
The EEOC’s lawsuit charged JDKD Enterprises fired an employee who worked at several McDonald’s restaurants for 37 years because of his autism spectrum disorder. The employee’s per-formance remained excellent throughout his decade-long employment at the Deptford, New Jersey McDonald’s, receiving numerous awards and accolades acknowledging his excellent job performance. However, two months after JDKD Enterprises, L.P., assumed ownership of this McDonald’s, it abruptly terminated the grill cook.
The EEOC argued the termination of the employee due to his autism disorder violates the Americans with Disabilities Act (ADA), which requires employers to provide reasonable accommodations to employees with disabilities and prohibits employers from taking adverse employment actions based on an individual’s disability or need for accommodations. After first attempting to reach a pre-litigation settlement through its voluntary conciliation process, the EEOC filed suit (Civil Action No. 1:21-cv-16441) in U.S. District Court for the District of New Jersey,
In addition to paying the former employee $100,000 in monetary relief, the two-year consent decree settling the suit provides for systemic relief intended to prevent further disability discrimination, periodic reporting to the EEOC, and training for all management personnel in responding to reasonable accommodation requests.
“The ADA protects people with autism spectrum disorder, and the EEOC is absolutely committed to aggressively enforcing the ADA requirement that employers reasonably accommodate their workers with disabilities absent undue hardship,” said Debra Lawrence, regional attorney for the EEOC’s Philadelphia District Office in the EEOC announcement of the settlement.
In the EEOC announcement of the settlement, quotes EEOC Philadelphia District Director Jamie Williamson as saying, “Ensuring that all employees, especially management, are properly trained regarding their obligations under the ADA – including their duty to engage in good faith, diligent communications with their disabled employees about accommodation needs – is a smart business practice and the right thing to do. Leadership means stewardship of an organization’s most valuable asset – its people.”
The EEOC suit and statements warn other organizations dealing with employees with autistic spectrum or other disabilities not to discriminate and to be prepared to defend the adequacy of their actions regardless of whether choosing to allow or deny accommodation.
For Help With Comments, Investigations Or Other Needs
If your organization would like to learn more about the concerns discussed in this update or seeks assistance auditing, updating, administering or defending its human resources, compensation, benefits, corporate ethics and compliance practices, or other performance related concerns, contact management attorney and consultant Cynthia Marcotte Stamer.
An attorney Board Certified in Labor & Employment Law by Texas Board of Legal Specialization, Ms. Stamer is recognized for work helping organizations management people, operations and risk as a Fellow in the American College of Employee Benefit Counsel, a “Top Woman Lawyer,” “Top Rated Lawyer,” and “LEGAL LEADER™” in Labor and Employment Law and Health Care Law; a “Best Lawyers” in “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law.”
For 35 years, Ms. Stamer’s work has focused on advising and assisting businesses and business leaders with these and other employment and other staffing, employee benefit, compensation, risk, performance and compliance management and other operational solutions and concerns. Her experience includes helping management both manage performance and manage legal risk and compliance. While helping businesses define and manage the conduct and performance of their employees, contractors and vendors, she also assists employers and others about compliance with federal and state equal employment opportunity, compensation, health and other employee benefit, workplace safety, leave, and other labor and employment laws, advises and defends businesses against labor and employment, employee benefit, compensation, fraud and other regulatory compliance and other related audits, investigations and litigation, charges, audits, claims and investigations by the IRS, Department of Labor, Department of Justice, SEC, Federal Trade Commission, HUD, HHS, DOD, Departments of Insurance, and other federal and state regulators. Ms. Stamer also speaks, coaches management and publishes extensively on these and other related matters. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
Other Helpful Resources & Information
If you found this article of interest, you also may be interested in reviewing other Breaking News, articles and other resources available including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here. For important information concerning this communication click here. If you do not wish to receive these updates in the future, unsubscribe by updating your profile here.
NOTICE: Terms. These materials are for general informational and educational purposes only. They do not establish an attorney-client relationship, are not legal advice, a substitute for legal advice, an offer or commitment to provide legal advice or an admission. The information and statements in these materials may not address all relevant issues or apply to any situation or circumstances. The author reserves the right to qualify or retract any of these statements at any time. and does not necessarily address all relevant issues. Because the law evolves and in ways that subsequent developments could impact the currency and completeness of this discussion. The author disclaims and has no responsibility to provide any update or otherwise notify anyone any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers are urged to engage competent legal counsel for consultation and representation considering the specific facts and circumstances presented in their unique circumstance at any time. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication. Readers acknowledge and agree to the conditions of this Notice as a condition of their access of this publication. Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein. ©2022 Cynthia Marcotte Stamer. Nonexclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on NJ McDonald’s Franchisee Pays $100K For Firing Autistic Employee |
Comments Off on NJ McDonald’s Franchisee Pays $100K For Firing Autistic Employee |  Accommodation, Corporate Compliance, Disability, Disability Plans, Discrimination, EEOC, Employer, Employers, Employment Discrimination, Retaliation |
Accommodation, Corporate Compliance, Disability, Disability Plans, Discrimination, EEOC, Employer, Employers, Employment Discrimination, Retaliation |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
February 17, 2022
Employers should put managing legal and operational demands for mental health accommodation for youth and other workers and their risk management agenda this year.
The Surgeon General’s recent release of an advisory report, “Protecting Young People’s Mental Health,” is one of a series of studies and guidance that the federal government has released in recent months on the impacts of the pandemic on mental health issues. The recently released Surgeon General report discusses impacts of the pandemic on mental health needs of young people. In connection with these findings, the United States Department of Labor is inviting employers and other interested persons to respond to a brief questionnaire from the National Youth Employment Coalition to help understand how workforce providers are grappling with this crisis. The DOL says this input will provide insight into the youth employment field’s current capacity to screen, connect, and serve youth with mental health needs. however, employers contemplating responding should note that the survey template requests that they respond it be identified by providing their name and other information. It is not clear whether the provision of this information may be used to target the employer for subsequent scrutiny.
The deadline for responding to the survey is March 11, 2022. To learn more, see here.
More Information
Want to know more? The author of this update, employment lawyer Cynthia Marcotte Stamer, conducted a briefing on these and other federal COVID-19 vaccination and other workforce requirements as a panelist on the “COVID-19 Vaccination Mandates & Incentives” virtual seminar the American Bar Association Joint Committee on Employee Benefits hosted on November 12, 2021. To purchase a recording of the program, see here. For information about obtaining Ms. Stamer’s slides, email here.
Solutions Law Press, Inc. also invites you to receive future updates by registering here and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy. If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here. For specific information about the these or other legal, management or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
About the Author
For help developing, administering or defending your organization’s workforce, employee benefits, compensation or compliance practices, contact the author. Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2022 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on DOL Invites Employer Input On Youth Employee Mental Health Needs |
Comments Off on DOL Invites Employer Input On Youth Employee Mental Health Needs |  ADA, Corporate Compliance, COVID-19, Disability, Disability Discrimination, Disability Plans, Discrimination, Drug & Alcohol, EEOC, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Employment Policies, group health plan, health benefit, Health Benefits, health Care, Health Plans, Mental Health, Mental Health Parity | Tagged: Discrimination, Mental Health, youth employment |
ADA, Corporate Compliance, COVID-19, Disability, Disability Discrimination, Disability Plans, Discrimination, Drug & Alcohol, EEOC, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Employment Policies, group health plan, health benefit, Health Benefits, health Care, Health Plans, Mental Health, Mental Health Parity | Tagged: Discrimination, Mental Health, youth employment |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
June 26, 2020
Earlier this week, the Internal Revenue Service (“IRS”) announced that employee benefit plan participants that already took a required minimum distribution (RMD) in 2020 from certain retirement accounts now has the opportunity through August 31, 2020 to roll those funds back into a retirement account following the Coronavirus Aid, Relief, and Economic Security (CARES) Act RMD waiver for 2020. The announcement of this relief covers one of a long and growing list of special tax and other COVID-19 responsive special rules and requirements that may change requirements, provide special relief or both for businesses and individuals that every business leader and individual should carefully monitor and respond to appropriately.
Retirement Plan Rollover Relief
On July 23, 2020, the IRS announced its extension of the 60-day rollover period for any RMDs already taken this year to August 31, 2020 to give taxpayers time to take advantage of this opportunity in Notice 2020-51 (PDF). The Notice also answers questions regarding the waiver of RMDs for 2020 under the Coronavirus Aid, Relief, and Economic Security Act, known as the CARES Act.
The CARES Act enabled any taxpayer with an RMD due in 2020 from a defined-contribution retirement plan, including a 401(k) or 403(b) plan, or an IRA, to skip those RMDs this year. This includes anyone who turned age 70 1/2 in 2019 and would have had to take the first RMD by April 1, 2020. This waiver does not apply to defined-benefit plans.
In addition to the rollover opportunity, an IRA owner or beneficiary who has already received a distribution from an IRA of an amount that would have been an RMD in 2020 can repay the distribution to the IRA by August 31, 2020. The notice provides that this repayment is not subject to the one rollover per 12-month period limitation and the restriction on rollovers for inherited IRAs.
The notice provides two sample amendments that employers may adopt to give plan participants and beneficiaries whose RMDs are waived a choice as to whether or not to receive the waived RMD.
Other COVID-19 Tax Rules & Relief
The guidance and relief in Notice 2020-51 highlights only one of a long list of special COVID-19 associated tax rules and relief that could apply to a business, its employees or employee benefit plan participants or both including the following:
- IR-2020-127, IRS announces rollover relief for required minimum distributions from retirement accounts that were waived under the CARES Act
- IR-2020-126, IRS extends July 15, other upcoming deadlines for tornado victims in parts of the South; provides other relief
- IR-2020-124, Relief for taxpayers affected by COVID-19 who take distributions or loans from retirement plans
- IR-2020-122, IRS outlines changes to health care spending available under CARES Act
- IR-2020-121, IRS alert: Economic Impact Payments belong to recipient, not nursing homes or care facilities
- IR-2020-120, Treasury, IRS provide tax relief to investors and businesses affected by COVID-19 in new markets tax credit transactions
- IR-2020-119, IRS provides guidance on employer leave-based donation programs that aid victims of the COVID-19 pandemic
- IR-2020-118, IRS reminder: File now, choose direct deposit or schedule tax payments electronically before the July 15 deadline
- IR-2020-117, IRS reminder: Deadline postponed to July 15 for those who pay estimated taxes
- IR-2020-115, IRS warns against COVID-19 fraud; other financial schemes
- IR-2020-114, IRS provides answers about Coronavirus related tax relief for Qualified Opportunity Funds and investors
- IR-2020-111, 159 million Economic Impact Payments processed; Low-income people and others who aren’t required to file tax returns can quickly register for payment with IRS Non-Filers tool
- IR-2020-110, IRS provides relief to retirement plan participants to sign elections remotely
- IR-2020-109, IRS reminder: June 15 tax deadline postponed to July 15 for taxpayers who live and work abroad
- IR-2020-106, Treasury, IRS provide safe harbor for taxpayers that develop renewable energy projects
- IR-2020-105, Economic Impact Payments being sent by prepaid debit cards, arrive in plain envelope; IRS.gov answers frequently asked questions
- IR-2020-101, Treasury, IRS release latest state-by-state Economic Impact Payment figures for May 22, 2020
- IR-2020-99, IRS.gov helps taxpayers get tax information they need; find tools for filing, paying, checking accounts and answering questions
- Treasury News Release: Treasury is Delivering Millions of Economic Impact Payments by Prepaid Debit Card
- IR-2020-97, IRS adds phone operators to answer Economic Impact Payment questions
- IR-2020-96, IRS expands partner materials for Economic Impact Payments; continues sweeping effort to share details in multiple languages
- IR-2020-95, IRS provides tax relief through increased flexibility for taxpayers in section 125 cafeteria plans
- IR-2020-93, Why the Economic Impact Payment amount could be different than anticipated
- IR-2020-92, Act by Wednesday for chance to get quicker Economic Impact Payment; timeline for payments continues to accelerate
- IR-2020-91, Treasury, IRS release latest state-by-state Economic Impact Payment figures
- IR-2020-89, IRS: Three new credits are available to many businesses hit by COVID-19
- IR-2020-87, IRS retools Settlement Days program in response to COVID-19 pandemic; allows unrepresented taxpayers to settle their cases virtually and reach finality
- IR-2020-86, VA, SSI recipients with eligible children need to act by Tuesday, May 5 to quickly add money to their automatic Economic Impact Payment; ‘Plus $500 Push’ continues
- IR-2020-85, Economic Impact Payments continue to be sent, check IRS.gov for answers to common questions
- IR-2020-83, Use IRS Non-Filers: Enter Payment Info Here tool to get Economic Impact Payment; many low-income, homeless qualify
- IR-2020-82, IRS enhances Get My Payment online application to help taxpayers
- IR-2020-81, VA, SSI recipients with eligible children need to act by May 5 to quickly add money to their automatic Economic Impact Payment; ‘Plus $500 Push’ continues
- IR-2020-80, Treasury, IRS deliver 89.5 million Economic Impact Payments in first three weeks, release state-by-state Economic Impact Payment figures (Updated: April 28, 2020)
- IR-2020-77, Treasury, IRS announce cross-border tax guidance related to travel disruptions arising from the COVID-19 emergency
- IR-2020-76, SSA, RRB recipients with eligible children need to act by Wednesday to quickly add money to their automatic Economic Impact Payment; IRS asks for help in the “Plus $500 Push”
- IR-2020-75, Veterans Affairs recipients will receive automatic Economic Impact Payments; Step follows work between Treasury, IRS, VA
- IR-2020-74, IRS: Free File use soars; taxpayers still have time to do their taxes for free
- IR-2020-73, Supplemental Security Income recipients will receive automatic Economic Impact Payments; step follows work between Treasury, IRS, Social Security Administration
- IR-2020-72, Treasury, IRS unveil online application to help with Economic Impact Payments
- IR-2020-71, IRS, Security Summit partners warn tax professionals on scams, urge additional security measures to protect taxpayer data
- IR-2020-70, REMINDER: Schedule and pay federal taxes electronically due by July 15; only a few hours remaining for taxpayers to reschedule payments set for April 15
- IR-2020-69, Treasury, IRS launch new tool to help non-filers register for Economic Impact Payments
- IR-2020-68, IRS urges taxpayers to use electronic options; outlines online assistance
- IR-2020-67, IRS provides guidance under the CARES Act to taxpayers with net operating losses
- IR-2020-66, To help taxpayers, the Department of Treasury and the Internal Revenue Service announced today that Notice 2020-23 extends additional key tax deadlines for individuals and businesses
- IR-2020-65, Follow IRS on social media, sign up for e-news subscriptions for urgent updates on COVID-19, scams and economic impact payment information
- IR-2020-64, IRS issues warning about coronavirus-related scams; watch out for schemes tied to economic impact payments
- Treasury News Release: Social Security recipients will automatically receive Economic Impact Payments
- IR 2020-62, IRS: Employee Retention Credit available for many businesses financially impacted by COVID-19
- IR 2020-61, Economic impact payments: What you need to know
- IR-2020-59, IRS unveils new People First Initiative; COVID-19 effort temporarily adjusts, suspends key compliance program
- IR-2020-58, Tax Day now July 15: Treasury, IRS extend filing deadline and federal tax payments regardless of amount
- IR-2020-57, Treasury, IRS and Labor announce plan to implement coronavirus-related paid leave for workers and tax credits for small and midsize businesses to swiftly recover the cost of providing Coronavirus-related leave
- Treasury News Release: Treasury and IRS issue guidance on deferring tax payments due to COVID-19 outbreak
- IR-2020-54, IRS: High-deductible health plans can cover coronavirus costs
Along with these tax rules, businesses and their employees also may be impacted by a broad range of special federal and state labor and employment and other rules adopted in response to the continuing COVID-19 health care emergency and its fallout. Businesses and their leaders should carefully review and monitor these and other COVID-19 specific rules to ensure that their businesses don’t trigger unanticipated liability by failing to meet critical requirements or to ensure that they take full advantage of all available relief.
More Information
We hope this update is helpful. For more information about the these or other health or other legal, management or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
Solutions Law Press, Inc. invites you receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years legal and operational management work, coaching, public policy and regulatory affairs leadership and advocacy, training and public speaking and publications. As a significant part of her work, Ms. Stamer has worked extensively domestically and internationally on an demand, special project and ongoing basis with health industry, health plan and insurance and other businesses of all types, government and community organizations and their leaders, spoken and published extensively on workforce and other services, compensation and benefits, and related tax; insurance; workers’ compensation and occupational disease; business reengineering, disaster and distress; and many other management concerns.
Board Certified in Labor and Employment Law By the Texas Board of Legal Specialization, Scribe for the ABA JCEB Annual Agency Meeting with OCR, Vice Chair of the ABA International Section Life Sciences Committee, and the ABA RPTE Employee Benefits & Other Compensation Group and a former Council Representative, Past Chair of the ABA Managed Care & Insurance Interest Group, former Vice President and Executive Director of the North Texas Health Care Compliance Professionals Association, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer has extensive experience advising, representing, defending and training health care providers, health plans and insurers, employers, community organizations and others about HIPAA and other privacy concerns and has published and spoken extensively on these concerns.
Her involvement with HIPAA and other privacy and data concerns has taken place as part of her more than 30 years involvement working with with public and private health industry, health insurance and other employers and organizations of all sizes, employee benefit plans, insurance and financial services, health industry and a broad range of public and private domestic and international business, community and government organizations and leaders on pandemic and other health and safety, workforce and performance preparedness, risks and change management, disaster preparedness and response and other operational and tactical concerns throughout her adult life. A former lead advisor to the Government of Bolivia on its pension project, Ms. Stamer also has worked internationally and domestically as an advisor to business, community and government leaders on crisis preparedness and response, privacy and data security, workforce, health care and other policy and enforcement, as well as regularly advises and defends organizations about the design, administration and defense of their organizations workforce, employee benefit and compensation, safety, discipline and other management practices and actions.
Ms. Stamer also serves in leadership of a broad range of professional and civic organizations and shares insights and thought leadership through her extensive publications and public speaking. For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources available here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here. ©2020 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.
 Comments Off on Businesses Should Confirm Using Benefits, Meeting Mandates Of Special COVID-19 Tax Rules |
Comments Off on Businesses Should Confirm Using Benefits, Meeting Mandates Of Special COVID-19 Tax Rules |  401(k), Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act, retirement plan, Retirement Plans, Retirements, Unemployment Benefits, Unemployment Insurance |
401(k), Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act, retirement plan, Retirement Plans, Retirements, Unemployment Benefits, Unemployment Insurance |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
June 16, 2020
While most COVID-19 test results won’t draw the widespread coverage and public interest that Elliott’s diagnosis did, businesses generally and health care providers, health plans, health care clearinghouses specifically need to recognize that coverage of the Elliott outrage will heighten awareness and therefore their need to properly handle and protect COVID-19 or other infectious disease and other testing, diagnosis, treatment and other medical and disability information collected or encountered in the course of their operation through the current COVID-19 health care emergency and otherwise in their own organizations.
ADA Responsibilities of Employers In Handling Medical Information
Protecting COVID-19 testing and other medical information isn’t just a concern for covered entities and their business associates, however. Businesses that are not covered entities also generally should use care in their collection, use, protection and disclosure of COVID-19 testing and other medical information to mitigate their potential liability under the disability discrimination requirements of the ADA, the Rehabilitation Act and other laws. For instance, along with prohibiting employers covered by the ADA from discriminating against qualified individuals with disabilities and requiring those employers to provide reasonable accommodations to such employees, the ADA also regulates the ability of covered employers to perform or require medical testing and imposes specific medical confidentiality requirements on all covered employers. See e.g., What You Should Know About COVID-19 and the ADA, the Rehabilitation Act, and Other EEO Laws.
The ADA’s medical confidentiality requirements dictate that covered employers maintain medical information and records about employees and applicants in separate, confidential files. Covered employers are responsible for maintaining the confidentiality of medical information and records and cannot disclose it without authorization from the subject employee except under the specific conditions allowed by the ADA.
EEOC guidance provided in its publication entitled Pandemic Preparedness in the Workplace and the Americans With Disabilities Act as updated as of March 19, 2020 emphasizes that covered employers remain accountable for complying with the requirements of the ADA and Rehabilitation Act during the current COVID-19 health care emergency and other pandemics.
While the EEOC Technical Assistance Questions and Answers in its publication What You Should Know About COVID-19 and the ADA, the Rehabilitation Act, and Other EEO Laws
Technical Assistance Questions and Answers as updated on June 11, 2020 recognizes temperature checks and certain other COVID-19 inquiries to screen for COVID-19 exposure or infection might be permitted under the safety exception to the ADA during the current COVID-19 health care emergency, that and other EEOC guidance makes clear that covered employers remain responsible for ensuring that the ADA medical confidentiality requirements are met with regarding to testing and related medical information. As a result, all ADA-covered employers generally and health care employers specifically are urged to use care both in the administration and collection of information regarding COVID-19 testing and diagnosis, and the protection of the confidentiality of COVID-19 and other medical information and records collected in the course of administering employment, safety, medical leave or other absence or other operations throughout the COVID-19 health care emergency.
Added HIPAA & Texas HIPAA Concerns For Health Plans & Other HIPAA Covered Entities
Assuming that the disclosure of Elliott’s information is traced to a testing provider, laboratory or other health care provider, health plan or insurer, health care clearing house subject to HIPAA (“covered entity”), a service provider acting as a business associate to a covered entity, or a member of their workforce, the unauthorized release of Elliott’s test results, that he underwent the testing, or other medical information, Elliott’s complaint about a possible HIPAA violation could be well-founded as both HIPAA and the somewhat broader provisions of the Texas Medical Privacy Act (“Tex-HIPAA”) (hereafter collectively the “HIPAA Laws”) both generally prohibit unauthorized disclosure of protected medical information such as his COVID-19 test or test results to the media.
The COVID-19 test results and of “individually identifiable personal health information” about Elliott and his encounter created, used, access or disclosed by the testing facility or other health care provider, a health plan, health care clearinghouse (“covered entity”) or a member of its workforce or a subcontractor acting as a business associated qualify as “protected health information subject to HIPAA’s privacy, security, breach and privacy rights protections of HIPAA and Tex-HIPAA.
The HIPAA and Tex-HIPAA prohibition against unauthorized disclosure of protected health information to the media stem from the HIPAA Laws’ broader requirement that covered entities and business associates affirmatively safeguard protected health information against unauthorized use, access or disclosure and sweeping prohibition against their disclosing or allowing the disclosure of protected health information without a HIPAA-compliant authorization except under the narrow and specifically delineated exceptions identified in the rule, none of which appear relevant to the media disclosure objected to by Elliott from the currently available public information.
Both HIPAA Laws expressly prohibit unauthorized disclosure of protected health information by covered entities or their business associates except under the specifically detailed conditions specified in one or more exceptions to this general rule. Assuming all relevant conditions to qualify for the exception are met, HIPAA does allow covered entities and business associates treatment, payment, operations, public health activities or another situation meeting all applicable requirements of an express exception to the HIPAA prohibition against disclosure.
The federal agency primarily responsible for the implementation and enforcement of HIPAA, the Department of Health & Human Services Office of Civil Rights (“OCR”) regulatory guidance and enforcement history clearly communicates OCR’s view that covered entities or business associates violate HIPAA by disclosing protected health information to the media or other third parties without first obtaining a HIPAA-compliant authorization from the subject of the information except under the specific circumstances described in an applicable Privacy Rule exception.
In its May 5, 2020 Guidance on Covered Health Care Providers and Restrictions on Media Access to Protected Health Information about Individuals in Their Facilities (“5/5 Guidance”), for instance, OCR specifically reminded HIPAA covered health care providers that the HIPAA Privacy Rule does not permit them to give media and film crews access to protected health information including access to facilities where patients’ protected health information will be accessible without the patients’ prior authorization. has made clear that testing facilities and other health care providers generally remain accountable for complying with the HIPAA Privacy Rule that prohibits unauthorized use, access or disclosure of test results and other protected health information except as specifically allowed in the applicable HIPAA Law.
The 5/5 Guidance specifically states, “The COVID-19 public health emergency does not alter the HIPAA Privacy Rule’s existing restrictions on disclosures of protected health information (PHI) to the media.’ Additionally, it states confirmed that even during the current COVID-19 public health emergency, covered health care providers remain required to obtain a valid HIPAA authorization from each patient whose PHI will be accessible to the media before the media is given access to that PHI. In this regard, the 5/5 Guidance states, As explained in prior guidance,1 HIPAA does not permit covered health care providers to give the media, including film crews, access to any areas of their facilities where patients’ PHI will be accessible in any form (e.g., written, electronic, oral, or other visual or audio form), without first obtaining a written HIPAA authorization from each patient whose PHI would be accessible to the media. 2 Additionally, covered health care providers may not require a patient to sign a HIPAA authorization as a condition of receiving treatment. The guidance clarifies that masking or obscuring patients’ faces or identifying information before broadcasting a recording of a patient is not sufficient, as a valid HIPAA authorization is still required before giving the media such access. Additionally, the guidance describes reasonable safeguards that should be used to protect the privacy of patients whenever the media is granted access to facilities.
OCR’s positions on disclosures to the media in the 5/5 Guidance reaffirm OCR’s longstanding interpretation and enforcement of HIPAA as prohibiting disclosures of PHI and media access to areas where patients or their protected health information might be visible or accessible is long standing.
In June, 2013, for instance, OCR sent a clear message to covered entities and business associates not to make unconsented disclosures of protected health information to or allow media access to areas where patients or their protected health information could be accessed or observed when it required Shasta Regional Medical Center (SRMC) to pay $275,000 to resolve OCR HIPAA charges stemming from SRMC’s unauthorized disclosure of protected health information to multiple media outlets as part of a public relations effort to mitigate damage from fraud and misconduct allegations made against it by the patient. See HIPAA Sanctions Triggered From Covered Entity Statements To Media, Workforce.
OCR subsequently reinforced its warning to covered entities and business associates about unauthorized disclosures of protected health information in a 2016 Frequently Asked Question (Media FAQ) that discussed covered entities HIPAA responsibilities when dealing with the media. The Media FAQ was issued in conjunction with OCR’s collection of its $2.2 million settlement with New York-Presbyterian Hospital and a series of other settlements totaling $999,000 from three other health care providers accused of violating HIPAA by allowing media personnel into treatment or other areas where patients or patient protected health information was accessible without first obtaining a HIPAA compliant written authorization from each patient or other subject present or whose protected health information otherwise would be accessible to the media. See $999K Price Hospitals Pay To Settle HIPAA Privacy Charges From Allowing ABC To Film Patients Without Authorization.
In the Media FAQ, OCR stated HIPAA required covered entities to obtain prior written authorization before disclosing protected health information to the media or allowing media to film or access exam rooms or other areas where patients or protected health information could be observed or accessed. The Media FAQ also stated that masking or blurring the identity of the patient or their specific information was not an adequate substitute for written authorization and that covered entities also were responsible for ensuring that reasonable safeguards were in place to protect against impermissible disclosures or to limit incidental disclosures of other PHI in areas where media is allowed access where prior authorization has not been obtained. While stressing the importance of compliance with these requirements, however, the Media FAQ clarified that the HIPAA Privacy Rule does not require health care providers to prevent members of the media from entering areas of their facilities that are otherwise generally accessible to the public like public waiting areas or areas where the public enters or exits the facility In addition, the Media FAQ states a health care provider or other Covered Entity also highlighted certain other limited circumstances where HIPAA might allow limited disclosure of protected health information to the media in accordance with specific provisions of the Privacy Rule about an incapacitated patient when in the patient’s best interest; or disclose a patient’s location in the facility and condition in general terms that do not communicate specific medical information about the individual to the media or any other person any person where the individual has not objected to his information being included in the facility directory and the media representative or other person asks for the individual by name.
In the intervening years, OCR periodically has issued additional reminders to covered entities about HIPAA’s general prohibition against unconsented disclosures to the media as well as sanctioned harshly various covered entities for violating these prohibitions. In 2017, OCR required the largest not-for-profit health system in Southeast Texas, Memorial Hermann Health System (MHHS), to pay OCR $2.4 million to settle charges it violated HIPAA by issuing a press release to the media that shared the name and other protected health information about a patient suspected of using a fraudulent insurance card to obtain care at a clinic without the patient’s prior HIPAA-compliant authorization. While OCR concluded a report made MHHS made to law enforcement about the patient was allowable under the Privacy Rule, OCR found MHHS violated the Privacy Rule by issuing the press release disclosing the patient’s name and other PHI without authorization from the patient and also by failing to timely document the sanctioning of its workforce members for impermissibly disclosing the patient’s information. See $2.4M HIPAA Settlement Warns Providers About Media Disclosures Of PHI.
While OCR has announced certain temporary enforcement relief from a narrow set of HIPAA requirements during the COVID-19 health care emergency as applied to certain qualifying testing facilities, telemedicine providers and other specific health care providers engaging in certain types of health care during the COVID-19 health care emergency, OCR consistently has made clear that its COVID-19 HIPAA relief is very limited in scope, applicability and duration and in no way waives the prohibition against unauthorized disclosure to the media or other third parties not generally permitted under HIPAA. See e.g., 5/5 Guidance; OCR Issues Guidance on How Health Care Providers Can Contact Former COVID-19 Patients About Blood and Plasma Donation Opportunities; OCR Announces Notification of Enforcement Discretion for Community-Based Testing Sites During the COVID-19 Nationwide Public Health Emergency; OCR Announces Notification of Enforcement Discretion to Allow Uses and Disclosures of Protected Health Information by Business Associates for Public Health and Health Oversight Activities During The COVID-19 Nationwide Public Health Emergency; OCR Issues Bulletin on Civil Rights Laws and HIPAA Flexibilities That Apply During the COVID-19 Emergency; OCR Issues Guidance to Help Ensure First Responders and Others Receive Protected Health Information about Individuals Exposed to COVID-19; OCR Issues Guidance on Telehealth Remote Communications Following Its Notification of Enforcement Discretion; OCR Announces Notification of Enforcement Discretion for Telehealth Remote Communications During the COVID-19 Nationwide Public Health Emergency. To the contrary, OCR’s announcement of the 5/5 guidance quotes OCR Director Roger Severino, as stating “Hospitals and health care providers must get authorization from patients before giving the media access to their medical information; obscuring faces after the fact just doesn’t cut it,” Severino added.
Minimize Exposures By Preventing Unauthorized Media & Other Disclosures
Even without Mr. Elliott’s outrage heightening awareness about HIPAA’s prohibitions against unauthorized disclosures of protected health information to the media, the recent warning about HIPAA’s restrictions on media disclosure and access to protected health information and patient treatment areas in OCR’s 5/5 Guidance alone should serve as a strong incentive for covered entities and business associate promptly to reverify that the adequacy of their current policies, practices and training to prevent inappropriate media disclosures of protected health information and otherwise defend their compliance with OCR’s interpretation of HIPAA’s requirements for dealing with the media. Predictable heightened patient and public awareness and expectations about these and other HIPAA responsibilities fueled by the widespread media coverage of Mr. Elliott’s COVID-19 test results and his outrage about the unauthorized disclosure of his test results makes it more important than ever that health care providers and other covered entities and business associates take steps to prepare to respond to foreseeable complaints and questions by other patients, their families and others.
As part of these efforts, most covered entities and business associates may want to consider, at minimum, reconfirming the adequacy and understanding of their current media and other disclosure policies and practices, as well as sending strategic communications to their business associates and members of their workforce reminding them of the covered entity’s policies regarding media access and disclosures.
As part of these activities, covered entities should consider conducting a well-documented assessment of their current policies, practices and workforce training on disclosure of information to the media and other parties generally, as well as policies on allowing media or other parties to enter, film, photograph or record within their facilities or otherwise disclosing or allowing media access to their facilities. Along with these efforts, most covered entities also may want to consider also reminding workforce members that their patient privacy responsibilities also requires that they not share or discuss patient protected health information, film, photograph, or otherwise record, patients or areas where patients or patient protected health information is or might be present without prior written consent of the patient and the consent of their organization.
Since covered entities and members of their workforce also are likely to be subject to other statutory, ethical, contractual or other privacy or confidentiality requirements beyond those imposed by the HIPAA Laws such as medical confidentiality duties applicable to physicians and other health care providers under medical ethics, professional licensure or other similar rules, contractual responsibilities, as well as common law or statutory privacy, theft of likeness or other statutory or common law tort claims and exposures. Covered entities and business associates generally should consider whether other steps are advisable to manage these exposures along with managing their HIPAA Law compliance.
Given the high incidence of COVID-19 exposure and infection within their workplace, covered entities, business associates and other employers should use care fulfill their HIPAA Law relevant employment law confidentiality responsibilities when dealing with testing or other medical information about employees. In this respect, along with any HIPAA Law obligations that a covered entity or business associate has in handling medical information about a patient who also is an employee or family member of an employee, covered entities also should use care to ensure that medical confidentiality requirements of the Americans With Disabilities Act (“ADA”) and other applicable employment laws are met.
Since this analysis and review in most cases will result in the uncovering or discussion of potentially legally or politically sensitive information, Covered Entities should consider consulting with or engaging experienced legal counsel for assistance in structuring and executing these activities to maximize their ability to claim attorney-client privilege or other evidentiary protections against discovery or disclosure of certain aspects of these activities.
Finally, covered entities should keep in mind that HIPAA and other medical privacy compliance and risk management is an ongoing process requiring constant awareness and diligence. Consequently, covered entities and business associates also should use care both to monitor OCR and other regulatory and enforcement developments as well as exercise ongoing vigilance to monitor and maintain compliance within their organizations.
More Information
We hope this update is helpful. For more information about the these or other health or other legal, management or public policy developments, please contact the author Cynthia Marcotte Stamer via e-mail or via telephone at (214) 452 -8297.
Solutions Law Press, Inc. invites you receive future updates by registering on our Solutions Law Press, Inc. Website and participating and contributing to the discussions in our Solutions Law Press, Inc. LinkedIn SLP Health Care Risk Management & Operations Group, HR & Benefits Update Compliance Group, and/or Coalition for Responsible Health Care Policy.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years legal and operational management work, coaching, public policy and regulatory affairs leadership and advocacy, training and public speaking and publications. As a significant part of her work, Ms. Stamer has worked extensively domestically and internationally on an demand, special project and ongoing basis with health industry, health plan and insurance and other business, government and community organizations and their leaders, spoken and published extensively on HIPAA and other privacy and data security concerns, as well as other health care and health benefits; human resources, employee benefits and other workforce and services; insurance; workers’ compensation and occupational disease; business reengineering, disaster and distress; and many other management concerns.
Board Certified in Labor and Employment Law By the Texas Board of Legal Specialization, Scribe for the ABA JCEB Annual Agency Meeting with OCR, Vice Chair of the ABA International Section Life Sciences Committee, and the ABA RPTE Employee Benefits & Other Compensation Group and a former Council Representative, Past Chair of the ABA Managed Care & Insurance Interest Group, former Vice President and Executive Director of the North Texas Health Care Compliance Professionals Association, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer has extensive experience advising, representing, defending and training health care providers, health plans and insurers, employers, community organizations and others about HIPAA and other privacy concerns and has published and spoken extensively on these concerns.
Her involvement with HIPAA and other privacy and data concerns has taken place as part of her more than 30 years involvement working with with public and private health industry, health insurance and other employers and organizations of all sizes, employee benefit plans, insurance and financial services, health industry and a broad range of public and private domestic and international business, community and government organizations and leaders on pandemic and other health and safety, workforce and performance preparedness, risks and change management, disaster preparedness and response and other operational and tactical concerns throughout her adult life. A former lead advisor to the Government of Bolivia on its pension project, Ms. Stamer also has worked internationally and domestically as an advisor to business, community and government leaders on crisis preparedness and response, privacy and data security, workforce, health care and other policy and enforcement, as well as regularly advises and defends organizations about the design, administration and defense of their organizations workforce, employee benefit and compensation, safety, discipline and other management practices and actions.
Ms. Stamer also serves in leadership of a broad range of professional and civic organizations and shares insights and thought leadership through her extensive publications and public speaking. For more information about Ms. Stamer or her health industry and other experience and involvements, see www.cynthiastamer.com or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources available here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here. ©2020 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.
 Comments Off on Ezekiel Elliott COVID-19 Diagnosis Disclosure Outrage Highlights Need To Handle COVID-19 & Other Medical Information With Care |
Comments Off on Ezekiel Elliott COVID-19 Diagnosis Disclosure Outrage Highlights Need To Handle COVID-19 & Other Medical Information With Care |  Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act |
Accommodation, ADA, adea, Association Health Plan, board of directors, Brokers, Child Safety, Civil Rights, Claims, Corporate Compliance, COVID, Data Breach, Disability, Disability Discrimination, Disability Leave, Disability Plans, Disaster, Discrimination, Disease Management, EBSA, Electronic Medical Record, Emergency, employee, Employee Benefits, Employer, Employment, Employment Discrimination, family leave, Fiduciary Responsibility, FMLA, Government Contractors, government employer, government plan, health benefit, Health Benefits, health Care, health plan, Health Plans, HIPAA, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Leave, Managed Care, Management, OFCCP, OSHA, Privacy, Rehabilitation Act |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 8, 2019
U.S. employers should start giving clear feedback to Congress about proposals to impose new federal paid family leave requirements on U.S. employers likely to move quickly through Congress given strong bipartisan Congressional and Presidential support. The push for enactment of federal paid leave legislation comes amid the enactment of a patchwork of state and local state paid leave laws over the past decade.
Strong bi-partisan Congressional support for expanded federal support for paid family leave was evident from statements and testimony at the House Ways and Means Committee Full Committee Hearing on Paid Family and Medical Leave: Helping Workers and Employers Succeed this morning.
In fact, Republican Representative Tom Brady, the Ranking Minority Member of the Committee, stated in his opening statement at the start of the hearing, “Today the question isn’t whether to expand paid family leave, but how best to achieve it.”
With the majority of Congress supporting federal legislation to expand the availability of paid family leave, U.S. employers should make sure to communicate their preferences about the “how” to Congress whole time remains to influence those decisions.
While both parties and the President Trump support expanded federal support for paid leave, the two Parties differ widely about the how federal legislation should promote paid family leave.
Republicans generally are urging the extension and support the “carrot” incentive approach they began in the last Congress when they led the enactment of The Paid Family and Medical Leave Tax Credit, doubling of the Child Tax Credit to its largest amount in history, increase of the Child Tac Credit refundability, and expansion of its availability to 8 million more families as part of the Tax Cuts and Jobs Act. The new paid leave credit reimburses qualifying businesses up to 25 percent of the cost of providing paid leave to their workers. In this first-ever pilot program, businesses can get help for offering up to 12 weeks of paid leave. Republicans now support continuation and possible expansion of these incentives.
In contrast, Democrats advocate Congress using a “stick” approach by mandating that employers provide paid family leave or government sponsored programs through a plethora of proposals including, for instance instance:
- S. 840, the Healthy Families Act and H.R. 1784, the Healthy Families Act would require covered employees of 15 or more employees to provide 1 hour of paid sick leave for care of self or a family member for every 30 hours an employee works that employees could carryover to subsequent years if not used with substantial penalties imposed employers; and
- H.R. 1185: FAMILY Act introduced by Democrat Representative Rosa DeLauro with 185 co-sponsors would establish government sponsored accounts to provide paid family leave.
In his comments this morning, Representative Brady noted the need to tailor paid mandates to account for differences in employer needs, stating: “As we work to expand access to paid medical leave, there are real concerns that a new one-size-fits-all Washington mandate limits family flexibility, could be extremely costly, and will lead to higher taxes on workers, reduced job benefits, or harmful cuts in education, Social Security, or Medicare to pay for the new mandate.
in addition, before the hearing the highest ranking Republicans on the Subcommittees for Select Revenue Measures, Worker and Family Support, and Social Security respectively, Representatives Kevin Brady, Adrian Smith, Jackie Walorski, and Tom Reed, sent a letter to Ways and Means Chairman Richard Neal (D-MA), urging the emphasis of incentives over “one size, fits all mandates.”
With both parties pushing to enact their preferred paid family leave approach, employers concerned about the cost and other challenges of a federal paid family leave mandate should review and provide feedback to key Congressional committees and members as soon as possible.
If you want addition information or assistance in reviewing or responding to these proposals, please contact the author directly.
We also invite you to share your own best practices ideas and resources and join the discussions about these and other human resources, health and other employee benefit and patient empowerment concerns by participating and contributing to the discussions in our Solutions Law Press HR & Benefits Update Group or COPE: Coalition On Patient Empowerment Groupon LinkedIn or Project COPE: Coalition on Patient Empowerment Facebook Page.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here. We also invite you to join the discussion of these and other human resources, health and other employee benefit and patient empowerment concerns by participating and contributing to the discussions in our Health Plan Compliance Group or COPE: Coalition On Patient Empowerment Groupon LinkedIn or Project COPE: Coalition on Patient Empowerment Facebook Page.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on Congress Moves To Enact Federal Paid Leave Rules |
Comments Off on Congress Moves To Enact Federal Paid Leave Rules |  compliance, Corporate Compliance, Disability Plans, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Family Leave, Fringe Benefit, Fringe Benefits, Uncategorized |
compliance, Corporate Compliance, Disability Plans, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Family Leave, Fringe Benefit, Fringe Benefits, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 26, 2019
Employers, health plans and others concerned about managing the high medical, disability and other costs of Type 2 Diabetes should use today’s annual Diabetes Awareness Day observances and resources to beef up their efforts and tools.
With 1 in 3 adult Americans at risk for Type 2 diabetes, the Centers for Disease Control (“CDC”) and other public and private organizations partnering in The National Diabetes Prevention Program are urging all Americans, their health plans, state and local agencies and communities to protect themselves and join their fight to prevent or delay Type 2 diabetes.
Celebrated every year on the fourth Tuesday in March, Diabetes Alert Day promotes awareness of the prevalence and risks of undiagnosed or unmanaged Type 2 Diabetes to Americans, American taxpayers, health benefit programs and their communities.
- More than 30 million people in the United States have diabetes and an additional 84 million adults—over a third—have prediabetes, and 90% of them don’t know they have it.
- Diabetes is the 7th leading cause of death in the United States (and may be underreported).
- Type 2 diabetes accounts for about 90% to 95% of all diagnosed cases of diabetes; type 1 diabetes accounts for about 5%.
- In the last 20 years, the number of adults diagnosed with diabetes has more than tripled as the American population has aged and become more overweight or obese
- Undiagnosed or unmanaged Type 2 diabetes threatens serious and disabling medical risks for afflicted individuals that also are financially costly for patients and their families, their health plans, taxpayers and communities.
Type 2 diabetes usually starts during adulthood; however, children, teens, and young adults increasingly also are developing it. Since Type 2 diabetes symptoms often develop over several years and can go on for a long time without being noticed it’s important individuals know the factors for Type 2 Diabetes and that people with these symptoms visit their doctor promptly.
Fortunately, Type 2 Diabetes and its costs often can be prevented or minimized through appropriate diagnosis and treatment. That’s why the CDC and its partners are urging all Americans, the employers, health plans, health care providers and communities to join the fight against Type 2 Diabetes.
To start with, the CDC and its partners ask every American to learn their risk for diabetes by taking the online Type 2 Diabetes Risk and promote use of CDC-recognized lifestyle change programs to individuals suffering or at risk for Type 2 diabetes.
The CDC and its partners also are asking American families, health care providers, employers and their health benefit programs, federal, local and state governments and communities to help identify and get people at risk or suffering from Type 2 diabetes involved in making appropriate lifestyle changes and other activities to help manage their Type 2 Diabetes and offers a multitude of free tools and resources to help promote Type 2 Diabetes Awareness and assist in its prevention and treatment.
Employers and their health plans and insurers should consider participating in Diabetes Alert Day and using some of the resources provided by CDC and other partners to beef up their Type 2 and other Diabetes prevention, screening and management efforts. Appropriate use of these resources could help mitigate exposure to the high medical, disability, productivity and other costs that employers and their health plans generally incur when employees or their family members suffer from undiagnosed or unmanaged diabetes. When utilizing these resources, however, employers and their health plan fiduciaries, insurers and administrators are reminded to use care to implement and administer these wellness and other programs in a manner that complies with the Americans With Disabilities Act (“ADA”), Health Insurance Portability & Accountability Act, Internal Revenue Code and other federal and state requirements concerning the design and administration of wellness and disease management programs including recent updates in the Equal Employment Opportunity Commission’s regulations and enforcement positions under the ADA.
Learn more about Type 2 Diabetes cost modeling, screening, prevention and other participant education resources in our companion article in the Project Cope: Coalition for Patient Empowerment Newsletter. We also invite you to share your own best practices ideas and resources and join the discussions about these and other human resources, health and other employee benefit and patient empowerment concerns by participating and contributing to the discussions in our Health Plan Compliance Group or COPE: Coalition On Patient Empowerment Groupon LinkedIn or Project COPE: Coalition on Patient Empowerment Facebook Page.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, FMLA and other leave, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; audits, investigations, enforcement and defense; Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on Use 3/26 Diabetes Alert Day Resources To Jumpstart Your Diabetes Management & Cost Containment Efforts |
Comments Off on Use 3/26 Diabetes Alert Day Resources To Jumpstart Your Diabetes Management & Cost Containment Efforts |  Disability, Disability, Disability Leave, Disability Plans, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, family leave, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HR, Human Resources, Leave, Management, medical leave, Military Leave, preventive care, Wellness | Tagged: department of labor, Employee, Employee Benefits, Employer, Health Insurance, Health Plans, Human Resources, Military Leave, Wellness, Wellness Programs |
Disability, Disability, Disability Leave, Disability Plans, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Employment Policies, enforcement, family leave, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HR, Human Resources, Leave, Management, medical leave, Military Leave, preventive care, Wellness | Tagged: department of labor, Employee, Employee Benefits, Employer, Health Insurance, Health Plans, Human Resources, Military Leave, Wellness, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 19, 2019
A new U.S. Department of Labor’s Wage and Hour Division (WHD) Family and Medical Leave Act (“FMLA”) opinion letter says warns employers not to delay providing FMLA notice or designating a leave as FMLA-covered when coordinating FMLA protected leave with otherwise available paid or unpaid leave.
FMLA Opinion 2019-1-A states that a FMLA-covered employer must designate as FMLA protected and, absent extenuating circumstances, must provide notice of the designation of the leave as FMLA protected within five business days of the date the employer has enough information to determine an employee has experienced a FMLA qualifying event. The Opinion says this designation and notice must happen even if the employee would prefer that the employer delay the designation of the absence as a FMLA protected leave until the employee exhausts other available leave.
According to WHD, its FMLA regulations require employers to provide a written “designation notice” to an employee within five business days—absent extenuating circumstances—after the employer “has enough information to determine whether the leave is being taken for a FMLA-qualifying reason.” Failure to provide timely notice requirement may constitute an interference with, restraint on, or denial of the exercise of an employee’s FMLA rights. 29 C.F.R. §§ 825.300(e), 825.301(e). Consequently, the Opinion concludes that the employer is responsible in all circumstances for designating leave as FMLA-qualifying and giving notice of the designation to the employee within five days of learning if events triggering the FMLA eligibility. 29 C.F.R. § 825.300(d).
The Opinion also emphasizes that employers cannot delay the designation of a leave as FMLA protected and provision of notice while a FMLA-eligible employee uses otherwise available leave. While acknowledging that the FMLA permits an employer to require, or to permit an employee to elect, to “substitute” accrued paid leave (e.g., paid vacation, paid sick leave, etc.) to cover any part of the unpaid FMLA entitlement period,the Opinion states that “[t]he term substitute means that the paid leave provided by the employer … will run concurrently with the unpaid FMLA leave.” 29 C.F.R. § 825.207(a) (emphasis added). While acknowledging that the FMLA allows employers to adopt leave policies more generous than those required by the FMLA. 29 U.S.C. § 2653; see 29 C.F.R. § 825.700, the Opinion also says an employer may not designate more than 12 weeks of leave—or more than 26 weeks of military caregiver leave—as FMLA-protected. See, e.g., Weidner v. Unity Health Plans Ins. Corp., 606 F. Supp. 2d 949, 956 (W.D. Wis. 2009) (citing cases for the principle that “a plaintiff cannot maintain a cause of action under the FMLA for an employer’s violation of its more-generous leave policy”).
Furthermore, the Opinion also openly rejects and disagrees with the Ninth Circuit’s holding in Escriba v. Foster Poultry Farms, Inc., 743 F.3d 1236, 1244 (9th Cir. 2014) that an employee may use non-FMLA leave for an FMLA-qualifying reason and decline to use FMLA leave in order to preserve FMLA leave for future use. Instead, the Opinion adopts the position that once an eligible employee communicates a need to take leave for an FMLA-qualifying reason, neither the employee nor the employer may decline FMLA protection for that leave. See 29 C.F.R. § 825.220(d) (“Employees cannot waive, nor may employers induce employees to waive, their prospective rights under FMLA.”); Strickland v. Water Works and Sewer Bd. of City of Birmingham, 239 F.3d 1199, 1204 (11th Cir. 2001) (noting that the employer may not “choose whether an employee’s FMLA-qualifying absence” is protected or unprotected by the FMLA). Accordingly, the Opinion concludes that when an employer determines that leave is for an FMLA-qualifying reason, the qualifying leave is FMLA-protected and counts toward the employee’s FMLA leave entitlement. Once the employer has enough information to make this determination, the employer must, absent extenuating circumstances, provide notice of the designation within five business days. Therefore, the employer may not delay designating leave as FMLA-qualifying or providing notification, even if the employee would prefer that the employer delay the designation.
The Opinion also clarifies the WHD’s interpretation of the FMLA limits the protection of the FMLA to the statutory period set by the FMLA. In this respect, the Opinion states, “An employer is also prohibited from designating more than 12 weeks of leave (or 26 weeks of military caregiver leave) as FMLA leave.” Thus, while acknowledging that “[a]n employer must observe any employment benefit program or plan that provides greater family or medical leave rights to employees than the rights established by the FMLA.” under 29 C.F.R. § 825.700, the Opinion also states that “providing such additional leave outside of the FMLA cannot expand the employee’s 12-week (or 26-week) entitlement under the FMLA.” Therefore, the Opinion states that if an employee substitutes paid leave for unpaid FMLA leave, the employee’s paid leave counts toward his or her 12-week (or 26-week) FMLA entitlement and does not expand that entitlement.
As many employers currently coordinate and administer their FMLA and other leaves inconsistently with the positions stated in the Opinion, employers generally should consult with experienced legal counsel within the scope of attorney client privilege about the implications of the guidance set forth in the Opinion on their existing practices and about whether any corrective action or modifications are advisable in light of the Opinion to minimize potential exposure to FMLA liability. In connection with this review, employers also generally will want to evaluate their other paid and unpaid military, medical, maternity/paternity, adoption and other absence and leave policies and associated employee benefit plans to confirm that these designs continue to operate as intended and that current coordination practices comport with existing guidance.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, FMLA and other leave, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; audits, investigations, enforcement and defense; Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2019 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on Employers Risk FMLA Violation By Delaying FMLA Notification, Designation While Employees Use Other Leave |
Comments Off on Employers Risk FMLA Violation By Delaying FMLA Notification, Designation While Employees Use Other Leave |  compliance, Corporate Compliance, Disability, Disability Leave, Disability Plans, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, enforcement, family leave, HR, Human Resources, Internal Controls, Internal Investigations, Leave, Management, medical leave, Military Leave, veterans, VEVRAA | Tagged: department of labor, Disability Leave, Employee, Employee Benefits, Employer, Family Leave, FMLA, Human Resources, medical leave, Military Leave, Wage and Hour division |
compliance, Corporate Compliance, Disability, Disability Leave, Disability Plans, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, enforcement, family leave, HR, Human Resources, Internal Controls, Internal Investigations, Leave, Management, medical leave, Military Leave, veterans, VEVRAA | Tagged: department of labor, Disability Leave, Employee, Employee Benefits, Employer, Family Leave, FMLA, Human Resources, medical leave, Military Leave, Wage and Hour division |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 7, 2018
The Internal Revenue Service is warning human resources and other business leaders about a growing wave of identity theft and W-2 scams targeting sensitive tax data employers collect on their employees. The warning highlights one of the many growing data breach exposures businesses must manage as identity thieves become ever more sophisticated.
Such data like Form W-2 data – is highly valued by identity thieves. While identity thieves use a variety of tactics to steal this information including hacking into the IRS’ own systems, the IRS this week is warning about one scheme that the IRS says has become one of the more dangerous email scams.
All employers are targets for the W-2 scam, according to the IRS.
Here’s how it works:
- These emails appear to be from an executive or organization leader to a payroll or human resources employee.
- The message usually starts with a simple greeting, like: “Hey, you in today?”
- By the end of the email exchange, all of an organization’s Forms W-2 for their employees may be in the hands of cybercriminals.
- Because payroll officials believe they are corresponding with an executive, it may take weeks for someone to realize a data theft has occurred.
- Generally, the criminals are trying to quickly take advantage of their theft, sometimes filing fraudulent tax returns a day or two.
The IRS warns this scam is such a threat to taxpayers that a special IRS reporting process has been established. The IRS says employers victimized should:
- Email dataloss@irs.gov to notify the IRS of a W-2 data loss and provide contact information. In the subject line, type “W2 Data Loss” so that the email can be routed properly. The business should not attach any employee personally identifiable information data.
- Email the Federation of Tax Administrators at StateAlert@taxadmin.org to get information on how to report victim information to the states.
- File a complaint with the FBI’s Internet Crime Complaint Center. Businesses and payroll service providers may be asked to file a report with their local law enforcement agency.
- Notify employees. The employee may then take steps to protect themselves from identity theft. The Federal Trade Commission’s www.identitytheft.govprovides guidance on general steps employees should take.
- Forward the scam email to phishing@irs.gov.
The IRS also recommends the following resources:
The IRS alert reminds businesses again about the growing challenges they face guarding sensitive tax, health and other employee benefit plan and other data about employees, customers, business partners and others. Aside from the disruptions businesses incur to organizations and relationships with employees, customers, business partners or others and often tremendous costs of investigation and mitigation, breaches also commonly trigger substantial legal liability under a myriad of federal and state laws and regulations, contracts, and common law tort claims. Businesses generally and Human Resources, tax and other systems and operations should take well documented steps to prevent and prepare for a potential breach.
About the Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for 30+ years of management focused employment, employee benefit and insurance, workforce and other management work, public policy leadership and advocacy, coaching, teachings, and publications.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving and author of “What To Do When Your Employee’s Personal Life Becomes Your Business@ and a multitude of other highly regarded works on data protection and breach, her work includes career-long, leading edge involvement counseling and representing human resources, employee benefit, insurance and financial, tax, healthcare and other businesses about data and other sensitive information privacy and breach.
Ms. Stamer’s clients include employers and other workforce management organizations; employer, union, association, government and other insured and self-insured health and other employee benefit plan sponsors, benefit plans, fiduciaries, administrators, and other plan vendors; domestic and international public and private health care, education and other community service and care organizations; managed care organizations; insurers, third-party administrative services organizations and other payer organizations; and other private and government organizations and their management leaders.
Throughout her 30 plus year career, Ms. Stamer has continuously worked with these and other management clients to design, implement, document, administer and defend hiring, performance management, compensation, promotion, demotion, discipline, reduction in force and other workforce, employee benefit, insurance and risk management, health and safety, and other programs, products and solutions, and practices; establish and administer compliance and risk management policies; comply with requirements, investigate and respond to government, accreditation and quality organizations, regulatory and contractual audits, private litigation and other federal and state reviews, investigations and enforcement actions; evaluate and influence legislative and regulatory reforms and other regulatory and public policy advocacy; prepare and present training and discipline; handle workforce and related change management associated with mergers, acquisitions, reductions in force, re-engineering, and other change management; and a host of other workforce related concerns. Ms. Stamer’s experience in these matters includes supporting these organizations and their leaders on both a real-time, “on demand” basis with crisis preparedness, intervention and response as well as consulting and representing clients on ongoing compliance and risk management; plan and program design; vendor and employee credentialing, selection, contracting, performance management and other dealings; strategic planning; policy, program, product and services development and innovation; mergers, acquisitions, bankruptcy and other crisis and change management; management, and other opportunities and challenges arising in the course of workforce and other operations management to improve performance while managing workforce, compensation and benefits and other legal and operational liability and performance.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, heavily involved in health benefit, health care, health, financial and other information technology, data and related process and systems development, policy and operations throughout her career, and scribe of the ABA JCEB annual Office of Civil Rights agency meeting, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues. She regularly helps employer and other health benefit plan sponsors and vendors, health industry, insurers, health IT, life sciences and other health and insurance industry clients design, document and enforce plans, practices, policies, systems and solutions; manage regulatory, contractual and other legal and operational compliance; vendors and suppliers; deal with Medicare, Medicaid, CHIP, Medicare/Medicaid Advantage, ERISA, state insurance law and other private payer rules and requirements; contracting; licensing; terms of participation; medical billing, reimbursement, claims administration and coordination, and other provider-payer relations; reporting and disclosure, government investigations and enforcement, privacy and data security; and other compliance and enforcement; Form 990 and other nonprofit and tax-exemption; fundraising, investors, joint venture, and other business partners; quality and other performance measurement, management, discipline and reporting; physician and other workforce recruiting, performance management, peer review and other investigations and discipline, wage and hour, payroll, gain-sharing and other pay-for performance and other compensation, training, outsourcing and other human resources and workforce matters; board, medical staff and other governance; strategic planning, process and quality improvement; HIPAA administrative simplification, meaningful use, EMR, HIPAA and other technology, data security and breach and other health IT and data; STARK, antikickback, insurance, and other fraud prevention, investigation, defense and enforcement; audits, investigations, and enforcement actions; trade secrets and other intellectual property; crisis preparedness and response; internal, government and third-party licensure, credentialing, accreditation, HCQIA, HEDIS and other peer review and quality reporting, audits, investigations, enforcement and defense; patient relations and care; internal controls and regulatory compliance; payer-provider, provider-provider, vendor, patient, governmental and community relations; facilities, practice, products and other sales, mergers, acquisitions and other business and commercial transactions; government procurement and contracting; grants; tax-exemption and not-for-profit; 1557 and other Civil Rights; privacy and data security; training; risk and change management; regulatory affairs and public policy; process, product and service improvement, development and innovation, and other legal and operational compliance and risk management, government and regulatory affairs and operations concerns.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in pensions, healthcare, workforce, immigration, tax, education and other areas, Ms. Stamer has been extensively involved in U.S. federal, state and local health care and other legislative and regulatory reform impacting these concerns throughout her career. Her public policy and regulatory affairs experience encompasses advising and representing domestic and multinational private sector health, insurance, employee benefit, employer, staffing and other outsourced service providers, and other clients in dealings with Congress, state legislatures, and federal, state and local regulators and government entities, as well as providing advice and input to U.S. and foreign government leaders on these and other policy concerns.
Author of leading works on a multitude of labor and employment, compensation and benefits, internal controls and compliance, and risk management matters and a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (214) 452-8297 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice or an offer or commitment to provide legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as legal advise or an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication or the topic of this article, please contact the author directly. All other rights reserved.
 Comments Off on Identity Theft Scan Targets Employee Tax Records |
Comments Off on Identity Theft Scan Targets Employee Tax Records |  ADA, Attorney-Client Privilege, Civil Rights, Claims Administration, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, defined contribution plan, directors, Disability, Disability Plans, Discrimination, Educational Privacy, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, fiduciary duty, Fiduciary Responsibility, Government Contractors, Identity Theft, Insurance, insurers, Non-Compete, Non-compete, Non-Competition Agreement, Protected Health Information, Retail, Tax, third party administrators, Trade secret, Uncategorized |
ADA, Attorney-Client Privilege, Civil Rights, Claims Administration, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, defined contribution plan, directors, Disability, Disability Plans, Discrimination, Educational Privacy, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, fiduciary duty, Fiduciary Responsibility, Government Contractors, Identity Theft, Insurance, insurers, Non-Compete, Non-compete, Non-Competition Agreement, Protected Health Information, Retail, Tax, third party administrators, Trade secret, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 5, 2018
Construction industry and other employers of employees working in summer heat impacted environments need to take appropriate steps to prevent heat related injuries and illnesses
Every year, dozensof workers die and thousands more become ill while working in extreme heat or humid conditions. More than 40 percent of heat-related worker deaths occur in the construction industry, but workers in every field are susceptible.
Working in extreme heat without appropriate precautions creates heightened risk of a range of heat illnesses. These risks can affect anyone, regardless of age or physical condition.
Employer Responsibility to Protect Workers
Protecting workers from extreme heat generally is part of the responsibility of an employer to provide a safe workplace under the Occupational Health & Safety Act (OSHA) and state occupational health and safety statutes.
Aside from the worker’s compensation, medical and disability costs and workplace disruptions that heat related illness can create, heat related injuries or illnesses to workers also create risks of civil penalties and other liabilities under OSHA.
To minimize risks of heat related OSHA violations and other exposures, an employer of workers exposed to high temperatures should establish and document their training and administration of a complete heat illness prevention program that meets or exceeds applicable OSHA standards.
Resources
OSHA’s Occupational Exposure to Heat page explains what employers can do to keep workers safe and what workers need to know – including factors for heat illness, adapting to working in indoor and outdoor heat, protecting workers, recognizing symptoms, and first aid training. The page also includes resources for specific industries and OSHA workplace standards.
Employers can help promote compliance and reduce heat related injury risks by training and requiring workers and their management to use three common sense elements for preventing heat related injuries and deaths to workers – Water. Rest. Shade.
OSHA guidance urges employers to prevent heat-related injuries by taking the following steps:
- Provide workers with water, rest and shade.
- Allow new or returning workers to gradually increase workloads and take more frequent breaks as they acclimatize, or build a tolerance for working in the heat.
- Plan for emergencies and train workers on prevention.
- Monitor workers for signs of illness.
- Take prompt action to provide appropriate intervention and medical care in response to signs of potential heat related health issues.
To ensure that they can prove these expectations are met, Most employers will want to adopt specific policies require in well-documented compliance with these requirements.
About The Author
If you need more information about or help with these or other workplace concerns, the author of this article may be able to help.
Board Certified in Labor and Employment Law, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing management attorney, consultant, coach, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on labor and employment, compensation, health, pension and other employee benefit, insurance, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following
▪DOL Spending Reports Required As Taxpayer Tool Need Improvement
▪Check & Protect Health & Other Electronic Systems & Data Against New Security Threat
▪April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26
▪Arizona Proposal To Ban Sexual Harassment Confidentiality Agreements Sign Of Growing Employer Risks
▪$23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses
▪Take Care of Your Good People
▪Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source
▪Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning
▪IRS Prepares To Nail Employers Under Obamacare Mandate While Giving Some Individual Mandate Relief
▪Hiring & Retaining Workers Growing Business Challenge
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on |
Comments Off on |  Absenteeism, ADA, board of directors, Claims, compensation, compliance, Construction, Corporate Compliance, Disability Discrimination, Disability Plans, Disaster, Disease Management, Emergency, employee, Employee Handbook, Employer, Employers, Employment, Employment Policies, enforcement, Government Contractors, health Care, health insurance, health plan, Health Plans, HR, Human Resources, Labor Management Relations, Management, mine safety, mining, occupational safety, OSHA, Retaliation, Risk Management, Schools, Uncategorized, Wellness, Wellness Programs, Worker, Workers' Compensation |
Absenteeism, ADA, board of directors, Claims, compensation, compliance, Construction, Corporate Compliance, Disability Discrimination, Disability Plans, Disaster, Disease Management, Emergency, employee, Employee Handbook, Employer, Employers, Employment, Employment Policies, enforcement, Government Contractors, health Care, health insurance, health plan, Health Plans, HR, Human Resources, Labor Management Relations, Management, mine safety, mining, occupational safety, OSHA, Retaliation, Risk Management, Schools, Uncategorized, Wellness, Wellness Programs, Worker, Workers' Compensation |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 10, 2018
Employer and sponsors, fiduciaries, administrators and insurers of employee benefitplansof any type covered by the Employee Retirement Income Security Act (ERISA) making any disability based determinations now have until April 1, 2018 to bring their plans’ claims and appeals procedures for disability-based decisions and related notices and communications into compliance with substantially more complicated requirements in new Department of Labor Employee Benefit Security Administration (EBSA) regulations.
The EBSA announced on January 5, 2018 the extension of the effective date of new requirements for benefit plan processing and providing notification about claims or appeals involving disability determinations from their originally scheduled effective date of January 1, 2018 to April 1, 2018.
While the extension gives employer and other sponsors, fiduciaries, administrators and insurers of employee benefit plans making disability-based benefit determinations a few extra months to review and update their plan documents, summary plan descriptions, procedures, processes and claims and appeals notices to meet tightened new federal rules on disability-based benefit determinations applicable to all post December 31, 2017 claims under the restated Final Rule on Claims Procedure for Plans Providing Disability Benefits (“Disability Claims Rule”), the nature and scope of these new requirements will require updates to virtually all ERISA-covered benefit plans with any disability dependent provisions. These updates are likely to include changes to plan documents, summary plan descriptions, notices, contracts, processes and procedures for a broad range of plans. Consequently, employer and other plan sponsors, fiduciaries, administrators, insurers and others responsible for any benefit plan not already reviewed and updated to comply should get moving to complete the necessary review and update to meet the April 1, 2018 deadline.
Cynthia Marcotte Stamer and others will lead a free telephone study group discussion of “Claims Regulations and Other Developments Affecting Plan Fiduciaries” on January 26, 2018 beginning at 1 PM (Eastern), Noon (Central), 11 AM (Mountain), and 10 AM (Pacific). For more details about the Study Group, see here.
New Disability Claims Rule Overview
Originally published in final form by the EBSA on December 16, 2016, the Disability Claims Rule generally require all ERISA-covered employee benefit plans making any disability benefit or other determination conditioned upon a finding of disability to comply with the new Disability Claims Rule for any claim received after March 31, 2018.
Based on EBSA’s previously adopted Patient Protection and Affordable Care Act (“ACA”) group health plan claims and appeals rules, the new Final Disability Claims Rule will apply to all disability determinations made under any ERISA-covered plan after March 31, 2018, regardless of how the plan characterizes the benefit or whether the plan is a health or other welfare, pension, 401(k) plan or other savings plan.
The new Disability Claims Rule will apply to a broad range of plans, most of which historically have not followed the detailed claims and appeals notification, independent and impartial decision-making, rescission, deemed exhaustion, “culturally and linguistically appropriate” and other procedural protections and safeguards that the Disability Claims Rule extends from the current group health plan rules to all ERISA-covered plans making benefit determinations based on disability. Consequently covered plans making disability-based benefit or other covered determinations are likely to require updates to plan documents, insurance or administrative services contracts, summary plan descriptions and other plan communications, claims and appeals notices, and other related processes, procedures and documentation to meet these new requirements. Since certain requirements of the Disability Claims Rules like the summary plan description advance disclosure requirements are required to be provided before the claim is received, plans and their sponsors, fiduciaries, insurers and administrators risk being accused of violating these requirements by waiting to update plans, their processes and materials until after claim involving a disability based determination arises.
Ensuring that impacted plans are updated before the April 1, 2018 deadline is important because the Disability Claims Rule, like the group health plan claims and appeals rules upon which it is based, also states that noncompliance with any of its requirements empowers a participant to immediately sue the plan for enforcement if his rights without further complying the the plan’s administrative procedures. Moreover, failing to comply with summary plan disclosure or claims or appeal adverse benefit determination notification requirements also may subject the plan administrator to administrative penalties under ERISA section 514(c); fiduciaries to ERISA fiduciary liability, and compromise the ability to defend otherwise defensible decisions. Consequently, employers and other plan sponsors, fiduciaries, administrators and insurers will want to act quickly to ensure that their plans, their summary plan descriptions and other communications, notices, processes, contracts and procedures are updated appropriately before April 1, 218.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |
Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |  401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |
401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 18, 2017
Employers, employee benefit plan sponsors and administrators, vendors and their advisors and service providers should re-evaluate their existing payroll and other settings and elections, planning, testing and related strategies and assumptions in light of the 2018 annual cost-of-living adjustments (COLAs) to the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits announced by the Internal Revenue Service (IRS) in Notice 2017-64, IRB 2017-45 on November 6, 2017.
H.R. 1, Tax Cuts and Jobs Act (Tax Refirm Bill) reported out of the Conference Committee last week and scheduled for a vote before Congress tomorrow leaves these limits substantially unchanged.
Notice 2017-64 adjusts the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits. The Section 415 limitations COLAs are made and published annually to comply with Section 415(d)’s requirement that the Treasury Security annually adjust these limits for cost-of-living increases. Other limitations applicable to deferred compensation plans are also affected by these adjustments under § 415. Under § 415(d), the adjustments are to be made under adjustment procedures similar to those used to adjust benefit amounts under § 215(i)(2)(A) of the Social Security Act.
In addition to impacting contribution limits permitted to defined benefit, 401(k) and other defined contribution and other plans, the changes can impact the definition of highly compensated employees, discrimination testing, plan funding and a broad range of employee benefit, compensation, tax, payroll, union or other contracting and other concerns for employers, employee benefit plan sponsors, fiduciaries, administrators, payroll, plan and other vendors, participants and beneficiaries and others.
The following is a chart of the adjusted limits compared to the currently applicable 2017 limitations. (Download chart)
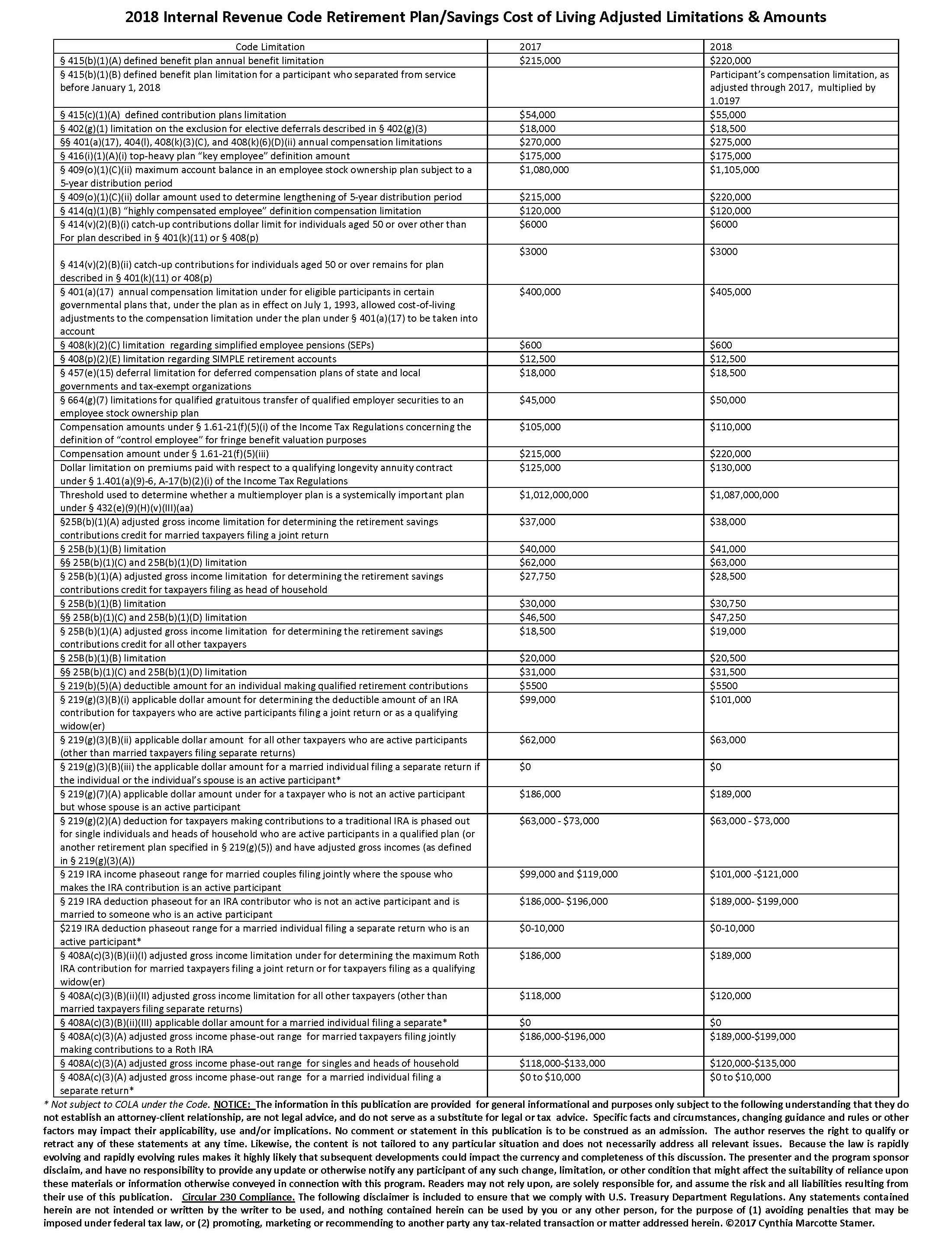
Employers, employee benefit plan sponsors, fiduciaries, administrators and other vendors, participants and beneficiaries and others working with employee benefit plans or compensation contributed to these arrangements should review these new 2018 COLA limitations to assess their potential impact and make appropriate adjustments to avoid compliance challenges or other unfortunate surprises in 2018. If they already have not already done so, reviewing the 2018 Social Security Act COLAs also would be wise. See 2018 Social Security COLAs Set.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |
Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |  401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |
401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 14, 2017
Employer and other sponsors, fiduciaries, administrators and insurers of the Employee Retirement Income Security Act (ERISA)-covered employee benefit plans making disability-based benefit determinations should confirm that their plan documents, summary plan descriptions, procedures and claims and appeals notices are updated and ready to meet tightened new federal rules on disability-based benefit determinations applicable to all post December 31, 2017 claims under the restated Final Rule on Claims Procedure for Plans Providing Disability Benefits (“Disability Claims Rule”). Given the nature and scope of these new requirements, most covered plans will require specific action be taken before the new rules take effect to update plan documents, summary plan descriptions, notices, contracts, processes and procedures to meet the January 1, 2018 deadline.
The Disability Claims Rule published by the Department of Labor Employee Benefit Security Administration (“EBSA”) on December 19, 2016 generally require all ERISA-covered employee benefit plans making any disability benefit or other determination conditioned upon a finding of disability to comply with the new Disability Claims Rule for any claim received after December 31, 2017.
The new Final Disability Claims Rule will apply to all disability determinations made under any ERISA-covered plan after December 31, 2017, regardless of how the plan characterizes the benefit or whether the plan is a health or other welfare, pension, 401(k) plan or other savings plan.
Significant affirmative action is likely required to prepare covered plans to meet these requirements since most plans historically have not followed the detailed claims and appeals notification, independent and impartial decision-making, rescission, deemed exhaustion, “culturally and linguistically appropriate” and other procedural protections and safeguards based on EBSA’s previously adopted Patient Protection and Affordable Care Act (“ACA”) group health plan claims and appeals rules, which the Disability Claims Rules extend and make applicable to all ERISA-covered plans making benefit determinations based on disability. Covered plans making disability-based benefit or other covered determinations are likely to require updates to plan documents, insurance or administrative services contracts, summary plan descriptions and other plan communications, claims and appeals notices, and other related processes, procedures and documentation to meet these new requirements. Since certain requirements of the Disability Claims Rules like the summary plan description advance disclosure requirements are required to be provided before the claim is received, plans and their sponsors risk being accused of violating these requirements by waiting to update plans, their processes and materials until after claim involving a disability based determination arises.
Ensuring that impacted plans are updated before the January 1, 2018 deadline is important because the Disability Claims Rule, like the group health plan claims and appeals rules upon which it is based, also states that noncompliance with any of its requirements empowers a participant to immediately sue the plan for enforcement if his rights without further complying the the plan’s administrative procedures. Moreover, failing to comply with summary plan disclosure or claims or appeal adverse benefit determination notification requirements also may subject the plan administrator to administrative penalties under ERISA section 514(c). Consequently, employers and other plan sponsors, fiduciaries, administrators and insurers will want to act quickly to ensure that their plans, their summary plan descriptions and other communications, notices, processes, contracts and procedures are updated appropriately before January 1, 2018.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediatepast RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, BenefitsMagazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Confirm Your Benefit Plans Ready For New Disability Determination Rules on 1/1/18 |
Comments Off on Confirm Your Benefit Plans Ready For New Disability Determination Rules on 1/1/18 |  401(k), ACA, ADA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Disability, Disability, Disability Plans, Drug & Alcohol, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, Leave, Management, medical leave, Mental Health, Mental Health Parity, Obamacare, Patient Protection & Affordable Care Act, Pay, pension plan, Plan Admistrator, Professional Liability, third party administrators, Uncategorized, Union, Worker | Tagged: Appeals, Claims, defined benefit plan, Disability, Disability Insurance, Disability Plan, EBSA, Employee Retirement Income Security act, ERISA, Fiduciary Responsibility, pension plan |
401(k), ACA, ADA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, compensation, compliance, Construction, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Disability, Disability, Disability Plans, Drug & Alcohol, EBSA, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, Leave, Management, medical leave, Mental Health, Mental Health Parity, Obamacare, Patient Protection & Affordable Care Act, Pay, pension plan, Plan Admistrator, Professional Liability, third party administrators, Uncategorized, Union, Worker | Tagged: Appeals, Claims, defined benefit plan, Disability, Disability Insurance, Disability Plan, EBSA, Employee Retirement Income Security act, ERISA, Fiduciary Responsibility, pension plan |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 14, 2017
Monthly Social Security and Supplemental Security Income (SSI) benefits for more than 66 million Americans will increase 2.0 percent in 2018.
The Social Security Administration announced the 2.0 cost of living adjustment (COLA) Friday announced a 2% increase in benefits for 2018.
The largest COLA increase since 2012 will increase the benefits payable to more than 61 million Social Security beneficiaries in January 2018. Increased payments to more than 8 million SSI beneficiaries will begin on December 29, 2017. The Social Security Administration deducts $1 from benefits for each $3 earned over $45,360 until the month the worker turns age 66.)
There is no limit on earnings for workers who are “full” retirement age or older for the entire year.
The slight increase in benefits also may result in a corresponding decrease in disability benefits under plans that integrate or otherwise offset plan benefits with Social Security.
Information about Medicare COLAs for 2018, when announced, will be available at www.Medicare.gov.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪ RAISE Act Immigration Reforms Touted As “Giving Americans A Raise”
▪ Health Clinic At Houston Convention Center, Other HHS Help For Hurricane Harvey Victims
▪ IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties
▪ DB Plan Sponsors Check Out New Bifurcated Distribution Model Amendmentsy
▪ U.S. News Names 2017-2018 “Best” Hospitals; Patient Usefulness Starts With Metholodogy Understanding
▪ Use Lessons Of Past Mistakes or Injustice To Build Better Future
▪ Prepare For Turnover, Other Challenges From Rising Workforce Competition
▪ Employers, Health Plans Should Brace For Tightened Federal Mental Health Coverage Mandate Disclosure And Enforcement
▪ Withholding Calculator Tool Helps Workers Figure Withholding
▪ Better Preparing U.S. Workers To Fill Your Jobs
▪ SCOTUS Ruling Bars Many State Arbitration Agreement Restrictions
▪ $2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on 2018 Social Security COLAs Set |
Comments Off on 2018 Social Security COLAs Set |  Claims Administration, defined benefit plan, Defined Benefit Plans, Disability, Disability Plans, Employee Benefits, Employer, Employers, Employment, ERISA, HR, Human Resources, pension plan, retirement plan, Retirement Plans, Retirements, Social Security, Uncategorized | Tagged: Social Security, SSI |
Claims Administration, defined benefit plan, Defined Benefit Plans, Disability, Disability Plans, Employee Benefits, Employer, Employers, Employment, ERISA, HR, Human Resources, pension plan, retirement plan, Retirement Plans, Retirements, Social Security, Uncategorized | Tagged: Social Security, SSI |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 1, 2017
Employers and employee benefit plan fiduciaries and administrators should consider sharing the free IRS Withholding Calculator resource offered in English, Spanish, and ASL formats with workers in annual employee benefit enrollment packages, new hire paperwork, bonus announcement and other wage related materials and other employee communications to help workers better understand and manage the tax and other effects of their annual employee benefit elections on their take-home pay. Including reminders to re-evaluate withholding and if necessary, change their W-4 withholding elections also helps employees and their families ensure that withholding elections that workers complete as part of new hire documentation are updated in response to changing taxable income and other relevant events.
Communicating the availability of these free government-resource tools to workers during the annual employee benefit plan enrollment period, year-end, raise or bonus time or other strategic times throughout the year could help employees better appreciate the tax-preferred benefit offerings provided by the employer as well as provide significant financial education benefits many workers need for little or no employer cost.
While enrollment packages typically tout the potential “tax savings” that employees can enjoy from participating in tax-favored, employer-sponsored health, group term life, qualified pension or profit-sharing, and other tax-preferred employee benefit or fringe benefit programs offered by their employers, few employees truly understand how to determine properly their necessary wage withholding on taxable wages, much less the specific effects of their employee benefit elections on their income or employment tax liability or withholding.
A better understanding of the relative tax benefits and savings of enrollment in tax-preferred benefits offered by an employer and their potential implications on the income tax withholding elected by the workers can benefit both employees and their employer. Aside from illustrating in real, meaningful terms specific to the worker the tax benefits of his election of employer-offered, tax preferred benefits, proper tax withholding helps employees avoid unnecessary over withholding that can reduce employees’ take-home pay as well as helps protect employees from unexpectedly higher year-end tax bills that often surprise workers when an employee sets his withholding too low.
While few employers or plans want to incur the potential financial costs or liability of estimating savings for individual workers, sharing information about free government-provided resources like the IRS calculator or using vendor-provided solutions that incorporate tools in employee enrollment and other communications can help employees appreciate the benefits of tax-preferred employee benefits and make more informed choices about their benefits and their withholding.
Educating employees about the availability of these free resources also is a low-cost way of providing valuable information to workers whether or not the employer or plan has a vendor offered solution that includes the same or similar tool. However, educating workers about the availability of the withholding calculator and other tools can be a particularly attractive option for an employer when the employer doesn’t have a vendor-provided option that includes that information or can only access the tool for added charges.
While many vendors offer similar tools and materials sold to employers and employee benefit plans, employers or benefit plan fiduciaries generally must pay fees, share promotional materials or meet at the requirements to deliver those resources as part of a vendor-supplied package. Utilizing these vendor supplied resources without fulfilling these preconditions could expose the employer or plan to potential copyright, trademark or other contractual or intellectual property claims from the vendor. In contrast, IRS withholding calculator and many other government tools can be used or shared freely without these concerns. Moreover, employers and plans are less likely to face challenges for sharing an unfiltered government resource than a similar tool packaged within a vendor communication package promoting other options.
Of course, regardless of whether these or other tools or information are shared as a free-standing tool or as part of a broader communication package, employers, plans and others sharing these government tools and other similar resources generally will want to ensure that the materials are distributed along with and subject to general tax advice and other disclaimers of reliance as well as statements encouraging users to consult with their own qualified tax or other qualified professionals about the users’ specific circumstance.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |
Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |  105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |
105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 31, 2016
U.S. employers, employment agencies, unions, their benefit plans and fiduciaries, and their management and service providers should move quickly to review and strengthen their employment and other practices to guard against a foreseeable surge in employee retaliation claims and judgements likely to follow the August 30, 2016 issuance by the Equal Employment Opportunity Commission (EEOC) of its new final EEOC Enforcement Guidance on Retaliation and Related Issues and concurrently published Question and Answer Guidance(Guidance).
Updating and superceding 2008 guidance previously set forth in the Retaliation Chapter of the EEOC Enforcement Manual, the Guidance details the EEOC’s current policy for investigating and enforcing the retaliation prohibitions under each of the equal employment opportunity (EEO) laws enforced by EEOC, including Title VII of the Civil Rights Act of 1964, the Age Discrimination in Employment Act (ADEA), Title V of the Americans with Disabilities Act (ADA), Section 501 of the Rehabilitation Act, the Equal Pay Act (EPA) and Title II of the Genetic Information Nondiscrimination Act (GINA) as well as the ADA’s separate “interference” prohibitions, which prohibit coercion, threats, or other acts that interfere with the exercise of ADA rights. Among other things, the Guidance discusses :
- What “retaliation means” and the scope of employee activity protected by the prohibitions against retaliation included in all laws enforced by the EEOC as well as the interference prohibitions of the ADA;
- Legal analysis the EEOC will use to determine if evidence supports a claim of retaliation against an employer or other party;
- Detailed examples of employer actions that the EEOC says may constitute prohibited retaliation; and
Remedies available for retaliation.
Understanding and properly responding to the Guidance is critically important for employers and other subject to the EEO laws because in light of the substantial and growing liability exposures retaliation claims present and the likely that the issuance of the Guidance will further fuel these risks.
Even before the EEOC published the Guidance, retaliation and interference exposures were a substantial source of concern for most employers. Employers, employment agencies and unions caught engaging in prohibited retaliation or intimidation in violation of EEO laws can incur compensatory and (except for governmental employers) punitive damage awards, back pay, front pay, reinstatement into a job or other equitable remedies, injunctive or administrative orders requiring changes in employer policies and procedures, managerial training, reporting to the EEOC and other corrective measures, as well as substantial investigation and defense costs.
These substantial liability exposures have become particularly concerning as retaliation and interference claims also have become increasingly common over the past decade. According to the EEOC, for example, EEO law retaliation charges have remained the most frequently alleged basis of charges filed with the EEOC since 2009 and in Fiscal Year 2015 accounted for 44.5 percent of all employment discrimination charges received by EEOC.
Since the EEOC’s issuance of the Retaliation Regs are likely to encourage additional retaliation or interference claims, employers, employment agencies, unions and their management, service providers and agents should quickly to evaluate the updated guidance provided in the Retaliation Reg and act to mitigate their exposure to retaliation retaliation and interference claims under these EEO laws.
Retaliation Risks Under EEO Laws
Federal EEO laws generally prohibit employers, employment agencies, or unions from punishing or taking other adverse actions against job applicants or employees for “asserting their rights” (often referred to as “protected activity”) to be free from harassment or other prohibited employment discrimination as well as certain other conduct. Such claims generally are referred to as “retaliation claims.”
Prohibited retaliation in violation of EEO laws occurs when an employer, employment agency or union takes a materially adverse action because an applicant or employee asserts rights or engages in certain other activities protected by the EEO laws.
To prevail in a retaliation claim, an applicant, employee or other individual generally must show that:
- The individual engaged in prior protected activity;
- The employer, employment agency or union took a materially adverse action; and
- More likely than not, retaliation caused the adverse action by the employer, employment agency or union.
Persons Protected By EEO Retaliation Rules
EEO retaliation prohibitions protect both applicants and current and former employees (full-time, part-time, probationary, seasonal, and temporary) against retaliation under the EEO laws. The retaliation prohibitions bar an employer from refusing to hire or otherwise taking adverse action against any current or former applicant or employee because of his EEO complaint or other protected activity under applicable EEO laws. The EEOC interprets the retaliation rules as prohibiting an employer from giving a false negative job reference to punish a former employee for making an EEO complaint or engaging in other protected activity as well as as prohibiting an employer from refusing to hire or otherwise retaliating or discriminating against an applicant or employee based on a complaint made or other protected activity engaged against any a prior employer. The Guidance also makes clear that the retaliation prohibitions apply regardless of an applicant or employee’s citizenship or work authorization status.
Protected Activity
“Protected activity” generally means either participating in an EEO process or reasonably opposing conduct made unlawful by an EEO law.
The prohibition against an employer retaliating against an individual for “participating” in an EEO process means that an employer cannot punish an applicant or employee for filing an EEO complaint, serving as a witness, or participating in any other way in an EEO matter, even if the underlying discrimination allegation is unsuccessful or untimely. As a part of these prohibitions, the EEOC says that an employer, employment agency or union is not allowed to do anything in response to EEO activity that would discourage someone from resisting or complaining about future discrimination. For example, depending on the facts of the particular case, it could be retaliation because of the employee’s EEO activity for an employer to:
- Reprimand an employee or give a performance evaluation that is lower than it should be;
- Transfer the employee to a less desirable position;
- Engage in verbal or physical abuse;
- Threaten to make, or actually make reports to authorities (such as reporting immigration status or contacting the police);
- Increase scrutiny;
- Spread false rumors, treat a family member negatively (for example, cancel a contract with the person’s spouse); or
-
Take action that makes the person’s work more difficult (for example, punishing an employee for an EEO complaint by purposefully changing his work schedule to conflict with family responsibilities).
The Guidance clearly states that the EEOC views participating in any capacity in a complaint process or other protected equal employment opportunity as protected activity which is protected from retaliation under all circumstances. The EEOC views other acts to oppose discrimination also as protected as long as the employee was acting on a reasonable belief that something in the workplace may violate EEO laws, even if he or she did not use legal terminology to describe the issue. EEOC’s view is that protections against retaliation extend to participation in an employer’s internal EEO complaint process, even if a charge of discrimination has not yet been filed with the EEOC. The EEOC also takes the position that participation in the EEO process is protected whether or not the EEO allegation is based on a reasonable, good faith belief that a violation occurred. While an employer is free to bring these to light in the EEO matter where it may rightly affect the outcome, the Retaliation Regs state it is unlawful retaliation for an employer to take matters into its own hands and impose consequences for participating in an EEO matter.
In addition to prohibition for participation in protected activities, EEO law also prohibits retaliation against an individual for “opposing” a perceived unlawful EEO practice. The EEOC construes prohibition against retaliation for opposition as prohibiting an employer or other covered entity from punishing an applicant or employee for communicating or taking other action in opposition of a perceived EEO violation if the individual acted reasonably and based on a reasonable good faith belief that the conduct opposed is or could become unlawful if repeated.
According to the EEOC, opposition also can be protected even if it is informal or does not include the words “harassment,” “discrimination,” or other legal terminology. A communication or act may be protected opposition as long as the circumstances show that the individual is conveying resistance to a perceived potential EEO violation such as, for example:
- Complaining or threatening to complain about alleged discrimination against oneself or others;
- Taking part in an internal or external investigation of employment discrimination, including harassment;
- Filing or being a witness in a charge, complaint, or lawsuit alleging discrimination;
- Communicating with a supervisor or manager about employment discrimination, including harassment;
- Answering questions during an employer investigation of alleged harassment;
- Refusing to follow orders that would result in discrimination;
- Resisting sexual advances, or intervening to protect others;
- Reporting an instance of harassment to a supervisor;
- Requesting accommodation of a disability or for a religious practice;
- Asking managers or co-workers about salary information to uncover potentially discriminatory wages;
- Providing information in an employer’s internal investigation of an EEO matter;
- Refusing to obey an order reasonably believed to be discriminatory;
- Advising an employer on EEO compliance;
- Resisting sexual advances or intervening to protect others;
- Passive resistance (allowing others to express opposition);
- Requesting reasonable accommodation for disability or religion;
- Complaining to management about EEO-related compensation disparities;
- Talking to coworkers to gather information or evidence in support of a potential EEO claim; or
- Other acts of opposition.
In order for the protection against opposition to apply, however, the individual must act with a reasonable good faith belief that the conduct opposed is unlawful or could become unlawful if repeated. Opposition not based on such a good faith belief is not protected. Employers should note that the EEOC takes the position that opposition by an employee could qualify as reasonable opposition protected against retaliation when an employee or applicant complains about behavior that is not yet legally harassment (i.e., even if the mistreatment has not yet become severe or pervasive) or to complain about conduct the employee believes violates the EEO laws if the EEOC has adopted that interpretation, even if some courts disagree with the EEOC on the issue.
Furthermore, an individual opposing a perceived violation of an EEO law is disqualified for protection against retaliation for his opposition unless the individual behaves in a reasonable manner when expressing his opposition. For example, threats of violence, or badgering a subordinate employee to give a witness statement, are not protected opposition.
Subject to these conditions, however, the Guidance states that retaliation for opposing perceived unlawful EEOC practices need not be applied directly to the employee to qualify for protection. If an employer, employment agency or union takes an action against someone else, such as a family member or close friend, in order to retaliate against an employee, the EEOC says both individuals would have a legal claim against the employer.
Moreover, according to the EEOC, the prohibitions against retaliation for participation and opposition apply regardless of whether the person is suffers the retaliation for acting as a witness or otherwise participating in the investigation of a prohibited practice regarding an EEO complaint brought by others, or for complaining of conduct that directly affects himself.
Materially Adverse Action
To fall within EEO law prohibitions against retaliation, the retaliatory actions must be “materially adverse,” which the Guidance defines to include any action that under the facts and circumstances might deter a reasonable person from engaging in protected activity. This definition of “materially adverse” sweeps broadly to include more than employment actions such as denial of promotion, non-hire, denial of job benefits, demotion, suspension, discharge, or other actions that can be challenged directly as employment discrimination. It also encompasses within the scope of retaliation employer action that is work-related, as well as other actions with no tangible effect on employment, or even an action that takes place exclusively outside of work, as long as it may well dissuade a reasonable person from engaging in protected activity.
Whether an action is materially adverse depends on the facts and circumstances of the particular case. The U.S. Supreme Court has held that transferring a worker to a harder, dirtier job within the same pay grade, and suspending her without pay for more than a month (even though the pay was later reimbursed) were both “materially adverse actions” that could be challenged as retaliation. The Supreme Court has also said that actionable retaliation includes: the FBI’s refusing to investigate death threats against an agent; the filing of false criminal charges against a former employee; changing the work schedule of a parent who has caretaking responsibilities for school-age children; and excluding an employee from a weekly training lunch that contributes to professional advancement.
In contrast, a petty slight, minor annoyance, trivial punishment, or any other action that is not likely to dissuade an employee from engaging in protected activity in the circumstances is not “materially adverse.” For example, courts have concluded on the facts of given cases that temporarily transferring an employee from an office to a cubicle was not a materially adverse action and that occasional brief delays by an employer in issuing refund checks to an employee that involved small amounts of money were not materially adverse.
The facts and circumstances of each case determine whether a particular action is retaliatory in that context. For this reason, the same action may be retaliatory in one case but not in another. Depending on the facts, other examples of “materially adverse” actions may include:
- Work-related threats, warnings, or reprimands;
- Negative or lowered evaluations;
- Transfers to less prestigious or desirable work or work locations;
- Making false reports to government authorities or in the media;
- Filing a civil action;
- Threatening reassignment;
- Scrutinizing work or attendance more closely than that of other employees, without justification;
- Removing supervisory responsibilities;
- Engaging in abusive verbal or physical behavior that is reasonably likely to deter protected activity, even if it is not yet “severe or pervasive” as required for a hostile work environment;
- Requiring re-verification of work status, making threats of deportation, or initiating other action with immigration authorities because of protected activity;
- Terminating a union grievance process or other action to block access to otherwise available remedial mechanisms; or
- Taking (or threatening to take) a materially adverse action against a close family member (who would then also have a retaliation claim, even if not an employee).
ADA Interference Claims
In addition to the need to manage potential exposures for prohibited retaliation, employers, employment agencies and unions also should be careful to manage their exposure to potential liability arising from claims for wrongful interference and individual’s exercise of the disability rights or protections granted under the ADA.
The ADA generally prohibits disability discrimination, limits an employer’s ability to ask for medical information, requires confidentiality of medical information, and gives employees who have disabilities the right to reasonable accommodations at work absent undue hardship and like other EEO laws, prohibits retaliation. In addition to its prohibitions against retaliation, however, the ADA also more broadly prohibits “interference” with statutory rights under the ADA.
Interference is broader than retaliation. The ADA’s interference provision makes it unlawful to coerce, intimidate, threaten, or otherwise interfere with an individual’s exercise of ADA rights, or with an individual who is assisting another to exercise ADA rights.
In addition, the ADA also prohibits employers from interfering with ADA rights by doing anything that makes it more difficult for an applicant or employee to assert any of these rights such as using threats or other actions to discourage someone from asking for, or keeping, a reasonable accommodation; intimidating an applicant or employee into undergoing an unlawful medical examination; or pressuring an applicant or employee not to file a disability discrimination complaint.
Prohibited interference may be actionable under the ADA even if ineffective and even if the person subjected to intimidation goes on to exercise his ADA rights.
- While acknowledging that some employer actions may be both retaliation and interference, or may overlap with unlawful denial of accommodation, the Guidance identifies the following actions as examples of interference prohibited under the ADA:
- Coercing an individual to relinquish or forgo an accommodation to which he or she is otherwise entitled;
- Intimidating an applicant from requesting accommodation for the application process by indicating that such a request will result in the applicant not being hired;
- Threatening an employee with loss of employment or other adverse treatment if he does not “voluntarily” submit to a medical examination or inquiry that is otherwise prohibited under the statute;
- Issuing a policy or requirement that purports to limit an employee’s rights to invoke ADA protections (e.g., a fixed leave policy that states “no exceptions will be made for any reason”);
- Interfering with a former employee’s right to file an ADA lawsuit against the former employer by stating that a negative job reference will be given to prospective employers if the suit is filed; and
- Subjecting an employee to unwarranted discipline, demotion, or other adverse treatment because he assisted a coworker in requesting reasonable accommodation.
According to the EEOC, a threat does not have to be carried out in order to violate the interference provision, and an individual does not actually have to be deterred from exercising or enjoying ADA rights in order for the interference to be actionable.
Strategies To Help Deter Or Rebut Retaliation Charges
Even though individuals claiming retaliation technically bear the burden of proving more likely than not that he suffered an adverse employment action more probably than not as a result of retaliation, an employer, employment agency or union charged with illegal retaliation frequently need to rebut or undermine a claimant’s evidence of retaliation by having and introducing admissible evidence that it a non-retaliatory reason for taking the challenged action such as evidence that:
- The employer was not, in fact, aware of the protected activity;
- There was a legitimate non-retaliatory motive for the challenged action, that the employer can demonstrate, such as poor performance; inadequate qualifications for position sought; qualifications, application, or interview performance inferior to the selectee; negative job references (provided they set forth legitimate reasons for not hiring or promoting an individual); misconduct (e.g., threats, insubordination, unexcused absences, employee dishonesty, abusive or threatening conduct, or theft); or reduction in force or other downsizing;
- Similarly-situated applicants or employees who did not engage in protected activity were similarly treated;
- Where the “but-for” causation standard applies, there is evidence that the challenged adverse action would have occurred anyway, despite the existence of a retaliatory motive; or
- Other credible evidence showing a legitimate, non-discriminatory and non-retalitory motive behind the action.
It is important that employer other other potential defendants in retaliation actions recognize and take appropriate steps to create and retain evidence documenting these or other legitimate business reasons justifying the action prior to taking adverse action. Many employer or other defendants charged with discrimination or retaliation discover too late that a rule of evidence commonly referred to as the “After Acquired Evidence Doctrine” often prevents an employer or other defendant from using documentation or other evidence of motive created after the adverse action occurs. Consequently, employer and other potential targets of retaliation claims before taking the adverse action would be wise to carefully collect, document and retain the evidence and analysis showing their adverse action was taken for a legitimate, nonretalitory, nondiscriminatory reason rather than for any retaliatory purpose.
Other Defensive Actions & Strategies
Beyond taking care to document and retain evidence of its legitimate motivations for taking an adverse employment action, employers, employment agencies and unions interested in avoiding or enhancing their defenses against retaliation or interference claims also may find it helpful to:
- Maintain a written, plain-language anti-retaliation and anti-interference policy that provides practical guidance on the employer’s expectations with user-friendly examples of what to do and not to do;
- Send a message from top management that retaliation and interference are prohibited and will not be tolerated;
- Ensure that top management understands and complies with policies against prohibited discrimination, retaliation and interference;
- Consistently and fairly administer all equal employment opportunity and other policies and procedures in accordance with applicable laws in a documented, defensible manner;
- Post and provide all required posters or other equal employment opportunity notices;
- Timely and accurately complete and file all required EEO reports;
- Clearly communicate orally and in writing the policy against prohibited retaliation and interference, as well as procedures for reporting, investigating and addressing concerns about potential violations of these policies in corporate policies as well as to employees complaining or participating in investigations or other protected activities;
- Conduct documented training for all managers, supervisors and other employees and agents of the employer about policies against prohibited discrimination, retaliation, and interference including, as necessary, specific education about specific behaviors or situations that could raise retaliation or interference concerns, when and how to report or respond to such concerns and other actions to take to prevent or stop potential retaliation and interference;
- Establish and administer clear policies and procedures for reporting and investigating claims or other indicators of potential prohibited employment discrimination, retaliation, interference including appropriate procedures for monitoring and protecting applicants and workers who have made claims of discrimination or have a record of involvement in activities that might qualify for corrective action;
- Review performance, compensation and other criteria for potential evidence of overt or hidden bias or other evidence of potential prohibited retaliation or interference and take documented corrective action as needed to prevent improper bias from adversely corrupting decision-making process;
- Conduct timely, well-documented investigations of all reports or other evidence of suspected discrimination, retaliation, and interference including any disciplinary, remedial or corrective action taken or foregone and the justification underlying these actions;
- Obtain and enforce contractual reassurances from recruiting, staffing and other contractors to adhere to, and cooperate with the employer in its investigation and redress of the nondiscrimination, data collection and reporting, anti-retaliation and anti-interference requirements of equal employment opportunity and other laws;
- Incorporate appropriate inquiries and other procedures for documented evaluating and monitoring that hiring, staffing, performance review, promotion, demotion, discipline, termination and other employment decisions and actions for evidence or other indicators of potential prohibited discrimination, retaliation, interference or other prohibited conduct and take corrective action as necessary based on the evidence developed; and
- Designate appropriately empowered and trained members of the management of the employer to receive and investigate complaints and other potential concerns;
Arrange for an unbiased third party review of the adverse action or the performance or other decision criteria, processes and analysis that the employer or other defendant contemplates relying on to decide and implement employment decisions for indicators of potential discriminatory, retaliatory or other illegal or undesirable biasand take corrective action as needed to address those concerns before undertaking employment actions;
- Evaluate and allocate appropriate funds within the employer’s budget to support the employer’s compliance efforts as well as to provide for the availability of sufficient funds to investigate and defend potential charges or public or private charges of illegal discrimination, retaliation or interference through the purchase of employment practices liablity or other insurance coverages or otherwise;
- If a manager or other party recommends an adverse action in the wake of an employee’s filing of an EEOC charge or participation in other protected activity, conducting or arranging for an another party to ndependently evaluate whether the adverse action is appropriate;
- Proactively seek assistance from qualified legal counsel with the design and review of policies, practices and operations, investigation and analysis of internal or external complaints or other concerns about potential prohibited discrimination, retaliation or interference, review and execution of termination, discipline or other workforce events to mitigate discrimination, retaliation or interference risks as well as the defense of EEOC or private enforcement actions; and
- Be ever diligent in your efforts to prevent, detect and redress actions or situations that could be a basis for retaliation or interference claims.
About The Author
Cynthia Marcotte Stamer is a noted Texas-based management lawyer and consultant, author, lecture and policy advocate, recognized for her nearly 30-years of cutting edge management work as among the “Top Rated Labor & Employment Lawyers in Texas” by LexisNexis® Martindale-Hubbell® and as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,”“Tax: Erisa & Employee Benefits” “Health Care” and “Business and Commercial Law” by D Magazine.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Chair and current committee Co-Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, former Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, a former ABA Joint Committee on Employee Benefits Council Representative and , Ms. Stamer helps management manage.
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal control and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.Solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. ©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
 Comments Off on Manage Retaliation Risks In Response To Updated EEOC Enforcement Guidance, Rising Retaliation Claims |
Comments Off on Manage Retaliation Risks In Response To Updated EEOC Enforcement Guidance, Rising Retaliation Claims |  Accommodation, ADA, Affirmative Action, Civil Rights, compensation, Corporate Compliance, corporate governance, Disability, Disability, Disability Discrimination, Disability Plans, Discrimination, E-Verify, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Government Contractors, Hiring, HR, Human Resources, Internal Controls, Internal Investigations, Leave, LEP, LGBT, Management, Managment, Risk Management, Sexual Harassment, Uncategorized, Workforce | Tagged: Civl Rights, Discrimination, EEOC, Employee, Employer, Employment Agency, employment discrimination, Equal Employment Opportunity, Interference, Retaliation, Union |
Accommodation, ADA, Affirmative Action, Civil Rights, compensation, Corporate Compliance, corporate governance, Disability, Disability, Disability Discrimination, Disability Plans, Discrimination, E-Verify, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Government Contractors, Hiring, HR, Human Resources, Internal Controls, Internal Investigations, Leave, LEP, LGBT, Management, Managment, Risk Management, Sexual Harassment, Uncategorized, Workforce | Tagged: Civl Rights, Discrimination, EEOC, Employee, Employer, Employment Agency, employment discrimination, Equal Employment Opportunity, Interference, Retaliation, Union |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 1, 2016
The U.S. Department of Labor’s just announced successful whistleblower prosecution in Perez v. Scott Brain, et al of an employee benefit plan trustee, and an individual lawyer and her law firm that served as the employee benefit plan’s outside legal counsel of violating the fiduciary responsibility and whistleblower rules of the Employee Retirement Income Security Act of 1974 (ERISA) illustrates why employee benefit plan sponsors, trustees or other fiduciaries, their management, legal counsel, auditors and other service providers must both prudently investigate whistleblower allegations or other evidence of potential wrongdoing involving their employee benefit plans and resist the temptation to retaliate against employees or others for reporting or cooperating in the investigation of alleged improprieties involving an employee benefit plan.
The Brain decision highlights the care that employee benefit plan sponsors, fiduciaries, advisors and service providers and their management must use when responding to allegations or other evidence of wrongdoing relating to an employee benefit plan or its administration, investigating and addressing alleged misconduct or other performance or disciplinary concerns involving parties whose report or involvement in investigations of ERISA or other misconduct could form the basis of a potential ERISA 510 or other retaliation complaint.
The decision also makes clear that outside legal counsel advising an employee benefit plan or its fiduciaries in relation to the investigation or response to charges of ERISA misconduct involving an employee benefit plan must use care to avoid actions that could render them liable for participation in acts of illegal retaliation, violating their duty of loyalty to the plan by allowing themselves to become involved in a conflict of interest when investigating or defending potential wrongdoing involving an employee benefit plan, or engaging in other discretionary actions that could constitute a breach of fiduciary duty in violation of ERISA.
In Perez v. Scott Brain, et al., the U.S. District Court for the Central District of California ruled that Cement Masons Southern California Trust Fund’s trustee and Cement Masons Local 600 business manager, Scott Brain (Brain) and outside trust fund legal counsel, Melissa Cook, violated sections 510 and 404 of ERISA by causing the firing a trust fund employee Cheryle Robbins (Robbins) and an employee of the plan’s third party administrator, Cory Rice (Rice), in retaliation for their involvement in filing an internal complaint about and cooperating with the Labor Department’s Employee Benefit Security Administration’s federal criminal investigation of reports of Brain’s wrongful interference as a trustee with collections and contributions from unionized employers.
In 2011, Robbins, director of the trust funds’ audit and collections department, responded to a federal criminal investigation into Brain’s activities with contractors. The same year, she and Rice, who worked for the third-party administrator to the trust fund, American Benefit Plan Administrators, now, Zenith American Solutions (Zenith), participated in an effort to complain about Brain’s interference with efforts to collect delinquent contributions from contractors. Within weeks of this conduct, Robbins was suspended from her employment with the trust fund. Less than six months later, both Robbins and Rice were fired.
The court’s 71-page decision chronicles the coordinated retaliatory campaign orchestrated by Brain and Cook that led to Robbins’ suspension and firing by the employee benefit plan as well as the termination of Cook by his employer, Zenith..
With respect to Robbins’ suspension, the court found that the evidence showed Brain and Cook “were very upset with Robbins due to her contact with the [Department of Labor],” and that Brain and Cook “used their positions and influence to cause the other trustees to vote in favor of” suspending Robbins. To do so, the court explained, Brain and Cook “took the lead at the . . . [b]oard meeting with respect to the discussion of Robbins’ contact with the [Department of Labor]” and “created an environment that was hostile to her,” which “caused the trustees to vote to place her on leave.” The court noted that the two “‘set in motion’ the decision by the Joint Board to put Robbins on leave [.]”
As for Rice’s firing, the court explained how Brain and Cook retaliated against Rice by pressuring his employer, Zenith, into firing Rice and manipulating the Zenith relationship to deter Zenith from rehiring Rice in retaliation for his involvement in efforts to make an internal complaint about Brain.
Based upon evidence introduced during a five-day trial, the District Court ruled that Brain, Cook and Cook’s law firm violated ERISA section 510 by suspending and then discharging Robbins, and causing Zenith to refuse to hire Robbins and to discharge Rice in retaliation for their participation in reporting Brian’s misconduct to the General President of the Operative Plasterers’ and Cement Masons’ International Association and because Robbins participated in a federal criminal investigation of Brain. Specifically, the District Court ruled:
- Brain, Cook and Cook’s law firm wrongfully retaliated against Robbins in violation of ERISA 510 for her communications with the DOL by placing her on administrative leave; causing the work performed by the department that Robbins previously managed to be outsourced to Zenith and by causing Zenith not to hire Robbins to participate in its work;
- Brain, Cook and Cook’s law firm wrongfully retaliated against Rice in violation of ERISA 510 by causing Zenith to terminate Cook;
- Brain breached his fiduciary duty under ERISA 404 by retaliating against Robbins and causing her to be placed on administrative leave and that Cook knowingly participated in that breach.
The court held that Brain and Cook’s retaliatory conduct violated section 510 of ERISA, which prohibits retaliation against whistleblowers for complaining of ERISA violations or cooperating with a governmental investigation of such violations. The court also held that the couple’s retaliation against Robbins breached Brain’s fiduciary duties under ERISA section 404 to the trust funds and that Cook participated knowingly in that breach.
In reaching its decision, the court rejected attorney Cook’s argument that she was somehow immunized from her unlawful conduct because she was an attorney to the trust funds. Among other things, the court noted the “apparent conflict of interest” Cook had in representing the trust funds while being in an undisclosed “romantic relationship” with Brain, which existed as defendants carried out their retaliatory scheme. Reminding lawyers of their ethical duties in California, the court cited California Rule of Professional Conduct 3-310(B), which the court explained “requires that an attorney disclose to a client any personal relationship or interest that he or she knows, or with the exercise of reasonable diligence should know, could substantially affect her his or her professional judgment in advising the client.”
As punishing for these criminal violations of ERISA, the District Court ordered the permanent removal of Brain as a trustee. It also ordered the permanent barring of Brain, Cook and her law firm from serving the Cement Masons Southern California Trust Funds. In addition, the court ordered Cook and her law firm to repay all attorneys’ fees she billed the trust funds for the actions she took in retaliating against whistleblowers Robbins and Rice. These criminal sanctions were in addition to the $630,000 civil damage award that the Labor Department previously secured in lost wages and damages for Robbins, Rice and another worker victimized by Brain and Cook in August 2015.
In addition to its successful prosecution of Brain, Cook and Cook’s law firm on these charges, the DOL also had sought, but failed to convince the District Court based on the evidence presented at trial to find Brain, Cook, Cook’s law firm and Brain’s fellow trust fund trustee Local 600 business agent and Joint Board of Trustees member Jaime Briceno guilty of wrongful retaliation against another alleged whistleblower or Briceno of breaching his fiduciary duties under ERISA by failing to prudently investigate Robbins’ allegations against Brain; or by voting to use assets of the Trust Funds to pay the cost of the settlement of the civil action brought by Robbins. The District Court also refused to consider a newly raised charge that Brain breached his fiduciary duty by failing to collect all monies owed to the Trust Funds on the grounds that the Labor Department had failed to timely raise the charge. While the court refused to convict Briceno, Brain, Cook or Cook’s law firm on the additional charges, the Labor Department’s prosecution of these claims illustrates that along with abstaining from retaliating against ERISA whistleblowers, employee benefit plan fiduciaries also should position themselves to defend against potential breach of fiduciary duty claims based on alleged inadequacies in their investigation or response to reports or other evidence of misconduct involving the plan by prudently investigating and acting to redress allegations or other evidence of potential wrongdoing in the administration of employee benefit plans or their assets.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, the author of this update, attorney Cynthia Marcotte Stamer, is AV-Preeminent (the highest) rated attorney repeatedly recognized as a Martindale-Hubble as a “LEGAL LEADER™” and “Texas Top Rated Lawyer” in Health Care Law, Labor and Employment Law, and Business & Commercial Law and among the “Best Lawyers In Dallas” in ERISA, Labor and Employment and Healthcare Law by D Magazine for her nearly 30 years of experience and knowledge representing and advising employers, employee benefit plans, their sponsors, fiduciaries, service providers and vendors and others on these and other planning, business transaction and contracting, administration, compliance, risk management, audits, investigations, government and private litigation and other enforcement and other related matters.
past Chair and current committee Co-Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, former Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, a former ABA Joint Committee on Employee Benefits Council Representative ,
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping management manage. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, she de[;pus jer her extensive legal and operational knowledge and experience to help organizations and their management use the law and process to manage people, process, compliance, operations and risk.
As a key part of this work, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well known for her extensive work with health care, insurance and other highly regulated entities on corporate compliance, internal controls and risk management, her clients range from highly regulated entities like employers, contractors and their employee benefit plans, their sponsors, management, administrators, insurers, fiduciaries and advisors, technology and data service providers, health care, managed care and insurance, financial services, government contractors and government entities, as well as retail, manufacturing, construction, consulting and a host of other domestic and international businesses of all types and sizes. Common engagements include internal and external workforce hiring, management, training, performance management, compliance and administration, discipline and termination, and other aspects of workforce management including employment and outsourced services contracting and enforcement, sentencing guidelines and other compliance plan, policy and program development, administration, and defense, performance management, wage and hour and other compensation and benefits, reengineering and other change management, internal controls, compliance and risk management, communications and training, worker classification, tax and payroll, investigations, crisis preparedness and response, government relations, safety, government contracting and audits, litigation and other enforcement, and other concerns.
Ms. Stamer uses her deep and highly specialized health, insurance, labor and employment and other knowledge and experience to help employers and other employee benefit plan sponsors; health, pension and other employee benefit plans, their fiduciaries, administrators and service providers, insurers, and others design legally compliant, effective compensation, health and other welfare benefit and insurance, severance, pension and deferred compensation, private exchanges, cafeteria plan and other employee benefit, fringe benefit, salary and hourly compensation, bonus and other incentive compensation and related programs, products and arrangements. She is particularly recognized for her leading edge work, thought leadership and knowledgeable advice and representation on the design, documentation, administration, regulation and defense of a diverse range of self-insured and insured health and welfare benefit plans including private exchange and other health benefit choices, health care reimbursement and other “defined contribution” limited benefit, 24-hour and other occupational and non-occupational injury and accident, expat and medical tourism, onsite medical, wellness and other medical plans and insurance benefit programs as well as a diverse range of other qualified and nonqualified retirement and deferred compensation, severance and other employee benefits and compensation, insurance and savings plans, programs, products, services and activities. As a key element of this work, Ms. Stamer works closely with employer and other plan sponsors, insurance and financial services companies, plan fiduciaries, administrators, and vendors and others to design, administer and defend effective legally defensible employee benefits and compensation practices, programs, products and technology. She also continuously helps employers, insurers, administrative and other service providers, their officers, directors and others to manage fiduciary and other risks of sponsorship or involvement with these and other benefit and compensation arrangements and to defend and mitigate liability and other risks from benefit and liability claims including fiduciary, benefit and other claims, audits, and litigation brought by the Labor Department, IRS, HHS, participants and beneficiaries, service providers, and others. She also assists debtors, creditors, bankruptcy trustees and others assess, manage and resolve labor and employment, employee benefits and insurance, payroll and other compensation related concerns arising from reductions in force or other terminations, mergers, acquisitions, bankruptcies and other business transactions including extensive experience with multiple, high-profile large scale bankruptcies resulting in ERISA, tax, corporate and securities and other litigation or enforcement actions.
A former lead consultant to the Government of Bolivia on its Social Security reform law Ms. Stamer also is well-known for her leadership on U.S. health and pension, wage and hour, tax, workforce, tax, education, insurance and other policies critical to the workforce, benefits, and compensation practices and other key aspects of a broad range of businesses and their operations. She both helps her clients respond to and resolve emerging regulations and laws, government investigations and enforcement actions and helps them shape the rules through dealings with Congress and other legislatures, regulators and government officials domestically and internationally. Ms. Stamer works with U.S. and foreign businesses, governments, trade associations, and others on workforce, social security and severance, health care, immigration, privacy and data security, tax, ethics and other laws and regulations. Founder and Executive Director of the Coalition for Responsible Healthcare Policy and its PROJECT COPE: the Coalition on Patient Empowerment and a Fellow in the American Bar Foundation and State Bar of Texas, Ms. Stamer for many years acted as the scribe responsible for leading the Joint Committee on Employee Benefits (JCEB) HHS Office of Civil Rights annual agency meeting and regularly participates in the OCR and other JCEB annual agency meetings, and participates in the development and submission of comments and other input to the agencies on regulatory, enforcement and other concerns. She also works as a policy advisor and advocate to many business, professional and civic organizations.
Author of the thousands of publications and workshops these and other employment, employee benefits, health care, insurance, workforce and other management matters, Ms. Stamer also is a highly sought out speaker and industry thought leader known for empowering audiences and readers. Ms. Stamer’s insights on employee benefits, insurance, health care and workforce matters in Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, Modern Healthcare, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications. Ms. Stamer also regularly serves on the faculty and planning committees for symposia of LexisNexis, the American Bar Association, ALIABA, the Society of Employee Benefits Administrators, the American Law Institute, ISSA, HIMMs, and many other prominent educational and training organizations and conducts training and speaks on these and other management, compliance and public policy concerns.
Ms. Stamer also is active in the leadership of a broad range of other professional and civic organizations. For instance, Ms. Stamer serves on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and as an editorial advisor and contributing author of many other publications. Her leadership involvements with the American Bar Association (ABA) include year’s serving many years as a Joint Committee on Employee Benefits Council representative; ABA RPTE Section current Practice Management Vice Chair and Substantive Groups & Committees Committee Member, RPTE Employee Benefits & Other Compensation Committee Past Group Chair and Diversity Award Recipient, current Defined Contribution Plans Committee Co-Chair, and past Welfare Benefit Plans Committee Chair Co-Chair; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; current Vice Chair of the ABA TIPS Employee Benefit Committee; International Section Life Sciences Committee Policy Vice Chair; and a speaker, contributing author, comment chair and contributor to numerous Labor, Tax, RPTE, Health Law, TIPS, International and other Section publications, programs and task forces. Other selected service involvements of note include Vice President of the North Texas Healthcare Compliance Professionals Association; past EO Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division; founding Board Member and President of the Alliance for Healthcare Excellence, as a Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; the Board President of the early childhood development intervention agency, The Richardson Development Center for Children; Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former Southwest Benefits Association Board of Directors member, Continuing Education Chair and Treasurer; former Texas Association of Business BACPAC Committee Member, Executive Committee member, Regional Chair and Dallas Chapter Chair; former Society of Human Resources Region 4 Chair and Consultants Forum Board Member and Dallas HR Public Policy Committee Chair; former National Board Member and Dallas Chapter President of Web Network of Benefit Professionals; former Dallas Business League President and others. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
If you found these updates of interest, you may be interested in other recent Solutions Law Press, Inc. updates like the following:
Go here to register to receive other Solutions Law Press, Inc. updates and announcements about other upcoming briefings, training or other programs, products, services, and activities or to learn more about Solutions Law Press, Inc., its publications, programs and training, PROJECT COPE: Coalition on Patient Empowerment community service and education projects, event management and other resources and services.
For important information concerning this communication see here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2016 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Criminal Conviction Of Plan Trustee, Outside Legal Counsel Shows Risks of Retaliating Against Whistleblowers For Reporting ERISA Violations |
Comments Off on Criminal Conviction Of Plan Trustee, Outside Legal Counsel Shows Risks of Retaliating Against Whistleblowers For Reporting ERISA Violations |  401(k), Appeals, Attorney-Client Privilege, Banking, Bankruptcy, board of directors, Brokers, Claims Administration, compensation, compliance, Corporate Compliance, corporate governance, Cybercrime, defined benefit plan, defined contribution plan, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Malpractice, Reporting & Disclosure, Uncategorized | Tagged: defined contribution plan, EBSA, employee benefit plans, Employer, ERISA, ERISA 404, ERISA 510, Fiduciary responsiility, Health Plan, Health Plans, Multiemployer collectively bargained employee benefit plans, Retailiation, Retirement Plans, Union, Whistleblower |
401(k), Appeals, Attorney-Client Privilege, Banking, Bankruptcy, board of directors, Brokers, Claims Administration, compensation, compliance, Corporate Compliance, corporate governance, Cybercrime, defined benefit plan, defined contribution plan, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Malpractice, Reporting & Disclosure, Uncategorized | Tagged: defined contribution plan, EBSA, employee benefit plans, Employer, ERISA, ERISA 404, ERISA 510, Fiduciary responsiility, Health Plan, Health Plans, Multiemployer collectively bargained employee benefit plans, Retailiation, Retirement Plans, Union, Whistleblower |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 10, 2014
Human resources and other management leaders are watching Washington to see if the change in Congressional control resulting from the November 4, 2014 mid-term election ushers in a more management friendly federal legal environment. Since President Obama took office, the Democrats aggressive pursuit of health care, minimum wage and other federal pro-labor legislation, regulations and enforcement has increased management responsibilities, costs and liabilities.
Nationally recognized management attorney, public policy advisor and advocate, author and lecturer Cynthia Marcotte Stamer will help human resources and other management leaders prepare for 2015 when she speaks on “2015 Federal Legislative, Regulatory & Enforcement Update: What HR & Benefit Leaders Should Expect & Do Now” at the 2015 Dallas HR monthly luncheon series kickoff meeting on January 13, 2014.
About The Program
While November 4, 2014 Republican election victories gave Republicans a narrow majority in both the House and Senate when the new Congress takes office January 3, 2015, the new Republican Majority may face significant challenges delivering on their promises to move quickly to enact more business-friendly health care, guest worker, tax and other key reforms Republicans say will boost the employment and the economy.
While President Obama and Democrat Congressional leaders say they plan to work with the new majority, President Obama already is threatening to use vetoes, regulations and executive orders to block Republicans from obstructing or rolling back his pro-labor policy and enforcement agenda. When the new Congress takes office, the narrowness of the Republican Majority in the Senate means Republicans can’t block a Democratic filibuster or override a Presidential veto without recruiting some Democratic support.
As the Democrats and Republicans head into battle again, Board Certified Labor & Employment attorney and public policy advocate Cynthia Marcotte Stamer will help human resources and other management leaders get oriented for the year ahead by sharing her insights and predictions on the legislative, regulatory and enforcement agendas that HR, benefit and other business leaders need to plan for and watch in 2015. Among other things, Ms. Stamer will:
- Discuss how management can benefit from monitoring and working to influence potential legislative, regulatory and enforcement developments when planning and administering HR and related workforce policies;
- Discuss the key workforce and other legislative, regulatory and enforcement priorities and proposals Democrats and Republicans plan to pursue during 2015;
- Share her insights and predictions about how the narrow Republican majority, Mr. Obama’s lame duck presidency and other factors could impact each Party’s ability to pursue its agenda
- Share tips management leaders can use to help monitor developments and to help shape legislation, regulation and enforcement through Dallas HR, SHRM and other organizations as well as individually;
- Learn tips for anticipating and maintaining flexibility to respond to legislative, regulatory and enforcement developments; and
- More
To register or get more details about the program, DallasHR, or both, see http://www.dallashr.org.
About Ms. Stamer
Board certified labor and employment attorney, public policy leader, author, speaker Cynthia Marcotte Stamer is nationally and internationally recognized and valued for her more than 25 years of work advising and representing employers, insurers, employee benefit plans, their fiduciaries and advisors, business and community leaders and governments about workforce, employee benefits, social security and pension, health and insurance, immigration and other performance and risk management, public policy and related regulatory and public policy, management and other operational concerns.
Throughout her career, Ms. Stamer continuously both has helped businesses and their management to monitor and respond to federal and state legislative, regulatory and enforcement concerns and to anticipate and shape federal, state and other laws, regulations, and enforcement in the United States and internationally.
Well known for her leadership on workforce, health and pension policy through her extensive work with clients as well as through her high profile involvements as the Founder and Executive Director of the Coalition for Responsible Healthcare Policy and its PROJECT COPE: the Coalition on Patient Empowerment, a founding Board member of the Alliance for Health Care Excellence, a Fellow in the American College of Employee Benefit Counsel, the American Bar Association (ABA), and the State Bar of Texas leadership and other involvements with the ABA including her annual service leading the annual agency meeting of Joint Committee on Employee Benefits (JCEB) representatives with the HHS Office of Civil Rights and participation in other JCEB agency meetings, past involvements with legislative affairs for the Texas Association of Business and Dallas HR and others, and many speeches, publications, and other educational outreach efforts, Ms. Stamer has worked closely with Congress and federal and state regulators on the Patient Protection & Affordable Care Act and other health care, pension, immigration, tax and other workforce-related legislative and regulatory reforms for more than 30 years. One of the primary drafters of the Bolivian Social Security reform law and a highly involved leader on U.S. workforce, benefits, immigration and health care policy reform, Ms. Stamer’s experience also includes working with U.S. and foreign government, trade association, private business and other organizations to help reform other countries’ and U.S. workforce, social security and severance, health care, immigration, privacy and data security, tax, ethics and other laws and regulations. Ms. Stamer also contributes her policy, regulatory and other leadership to many professional and civic organizations including as Vice President of the North Texas Healthcare Compliance Professionals Association; Immediate Past Chair of the American Bar Association RPTE Employee Benefits & Other Compensation Committee and its current Welfare Benefit Plans Committee Co-Chair, a Substantive Groups & Committee Member; a member of the leadership council of the ABA Joint Committee on Employee Benefits; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; the current Vice Chair of the ABA TIPS Employee Benefit Committee, and the past Coordinator of the Gulf Coast TEGE Council TE Division.
The publisher and editor of Solutions Law Press, Inc. who serves on the Editorial Advisory Boards of Employee Benefit News, HR.com, InsuranceThoughtLeadership.com and many other publications, Ms. Stamer also is a prolific and highly respected author and speaker, National Public Radio, CBS, NBC, and other national and regional news organization, Atlantic Information Services, The Bureau of National Affairs, HealthLeaders, Telemundo, Modern Healthcare, Business Insurance, Employee Benefit News, the Employee Benefits News, World At Work, Benefits Magazine, InsuranceThoughtLeadership.com, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, CEO Magazine, CFO Magazine, CIO Magazine, the Houston Business Journal, and many other prominent news and publications. She also serves as a planning faculty member and regularly conducts training and speaks on these and other management, compliance and public policy concerns for these and a diverse range of other organizations. For additional information about Ms. Stamer, see www.cynthiastamer.com.
For Added Information and Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For Help Or More Information
If you need assistance in auditing or assessing, updating or defending your organization’s compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 24 years of work helping employers and other management; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend union-management relations, wage and hour, discrimination and other labor and employment laws, privacy and data security, internal investigation and discipline and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on management, reengineering, investigations, human resources and workforce, employee benefits, compensation, internal controls and risk management, federal sentencing guideline and other enforcement resolution actions, and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters.Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see hereor contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2014 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Stamer Kicks Off Dallas HR 2015 Monthly Lunch Series With 2015 Federal Legislative, Regulatory & Enforcement Update |
Comments Off on Stamer Kicks Off Dallas HR 2015 Monthly Lunch Series With 2015 Federal Legislative, Regulatory & Enforcement Update |  105(h), ACA, ADA, Affirmative Action, Affordable Care Act, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Civil Rights, Claims Administration, COBRA, compensation transparency, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, ESOP, Excise Tax, Executive Compensation, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Mental Health, Mental Health Parity, MEWA, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Premium Subsidies, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Tax, Tax Credit, Telecommuting, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs | Tagged: Administrative Simplification, CMS, Health Benefits, Health Insurance, Health insurers, Health Plans, HHS, HPID, HPOES, out-of-pocket maximum, TPAs |
105(h), ACA, ADA, Affirmative Action, Affordable Care Act, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Civil Rights, Claims Administration, COBRA, compensation transparency, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, ESOP, Excise Tax, Executive Compensation, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Mental Health, Mental Health Parity, MEWA, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Premium Subsidies, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Tax, Tax Credit, Telecommuting, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs | Tagged: Administrative Simplification, CMS, Health Benefits, Health Insurance, Health insurers, Health Plans, HHS, HPID, HPOES, out-of-pocket maximum, TPAs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 21, 2013
If you have employees that had too much or too little tax taken out of their paychecks, refer them to this new YouTube video about using the IRS withholding calculator at inbox:body:0000000001510000020000000800000000000000:Read#Third.
For Help With These Or Other Matters
If you need assistance in conducting a risk assessment of or responding to an IRS, Labor Department or other legal challenges to your organization’s labor and employment, employee benefit or compensation practices, please contact the author of this update, attorney Cynthia Marcotte Stamer.
Ms. Stamer has more than 24 years experience advising and representing employer, employee benefit and other clients before the Internal Revenue Service, the Department of Labor, Immigrations & Customs, and other agencies, private plaintiffs and others on worker classification and related human resources, employee benefit, internal controls and risk management matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experience worker classification and other employment, employee benefits and workforce matters, Ms. Stamer works extensively with employers, employee benefit plan sponsors, insurers, administrators, and fiduciaries, payroll and staffing companies, technology and other service providers and others to develop and operate legally defensible programs, practices and policies that promote the client’s human resources, employee benefits or other management goals.
A featured presenter in the recent “Worker Classification & Alternative Workforce: Employee Plans & Employment Tax Challenges” teleconference sponsored by the American Bar Association Joint Committee on Employee Benefits, Ms. Stamer also is a widely published author and highly regarded speaker on these and other employee benefit and human resources matters who is active in many other employee benefits, human resources and other management focused organizations.
A Fellow in the American College of Employee Benefits Council, the immediate past Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, the Vice Chair of the ABA TIPS Employee Benefits Committee, the Gulf States Area TEGE Council Exempt Organizations Coordinator, past-Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, and the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications.
You can learn more about Ms. Stamer and her experience, find out about upcoming training or other events, review some of her past training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer at www.CynthiaStamer.com.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at www.solutionslawpress.com.
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2011 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on IRS Witholding Calculator Can Help Avoid Over & Underwithholding |
Comments Off on IRS Witholding Calculator Can Help Avoid Over & Underwithholding |  105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |
105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 10, 2013
The Obama Administration again is proposing that the Board of the Pension Benefit Guaranty Corporation (PBGC) get the power to set premium rates based on the financial soundness of company sponsors to shore up the agency’s finances in hopes of heading off the need for a government bailout of the agency’s liabilities.
PBGC, which insures traditional pensions offered by non-governmental employers continues to struggle for funding to meet the costs of funding its program of insuring failed private defined benefit pension plans. Always challenging, maintaining financial solvency has become particularly problematic with company failures soaring and investment returns down in the ailing economy. On November 16, 2012, the agency said its deficit increased to $34 billion, the largest in PBGC’s 38-year history.
The PBGC currently relies exclusively on premiums set by Congress and assets recovered from failed plans to operate and fund its private pension guarantee obligations. It presently doesn’t receive taxpayer dollars. Premiums, set by Congress, have historically been too low to meet the agency’s needs.
The Government Accountability Office issued a report saying Congress should consider “revising PBGC’s premium structure to better reflect the agency’s risk from individual plans and sponsors
The proposal to give the PBGC authority to determine premiums is intended to shore up the agency’s funding. “Without premium increases PBGC will be faced with requesting a taxpayer bailout or shutting down,” said PBGC Director Josh Gotbaum. “The current system punishes responsible companies by making them pay for the mistakes of others and punishes plans by raising rates just when companies can least afford it. Tha’s why administrations of both parties, and recently GAO, have supported giving PBGC what the FDIC has long had — the ability to set its own rates and to set them in ways that are fair.”
The Administration originally introduced the idea of allowing the PBGC to set its own premiums in 2012. It now has reintroduced the effort that ties premiums to company risk in its 2014 budget. Under the current proposal, the PBGC Board, which consists of secretaries of Labor, Commerce, and Treasury, with the secretary of Labor as chair, wouldn’t get the authority to set rates until 2015. The budget requires the board to perform a one-year study with a public comment period. Additionally, premium increases would be gradually phased in to give company sponsors time to prepare for the new rates.
For Help With These Or Other Matters
If you need help dealing with pension or other employee benefit funding, design or administration challenges, dealing with the PBGC, IRS, Labor Department or other agency or legal challenge to your organization’s existing employee benefit or other practices, or other workforce re-engineering, labor and employment, employee benefit or compensation practices, please contact the author of this update, attorney Cynthia Marcotte Stamer.
Ms. Stamer has more than 26 years experience advising and representing employer, employee benefit and other clients on human resources, employee benefit, internal controls and risk management matters including extensive work on workforce re-engineering and other human resources and employee benefits challenges of distressed and other companies, and related matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experience worker classification and other employment, employee benefits and workforce matters, Ms. Stamer works extensively with employers, employee benefit plan sponsors, insurers, administrators, and fiduciaries, payroll and staffing companies, technology and other service providers and others to develop and operate legally defensible programs, practices and policies that promote the client’s human resources, employee benefits or other management goals. Ms. Stamer also is a widely published author and highly regarded speaker on these and other employee benefit and human resources matters who is active in many other employee benefits, human resources and other management focused organizations.
A Fellow in the American College of Employee Benefits Council, the immediate past Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, the Vice Chair of the ABA TIPS Employee Benefits Committee, the Gulf States Area TEGE Council Exempt Organizations Coordinator, past-Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, and the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications.
You can learn more about Ms. Stamer and her experience, find out about upcoming training or other events, review some of her past training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer at www.CynthiaStamer.com.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at www.solutionslawpress.com.
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2011 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Administration Proposes To Let PBGC Board Set Premiums In Effort To Shore Up Finances |
Comments Off on Administration Proposes To Let PBGC Board Set Premiums In Effort To Shore Up Finances |  105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: Bankruptcy, contract labor, defined benefit, Determination Letters, distressed, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, PBGC, Pension, Pension Funding, plan qualification, Reengineering, Retirement Plans, staffing, Tax, Worker Classification |
105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: Bankruptcy, contract labor, defined benefit, Determination Letters, distressed, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, PBGC, Pension, Pension Funding, plan qualification, Reengineering, Retirement Plans, staffing, Tax, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 10, 2013
Businesses using non-employee workers should heed the recently announced expansion of the Internal Revenue Service (IRS) Voluntary Classification VCS Program (VCS Program) as yet another warning to clean up their worker classification practices and defenses for all workers performing services for the business in any non-employee capacity.
Relying upon misclassifications of workers as nonemployed service providers presents many financial, legal and operational risks for businesses. When businesses treat workers as nonemployees who render services in such a way that makes the worker likely to qualify as a common law employee, the business runs the risk of overlooking or underestimating the costs and liabilities of employing those workers. The enforcement records of the U.S. Department of Labor Wage & Hour Division contains a lengthy and ever-lengthening record of businesses subjected to expensive backpay and penalty awards because the business failed to pay minimum wage or overtime to workers determined to qualify as common law employees entitled to minimum wage and overtime under the Fair Labor Standards Act. See, e.g., Employers Should Tighten Worker Classification Practices As Obama Administration Moves To Stamp Out Misclassification Abuses; $1 Million + FLSA Overtime Settlement Shows Employers Should Tighten On-Call, Other Wage & Hour Practices; Employer Charged With Misclassifying & Underpaying Workers To Pay $754,578 FLSA Back Pay Settlement.
Originally announced on September 22, 2011 in Announcement 2011-64, the VCS Program as modified by Announcement 2012-45 continues to offer businesses a carrot to reclassify as employees workers misclassified for payroll tax purposes as independent contractors, leased employees or other non-employee workers backed by the enforcement stick of the IRS’ promise to zealously impose penalties and interest against employers caught wrongfully misclassifying workers. While the IRS’s VCS Program and stepped up audits of worker classification provide a strong incentive for business to address their worker classification risks, the IRS is only one of many agencies on the alert for worker misclassification exposures. Worker misclassification also impacts wage and hour, safety, immigration, worker’s compensation, employee benefits, negligence and a host of other obligations.
All of these exposures carry potentially costly compensation, interest, and civil and in some cases even criminal penalty exposures for the businesses and their leaders. Consequently, businesses should act prudently and promptly to identify and address all of these risks and move forward holistically to manage their misclassification exposures.
Agencies charged with enforcement of these other laws as well as private plaintiffs also are on the alert for and pursing businesses for aggressive misclassification of workers in these other exposure areas. Since most businesses uniformly classify workers as either employees or non-employees for most purposes, business leaders must understand and manage the full scope of their businesses’ misclassification exposures when charting and implementing their strategy in response to the VCS Program or another voluntary compliance program, responding to an audit or other agency action, addressing a private plaintiff suit or conducting other risk management and compliance activities impacting or affected by worker classification concerns.
VCS Program Offers Limited Worker Misclassification Exposure Relief
Worker misclassification impacts a broad range of tax and non-tax legal obligations and risks well beyond income tax withholding, payroll and other employment tax liability and reporting and disclosure. A worker classification challenge or necessity determination in one area inherently prompts the need to address the worker reclassification and attendant risks in other areas.
Typically, in addition to treating a worker as a non-employee for tax purposes, a business also will treat the worker as a non-employee for immigration law eligibility to work, wage and hour, employment discrimination, employee benefits, fringe benefits, worker’s compensation, workplace safety, tort liability and insurance and other purposes.
Health Care Reform To Increase Worker Classification Risks
Businesses can look forward to these risks rising in 2014, when the “pay or play” employer shared responsibility, health plan non-discrimination, default enrollment and other new rules take effect under the Patient Protection & Affordable Care Act (ACA). Given these new ACA requirements and the government’s need to get as many workers covered as employees to make them work, as well as existing laws, IRS and other agencies are expanding staffing and stepping up enforcement against businesses that misclassify workers.
Whether and how ACA’s “pay-or-play” employer shared responsibility payment, default enrollment, insured health plan non-discrimination and other federal health plan rules apply to a business’ health plan requires a correct understanding of what workers considered employed by the business and how these workers are counted and classified for purposes of ACA and other federal health plan mandates.
ACA and other federal health plan rules decide what rules apply to which businesses or health plans based on the number of employees a business is considered to employ, their hours worked, their seasonal or other status, and other relevant classification as determined by the applicable rule. The ACA and other rules vary in the relevant number of employees that trigger applicability of the rule and how businesses must count workers to decide when a particular rule applies. Consequently, trying to predict the employer shared responsibility payment, if any under Internal Revenue Code (Code) Section 4980H or model the burden or cost of any other federal health benefit mandates requires each business know who counts and how to classify workers for each of these rules. Most of these rules start with a “common law” definition of employee then apply rules to add or ignore various workers. Because most federal health plan rules also take into account “commonly controlled” and “affiliated” businesses’ employees when determining rule coverage, businesses also may need to know that information for other related or commonly owned businesses.
For instance, when a business along with all commonly controlled or affiliated employers, if any, employ a combined workforce of 50 or more “full-time” and “full-time equivalent employees” (Large Employer) does not offer “affordable,” “minimum essential coverage” to every full-time employee and his dependents under a legally compliant health plan that provides “minimum essential value” within the meaning of ACA after 2013, the business generally should expect to pay a shared responsibility payment under Code Section 4980H for each month after 2013 that any “full-time” employee receives a tax subsidy or credit for enrolling in one of ACA’s health care exchanges. The amount of this required shared responsibility payment will be calculated under Code Section 4980H based on the plan design and coverage the employer health plan offers and the required employee contribution for employee only coverage.
If the business intends to continue to offer health coverage, it similarly will need to accurately understand which workers count as its employees for purposes of determining who gets coverage and the consequences to the business for those workers that qualify as full-time, common law employees not offered coverage.
In either case, ACA uses the common law employee test as the basis for classification of workers both to determine what businesses have sufficient full-time employees to become covered under these rules, the payment, if any, required under Code Section 4980H’s new employer shared responsibility payment requirements, as well as the workers entitled to benefit from these rules under employer sponsored health plans. Accordingly, These the already significant legal and financial consequences for employers that misclassify workers will rise significantly when ACA gets fully implemented beginning in 2014.
Consider VCP Program Relief In Context Of Other Worker Classification Risks
As part of a broader effort to get businesses properly to classify and fulfill tax and other responsibilities to workers, the IRS is offering certain qualifying businesses an opportunity to resolve payroll liabilities arising from past worker misclassifications under the VCS Program. The VCS Program settlement opportunity emerged in 2011 as worker misclassification amid rising scrutiny and enforcement by the IRS and other agencies against businesses for misclassification related violations of the Code, wage and hour, safety, discrimination, immigration and various other laws.
Touted by the IRS as providing “greater certainty for employers, workers and the government,” the VCS Program offers businesses that meet the eligibility criteria for the program the option to resolve past payroll tax liability for the misclassified workers by paying a settlement payment of just over one percent of the wages paid to the reclassified workers for the past year and by meeting other program criteria. When a business meets the VCS Program requirements, the IRS promises not to conduct a payroll tax audit or assess interest or penalties against the business for unpaid payroll taxes for the previously misclassified workers covered by the VCS Program. For more detail, see New IRS Voluntary IRS Settlement Program Offers New Option For Resolving Payroll Tax Risks Of Misclassification But Employers Also Must Manage Other Legal Risks; Medical Resident Stipend Ruling Shows Health Care, Other Employers Should Review Payroll Practices; Employment Tax Takes Center Stage as IRS Begins National Research Project , Executive Compensation Audits.
The IRS hoped the threat of much larger liability if the IRS catches their misclassification in an audit would induce businesses to settle their exposure and come into compliance by participating in the VCS Program.
Part of the low participation stemmed from restrictions incorporated into the VCS Program. Not all businesses with misclassified workers qualified to use the program. The original criteria to enter the VCS Program established in 2011 required that a business:
- Be treating the workers as nonemployees;
- Consistently have treated the workers in the past as nonemployees;
- To have filed all required Forms 1099 for amounts paid to the workers;
- Not currently be under IRS audit;
- Not be under audit by the Department of Labor or a state agency on the classification of these workers or contesting the classification of the workers in court; and
- To agree to extend the statute of limitations on their payroll tax liabilities from three to six years.
After only about 1000 employers used the VCS Program to voluntarily resolve their payroll tax liability for misclassified workers, the IRS modified the program in hopes of making participation more attractive to businesses in Announcement 2012-45. As modified by Announcement 2012-45, employers under IRS audit, other than an employment tax audit, now qualify for the VCS Program. Announcement 2012-45 also eliminates the requirement that employers agree to extend their statute of limitations on payroll tax liability from three to six years.
A business that meets these adjusted criteria for participation now follows the following steps to enter the VCS Program:
- Files the Form 8952, Application for Voluntary Classification Settlement Program, at least 60 days before the business plans to begin treating the workers as employees;
- Adjusts its worker classification practices prospectively with respect to the previously misclassified workers;
- Pays the required settlement fee; and
- Properly classifies workers going forward.
While these changes may make participation in the VCS Program more attractive to some employers, many employers may view use of the VCS Program as too risky because of uncertainties about the proper classification of certain workers in light of the highly fact specific nature of the determination, as well as concerns about the effect that use of the VCS Program might have on the businesses non-tax misclassification exposures for workers that would be reclassified under the VCS Program.
Uncertainties Complication Worker Classification Risk Management
One of the biggest challenges to getting businesses to change their worker classifications is getting the businesses to accept the notion that long-standing worker classification practices in fact might not be defensible.
Although existing precedent and regulatory guidance makes clear that certain long-standing worker classification practices of many businesses would not hold up if scrutinized, business leaders understandably often discount the risk because these classifications historically have continued with little or no challenge in the past.
Even when business leaders recognize that changing enforcement patterns merit reconsideration of historical worker classification practices, they may be reluctant to reclassify the workers.
The common law employment test applied to decide if a worker is an employee for payroll, income tax, employee benefit plan and other purposes under the Code often relies on a subjective, highly fact-specific analysis of the particular circumstances of the worker. Employment status typically is presumed under the common law test for purposes of the Code and most other laws. This means that the business, rather than the IRS or other agency, generally bears the burden of proving the correctness of its classification of a worker as a non-employee for purposes of these determinations.
Given the business typically bears the burden of proving a worker is not an employee, a business receiving services from workers performing services in a capacity other than as a employee should ensure that the position in structural form and operation will withstand scrutiny under the common law and other applicable tests and retain the necessary evidence to support this characterization in anticipation of a potential future audit or other challenge.
Since the business can expect to bear the burden of proving the appropriateness of a nonemployee characterization, businesses also should exercise special care to avoid relying upon overly optimistic assessment of the facts and circumstances when assessing the defensibility of their characterization of the position.
When the factual evidence creates significant questions about the defensibility of a worker’s classification as a non-employee, an employing business generally should consider reclassifying or restructuring the position to be more defensible pursuant to a process designed to mitigate or resolve risks of the prior classification. Often, it also may be desirable for the business to incorporate certain contractual, compensation and other safeguards into the worker relationship, both to support the nonemployee characterization and to minimize future reclassification challenges and exposures.
Consider Importance of Attorney-Client Privilege As Risk Management Tool
Because of the broad reaching and potentially significant liability exposures arising from misclassification, business leaders generally should work to ensure that their risk analysis and decision-making discussion is conducted in a way that positions these discussions for protection under attorney-client privilege and attorney work product privilege.
The availability of the attorney-client and other evidentiary privilege to help shield the investigation and associated decision-making is particularly important because of the potentially significant civil and even criminal liability exposures that often arise from worker misclassification under various relevant laws.
The interwoven nature of the tax and non-tax risks merits particular awareness by business leaders of the need to use care in deciding the outside advisors and consultants that will help in the evaluation of the risks and structuring of solutions. With the VCS Program and other tax exposures in the limelight, businesses can expect that their accounting and other consultant advisors will recommend and even offer to lead the review. While appropriately structured involvement by these non-legal consultants can be a valuable tool, the blended nature of the misclassification exposures means that the evidentiary privileges that accountants often assert to help shield their tax related discussions from discovery in certain federal tax prosecutions are likely to provide inadequate protection against discovery given the broad non-tax related exposures inherent in the misclassification problem. For this reason, business leaders are urged to require that any audits and other activities by these non-legal consultants to evaluate or mitigate these exposures be engaged and conducted whenever possible within attorney-client privilege to protect and promote the ability to assert evidentiary protections against disclosure and discovery of sensitive discussions. Accordingly, while businesses definitely should incorporate appropriate tax advisors into the evaluation process, most businesses before commencing meaningful discussions with or engaging assessments by their accounting firm or other non-attorney tax advisor will want to engage counsel and coordinate their accounting and other non-attorney tax advisors” involvement and activities through qualified legal counsel to protect and maximize the ability to conduct the analysis of their risks and options within the protection of attorney-client privilege.
For Help With These Or Other Matters
If you need assistance in conducting a risk assessment of or responding to an IRS, Labor, HHS, DOJ, ICE, private claim or other legal challenges to your organization’s existing workforce classification or other labor and employment, employee benefit, compensation practices, compliance, or other internal controls and management concerns, please contact the author of this update, attorney Cynthia Marcotte Stamer.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experience worker classification and other employment, employee benefits and workforce matters, Ms. Stamer has more than 25 years experience advising and representing employer, employee benefit and other clients before the Internal Revenue Service, the Department of Labor, Immigration & Customs, Justice, and Health & Human Services, the Securities and Exchange Commission, Federal Trade Commission, state labor, insurance, tax and attorneys’ general, and other agencies, private plaintiffs and others on worker classification and related human resources, employee benefit, tax, internal controls, risk management and other legal and operational management concerns.
Ms. Stamer works extensively with employers, employee benefit plan sponsors, insurers, administrators, and fiduciaries, payroll and staffing companies, technology and other service providers and others to develop and run legally defensible programs, practices and policies that promote the client’s human resources, employee benefits or other management goals.
A Fellow in the American College of Employee Benefits Council, the immediate past Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, the Vice Chair of the ABA TIPS Employee Benefits Committee, the Gulf States Area TEGE Council Exempt Organizations Coordinator, past-Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, and the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, Ms. Stamer also is a widely published author and highly regarded speaker on these and other employee benefit and human resources matters who is active in many other employee benefits, human resources and other management focused organizations who is published and speaks extensively on worker classification and related matters. She is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications.
You can learn more about Ms. Stamer and her experience, find out about upcoming training or other events, review some of her past training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer at www.CynthiaStamer.com.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at www.solutionslawpress.com including:
- Alert Employees Claiming Qualified Adoption Expenses and Education Credits About Changed IRS Procedures
- 13 Employer Tips For Coping With Health Care Reform Now!
- Sequester Will Cut ACA Small Businesses Health Care Tax Credits
- Premier Insurance Services Pays $120,000 In Back Wages, Damages, Penalties Because Commission-Only Comp Violated Minimum Wage, Overtime Laws
- OSHA Citation Of Michigan VA Reminder To Manage Workplace Safety
- Labor Department Targeting Businesses Violating Overtime, Other Wage & Hour Laws
- Wal-Mart Settlement Shows ADA Risks When Considering Employee Return To Work Accommodation Requests & Inquiries
- HHS Releases Final Rule on Health Insurance Market, Rate Review, Pre-Existing Conditions & Other ACA Market Reform Rules
- FTC, HIPAA Rules Require Health Plans & Employers Strengthen Data Security on Mobile Devices and Applications
- 3/13 JCEB Teleconference Explores Foreign Transferees: Outbound, Inbound, Equity And Treaty Issues
- Stamer Talks on “What the Wind Blew In: Coping with Health Care Reform: 2013 and Beyond” May 2 At 24th Annual RPTE Spring Symposia In Washington, D.C.
- IRS Will Begin Accepting Returns Claiming Education Credits By Mid-February
- IRS Shares Procedures Employers Use To Claim Increased Monthly Transit Benefit Exclusion Allowed By Administrative Taxpayer Relief Act
- Employers ACA Health Reforms Prohibit Using HRAs To Pay Individual Medical Policy Premiums & Impact Other HRA Arrangements
For important information about this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2013 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 1 Comment |
1 Comment |  105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |
105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 1, 2012
President Obama’s declaration today (October 1, 2012) of October as National Disability Employment Awareness Month reminds business that U.S. businesses and their leaders need to tighten their disability discrimination risk management and compliance in light of the Obama Administration’s emphasis on aggressively interpreting and enforcing disability discrimination laws, rising private plaintiff lawsuits and other recent regulatory and judicial changes.
In his proclaimation today, President Obama reaffirmed his often stated commitment to the aggressive enforcement of disability laws and other efforts to promote opportunities for disabled individuals, stating:
“[My Administration remains committed to helping our businesses, schools, and communities support our entire workforce. To meet this challenge,… we are striving to make it easier to get and keep those jobs by improving compliance with Section 508 of the Rehabilitation Act.
As the administration marks the month, U.S. employers and other business leaders can expect the Obama Administration will be stepping up its already aggressive outreach to disabled Americans to promote awareness of their disability law rights and tools for asserting and enforcing these rights.
Business Faces Growing Employment Disability Exposures
As part of his administration’s commitment, the Obama Administration has moved to aggressively enforce the disability and accommodations of teh Americans With Disabilities Act, Section 508 of the Rehabilitation Act, and other federal disability discrimination laws. The reach and effectiveness of these efforts has been enhanced by statutory and regulatory changes that require employers to exercise greater efforts to meet their compliance obligations and manage their disability and other discrimination risks.
ADA Exposures Heightened
The ADA, for instance, generally prohibits disability discrimination and requires employers to make reasonable accommodations to employees’ and applicants’ disabilities as long as this does not pose an undue hardship. Violations of the ADA can expose businesses to substantial liability. Violations of the ADA may be prosecuted by the EEOC or by private lawsuits. Employees or applicants that can prove they were subjected to prohibited disability discrimination under the ADA generally can recover actual damages, attorneys’ fees, and up to $300,000 of exemplary damages (depending on the size of the employer).
In recent years, amendments to the original provisions of the ADA have made it easier for plaintiffs and the EEOC to establish disabled status of an individual. Businesses should exercise caution to carefully document legitimate business justification for their hiring, promotion and other employment related decisions about these and other individuals who might qualify as disabled. Provisions of the ADA Amendments Act (ADAAA) that expand the definition of “disability” under the ADA, As signed into law on September 25, 2008, the ADAAA amended the definition of “disability” for purposes of the disability discrimination prohibitions of the ADA to make it easier for an individual seeking protection under the ADA to establish that that has a disability within the meaning of the ADA. The ADAAA retains the ADA’s basic definition of “disability” as an impairment that substantially limits one or more major life activities, a record of such an impairment, or being regarded as having such an impairment. However, provisions of the ADAAA that took effect January 1, 2009 change the way that these statutory terms should be interpreted in several ways. Most significantly, the Act:
- Directs EEOC to revise that portion of its regulations defining the term “substantially limits;”
- Expands the definition of “major life activities” by including two non-exhaustive lists: (1) The first list includes many activities that the EEOC has recognized (e.g., walking) as well as activities that EEOC has not specifically recognized (e.g., reading, bending, and communicating); and (2) The second list includes major bodily functions (e.g., “functions of the immune system, normal cell growth, digestive, bowel, bladder, neurological, brain, respiratory, circulatory, endocrine, and reproductive functions”);
- States that mitigating measures other than “ordinary eyeglasses or contact lenses” shall not be considered in assessing whether an individual has a disability;
- Clarifies that an impairment that is episodic or in remission is a disability if it would substantially limit a major life activity when active;
- Changes the definition of “regarded as” so that it no longer requires a showing that the employer perceived the individual to be substantially limited in a major life activity, and instead says that an applicant or employee is “regarded as” disabled if he or she is subject to an action prohibited by the ADA (e.g., failure to hire or termination) based on an impairment that is not transitory and minor; and
- Provides that individuals covered only under the “regarded as” prong are not entitled to reasonable accommodation.
The ADAAA also emphasizes that the definition of disability should be construed in favor of broad coverage of individuals to the maximum extent permitted by the terms of the ADA and generally shall not require extensive analysis.In adopting these changes, Congress expressly sought to overrule existing employer-friendly judicial precedent construing the current provisions of the ADA and to require the EEOC to update its existing guidance to confirm with the ADAAA Amendments. Under the leadership of the Obama Administration, the EEOC and other federal agencies have embraced this charge and have sigificantly stepped up enforcement of the ADA and other federal discrimination laws.
Recent enforcement, regulatory and other activities by the EEOC demonstrate that the EEOC is enthusiastically moving forward to exercise its regulatory and enforcement powers under these enhanced ADA provisions to tighten requirements for employers and to enforce its rules. See e.g., Leprino Foods To Pay $550K To Settle OFCCP Charge Pre-Hire Screening Test Illegally Discriminated « As EEOC Steps Up ADA Accommodation Enforcement, New DOD Apple App, Other Resources Released; Wal-Mart Settlement Shows ADA Risks When Considering Employee Return To Work Accommodation Requests & Inquiries; Employer Pays $475,000 To Settle ADA Discrimination Lawsuit Challenging Medical Fitness Testing For EMTs, Firefighters & Other Public Safety Worker’s.
Rehabilitation Act Risks For Government Contractors
Beyond the generally applicable risks applicable to all employers of more than 15 employees under the ADA, federal and state government contractors face additional responsibilities and risks.
Subject to limited exceptions, government contractors providing services or supplies on ARRA or other government funded contracts or projects must comply both with generally applicable employment discrimination requirements and special statutory and contractual nondiscrimination, affirmative action, and recordkeeping requirements applicable government contractors. For instance, federal law generally requires government contractors to comply with the special equal employment opportunity requirements of Executive Order 11246 (EO 11246); Section 503 of the Rehabilitation Act of 1973 (Section 503); and the Vietnam Veterans’ Readjustment Assistance Act of 1974 (VEVRAA). Pursuant to these laws, business with the federal government, both contractors and subcontractors, generally must follow a number of statutory and contractual requirements to follow the fair and reasonable standard that they not discriminate in employment on the basis of sex, race, color, religion, national origin, disability or status as a protected veteran. OFCCP generally audits and enforces these requirements. Memo to Funding Recipients: Compliance with Applicable Nondiscrimination and Equal Opportunity Statutes, Regulations, and Executive Orders.
OFCCP has made clear that it will conduct compliance evaluations and host compliance assistance events to ensure that federal contractors comply and are aware of their responsibilities under EO 11246, Section 503 and VEVRAA.
While many government contractors may be tempted to become complacent about OFCCP exposures based on reports of the OFCCP’s relatively low enforcement in the past, see Report Says OFCCP Enforcement Data Show Infrequent Veteran, Disability Bias Findings | Bloomberg BNA recent enforcement data documents OFCCP is getting much more serious and aggressive about auditing and enforcing compliance with its affirmative action and other requirements against government contractors under the Obama Administration. See, OFCCP Enforcement Data is Available on a New DOL Website. See also, Affirmative Action Update: OFCCP Enforcement Statistics Show Increase in Violations. The readiness of OFCCP to enforce its rules is illustrated by the settlement of an OFCCP action filed against federal contractor Nash Finch Co. (Nash Finch) announceed last week. Under the settlement, Nash Finch to pay $188,500 in back wages and interest and offer jobs to certain women applicants who OFCCP charged Nash rejected for the entry-level position of order selector at the company’s distribution facility in Lumberton, Minnesota. See Settlement of OFCCP Employment Discrimination Charge Reminder To ARRA, Other Government Contractors Of Heightened Enforcement Risks.
These government contractor disability discrimination risks are particularly acute where the government contractor works on or provides supplies on contacts or projects funded in whole or in part by monies provided under the American Recovery and Reinvestment Act of 2009 (“ARRA”). When the contract or project in question receives any funding out of the $787 billion of stimulus funding provided by ARRA, special OFCCP rules applicable to ARRA funded projects necessitates that federal contractors exercise special care to understand and meet their responsibilities and manage associated exposures. See, e.g. Settlement of OFCCP Employment Discrimination Charge Reminder To ARRA, Other Government Contractors Of Heightened Enforcement Risks.
Businesses Should Act To Manage Risks
The ADAAA amendments, the Rehabilitation Act’s expanded reach, and the Obama Administration’s emphasis on enforcement make it likely that businesses generally will face more disability claims from a broader range of employees and will possess fewer legal shields to defend themselves against these claims. These changes will make it easier for certain employees to qualify and claim protection as disabled under the ADA, the Rehabilitation Act, and other disability discrimination laws.
In light of these and other developments and risks, businesses generally should act cautiously when dealing with applicants or employees with actual, perceived, or claimed physical or mental impairments to minimize exposures under the ADA, the Rehabilitation Act and other laws. Management should exercise caution to carefully and appropriate the potential legal significance of physical or mental impairments or conditions that might be less significant in severity or scope, correctable through the use of eyeglasses, hearing aids, daily medications or other adaptive devices, or that otherwise have been assumed by management to fall outside the ADA’s scope.
Likewise, businesses should be prepared for the EEOC, OFCCP and the courts to treat a broader range of disabilities, including those much more limited in severity and life activity restriction, to qualify as disabling for purposes of the Act. Businesses should assume that a greater number of employees with such conditions are likely to seek to use the ADA as a basis for challenging hiring, promotion and other employment decisions. For this reason, businesses generally should tighten job performance and other employment recordkeeping to enhance their ability to demonstrate nondiscriminatory business justifications for the employment decisions made by the businesses.
Businesses also should consider tightening their documentation regarding their procedures and processes governing the collection and handling records and communications that may contain information regarding an applicant’s physical or mental impairment, such as medical absences, worker’s compensation claims, emergency information, or other records containing health status or condition related information. The ADA generally requires that these records be maintained in separate confidential files and disclosed only to individuals with a need to know under circumstances allowed by the ADA.
As part of this process, businesses also should carefully review their employment records, group health plan, family leave, disability accommodation, and other existing policies and practices to comply with, and manage exposure under the new genetic information nondiscrimination and privacy rules enacted as part of the Genetic Information and Nondiscrimination Act (GINA) signed into law by President Bush on May 21, 2008. Effective November 21, 2009, Title VII of GINA amends the Civil Rights Act to prohibit employment discrimination based on genetic information and restricts the ability of employers and their health plans to require, collect or retain certain genetic information. Under GINA, employers, employment agencies, labor organizations and joint labor-management committees face significant liability for violating the sweeping nondiscrimination and confidentiality requirements of GINA concerning their use, maintenance and disclosure of genetic information. Employees can sue for damages and other relief like currently available under Title VII of the Civil Rights Act of 1964 and other nondiscrimination laws. For instance, GINA’s employment related provisions include rules that will:
- Prohibit employers and employment agencies from discriminating based on genetic information in hiring, termination or referral decisions or in other decisions regarding compensation, terms, conditions or privileges of employment;
- Prohibit employers and employment agencies from limiting, segregating or classifying employees so as to deny employment opportunities to an employee based on genetic information;
- Bar labor organizations from excluding, expelling or otherwise discriminating against individuals based on genetic information;
- Prohibit employers, employment agencies and labor organizations from requesting, requiring or purchasing genetic information of an employee or an employee’s family member except as allowed by GINA to satisfy certification requirements of family and medical leave laws, to monitor the biological effects of toxic substances in the workplace or other conditions specifically allowed by GINA;
- Prohibit employers, labor organizations and joint labor-management committees from discriminating in any decisions related to admission or employment in training or retraining programs, including apprenticeships based on genetic information;
- Mandate that in the narrow situations where limited cases where genetic information is obtained by a covered entity, it maintain the information on separate forms in separate medical files, treat the information as a confidential medical record, and not disclosure the genetic information except in those situations specifically allowed by GINA;
- Prohibit any person from retaliating against an individual for opposing an act or practice made unlawful by GINA; and
- Regulate the collection, use, access and disclosure of genetic information by employer sponsored and certain other health plans.
These employment provisions of GINA are in addition to amendments to the Health Insurance Portability and Accountability Act of 1996 (HIPAA), the Employee Retirement Income Security Act of 1974 (ERISA), the Public Health Service Act, the Internal Revenue Code of 1986, and Title XVIII (Medicare) of the Social Security Act that are effective for group health plan for plan years beginning after May 20, 2009.
If you have any questions or need help reviewing and updating your organization’s employment and/or employee practices in response to the Rehabilitation Act, ADA, GINA or other applicable laws, or if we may be of assistance with regard to any other workforce management, employee benefits or compensation matters, please do not hesitate to contact the author of this update, Board Certified Labor and Employment Attorney and Management Consultant Cynthia Marcotte Stamer at 469..
About The Author
Management attorney and consultant Cynthia Marcotte Stamer helps businesses, governments and associations solve problems, develop and implement strategies to manage people, processes, and regulatory exposures to achieve their business and operational objectives and manage legal, operational and other risks. Board certified in labor and employment law by the Texas Board of Legal Specialization, with more than 25 years human resource, employee benefits and management experience, Ms. Stamer helps businesses manage their people-related risks and the performance of their internal and external workforce though appropriate human resources, employee benefit, worker’s compensation, insurance, outsourcing and risk management strategies domestically and internationally. Recognized in the International Who’s Who of Professionals and bearing the Martindale Hubble AV-Rating, Ms. Stamer also is a highly regarded author and speaker, who regularly conducts management and other training on a wide range of labor and employment, employee benefit, human resources, internal controls and other related risk management matters. Her writings frequently are published by the American Bar Association (ABA), Aspen Publishers, Bureau of National Affairs, the American Health Lawyers Association, SHRM, World At Work, Government Institutes, Inc., Atlantic Information Services, Employee Benefit News, and many others. For a listing of some of these publications and programs, see here. Her insights on human resources risk management matters also have been quoted in The Wall Street Journal, various publications of The Bureau of National Affairs and Aspen Publishing, the Dallas Morning News, Spencer Publications, Health Leaders, Business Insurance, the Dallas and Houston Business Journals and a host of other publications. Chair of the ABA RPTE Employee Benefit and Other Compensation Committee, a council member of the ABA Joint Committee on Employee Benefits, and the Legislative Chair of the Dallas Human Resources Management Association Government Affairs Committee, she also serves in leadership positions in numerous human resources, corporate compliance, and other professional and civic organizations. For more details about Ms. Stamer’s experience and other credentials, contact Ms. Stamer, information about workshops and other training, selected publications and other human resources related information, see here or contact Ms. Stamer via telephone at 214.270.2402 or via e-mail here.
Other Helpful Resources & Other Information
If you found these updates of interest, you also be interested in one or more of the following other recent articles published in this electronic Solutions Law publication available for review here including:
- $1.25M NLRB Backpay Order Highlights Risks of Mismanaging Union Risks In Health Care & Others M&A Deals
- As EEOC Steps Up ADA Accommodation Enforcement, New DOD Apple App, Other Resources Released
- $1.5 M HIPAA Security Breach Resolution Agreement Shows Looming HIPAA Risks
- ARRA, Other Government Contractors Face Growing Enforcement & Audit Risks
- Disability Exposures Big US Business Risk; New DOD App Helps ID Resources
- Personal Consumer Information Protection in Hospital/Healthcare Setting At HIMSS November 11
- Obama Administration Continues War On Management Despite NLRB’s Tempoary Setback In Suit Against Arizona Secret Ballot Law
- Companies, Officers, Directors, Fiduciaries & Vendors Urged To Confirm ERISA Credentials & Bonding For Internal Staff, Plan Fidiciaries, Vendors Dealing With Benefits
- Labor Risks Rising For Employers Despite NLRB Loss Of Arizona Secret Ballot Challenge
- USI Advisors Will Pay $1.27 Million To Settle Charges It Violated ERISA Fee Disclosure Requirements
- Wal-Mart Settlement Shows ADA Risks When Considering Employee Return To Work Accommodation Requests & Inquiries
- Stamer Speaks On HIPAA Developments On 9/14 At ABA Joint Tax/RPTE Fall Meeting In Boston
- Employer Pays $475,000 To Settle ADA Discrimination Lawsuit Challenging Medical Fitness Testing For EMTs, Firefighters & Other Public Safety Worker’s
- Employers & Plan Fiduciaries Reminded To Confirm Credentials & Bonding For Internal Staff, Plan Fidiciaries & Vendors Dealing With Benefits
- HIPAA & Texas Law Require HIPAA Training. Register Now For August 14 HIPAA Update Workshop!
- EBSA Updates Guidance On Fee Disclosure Requirements For 401(k) Plan Brokerage Window Arrangements
- Federal Mandate That Employer Health Plans Must Cover 100% Of Contraceptive, Other Women’s Health Services With No Cost Sharing Now Effective
- Use NIH & Other Free Government Resources To Help Round Out Wellness Programs
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here.
For important information concerning this communication click here. If you do not wish to receive these updates in the future, send an e-mail with the word “Remove” in the Subject to support@solutionslawyer.net.
©2012 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Tighten Employment Disability Risk Management As Obama Declares 12/10 National Disability Employment Awareness Month |
Comments Off on Tighten Employment Disability Risk Management As Obama Declares 12/10 National Disability Employment Awareness Month |  ADA, Affirmative Action, Corporate Compliance, Disability, Disability, Disability Plans, EEOC, EEOC, Employers, FMLA, GINA, Government Contractors, Human Resources, Labor Management Relations, OFCCP, Retaliation, USERRA, VEVRRA | Tagged: ADA, Corporate Compliance, Disability Discrimination, Employee Benefits, Employers, Employment, Health Insurance, Health Plans, Human Resources |
ADA, Affirmative Action, Corporate Compliance, Disability, Disability, Disability Plans, EEOC, EEOC, Employers, FMLA, GINA, Government Contractors, Human Resources, Labor Management Relations, OFCCP, Retaliation, USERRA, VEVRRA | Tagged: ADA, Corporate Compliance, Disability Discrimination, Employee Benefits, Employers, Employment, Health Insurance, Health Plans, Human Resources |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 1, 2012
President Obama’s declaration today (October 1, 2012) of October as National Disability Employment Awareness Month reminds business that U.S. businesses and their leaders need to tighten their disability discrimination risk management and compliance in light of the Obama Administration’s emphasis on aggressively interpreting and enforcing disability discrimination laws, rising private plaintiff lawsuits and other recent regulatory and judicial changes. With the Administration expected to step up further its already substantial educational outreach to the disabled and their advocates, U.S. employers should brace for this month’s celebration to fuel even more disability discrimination claims and other activity by the disabled and their activists.
Since taking office, President Obama has make enforcing and expanding the rights of the disabled in employment and other areas a leading priority.
In his proclamation today, President Obama reaffirmed his often stated commitment to the aggressive enforcement of disability laws and other efforts to promote opportunities for disabled individuals, stating:
“[My Administration remains committed to helping our businesses, schools, and communities support our entire workforce. To meet this challenge,… we are striving to make it easier to get and keep those jobs by improving compliance with Section 508 of the Rehabilitation Act.”
As the administration marks the month, U.S. employers and other business leaders can expect the Obama Administration will be stepping up its already aggressive outreach to disabled Americans to promote awareness of their disability law rights and tools for asserting and enforcing these rights. See, e.g. October Is National Disability Employment Awareness Month (NDEAM).
Business Faces Growing Employment Disability Exposures
As part of his administration’s commitment, the Obama Administration has moved to aggressively enforce the disability and accommodations of the Americans With Disabilities Act (ADA), Section 508 of the Rehabilitation Act, and other federal disability discrimination laws. The reach and effectiveness of these efforts has been enhanced by statutory and regulatory changes that require employers to exercise greater efforts to meet their compliance obligations and manage their disability and other discrimination risks.
ADA Exposures Heightened
The ADA, for instance, generally prohibits disability discrimination and requires employers to make reasonable accommodations to employees’ and applicants’ disabilities as long as this does not pose an undue hardship. Violations of the ADA can expose businesses to substantial liability. Violations of the ADA may be prosecuted by the EEOC or by private lawsuits. Employees or applicants that can prove they experienced prohibited disability discrimination under the ADA generally can recover actual damages, attorneys’ fees, and up to $300,000 of exemplary damages (depending on the size of the employer).
In recent years, amendments to the original provisions of the ADA have made it easier for plaintiffs and the EEOC to prove disabled status of an individual. Businesses should exercise caution to carefully document legitimate business justification for their hiring, promotion and other employment related decisions about these and other individuals who might qualify as disabled. Provisions of the ADA Amendments Act (ADAAA) that expand the definition of “disability” under the ADA, As signed into law on September 25, 2008, the ADAAA amended the definition of “disability” for purposes of the disability discrimination prohibitions of the ADA to make it easier for an individual seeking protection under the ADA to establish that that has a disability within the meaning of the ADA. The ADAAA retains the ADA’s basic definition of “disability” as an impairment that substantially limits one or more major life activities, a record of such an impairment, or being regarded as having such an impairment. However, provisions of the ADAAA that took effect January 1, 2009 change the way that these statutory terms should be interpreted in several ways. Most significantly, the Act:
- Directs EEOC to revise that part of its regulations defining the term “substantially limits;”
- Expands the definition of “major life activities” by including two non-exhaustive lists: (1) The first list includes many activities that the EEOC has recognized (e.g., walking) as well as activities that EEOC has not specifically recognized (e.g., reading, bending, and communicating); and (2) The second list includes major bodily functions (e.g., “functions of the immune system, normal cell growth, digestive, bowel, bladder, neurological, brain, respiratory, circulatory, endocrine, and reproductive functions”);
- States that mitigating measures other than “ordinary eyeglasses or contact lenses” shall not be considered in assessing whether an individual has a disability;
- Clarifies that an impairment that is episodic or in remission is a disability if it would substantially limit a major life activity when active;
- Changes the definition of “regarded as” so that it no longer requires a showing that the employer perceived the individual to be substantially limited in a major life activity, and instead says that an applicant or employee is “regarded as” disabled if he or she is subject to an action prohibited by the ADA (e.g., failure to hire or termination) based on an impairment that is not transitory and minor; and
- Provides that individuals covered only under the “regarded as” prong are not entitled to reasonable accommodation.
The ADAAA also emphasizes that the definition of disability should be construed in favor of broad coverage of individuals to the maximum extent permitted by the terms of the ADA and generally shall not require extensive analysis.In adopting these changes, Congress expressly sought to overrule existing employer-friendly judicial precedent construing the current provisions of the ADA and to require the EEOC to update its existing guidance to confirm with the ADAAA Amendments. Under the leadership of the Obama Administration, the EEOC and other federal agencies have embraced this charge and have significantly stepped up enforcement of the ADA and other federal discrimination laws.
Recent enforcement, regulatory and other activities by the EEOC show that the EEOC is enthusiastically moving forward to exercise its regulatory and enforcement powers under these enhanced ADA provisions to tighten requirements for employers and to enforce its rules. See e.g., Leprino Foods To Pay $550K To Settle OFCCP Charge Pre-Hire Screening Test Illegally Discriminated « As EEOC Steps Up ADA Accommodation Enforcement, New DOD Apple App, Other Resources Released; Wal-Mart Settlement Shows ADA Risks When Considering Employee Return To Work Accommodation Requests & Inquiries; Employer Pays $475,000 To Settle ADA Discrimination Lawsuit Challenging Medical Fitness Testing For EMTs, Firefighters & Other Public Safety Worker’s.
Rising Rehabilitation Act Risks For Government Contractors
Beyond the generally applicable risks applicable to all employers of more than 15 employees under the ADA, federal and state government contractors face more responsibilities and risks.
Subject to limited exceptions, government contractors providing services or supplies on ARRA or other government-funded contracts or projects must comply both with generally applicable employment discrimination requirements and special statutory and contractual nondiscrimination, affirmative action, and recordkeeping requirements applicable government contractors. For instance, federal law generally requires government contractors to comply with the special equal employment opportunity requirements of Executive Order 11246 (EO 11246); Section 503 of the Rehabilitation Act of 1973 (Section 503); and the Vietnam Veterans’ Readjustment Assistance Act of 1974 (VEVRAA). Pursuant to these laws, business with the federal government, both contractors and subcontractors, generally must follow a number of statutory and contractual requirements to follow the fair and reasonable standard that they not discriminate in employment on the basis of sex, race, color, religion, national origin, disability or status as a protected veteran. OFCCP generally audits and enforces these requirements. Memo to Funding Recipients: Compliance with Applicable Nondiscrimination and Equal Opportunity Statutes, Regulations, and Executive Orders.
OFCCP has made clear that it will conduct compliance evaluations and host compliance assistance events to ensure that federal contractors comply and are aware of their responsibilities under EO 11246, Section 503 and VEVRAA.
While many government contractors may be tempted to become complacent about OFCCP exposures based on reports of the OFCCP’s relatively low enforcement in the past, see Report Says OFCCP Enforcement Data Show Infrequent Veteran, Disability Bias Findings | Bloomberg BNA recent enforcement data documents OFCCP is getting much more serious and aggressive about auditing and enforcing compliance with its affirmative action and other requirements against government contractors under the Obama Administration. See, OFCCP Enforcement Data is Available on a New DOL Website. See also, Affirmative Action Update: OFCCP Enforcement Statistics Show Increase in Violations. The readiness of OFCCP to enforce its rules is illustrated by the settlement of an OFCCP action filed against federal contractor Nash Finch Co. (Nash Finch) announceed last week. Under the settlement, Nash Finch to pay $188,500 in back wages and interest and offer jobs to certain women applicants who OFCCP charged Nash rejected for the entry-level position of order selector at the company’s distribution facility in Lumberton, Minnesota. See Settlement of OFCCP Employment Discrimination Charge Reminder To ARRA, Other Government Contractors Of Heightened Enforcement Risks.
These government contractor disability discrimination risks are particularly acute where the government contractor works on or provides supplies on contacts or projects funded in whole or in part by monies provided under ARRA. When the contract or project in question receives any funding out of the $787 billion of stimulus funding provided by ARRA, special OFCCP rules applicable to ARRA funded projects necessitates that federal contractors exercise special care to understand and meet their responsibilities and manage associated exposures. See, e.g. Settlement of OFCCP Employment Discrimination Charge Reminder To ARRA, Other Government Contractors Of Heightened Enforcement Risks.
GINA & Other Medical Information Nondiscrimination & Privacy Risks
Employers also need to use care to ensure that their hiring and other employment practices, as well as their employee benefits, workers’ compensation and wellness practices are up to date and properly managed to mitigate exposures under laws like the Genetic Information and Nondiscrimination Act (GINA), the ADA’s medical information privacy requirements, as well as the privacy and nondiscrimination rules of the Health Insurance Portability & Accountability Act and other relevant federal and state laws.
Signed into law by President Bush on May 21, 2008 and in effect since November 21, 2009, for instance, Title VII of GINA amended the Civil Rights Act to prohibit employment discrimination based on genetic information and to restrict the ability of employers and their health plans to require, collect or retain certain genetic information. Under GINA, employers, employment agencies, labor organizations and joint labor-management committees face significant liability for violating the sweeping nondiscrimination and confidentiality requirements of GINA concerning their use, maintenance and disclosure of genetic information. Employees can sue for damages and other relief like now available under Title VII of the Civil Rights Act of 1964 and other nondiscrimination laws. For instance, GINA’s employment related provisions include rules that:
- Prohibit employers and employment agencies from discriminating based on genetic information in hiring, termination or referral decisions or in other decisions regarding compensation, terms, conditions or privileges of employment;
- Prohibit employers and employment agencies from limiting, segregating or classifying employees so as to deny employment opportunities to an employee based on genetic information;
- Bar labor organizations from excluding, expelling or otherwise discriminating against individuals based on genetic information;
- Prohibit employers, employment agencies and labor organizations from requesting, requiring or purchasing genetic information of an employee or an employee’s family member except as allowed by GINA to satisfy certification requirements of family and medical leave laws, to monitor the biological effects of toxic substances in the workplace or other conditions specifically allowed by GINA;
- Prohibit employers, labor organizations and joint labor-management committees from discriminating in any decisions related to admission or employment in training or retraining programs, including apprenticeships based on genetic information;
- Mandate that in the narrow situations where limited cases where genetic information is obtained by a covered entity, it maintain the information on separate forms in separate medical files, treat the information as a confidential medical record, and not disclosure the genetic information except in those situations specifically allowed by GINA;
- Prohibit any person from retaliating against an individual for opposing an act or practice made unlawful by GINA; and
- Regulate the collection, use, access and disclosure of genetic information by employer sponsored and certain other health plans.
These employment provisions of GINA are in addition to amendments to HIPAA, the Employee Retirement Income Security Act of 1974 (ERISA), the Public Health Service Act, the Internal Revenue Code of 1986, and Title XVIII (Medicare) of the Social Security Act that are effective for group health plan for plan years beginning after May 20, 2009. Under these HIPAA and GINA rules, health plans generally may not make certain medical inquiries or discriminate against employees or their family members based on family or individual medical history or genetic information. In addition, health plans and others are required to safeguard personal medical information and may only share that information only under very limited circumstances requiring specific documentation be in place and that the parties can prove that the access and use of that information is appropriately restricted. Violation of these and other rules can have significant civil and in some cases even criminal liabilities for companies, plans, plan fiduciaries and company officials that take part in violations of these rules.
Businesses Should Act To Manage Risks
The ADAAA amendments, the Rehabilitation Act’s expanded reach, and the Obama Administration’s emphasis on enforcement make it likely that businesses generally will face more disability claims from a broader range of employees and will have fewer legal shields to defend themselves against these claims. These changes will make it easier for certain employees to qualify and claim protection as disabled under the ADA, the Rehabilitation Act, and other disability discrimination laws.
All U.S. businesses should review and tighten the adequacy of their existing compliance and risk management practices to promote and document compliance. These efforts should focus on all relevant hiring, recruitment, promotion, compensation, recordkeeping and reporting policies and practices internally, as well as those of any recruiting agencies, subcontractors or other business partners whose actions might impact on compliance.
In light of these and other developments and risks, businesses generally should act cautiously when dealing with applicants or employees with actual, perceived, or claimed physical or mental impairments to minimize exposures under the ADA, the Rehabilitation Act and other laws. Management should exercise caution to carefully and appropriately assess and identify the potential legal significance of physical or mental impairments or conditions that might be less significant in severity or scope, correctable through the use of eyeglasses, hearing aids, daily medications or other adaptive devices, or that management might be tempted to assume fall outside the ADA’s scope.
Likewise, businesses should be ready for the EEOC, OFCCP and the courts to treat a broader range of disabilities, including those much more limited in severity and life activity restriction, to qualify as disabling for purposes of the Act. Businesses should assume that a greater number of employees with such conditions are likely to seek to use the ADA as a basis for challenging hiring, promotion and other employment decisions. For this reason, businesses generally should tighten job performance and other employment recordkeeping to enhance their ability to demonstrate nondiscriminatory business justifications for the employment decisions made by the businesses.
Businesses also should consider tightening their documentation regarding their procedures and processes governing the collection and handling records and communications that may contain information regarding an applicant’s physical or mental impairment, such as medical absences, worker’s compensation claims, emergency information, or other records containing health status or condition related information. The ADA generally requires that these records be maintained in separate confidential files and disclosed only to individuals with a need to know under circumstances allowed by the ADA.
As part of this process, businesses also should carefully review their employment records, group health plan, family leave, disability accommodation, and other existing policies and practices to comply with, and manage exposure under the genetic information nondiscrimination and privacy rules enacted as part of GINA, the health care privacy rules of the HIPAA, and the medical record privacy rules of the ADA. Particular care should be used when planning wellness, health risk assessment, work-related injury, family or other medical leave or related programs, all of which raise particular risks and concerns.
In the face of the rising emphasis of OFCCP, the EEOC and other federal and state agencies on these audit and enforcement activities, government contractors should exercise additional compliance and risk management efforts beyond these generally recommended steps. Among other things, these steps should include the following:
- Government contractors and subcontractors should specifically review their existing or proposed contracts and involvements to identify projects or contracts which may involve federal or state contracts or funding that could trigger responsibility. In this respect, businesses should conduct well-documented inquiries when proposing and accepting contracts to ensure that potential obligations as a government contractor are not overlooked because of inadequate intake procedures. Businesses also should keep in mind that ARRA and other federal program funds often may be filtered through a complex maze of federal grants or program funding to states or other organizations, which may pass along government contractor status and liability when subcontracting for services as part of the implementation of broader programs. Since the existence of these obligations often is signaled by contractual representations in the contracts with these parties, careful review of contractual or bid specifications and commitments is essential. However, it also generally is advisable also to inquire about whether the requested products or services are provided pursuant to programs or contracts subject to these requirements early in the process.
- In addition to working to identify contracts and arrangements that are covered by OFCCP or other requirements, government contractors and other businesses also should reconfirm and continuously monitor the specific reporting, affirmative action, and other requirements that apply to any programs that may be subject to OFCCP requirements to ensure that they fully understand and implement appropriate procedures to comply with these conditions as well as pass along the obligation to make similarly necessary arrangements to any subcontractors or suppliers that the government contractor involves as a subcontractor.
- Throughout the course of the contract, the government contractor also should take steps to maintain and file all required reports and monitor and audit operational compliance with these and other requirements.
- The organization should develop and administer appropriate procedures for monitoring and investigating potential compliance concerns and maintaining documentation of that activity. Any known potential deficiencies or complaints should be promptly investigated and redressed with the assistance of qualified counsel in a prompt manner to mitigate potential risks.
- Documentation should be carefully retained and organized on a real time and continuous basis to faciliate efficiency and effectiveness in completing required reports, monitoring compliance indicators and responding to OFCCP, EEOC or private plaintiff charges as well as other compliance inquiries.
- Any audit inquiries or charges should be promptly referred to qualified legal counsel for timely evaluation and response.
- When available and affordable, management should consider securing appropriate employment practices liability coverage, indemnification from business partners and other liability protection and assurance to help mitigate investigagtion and defense costs.
- Board members or other senior management should include periodic review of compliance in their agenda.
If you have any questions or need help reviewing and updating your organization’s employment and/or employee practices in response to the Rehabilitation Act, ADA, GINA or other applicable laws, or if we may be of help with regard to any other workforce management, employee benefits or compensation matters, please do not hesitate to contact the author of this update, Board Certified Labor and Employment Attorney and Management Consultant Cynthia Marcotte Stamer at 469.767.8872.
About The Author
Management attorney and consultant Cynthia Marcotte Stamer helps businesses, governments and associations solve problems, develop and implement strategies to manage people, processes, and regulatory exposures to meet their business and operational goals and manage legal, operational and other risks. Board certified in labor and employment law by the Texas Board of Legal Specialization, with more than 25 years human resource, employee benefits and management experience, Ms. Stamer helps businesses manage their people-related risks and the performance of their internal and external workforce though appropriate human resources, employee benefit, worker’s compensation, insurance, outsourcing and risk management strategies domestically and internationally. Recognized in the International Who’s Who of Professionals and bearing the Martindale Hubble AV-Rating, Ms. Stamer also is a highly regarded author and speaker, who regularly conducts management and other training on a wide range of labor and employment, employee benefit, human resources, internal controls and other related risk management matters. Her writings frequently are published by the American Bar Association (ABA), Aspen Publishers, Bureau of National Affairs, the American Health Lawyers Association, SHRM, World At Work, Government Institutes, Inc., Atlantic Information Services, Employee Benefit News, and many others. For a listing of some of these publications and programs, see here. Her insights on human resources risk management matters also have been quoted in The Wall Street Journal, various publications of The Bureau of National Affairs and Aspen Publishing, the Dallas Morning News, Spencer Publications, Health Leaders, Business Insurance, the Dallas and Houston Business Journals and a host of other publications. Chair of the ABA RPTE Employee Benefit and Other Compensation Committee, a council member of the ABA Joint Committee on Employee Benefits, and the Legislative Chair of the Dallas Human Resources Management Association Government Affairs Committee, she also serves in leadership positions in many human resources, corporate compliance, and other professional and civic organizations. For more details about Ms. Stamer’s experience and other credentials, contact Ms. Stamer, information about workshops and other training, selected publications and other human resources related information, see here or contact Ms. Stamer via telephone at 469.767.8872 or via e-mail here.
Other Helpful Resources & Other Information
If you found these updates of interest, you also be interested in one or more of the following other recent articles published in this electronic Solutions Law publication available for review here including:
- $1.25M NLRB Backpay Order Highlights Risks of Mismanaging Union Risks In Health Care & Others M&A Deals
- As EEOC Steps Up ADA Accommodation Enforcement, New DOD Apple App, Other Resources Released
- $1.5 M HIPAA Security Breach Resolution Agreement Shows Looming HIPAA Risks
- ARRA, Other Government Contractors Face Growing Enforcement & Audit Risks
- Disability Exposures Big US Business Risk; New DOD App Helps ID Resources
- Personal Consumer Information Protection in Hospital/Healthcare Setting At HIMSS November 11
- Obama Administration Continues War On Management Despite NLRB’s Tempoary Setback In Suit Against Arizona Secret Ballot Law
- Companies, Officers, Directors, Fiduciaries & Vendors Urged To Confirm ERISA Credentials & Bonding For Internal Staff, Plan Fidiciaries, Vendors Dealing With Benefits
- Labor Risks Rising For Employers Despite NLRB Loss Of Arizona Secret Ballot Challenge
- USI Advisors Will Pay $1.27 Million To Settle Charges It Violated ERISA Fee Disclosure Requirements
- Wal-Mart Settlement Shows ADA Risks When Considering Employee Return To Work Accommodation Requests & Inquiries
- Stamer Speaks On HIPAA Developments On 9/14 At ABA Joint Tax/RPTE Fall Meeting In Boston
- Employer Pays $475,000 To Settle ADA Discrimination Lawsuit Challenging Medical Fitness Testing For EMTs, Firefighters & Other Public Safety Worker’s
- Employers & Plan Fiduciaries Reminded To Confirm Credentials & Bonding For Internal Staff, Plan Fidiciaries & Vendors Dealing With Benefits
- HIPAA & Texas Law Require HIPAA Training. Register Now For August 14 HIPAA Update Workshop!
- EBSA Updates Guidance On Fee Disclosure Requirements For 401(k) Plan Brokerage Window Arrangements
- Federal Mandate That Employer Health Plans Must Cover 100% Of Contraceptive, Other Women’s Health Services With No Cost Sharing Now Effective
- Use NIH & Other Free Government Resources To Help Round Out Wellness Programs
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here.
For important information concerning this communication click here. If you do not wish to receive these updates in the future, send an e-mail with the word “Remove” in the Subject to support@solutionslawyer.net.
©2012 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Tighten Disability Discrimination Defenses As National Disability Employment Awareness Month Promises To Whip Up New Claims & Awareness |
Comments Off on Tighten Disability Discrimination Defenses As National Disability Employment Awareness Month Promises To Whip Up New Claims & Awareness |  ADA, Affirmative Action, Civil Rights, Corporate Compliance, Data Security, Disability Plans, Discrimination, EEOC, Employers, GINA, Government Contractors, VEVRRA | Tagged: ADA, Disability, Disability Discrimination, EEOC, Employer, GINA, Human Resources, Rehabilitation Act, Risk Management |
ADA, Affirmative Action, Civil Rights, Corporate Compliance, Data Security, Disability Plans, Discrimination, EEOC, Employers, GINA, Government Contractors, VEVRRA | Tagged: ADA, Disability, Disability Discrimination, EEOC, Employer, GINA, Human Resources, Rehabilitation Act, Risk Management |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 3, 2011
HR Key Player In Managing Rising Race & Other Discimination Suits Under Obama Administration Justice Department
The Obama Administration’s December 2 announcement of its revocation and replacement of Bush Administration policies on affirmative action in education highlights the heightened aggressiveness under the Obama Administration on the implementation, interpretation and enforcement of race, sex, disability, national origin and other federal discrimination and Civil Rights laws.
The new guidance discussed in more detail at http://wp.me/p1hsKH-1k makes clear the Administration’s view that schools can and should be doing more to promote integration and other affirmative action efforts in the schools and other organizations. It also gives a number of examples of the types of steps that the Administration believes schools should be pursuing. While specifically directed in schools, it provides insights about the affirmative action expectations of the Administration that merit notice by all public and private organizations and businesses.
The Justice Department under the Obama Administration in making discrimination in schools and other state and local agencies as well as by private businesses a priority. For instance, in addition to tightening and enforcing race discrimination laws, the Justice Department on November 23, 2011 sued the University of Nebraska at Kearney (UNK), the Board of Regents of the University of Nebraska and employees of UNK for violating the Fair Housing Act by discriminating against students with disabilities.
These and other activities are part of a growing number of regulatory and enforcement actions under the Obama Administation that illustrate the growing risk created for private and public organizations by failing to manage compliance with discrimination or other civil rights laws in the conduct of their business operations, as well as employment practices.
While most governmental agencies and businesses recognize the need to manage compliance with discrimination laws in their employment practices, many fail to adequately recognize and provide policies, management controls and training to maintain compliance with federal discrimination laws prohibiting discrimination in dealing with customers, vendors or other swith whom they do business.
Human resources and other management leaders should position their organizations to guard against rising enforcement of these laws by updating policies, oversight and training to ensure that their workers and business partners recognize and know how to conduct themselves properly to fulfill responsibilities with whom the business deals who may be protected under Federal or state race or other discrimination laws. In addition to adopting and training workers on policies requiring compliance with these laws, businesses should include contractual provisions requiring compliance with these laws in leases and other relevant business contracts. Most businesses also may want to provide and post information about processes that customers or others who may have a concern about potential prohibited discrimination to position the business to address concerns that otherwise might go unnoticed until they arise to the level of an agency or other legal complaint.
If you need assistance in conducting a risk assessment of or responding to a challenge to your organization’s existing policies or practices for dealing with the issues addressed in these publications or other compliance, labor and employment, employee benefit, compensation, internal controls or other management practices, contact attorney Cynthia Marcotte Stamer.
For Added Information and Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For Help Or More Information
If you need assistance in auditing or assessing, updating or defending your organization’s compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 24 years of work helping employers and other management; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend union-management relations, wage and hour, discrimination and other labor and employment laws, privacy and data security, internal investigation and discipline and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on management, reengineering, investigations, human resources and workforce, employee benefits, compensation, internal controls and risk management, federal sentencing guideline and other enforcement resolution actions, and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on New Obama Administration Affirmative Action Guidance Highlights Organization’s Need To Tighten Nondiscrimination Practices |
Comments Off on New Obama Administration Affirmative Action Guidance Highlights Organization’s Need To Tighten Nondiscrimination Practices |  Civil Rights, Disability, Disability, Disability Plans, Discrimination | Tagged: Accommodation, ADA, Consumer Rights, Disability Discrimination, Discrimination, Internal Controls, Justice Department, Real Estate |
Civil Rights, Disability, Disability, Disability Plans, Discrimination | Tagged: Accommodation, ADA, Consumer Rights, Disability Discrimination, Discrimination, Internal Controls, Justice Department, Real Estate |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 26, 2011
Latest Action Shows Obama Justice Department Aggressively Enforcing Discrimination Laws
The Justice Department on November 23, 2011 sued the University of Nebraska at Kearney (UNK), the Board of Regents of the University of Nebraska and employees of UNK for violating the Fair Housing Act by discriminating against students with disabilities. The latest in a growing string of disability and other discrimination suits brought by the Justice Department since the Obama Administration took office, it highlights the growing risk created for private and public organizations by failing to manage compliance with disability or other civil rights laws in the conduct of their business operations, as well as employment practices.
The lawsuit filed in the U.S. District Court for Nebraska, charges that UNK and its employees engaged in a pattern or practice of violating the Fair Housing Act or denied rights protected by the act by denying reasonable accommodation requests by students with psychological or emotional disabilities seeking to live with emotional assistance animals in university housing.
The Justice Department suit also charges that UNK requires students with psychological disabilities to disclose sensitive medical and other information that is unnecessary to evaluate their accommodation requests.
The latest in a growing series of disability discrimination lawsuits brought by the Justice Department against public and private landlords and a growing list of other businesses, the UNK lawsuit arises from a complaint filed with the Department of Housing and Urban Development (HUD) by a student enrolled at UNK who sought to live with an emotional assistance dog that had been prescribed. The lawsuit seeks a court order prohibiting future discrimination by the defendants, monetary damages for those harmed by the defendants’ actions, and a civil penalty.
The federal Fair Housing Act prohibits discrimination in housing on the basis of race, color, religion, sex, familial status, national origin and disability. With regard to disability discrimination, the Fair Housing Act requires housing providers to give reasonable accommodations for people with disabilities so that all have equal housing opportunities and limits the medical information that landlords can require from persons seeking disability accommodation in order to receive an accommodation.
The Obama Administration Justice Department has made enforcement of disability and other federal discrimination laws a key priority. Businesses should tighten policies, practices and training to minimize exposures to Justice Department or private plaintiff complaints for violations under these laws.
While most businesses recognize the need to manage compliance with the ADA and other discrimination laws in their employment practices, many businesses and business leaders fail to adequately recognize and provide policies, management controls and training to maintain compliance with federal disability and other discrimination laws prohibiting discrimination against disabled or other customers or others with whom they do business. Human resources and other management leaders should position their organizations to guard against rising enforcement of these laws by updating policies, oversight and training to ensure that their workers and business partners recognize and know how to conduct themselves properly to fulfill responsibilities to persons with disabilities or others with whom the business deals who may be protected under Federal or state disability discrimination laws. In addition to adopting and training workers on policies requiring compliance with these laws, businesses should include contractual provisions requiring compliance with these laws in leases and other relevant business contracts. Most businesses also may want to provide and post information about processes that customers or others who may have a concern about the needs of persons with these special needs to position the business to address concerns that otherwise might go unnoticed until they arise to the level of an agency or other legal complaint.
If you need assistance in conducting a risk assessment of or responding to a challenge to your organization’s existing policies or practices for dealing with the issues addressed in these publications or other compliance, labor and employment, employee benefit, compensation, internal controls or other management practices, contact attorney Cynthia Marcotte Stamer.
For Added Information and Other Resources
If you found this update of interest, you also may be interested in reviewing some of the other updates and publications authored by Ms. Stamer available including:
For Help Or More Information
If you need assistance in auditing or assessing, updating or defending your organization’s compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 24 years of work helping employers and other management; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend union-management relations, wage and hour, discrimination and other labor and employment laws, privacy and data security, internal investigation and discipline and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on management, reengineering, investigations, human resources and workforce, employee benefits, compensation, internal controls and risk management, federal sentencing guideline and other enforcement resolution actions, and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on HR Key Player In Managing Rising Risk of Disability, Other Discimination Suits Under Obama Administration Justice Department |
Comments Off on HR Key Player In Managing Rising Risk of Disability, Other Discimination Suits Under Obama Administration Justice Department |  Civil Rights, Disability, Disability, Disability Plans, Discrimination | Tagged: Accommodation, ADA, Consumer Rights, Disability Discrimination, Discrimination, Internal Controls, Justice Department, Real Estate |
Civil Rights, Disability, Disability, Disability Plans, Discrimination | Tagged: Accommodation, ADA, Consumer Rights, Disability Discrimination, Discrimination, Internal Controls, Justice Department, Real Estate |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
September 26, 2011
Program Another Sign of Growing Audit & Enforcement Risks. Businesses Urged To Strengthen Their Worker Classification Defenses
The September 22, 2011 launch by the Internal Revenue Service of a new Voluntary Worker Classification Settlement Program (“Settlement Program”) is the latest warning to businesses using independent contractors, leased employees or other non-employee workers of the need to review critically within the scope of attorney-client privilege the defensibility of their existing classification and treatment of those workers as non-employees in light of the in light of stepped up scrutiny and enforcement emphasis by the IRS and other federal and state regulators as well as workers and others in private litigation.
Coupled with growing scrutiny and challenges to businesses efforts to avoid employment-related liability and obligations through the use or workers that the business characterizes as non-employees by other federal and state agencies and plaintiff attorneys, the Settlement Agreement announcement is another sign that businesses using workers who are not employees need to be prepared to defend their worker classification and the legality of their dealings with these workers under applicable federal and state laws.
To guard against these and other growing risks of worker classification, employers receiving services from workers who are not considered employees for purposes of income or payroll should review within the scope of attorney-client privilege the defensibility of their existing worker classification, employee benefit, fringe benefit, employment, wage and hour, and other workforce policies and consult with qualified legal counsel about the advisability to adjust these practices to mitigate exposures to potential IRS, Labor Department or other penalties associated with worker misclassification.
Settlement Program Establishment Should Prompt Review Defensibility of Worker Classifications
The new Settlement Program established under Announcement 2011-64 reflects the widespread emphasis by the IRS and other federal and state regulators on uncovering and redressing misclassification of workers as non-employees by businesses for purposes of tax and other laws. IRS scrutiny of worker classification practices by businesses has risen significantly over the past decade.
The IRS’ launch of the Settlement Program follows its announcement in September, 2010 of plans to conduct approximately 6,000 payroll tax audits over a three year period focusing on the appropriateness of employer worker classification and other payroll tax practices. The announcement of the new Settlement Program signals that the IRS perceives that worker misclassification by business in violation of Federal tax laws is sufficiently widespread and pervasive to merit both efforts to incentive voluntary correction through participation in the Settlement Program, as well as stiff enforcement against businesses that fail to self-correct worker classification compliance concerns.
Designed to increase tax compliance and provide what the IRS says will be “greater certainty for employers, workers and the government,” the IRS says the Settlement Program offers eligible employers concerned about potential worker misclassification exposures that might arise from a payroll tax audit the opportunity to come into compliance by making the required filing, adjusting their practices and paying the required settlement fee effectively equaling just over one percent of the wages paid to the reclassified workers for the past year. If this settlement fee is paid and the other requirements of the Settlement Program are met, the Settlement Program specifies that employers accepted into the program will not be assessed interest or penalties and not be audited on payroll taxes related to these workers for prior years.
For businesses that can meet applicable requirements for participation, participation in the Settlement Program may offer an attractive option for resolving payroll related tax risks. However, not all employers will qualify for the Settlement Program. Employers must meet the eligibility requirements for participation.
Also, employers electing to use the Settlement Program need to understand the implications of that participation on the Statute of Limitations on their payroll tax liabilities. For the first three years of participation in the program, the Settlement Program specifies that participating employers will be subject to a special six-year statute of limitations, rather than the usual three years that generally applies to payroll taxes. Businesses will need to weigh the benefits of using the Settlement Program, if available, against the risk of reclassification and the availability of other resolution options that may be available under applicable Internal Revenue Code and IRS rules and procedures. Furthermore, many businesses evaluating worker classifications also may find it difficult to determine with certainty the risk of reclassification for certain categories of workers. Whether a worker is properly classified as an employee for most purposes under the Internal Revenue Code’s income tax withholding and reporting, payroll tax and most other employment tax turns on a highly fact specific analysis of under a common law employment test. When an analysis of the evidence reflects a high degree of certainty that the classification of a worker as a non-employee was not defensible under existing tax authorities, use of the Settlement Program or other tools to resolve liability definitely merits consideration. Because of the factual nature of the analysis, however, the decision whether to use the Settlement Program where the circumstances under which the worker renders services are less clear may be more difficult. When making these assessments, businesses should avoid the temptation of being overly optimistic in their assessment of the facts and circumstances given that the Internal Revenue Code generally assigns responsibility to the business to prove the appropriateness of its classification of a worker as a non-employee. While this allocation of the burden of proof means businesses should exercise caution when engaging workers in non-employee capacities, where the facts support this characterization, classification of a worker as a non-employee can be appropriate. When deciding to continue the non-employee characterization for purposes of the Internal Revenue Code, however, businesses are urged to document the evidentiary basis and evidence supporting that determination in anticipation of a potential future audit or other challenge.
Learn more about the Settlement Program and worker classification risk management here.
Businesses Should Address Other Worker Reclassification Risks When Conducting Settlement Program Risk Analysis
As welcome as the opportunity to resolve potential payroll tax exposures through participation in the Settlement Program, businesses considering using the Settlement Program also will need to understand and prepared to address various non-tax legal concerns. Because worker misclassification tends to impact on a broad range of legal obligations and risks, businesses evaluating or planning to use the Settlement Program are act quickly, but carefully, to evaluate and determine whether and how to use the Settlement Program and to identify and take appropriate steps to address both the tax-related liabilities targeted for resolution under the Settlement Program, as well as misclassification exposures likely to arise with respect to workers to be reclassified in connection with the use of the Settlement Program.
When conducting this evaluation and deciding whether to use the Settlement Program, businesses also need to keep the wider implications of the analysis and their decisions regarding how to handle a potential aggressive or misclassification as a worker as a non-employee. A determination of potential aggressive or misclassification for purposes of the Internal Revenue Code’s payroll tax rules generally will necessitate the need to evaluate potential exposures that may arise from the worker misclassification under other federal and state laws.
Typically, in addition to treating a worker as a non-employee for tax purposes, a business also will treat the worker as a non-employee for immigration law eligibility to work, wage and hour, employment discrimination, employee benefits, fringe benefits, worker’s compensation, workplace safety, tort liability and insurance and other purposes. Consequently, a determination that reclassification is advisable for tax purposes generally will prompt the need to consider how to address the worker reclassification and attendant risk for purposes of other legal risks and requirements, as well as those covered by the Settlement Program. Businesses will need to consider how the voluntary reclassification of workers and settlement under the Settlement Program may impact their exposures and obligations under other laws. As the Settlement Program does not provide relief from the exposures arising from misclassification under other laws, businesses should be prepared to evaluate the advisability of reclassification of the worker for purposes of these other laws, the potential exposures attendant to misclassification of workers under those laws, and risks, challenges and opportunities for mitigating these exposures.
Businesses Cautioned To Conduct Evaluations & Discussions In Attorney-Client Privilege Due To Complexity & Significance of Potential Exposures
Conducting and discussing the Settlement Program and other related concerns within the scope of attorney-client privilege is particularly important because of the potentially significant civil and even criminal liability exposures that may arise from misclassification of workers for purposes of the various relevant laws. Because of the broad reaching and potentially significant non-tax exposure inherent in these discussions, business leaders are cautioned that the evidentiary privileges that often provides protection against disclosure of certain discussions with accountants and certain other non-attorney tax advisors for purposes of certain tax laws may be inadequate in scope to protect discussions against discovery for purposes of these other laws. Accordingly, while businesses definitely should incorporate appropriate tax advisors into the evaluation process, most businesses before commencing meaningful discussions with or engaging assessments by their accounting firm or other non-attorney tax advisor will want to engage counsel and coordinate the involvement of their accounting and other non-attorney tax advisors through qualified legal counsel to protect and maximize the ability to conduct the analysis of their risks and options within the protection of attorney-client privilege.
For Help With These Or Other Matters
If you need assistance in conducting a risk assessment of or responding to an IRS, Labor Department or other legal challenges to your organization’s existing workforce classification or other labor and employment, employee benefit or compensation practices, please contact the author of this update, attorney Cynthia Marcotte Stamer.
Ms. Stamer has more than 24 years experience advising and representing employer, employee benefit and other clients before the Internal Revenue Service, the Department of Labor, Immigrations & Customs, and other agencies, private plaintiffs and others on worker classification and related human resources, employee benefit, internal controls and risk management matters.
A board certified labor and employment attorney widely known for her extensive and creative knowledge and experience worker classification and other employment, employee benefits and workforce matters, Ms. Stamer works extensively with employers, employee benefit plan sponsors, insurers, administrators, and fiduciaries, payroll and staffing companies, technology and other service providers and others to develop and operate legally defensible programs, practices and policies that promote the client’s human resources, employee benefits or other management goals.
A featured presenter in the recent “Worker Classification & Alternative Workforce: Employee Plans & Employment Tax Challenges” teleconference sponsored by the American Bar Association Joint Committee on Employee Benefits, Ms. Stamer also is a widely published author and highly regarded speaker on these and other employee benefit and human resources matters who is active in many other employee benefits, human resources and other management focused organizations.
A Fellow in the American College of Employee Benefits Council, the immediate past Chair and current Welfare Benefit Committee Co-Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, the Vice Chair of the ABA TIPS Employee Benefits Committee, the Gulf States Area TEGE Council Exempt Organizations Coordinator, past-Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, and the editor and publisher of Solutions Law Press HR & Benefits Update and other Solutions Law Press Publications, She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications.
You can learn more about Ms. Stamer and her experience, find out about upcoming training or other events, review some of her past training, speaking, publications and other resources, and register to receive future updates about developments on these and other concerns from Ms. Stamer at www.CynthiaStamer.com.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available at www.solutionslawpress.com.
For important information concerning this communication click here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2011 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on New IRS Voluntary IRS Settlement Program Offers New Option For Resolving Payroll Tax Risks Of Misclassification But Employers Also Must Manage Other Legal Risks |
Comments Off on New IRS Voluntary IRS Settlement Program Offers New Option For Resolving Payroll Tax Risks Of Misclassification But Employers Also Must Manage Other Legal Risks |  105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |
105(h), Cafeteria Plans, COBRA, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, Employment Tax, ERISA, Fair Labor Standards Act, family leave, FMLA, Government Contractors, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, medical leave, Military Leave, Nonresident aliens, OSHA, Payroll Tax, Restructuring, Retirement Plans, Tax, Tax Qualification, Unemployment Benefits, Unemployment Insurance, Union, VEVRRA, Wage & Hour | Tagged: contract labor, Determination Letters, Employee, Employee Benefits, Independent Contractor, leased employee, misclassificaton, payroll tax, plan qualification, Retirement Plans, staffing, Tax, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 16, 2011
The American Bar Association Tort Trial & Insurance Practice Section recently appointed Solutions Law Press Managing Editor Cynthia Marcotte Stamer to serve as Vice-Chair Appointment of the Employee Benefits General Committee for the 2011-2012 fiscal year.
The TIPS Employee Benefits Committee concentrates on helping attorneys and others keep on top of and respond to developments in the constantly evolving practice area of employee benefits, with particular emphasis on litigation and regulatory compliance issues through programs, meetings, publications and other projects and activities. Additional information about involvement in the Employee Benefits Committee and its programs, publications and activities is available here.
A noted Texas-based employee benefits and employment lawyer with extensive involvement in the leadership of the ABA and other professional organizations involved in employee benefits, health care and workforce matters, is nationally and internationally known for her pioneering leadership and work as an attorney, consultant, policy advocate, speaker and author helping businesses, governments, and communities on health and other insurance and employee benefits, patient education and empowerment, wellness and disease management, and other programs, policies, and processes. For more than 24 years, Ms. Stamer’s legal practice has focused on advising and representing employers, insurers, health care providers, community leaders and governments about health care and employee benefits policy and process improvement, quality, performance management, education, compliance, communications, risk management, reimbursement and finance, and other related matters. In addition to her legal practice, Stamer also extensively consults and provides leadership to a broad range of clients, professional and civic organizations, and others on strategies for improving the health care system and the ability of health care providers, payers, employers, community organizations, government agencies to help patients and their families to access cost-effective, quality, affordable health care and other resource needs. She also has worked extensively with a broad range of business and government clients on health care, pension, social security, workforce, insurance and many other related policy matters.
In addition to her service with TIPS, Ms. Stamer also is active in the leadership of a broad range of other professional and civil organizations. For instance, Ms. Stamer presently serves as Executive Director of Project COPE, the Coalition on Patient Empowerment and the Coalition for Responsible Healthcare Policy; Vice President of the North Texas Healthcare Compliance Professionals Association; Immediate Past Chair of the American Bar Association RPTE Employee Benefits & Other Compensation Committee and its representative to the ABA Joint Committee on Employee Benefits and Vice Chair of its Welfare Benefits Committee; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; and as the Gulf Coast TEGE Council TE Committee Coordinator. She previously served as a founding Board Member and President of the Alliance for Healthcare Excellence, as a Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; the Board President of the early retirement intervention agency, The Richardson Development Center for Children; Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a member of the Board of Directors of the Southwest Benefits Association; on many seminar faculties and in many other professional and civic leadership and volunteer roles.
Author of the hundreds of publications and workshops these and other employment, employee benefits, health care, insurance, workforce and other management matters, Ms. Stamer’s insights on employee benefits, insurance, health care and workforce matters in Atlantic Information Services, The Bureau of National Affairs, HealthLeaders, Modern Healthcare, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other publications. She also regularly conducts training and speaks on these and other management, compliance and public policy concerns. Some recent publications and programs that may be of interest include:
For additional information about Ms. Stamer, upcoming training, publications or other materials or events, see here or contact Ms. Stamer directly via email here or (469) 767-8872.
IIf you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here. For important information concerning this communication click here. If you do not wish to receive these updates in the future, send an e-mail with the word “Remove” in the Subject to here.
©2011 Cynthia Marcotte Stamer, P.C. All rights reserved.
 Comments Off on ABA TIPS Section Appoints Cynthia Marcotte Stamer Vice Chair of Employee Benefits General Committee |
Comments Off on ABA TIPS Section Appoints Cynthia Marcotte Stamer Vice Chair of Employee Benefits General Committee |  Cafeteria Plans, COBRA, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, Fiduciary Responsibility, Health Plans, HIPAA, Human Resources, Insurance, Internal Controls, Malpractice, Medicare Part D, Mental Health, Mental Health Parity, Preemption, Prescription Drugs, Retirement Plans, Wellness, Wellness Programs |
Cafeteria Plans, COBRA, Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, Fiduciary Responsibility, Health Plans, HIPAA, Human Resources, Insurance, Internal Controls, Malpractice, Medicare Part D, Mental Health, Mental Health Parity, Preemption, Prescription Drugs, Retirement Plans, Wellness, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 29, 2011
A new 2011 U.S. Department of Labor Bureau of Labor Statistics Study of employee benefits offered shares key insights into how many employers offer employer-provided health and other benefits The study shows that health and other benefits offered by employers, how much employers contribute and when employees enroll in offered benefits varies widely varied by whether the employer is a government or private sector employer, the industry, size and other characteristics of the employer and the income, profession, education and other characteristics of the employee. It is no surprise that government employers that can pass along costs to taxpayers provide coverage more broadly and subsidize more of the cost.
With regard to health benefits, the report reveals that practices vary significantly among employers, on average, medical care benefits were available to 69 percent of private industry workers and half of workers participated in a medical plan. For single coverage, private sector employers paid 80 percent of the medical care premiums for full-time workers and 69 percent of medical care premiums for full-time workers in private industry. Data shows employees often elect not to take offered coverage.
In addition to data on medical benefits, the study also reports that paid leave remains the most commonly provided benefit nationally and includes data on other benefits.
The DOL highlights 1st time reporting of domestic partner status for 1st time in its announcement. Data also provided on paid vacation and other leave.
Read report summary and access report at http://www.bls.gov/news.release/ebs2.nr0.htm.
For Help or More Information
If you have questions or need help understanding or responding to the Regulations, with other health benefit design, administration or operations concerns, or with other employee benefits, compensation, labor or employment or other workforce management concerns, please contact the author of this update, Board Certified Labor and Employment attorney and management consultant Cynthia Marcotte Stamer here or at (469)767-8872.
Past Chair of the American Bar Association (ABA) Health Law Section Managed Care & Insurance Interest Group, Chair of the ABA RPTE Employee Benefit and Other Compensation Committee, and a council member of the ABA Joint Committee on Employee Benefits, Ms. Stamer is nationally recognized for her more than 23 years pragmatic and innovative health program work.
Board certified in labor and employment law by the Texas Board of Legal Specialization with extensive leading edge health plan experience, Ms. Stamer has worked continuously throughout her career helping health plan sponsors, fiduciaries, administrators, insurers and others design, administer and defend health and other employee benefit and insurance programs domestically and internationally. She is widely recognized for her experience helping design and implement legally compliant self-insured and insured health reimbursement, mini-med, high-deductible health plans, limited benefit plans, 24-hour and occupational medicine, ex-pat and medical tourism, deductible reimbursement and other creative health benefit programs to solve a wide range of financial and other challenges while coping with changing regulatory and market realities. Her work includes both working with clients to design, document, implement and administer these and other arrangements, as well as the development of wellness and disease management, claims administration and appeals, eligibility, and other administrative services, processes and technologies. She also works with plan fiduciaries, plan sponsors, insurers, administrators, brokers and advisors, bankruptcy trustees, creditors, debtors, service providers and their officers and directors about the prevention, investigation, mitigation and resolutions of civil and criminal liability arising from suspected or known benefit administration claims, breaches of fiduciary duty, privacy and data security breach, vendor disputes and other disputes arising in relation to employee benefit and insurance arrangements. As a continuing part of this representation, Ms. Stamer regularly represents and defends plan sponsors, fiduciaries, third party administrators and other service providers and management officials in dealings with the Department of Labor, Department of Justice, Department of Health & Human Services, Department of Defense, Securities and Exchange Commission, state insurance regulators, state attorneys general and other federal and state regulators and prosecutors and private plaintiffs in connection with investigations, prosecutions, audits and other actions arising from employee benefit, insurance and related arrangements and products.
Recognized in the International Who’s Who of Professionals and bearing the Martindale Hubble Premier AV-Rating, Ms. Stamer also is a highly regarded author and speaker, who regularly conducts management and other training on a wide range of labor and employment, employee benefit, human resources, internal controls and other related risk management matters. Her writings frequently are published by the American Bar Association (ABA), Aspen Publishers, Bureau of National Affairs, the American Health Lawyers Association, SHRM, World At Work, Government Institutes, Inc., Atlantic Information Services, Employee Benefit News, and many others. For a listing of some of these publications and programs, see here. Her insights on human resources risk management matters also have been quoted in The Wall Street Journal, various publications of The Bureau of National Affairs and Aspen Publishing, the Dallas Morning News, Spencer Publications, Health Leaders, Business Insurance, the Dallas and Houston Business Journals and a host of other publications. In addition to her many ABA leadership involvements, she also serves in leadership positions in numerous human resources, corporate compliance, and other professional and civic organizations. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, World At Work, the ICEBS, SHRM and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Labor Department 2011 Stats Show Employer Health Coverage & Other Benefit Statistics |
Comments Off on Labor Department 2011 Stats Show Employer Health Coverage & Other Benefit Statistics |  105(h), Absenteeism, Affordable Care Act, COBRA, Disability, Disability, Disability Plans, Employers, ERISA, FMLA, Health Care Reform, Health Plans, Human Resources, Insurance, Public Policy | Tagged: Affordable Care Act, Employee Benefits, grandfathered health plan, grandfathered plan, Health Care Reform, Health Insurance, Health Plans, Insurance, medical insurance |
105(h), Absenteeism, Affordable Care Act, COBRA, Disability, Disability, Disability Plans, Employers, ERISA, FMLA, Health Care Reform, Health Plans, Human Resources, Insurance, Public Policy | Tagged: Affordable Care Act, Employee Benefits, grandfathered health plan, grandfathered plan, Health Care Reform, Health Insurance, Health Plans, Insurance, medical insurance |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 20, 2011
The National Labor Regulations Board (NLRB)’s announcement of a settlement against a Connecticut nursing home operator this week in conjunction with a series of other enforcement actions highlight the need for businesses to tighten defenses and exercise other caution to minimize their organization’s exposure to potential NLRB charges or investigation. As reflected by many of these enforcement acts, the exposures arise both from active efforts by businesses to suppress union organizing or contracting activities, as well as the failure to identify and manage hidden labor law exposures in the design and administration of more ordinary human resources, compliance, business operations and other policies and practices.
On May 17, 2011, the NLRB announced here that Connecticut nursing home operator Spectrum Healthcare has agreed to settle a NLRB case involving multiple allegations of unlawful suspensions, discharges and unilateral changes in violation of the National Labor Relations Act and other federal labor laws by offering reinstatement and back pay to all discharged and striking workers and signing a new three-year collective bargaining agreement with its employees’ union, New England Health Care Employees Union District 1199, SEIU.
Along with the contract and reinstatement of all employees, the company agreed to pay $545,000 in back pay and pension benefits to employees who were harmed by the unfair labor practices, and to expunge any disciplinary records related to the case. As a result, all NLRB charges against the company have been withdrawn. Spectrum admits to no wrongdoing in the settlement.
The settlement, reached midway through a hearing before an NLRB administrative law judge in Connecticut and approved by the judge yesterday, ends a long-running dispute which grew into a strike by almost 400 employees at four nursing homes in Connecticut operated by Spectrum Healthcare, LLC. Complaints issued by the NLRB Regional Office in Hartford alleged that, beginning in the fall of 2009, several months after the prior collective bargaining agreement expired, Spectrum discharged seven employees and suspended three others to retaliate against their union activities and to discourage other employees from supporting the union. In addition, one employee was discharged and seven others were suspended after the employer unilaterally changed its tardiness discipline policy without first bargaining with the union.
The complaints further alleged that in April 2010, employees at the four nursing homes — in Derby, Ansonia, Winsted, and Hartford — went on strike to protest the unfair labor practices. When the strikers offered unconditionally to return to work in late August, the employer refused to take them back. Under federal labor law, if a strike is called because of an unfair labor practice, employees are entitled to reinstatement after an unconditional offer to return to work.
The reinstated employees are due to return to the facilities this week.
The Spectrum Healthcare settlement is reflective of the growing number of NLRB enforcement orders against employers generally and health care providers specifically under the Obama Administration. The Obama Administration has close ties and has expressed its strong and open support for union and union organizing activities. The adoption of a series of union friendly labor law reforms was one of the key campaign promises of President Obama during his election campaign. While other legislative priorities and the change in the leadership of the House of Representatives appears to have slowed efforts to push through this agenda, it has not slowed the Administration’s efforts to support unions with strong enforcement activities. Empowered by a difficult economic and job situation and an awareness of the Obama Administration’s strong support for union organizing and other activities, unions are stepping up organizing efforts and more aggressively challenging employers actions.
Over the past few months, public awareness of the Obama Administration’s aggressive enforcement agenda on behalf of unions has drawn new attention as a result of the widespread media coverage of NLRB actions challenging Boeings planned relocation of certain manufacturing jobs intervention in a planned relocation of certain manufacturing operations. See, e.g., Acting General Counsel Lafe Solomon releases statement on Boeing complaint; National Labor Relations Board issues complaint against Boeing Company for unlawfully transferring work to a non-union facility. However, the Boeing and Spectrum Healthcare actions represent only the tip of the iceberg of the rising number of NLRB enforcement activities, most of which take place with little media or public attention.
Along side the Spectrum Healthcare and Boeing actions, in recent weeks, the NLRB also has been busy with several other enforcement activities. For instance:
- On May 9 2011, the NLRB issued a complaint against Hispanics United of Buffalo (HUB), a nonprofit that provides social services to low-income clients, that alleges that HUB unlawfully discharged five employees after they took to Facebook to criticize working conditions, including work load and staffing issues. The case involves an employee who, in advance of a meeting with management about working conditions, posted to her Facebook ; and
- On May 17, the NLRB secured a temporary injunction from a U.S. District Court in San Jose California against San Jose area waste hauling company OS Transport LLC, charged with engaging in unfair labor practices including the termination of a lead organizer and another Union supporter, retaliation against Union efforts in the form of unfavorable assignments, threats to Union supporters, and promises of improved treatment of employees who disavow the Union for the alleged purpose of defeating a union. o offer reinstatement to two drivers and restore full assignments to other drivers who had expressed support for a union during an organizing campaign. More Details here.,
In addition, in recent weeks, the NLRB also has:
Amid this difficult enforcement environment, business leaders should exercise special care to prepare to defend their actions against both potential organizing efforts, to understand the types of actions and activities that may help fuel charges, and take steps to manage these and other union organization and other labor risks.
For Help With Labor & Employment, Employee Benefits Or Other Risk Management and Defense
If you need assistance in auditing or assessing, updating or defending your labor and employment, employee benefits, compliance, risk manage or other internal controls practices or actions, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here .
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Spectrum Healthcare NLRB Charge Settlement Highlights Need To Defend Against Possible Unfair Labor Practices & Other Union Exposures |
Comments Off on Spectrum Healthcare NLRB Charge Settlement Highlights Need To Defend Against Possible Unfair Labor Practices & Other Union Exposures |  105(h), Absenteeism, ADA, Affirmative Action, Affordable Care Act, ARRA, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Claims Administration, COBRA, COBRA Subsidy, Corporate Compliance, Data Security, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, Excise Tax, Fair Labor Standards Act, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, H.R. 4872, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Malpractice, medical leave, Medicare Part D, Mental Health, Mental Health Parity, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Pandemic, Patient Empowerment, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Refunds, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Stimulus Bill, Swine Flu, Tax, Tax Credit, Tax Qualification, Telecommuting, Uncategorized, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs, Whistleblower | Tagged: ADAAA, Americans With Disabiltiies Act, Employer, employment discrimination, facebook, HR, Human Resources, NLRA, social medial, unfair labor practices, Union |
105(h), Absenteeism, ADA, Affirmative Action, Affordable Care Act, ARRA, Bankruptcy, Cafeteria Plans, Child Labor, CHIP, Claims Administration, COBRA, COBRA Subsidy, Corporate Compliance, Data Security, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability, Disability Plans, Discrimination, Disease Management, Drug & Alcohol, E-Verify, EEOC, Employee Benefits, Employers, Employment Agreement, Employment Tax, ERISA, Excise Tax, Fair Labor Standards Act, family leave, Fiduciary Responsibility, FMLA, GINA, Government Contractors, H.R. 4872, Health Care Reform, Health Plans, HIPAA, Human Resources, I-9, Immigration, Income Tax, Insurance, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Malpractice, medical leave, Medicare Part D, Mental Health, Mental Health Parity, Military Leave, Non-Compete, Non-Competition Agreement, Nonresident aliens, OFCCP, OSHA, Pandemic, Patient Empowerment, Patient Protection and Affordable Care Act, Payroll Tax, Preemption, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Public Policy, Refunds, Rehabilitation Act, Reporting & Disclosure, Restructuring, Retaliation, Retirement Plans, Risk Management, Safety, Sexual Harassment, Stimulus Bill, Swine Flu, Tax, Tax Credit, Tax Qualification, Telecommuting, Uncategorized, Unemployment Benefits, Unemployment Insurance, Union, USERRA, VEVRRA, Wage & Hour, Wellness, Wellness Programs, Whistleblower | Tagged: ADAAA, Americans With Disabiltiies Act, Employer, employment discrimination, facebook, HR, Human Resources, NLRA, social medial, unfair labor practices, Union |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 24, 2011
Employers Urged To Tighten Disability Related Discrimination Risk Management
Employers should review and update their existing employment and employee benefit practices in response to updated regulations (Final Regulations) governing the disability discrimination rules of the Americans With Disabilities Act as amended by the ADA Amendments Act (ADAAA) that the Equal Employment Opportunity Commission (EEOC) will publish in the Friday, March 25, 2011 Federal Register.
On Thursday, March 24, 2011, the EEOC released an advance copy of the Final Regulations along with two Question-and-Answer documents about the Final Regulations to aid the public and employers – including small business – in understanding the law and new regulations. The Final Regulations, accompanying Question and Answer documents and a fact sheet are available on the EEOC website here .
The changes contained in the updated Final Regulations update the EEOC’s disability regulations in response to amendments made to the ADA by Congress as part of the ADAAA. Like the ADAAA they implement, the Final regulations are designed to simplify the determination of who has a “disability” and make it easier for people to establish that they are protected by the Americans with Disabilities Act (ADA).
The Final Regulations and the ADAAA amendments they implement make it likely that businesses generally will face more disability claims from a broader range of employees and will possess fewer legal shields to defend themselves against these claims. Since these changes make it easier for certain employees to qualify as disabled under the ADA, businesses should act strategically to mitigate their ADA exposures in response to the Final Regulations. Learn more about the Final Regulations and get suggestions for risk management of expanding disabilities discrimination exposures here.
For Help With Disability Discrimination Risk Management or Other Needs
If you need assistance in auditing or assessing, updating or defending your disability management or with other labor and employment, employee benefit, compensation or internal controls practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer is nationally and internationally recognized for more than 23 years of work helping employers; employee benefit plans and their sponsors, administrators, fiduciaries; employee leasing, recruiting, staffing and other professional employment organizations; and others design, administer and defend innovative workforce, compensation, employee benefit and management policies and practices. Her experience includes extensive work helping employers implement, audit, manage and defend wage and hour and other workforce and internal controls policies, procedures and actions. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on wage and hour, worker classification and other human resources and workforce, employee benefits, compensation, internal controls and related matters. She also is recognized for her publications, industry leadership, workshops and presentations on these and other human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here .
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on EEOC Finalizes Updates To Disability Regulations In Response to ADA Amendments Act |
Comments Off on EEOC Finalizes Updates To Disability Regulations In Response to ADA Amendments Act |  Absenteeism, ADA, Affirmative Action, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Drug & Alcohol, EEOC, Employee Benefits, Employers, GINA, Government Contractors, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Leave, Military Leave, Non-Compete, Rehabilitation Act, Retaliation, Union | Tagged: ADA, ADAAA, Americans With Disabiltiies Act, Disability Discrimination, Employer, employment discrimination, HR, Human Resources |
Absenteeism, ADA, Affirmative Action, Corporate Compliance, Disability, Disability, Disability Plans, Discrimination, Drug & Alcohol, EEOC, Employee Benefits, Employers, GINA, Government Contractors, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Leave, Military Leave, Non-Compete, Rehabilitation Act, Retaliation, Union | Tagged: ADA, ADAAA, Americans With Disabiltiies Act, Disability Discrimination, Employer, employment discrimination, HR, Human Resources |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
February 25, 2011
TPA’s Embezzlement Guilty Plea Reminds Plan Sponsors, Fiduciaries & Service Providers To Ensure Fiduciaries, Administrators & Staff Prudently Selected, Monitored & Bonded
The guilty plea of an Ohio-based third-party administrator to embezzlement of $1 million in plan assets reminds employers and other employee benefit plan sponsors and members of their management participating in plan related activities, plan administrators and other plan fiduciaries and plan service providers (“plan decision-makers”) of the importance of ensuring appropriate, well-documented credentialing and selection, oversight, auditing and bonding the individuals and companies acting as fiduciaries and others participating in administration of plans or their assets (“plan workforce members”) to minimize their potential exposure to potential personal liability as a result of the fraud under the Employee Retirement Income Security Act (ERISA).
Cox Prosecution Reflective DOL Readiness To Prosecute Parties For Misuse of Plan Monies & Other Plan Fraud
According to a February 23, 2011 U.S. Department of Labor (DOL) announcement, Rhonda Sue Irvin Cox, owner of Irvin Administrative Solutions LLC (IAS), pleaded guilty to the embezzlement of $1 million of retirement plan assets from client plans administered by IAS. The DOL reports that between January 2003 and April 2007, Cox plead guilty to using used her position with ISC to embezzle the funds from 12 of 59 plans for which IAS served as a third party administrator. Cox also pleaded guilty to one count of making false statements in documents required under ERISA to be kept and certified by the plans’ administrator. Scheduled to be sentenced on June 1, 2011, Cox faces a maximum of five years in prison on each criminal count, a $250,000 fine and a special assessment. Cox is scheduled to be sentenced on June 1, 2011.
The DOL and Justice Department have a long-standing record of aggressive investigation and prosecution of embezzlement or other fraud impacting health and other employee benefit plans. Their criminal and civil enforcement and prosecution record makes clear this commitment remains strong.
Plan Sponsors, Fiduciaries & Service Providers May Face Civil Liability From When Others Defraud Their Plans
While plan decision-makers generally are aware that individuals defrauding health or other employee benefit plans risk criminal and civil prosecution, many fail to recognize their own potential civil liability exposures that may arise out of the fraudulent acts or other misconduct of another plan workforce member.
Embezzlement of plan assets is one of many acts of misconduct that can create potential fiduciary liability exposure for plan decision-makers under ERISA. Until confronted with potential fraud, misconduct or other misfeasance by a plan fiduciary, service provider or other plan workforce member, many plan decision-makers lack an adequate appreciation of the personal liability they may incur if they cannot demonstrate appropriate steps were taken to protect their health plan from this misconduct.
Under ERISA’s fiduciary responsibility rules, embezzlement or other misuse of employee contributions or other plan assets as well as certain other misconduct or misfeasance by a plan fiduciary, service provider or other plan workforce member can create personal liability exposures for plan decision-makers with responsibility or discretionary authority over the selection, retention, or management of plan workforce members if the plan decision-maker cannot demonstrate appropriate steps were taken to select, monitor and bond the plan workforce and other prudent action was taken to prevent and redress the fraud. Accordingly, health plans, their sponsors, fiduciaries, service providers, their management, and others serving as, or selecting, managing or retaining companies or individuals that participate in the handling of health plan assets or administration should act to strengthen their health plans and themselves against these exposures.
Risk Management Strategies & Tips
When embezzlement or other concern affecting their health plan arises, plan decision-makers concerned about protecting their health plans and themselves must act promptly in a carefully documented, prudent manner to investigate and respond to the concern. They should be prepared to present well-documented evidence of the scope and limits of their responsibility, authority, awareness, and potential for the selection, monitoring and oversight of the plan workforce member or others responsible for the performance of those actions, the adequacy of the bonding arrangements for the plan, and other efforts to prudently protect the plan before, during and after the discovery of the concern. While these and other steps can help strengthen the ability of a plan decision-maker to liability exposures that can result from the other plan workforce member’s embezzlement of plan assets or other misconduct, plan sponsors and plan decision-makers also should acquire suitable fiduciary and other liability insurance coverage and make other arrangements to help provide for the potential financial costs and other demands that are likely to arise in the event that it becomes necessary to investigate or redress fraud or other misconduct. Learn more here.
For Help With Investigations, Policy Review & Updates Or Other Needs
If you need help investigating or responding to fraud or other misconduct affection a health or other employee benefit plan, dealing with an employee benefit plan investigation or enforcement action by the Labor Department, private plaintiffs or another public or private party, reviewing current or proposed health plan processes or procedures, or responding to other employee benefit, labor and employment or other related controls and practices, please contact the author of this update, attorney Cynthia Marcotte Stamer here or at (469)767-8872.
The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, and past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer works, publishes and speaks extensively on HIPAA and other privacy and data security, health plan, health care and other human resources and workforce, employee benefits, compensation, internal controls and related matters.
For more than 23 years, Ms. Stamer has counseled, represented and trained employers and other employee benefit plan sponsors, plan administrators and fiduciaries, insurers and financial services providers, third party administrators, human resources and employee benefit information technology vendors and others privacy and data security, fiduciary responsibility, plan design and administration and other compliance, risk management and operations matters. In connection with this work, Ms. Stamer regularly counsels and helps clients to defend a broad range of clients about employee benefit plan fraud and other fiduciary responsibility concerns. Throughout her career, she has represented and served as special counsel to health and other employee benefit plans, plan sponsors, plan service providers, officers, directors and other management officials, bankruptcy trustees, debtors and creditors, and others in connection with health and other employee benefit plan fraud and other fiduciary responsibility and related investigations, prosecutions and other actions involving the Labor Department, IRS, HHS, Justice Department, state insurance and attorneys general, bankruptcy actions, and participant, beneficiary and vendor disputes. She also is recognized for her publications, industry leadership, workshops and presentations on these and other employee benefits, insurance and human resources concerns and regularly speaks and conducts training on these matters. Her insights on these and other matters appear in the Bureau of National Affairs, Spencer Publications, the Wall Street Journal, the Dallas Business Journal, the Houston Business Journal, and many other national and local publications. For additional information about Ms. Stamer and her experience or to access other publications by Ms. Stamer see here or contact Ms. Stamer directly.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on health care, human resources, employee benefits, data security and privacy, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile at here or e-mailing this information here. To unsubscribe, e-mail here.
©2011 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Avoiding Liability For Another’s Health Plan Fraud |
Comments Off on Avoiding Liability For Another’s Health Plan Fraud |  Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Malpractice, Professional Liability, Retirement Plans, Risk Management | Tagged: co-fiduciary liability, embezzlement, employee benefit, ERISA, Fiduciary Liability, fraud, Health Plan |
Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Malpractice, Professional Liability, Retirement Plans, Risk Management | Tagged: co-fiduciary liability, embezzlement, employee benefit, ERISA, Fiduciary Liability, fraud, Health Plan |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 29, 2010
With New Years Eve celebrations approaching and the Holiday Season wrapping up, businesses should take some common sense steps to decrease the risk of waking up in 2011 with a liability hangover. Participation of employees and clients in company sponsored and other social celebrations and activities can promote big rewards in relationship development and morale if properly managed. However, the music, food, game playing, toasting with alcohol and other aspects of the celebratory atmosphere at New Years Eve and other parties and social activities heighten the risk that certain employees or other business associates will engage in, or be subject to, risky or other inappropriate behavior that can create liability exposures or other business concerns for your business whether or not company sponsored. Read about other common Holiday Season-related celebration risks and management tips here.
Celebrations Raise Foreseeable Risks
Whether or not company-sponsored, holiday parties and other celebrations where employees celebrate with other employees or clients tend to fuel bad behavior by inviting fraternization, lowering inhibitions and obscuring the line between appropriate and inappropriate social and business behavior. The relaxation of the environment heightens the risk that certain employees or clients will make unwelcome sexual advances, make sexually suggestive or other inappropriate statements, or engage in other actions that expose the business to sexual harassment or other employment discrimination liability. Businesses also should use care to manage other discrimination exposures in the planning of holiday festivities, gift exchanges, and other activities. Businesses also should be vigilant in watching for signs of inappropriate patterns of discrimination in the selection of employees invited to participate in company-connected social events as well as off-duty holiday gatherings sponsored by managers and supervisors. In addition, businesses also should critically review their own plans for possible insensitivity. Business connected holiday parties, communications, gifts and other festivities should be designed to show appropriate sensitivity to religious and other cultural diversity.
To minimize these exposures, businesses should take steps to communicate and reinforce company policies and expectations about sexual harassment, discrimination, fraternization and other conduct viewed as inappropriate by the company and communicating reminders about these policies to employees and business associates during the Holiday Season.
Timely Investigation & Notification
Businesses faced with allegations of discrimination, sexual harassment or other misconduct also should act promptly to investigate any concerns and if necessary, take timely corrective action. Delay in investigation or redress of discrimination or other improprieties can increase the liability exposure of a business presented with a valid complaint and complicate the ability to defend charges that may arise against the business. Additionally, delay also increases the likelihood that a complaining party will contact governmental officials, plaintiff’s lawyers or others outside the corporation in the redress of his concern.
If a report of an accident, act of discrimination or sexual harassment or other liability related event arises, remember to consider as part of your response whether you need to report the event to any insurers or agencies. Injuries occurring at company related functions often qualify as occupational injuries subject to worker’s compensation and occupational safety laws. Likewise, automobile, employment practices liability, and general liability policies often require covered parties to tell the carrier promptly upon receipt of notice of an event or claim that may give rise to coverage, even though the carrier may not be obligated to tender a defense or coverage at that time.
For Help With Investigations, Policy Updates Or Other Needs
If your organization needs help investigating a reported concern, reviewing and updating its policies or assessing, managing or defending these or other labor and employment, compensation or benefit practices, or needs other assistance auditing, updating or defending its human resources, corporate ethics, and compliance practices, or responding to employment related or other charges or suits, please contact management attorney and consultant Cynthia Marcotte Stamer at cstamer@solutionslawyer.net, (468) 767-8872.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization and Chair of the American Bar Association RPTE Employee Benefits & Other Compensation Group and a nationally recognized author and speaker, Ms. Stamer helps business manage people, operations and risk. She is experienced with advising and assisting employers with these and other labor and employment, employee benefit, compensation, risk management and internal controls matters. Her experience includes helping management both manage performance and manage legal risk and compliance. While helping businesses define and manage the conduct and performance of their employees, contractors and vendors, she also assists employers and others about compliance with federal and state equal employment opportunity, compensation, health and other employee benefit, workplace safety, and other labor and employment laws, advises and defends businesses against labor and employment, employee benefit, compensation, fraud and other regulatory compliance and other related audits, investigations and litigation, charges, audits, claims and investigations by the IRS, Department of Labor, Department of Justice, SEC, Federal Trade Commission, HUD, HHS, DOD, Departments of Insurance, and other federal and state regulators. She has counseled and represented businesses and their management on workforce and other internal controls and risk management matters for more than 23 years. Ms. Stamer also speaks and writes extensively on these and other related matters. For additional information about Ms. Stamer and her experience or to get access to other publications by Ms. Stamer see here or contact Ms. Stamer directly.
Other Helpful Resources & Information
If you found this article of interest, you also may be interested in reviewing other Breaking News, articles and other resources available CynthiaStamer.com or Solutions Law Press articles authored by Ms. Stamer including:
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available for review here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here. For important information concerning this communication click here. If you do not wish to receive these updates in the future, unsubscribe by updating your profile here.
©2010 Cynthia Marcotte Stamer, P.C. Non-exclusive right to republish granted to Solutions Law Press. All other rights reserved.
 Comments Off on Avoiding Post-Holiday Celebration Sexual Harassment & Discrimination Liability |
Comments Off on Avoiding Post-Holiday Celebration Sexual Harassment & Discrimination Liability |  ADA, Affirmative Action, Corporate Compliance, Disability Plans, Discrimination, EEOC, Employee Benefits, Employers, Human Resources, Internal Controls, Internal Investigations, Uncategorized |
ADA, Affirmative Action, Corporate Compliance, Disability Plans, Discrimination, EEOC, Employee Benefits, Employers, Human Resources, Internal Controls, Internal Investigations, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 21, 2010
The U.S. Department of Labor Employee Benefit Security Administration (EBSA) today published a Proposed Regulation that would expand the circumstances when individuals giving investment advice to an employee benefit or employee benefit plan or individual retirement account participant for purposes of the fiduciary definition of Employee Retirement Income Security Act (ERISA) § 3(21) and the prohibited transaction provisions of Internal Revenue Code (Code) § 4975(e)(3)(B).
If adopted as proposed, the Proposed Regulation would broaden the persons considered fiduciaries based on their provision of investment related advice or services to plans, participants or beneficiaries. Additionally, the restatement of these standards also likely will necessitate that both plan fiduciaries and providers of these services tighten agreements and other practices and procedures governing the engagement and delivery of services in order to maintain or protect desired allocations of fiduciary responsibility over these activities.
The deadline for individuals and organizations to comment on the proposed rule is January 19, 2011. Plan sponsors, fiduciaries, service providers and others concerned about the potential impact of the proposed changes should assess the potential implications of the rule and timely submit any comments or concern to the EBSA by this date.
To learn more about the Proposed Rule and its implications, see the more detailed article here.
If your organization needs assistance to evaluate or respond to the Proposed Regulation or reviewing, updating, administering or defending your employee benefit, human resources, compensation or internal control and risk management procedures, documentation, or policies or procedures, please contact the author of this update, Board Certified Labor & Employment attorney Cynthia Marcotte Stamer at (469) 767-8872 or via e-mail here.
Other Resources
If you found this information of interest, you also may be interested in reviewing other recent Solutions Law Press updates including:
About Ms. Stamer
Chair of the American Bar Association (ABA) RPTE Employee Benefit & Other Compensation Group, a Council Member of the ABA Joint Committee on Employee Benefits and Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Cynthia Marcotte Stamer is nationally recognized for her extensive work helping clients develop, implement and defend innovative, practical, legally defensible solutions to their particular health and other employee benefit, employment and insurance needs. Ms. Stamer has more than 23 years experience advising and representing employer, association and other plan sponsors, health and other employee benefit plans, their fiduciaries, plan administrators, consultants, vendors, outsourcers, insurers, governments and others about health plan and product design; administration, legal and operational risk management, vendor and fiduciary credentialing, managed care and vendor contracting, cost-containment, documentation, public policy, enforcement, privacy, technology, litigation and other concerns. Ms. Stamer also publishes, conducts client and other training, speaks and consults extensively on these and other health and managed care program concerns and practices for the ABA, American Health Lawyers Association, Institute of Internal Auditors, Society for Professional Benefits Administrators, HCCA, Southwest Benefits Association and many other organizations. Her insights on these and related topics have appeared in Atlantic Information Service, Bureau of National Affairs, World At Work, The Wall Street Journal, Business Insurance, Managed Healthcare, Health Leaders, various ABA publications and a many other national and local publications. To learn more about Ms. Stamer, her experience, involvements, programs and publications, see here or contact Ms. Stamer.
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available for review here. If you or someone else you know would like to receive future updates and notices about other upcoming Solutions Law Press events, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here. For important information concerning this communication click here.
©2010 Cynthia Marcotte Stamer PC. Reprint Permission Granted To Solutions Law Press. All other rights reserved.
 Comments Off on DOL Proposes To Expand Investment Related Services Giving Rise to ERISA Fiduciary Status As Investment Fiduciary |
Comments Off on DOL Proposes To Expand Investment Related Services Giving Rise to ERISA Fiduciary Status As Investment Fiduciary |  Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Retirement Plans, Risk Management, Tax, Tax Qualification |
Corporate Compliance, Defined Benefit Plans, Defined Contribution Plans, Disability Plans, Employee Benefits, Employers, ERISA, Excise Tax, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Internal Controls, Internal Investigations, Retirement Plans, Risk Management, Tax, Tax Qualification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 19, 2010
Two new Equal Employment Opportunity Commission (EEOC) lawsuits filed against a Texas concrete manufacturer and Los Angeles garment manufacturer highlight the need for U.S. employers with more than 14 employees to consider and prepare to defend against potential disability discrimination exposures when dealing with medical leave requests by employees who might be considered disabled under the Americans with Disabilities Act (ADA) as well as other expanding ADA enforcement exposures. Read more.
The lawsuits reflect that employers considering an employee’s request for medical leave should evaluate if the ADA requires the employer to grant the requested medical leave in addition to considering any otherwise applicable leave entitlement the requesting employee qualifies for under the Family & Medical Leave Act, state leave laws or otherwise applicable employer policies. As a result, all employers of 15 or more employees generally should review and tighten their policies and processes for evaluating requests for medical leave to minimize their exposure to claims that the denial of a requested medical leave violated the ADA.
Furthermore, employers also should consider the advisability of other more generalized policy or procedure updates to strengthen their defensibility against potential ADA and other disability claims generally in light of stepped up enforcement by the EEOC and private plaintiffs changes to the ADA made by the ADA Amendments Act of 2008 (ADAAA) that makes it easier for employees to win ADA suits. To mitigate growing exposures to these claims, employers covered by the ADA and/or the Rehabilitation Act of 1973 should review and strengthen their existing hiring and other employment practices and documentation to strengthen their defensibility in the face of these new challenges.
If you need assistance responding an employee’s request for medical leave or other accommodations, or otherwise to review, update or defend your disability discrimination or other employment, compensation, benefits or other workforce, internal controls or risk management practices, please contact the author of this update, Board Certified Labor & Employment attorney Cynthia Marcotte Stamer at (469) 767-8872 or via e-mail here.
Other Resources
If you found this information of interest, you also may be interested in reviewing other recent Solutions Law Press updates including:
About Ms. Stamer
Management attorney and consultant Cynthia Marcotte Stamer helps businesses, governments and associations solve problems, develop and implement strategies to manage people, processes, and regulatory exposures to achieve their business and operational objectives and manage legal, operational and other risks. When working with clients, Ms. Stamer combines a client-oriented approach with an extensive practical and technical knowledge of human resources, insurance, employee benefits, health care, privacy & security, corporate compliance and other legal matters to assist clients to formulate and administer pragmatic operational and risk management strategies and effective internal controls taking into account the financial, operational, political, legal and other realities confronting the client.
Recognized in the International Who’s Who of Professionals and bearing the Martindale Hubble Premier AV-Rating, Ms. Stamer also is a highly regarded author and speaker who serves in the leadership of many professional and civil organizations. She regularly conducts management and other training on a wide range of workforce management, employee benefits, compensation, risk management internal controls, and other related matters for businesses, trade and professional associations and others. Her insights on human resources risk management matters appear in The Wall Street Journal, various publications of The Bureau of National Affairs and Aspen Publishing, the Dallas Morning News, Spencer Publications, Health Leaders, Business Insurance, the Dallas and Houston Business Journals and a host of other publications. To request Ms. Stamer’s assistance, for information about arranging for Ms. Stamer to provide workshops and other training, to access other publications or resources or for more details about Ms. Stamer’s experience and other credentials, contact Ms. Stamer at via telephone at 469.767.8872 or via e-mail at cstamer@solutionslawyer.net or see CynthiaStamer.com.
If you or someone else you know would like to receive future updates and notices about upcoming programs and events, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here. To unsubscribe, send an e-mail with “Unsubscribe” in the subject here. For important information concerning this communication see here.
©2010 Cynthia Marcotte Stamer. License to reprint granted to Solutions Law Press. All other rights reserved.
 Comments Off on EEOC Attacks Medical Leave Denials As Prohibited Disability Discrimination |
Comments Off on EEOC Attacks Medical Leave Denials As Prohibited Disability Discrimination |  Absenteeism, ADA, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, family leave, Human Resources, Leave, medical leave, Rehabilitation Act | Tagged: absence management, Absenteeism, ADA, Disability, Disability Discrimination, Discrimination, EEOC, Employer, FMLA, medical leave, Risk Management |
Absenteeism, ADA, Disability, Disability, Disability Plans, Discrimination, Employee Benefits, Employers, family leave, Human Resources, Leave, medical leave, Rehabilitation Act | Tagged: absence management, Absenteeism, ADA, Disability, Disability Discrimination, Discrimination, EEOC, Employer, FMLA, medical leave, Risk Management |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 13, 2010
Health Care Reform: What You Need To Know To Build Your Family’s Healthcare Survival Plan
August 26, 2010
6:30-8:00 PM
Sunrise of Plano Center
4800 West Parker Road
Plano, Texas 75093
Sunrise Senior Living is inviting members of the public to learn from attorney and author Cynthia Marcotte Stamer about health care reform and learn practical tips to help senior and other patients and their caregivers plan their family’s healthcare survival plan.
The program will be held on August 26, 2010 from 6:30 PM-8:00 PM at the Sunrise of Plano Center located at 4800 West Parker Road, Plano, TX 75093.
During the program, Ms. Stamer will overview the impending health care reforms recently enacted by Congress and share some practical tools and information to help patients and their families, caregivers, employer and others plan for and prepare to deal with various challenges that commonly arise when caring for an elderly or ill person.
For more details about the program, see here. To RSVP, contact Sunrise Director of Community Relations Loretta Ressler by telephone at 972-985-9181 or by fax to 866-898-9748.
About Ms. Stamer
Cynthia Marcotte Stamer is a leader on the development of practical strategies for helping patients and their families, health care providers, employers, insurers, and others help patients and their families better handle health care and disability related challenges. The founder and President of the Project COPE: The Coalition On Patient Empowerment and author of the “Health Care Toolkit” and the many other highly regarded publications and works on patient empowerment and related matters, “Cindy” is nationally and locally recognized for her activism in developing practical solutions for common health, disability and other employment challenges for employers, insurers and others.
An AV-rated attorney Board Certified in Labor and Employment Law by the Texas Board of Legal Specialization and recognized in International Who’s Who, “Cindy” regularly helps put these and other solutions in effect in her day-to-day practice of advising health care providers, employers, health care organizations, insurers, and others about the design and implementation of patient and employee communications and consumer directed health care, patient empowerment, patient education and “patient centric” care strategies and other health care, employee benefits, disability management, human resources, insurance, and related matters.
A popular speaker nationally recognized for her legal and practical experience with patient empowerment and consumer driven health care, health care quality, and other human resources, employee benefit, and health matters, Cindy works extensively on a wide range of efforts to improve health care domestically and international. Past President and the founding Chair of the Alliance for Health Care Excellence’s Patient Empowerment Project, the current Chair of the American Bar Association (ABA) Real Property Trusts and Estate Section Employee Benefit and Other Compensation Programs Group Chair and Past Chair of the ABA Health Law Section Managed Care and Insurance Interest Group A widely published author, Cindy is the author of a diverse array of employee benefit, human resources and health law publications and tools for The Bureau of National Affairs, Aspen Publishers, the Thompson Publishing Group, and Spencer Publications. Her insights on patient empowerment and consumer directed health care have been quoted in the publications of BNA, Business Insurance, World At Work, the American Bar Association, the American Health Lawyers Association, Health Leaders, the Wall Street Journal, Aging Magazine, Spencer Publications, Health Care Report, the Dallas and Houston Business Journal, the Dallas Morning News and a host of other publications.
You can get more information about Ms. Stamer and her experiences, publications, programs, community service, and professional activities here. If you need assistance with these or concerns or wish to inquire about arranging for Ms. Stamer to speak on this or another topic, please contact Ms. Stamer at (469) 767-8872 or via e-mail here. =
About Project COPE
Project COPE works together with employers, health care providers, insurers and other payers, community leaders, patients and others to develop, educate and share practical strategies, information and tools that help empower patients to use health care resources and payers, providers and communities to provide access to quality affordable care.
The most overlooked opportunities for quality and cost improvements rests with the people in health care:
- The patients, their families and friends
- Health care providers
- Employers, churches, social organizations and other community organizations and resources that deal with patients and their families;
- Health plans, insurers, and others that administer care; and
- Others that encounter patients and their families.
The best opportunity to improve access to quality, affordable health care for every American and every employer, insurer, and community organization to understand their role in the health care system and to get and share the education and resources to make understanding and dealing with the realities of illness, disability or aging easier for a patient and their family, the affected employers and others. At the end of the day, caring for elderly, disabled or ill Americans people requires the human touch. Americans can best improve health care by not waiting for someone else to step up: Speak up, step up and help bridge the gap when you or your organization can do so by extending yourself a little bit. Speak up to help communicate and facilitate when you can. Building health care neighborhoods filled with good neighbors throughout the community is the key.
The outcome of this latest health care reform push is only a small part of a continuing process. Whether or not the Affordable Care Act makes financing care better or worse, the same challenges exist. The real meaning of the enacted reforms will be determined largely by the shaping and implementation of regulations and enforcement actions which generally are conducted outside the public eye. Americans individually and collectively clearly should monitor and continue to provide input through this critical time to help shape constructive rather than obstructive policy. Regardless of how the policy ultimately evolves, however, Americans, American businesses, and American communities still will need to roll up their sleeves and work to deal with the realities of dealing with ill, aging and disabled people and their families. While reimbursement is an important element, money is not the only issue. Improving and maintaining quality health care requires that Americans and American employers, health care providers, government and community leaders and others understand, and share education and resources to make understanding and dealing with the realities of illness, disability or aging easier for a patient and their family, the affected employers and others.
If you or someone else is interested in learning more about Project Cope, e-mail cstamer@solutionslawyer.net or register to participate in the COPE linked in group here.
To stay in touch with these and other activities and developments of Ms. Stamer, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here. For important information concerning this communication click here.
©2010 Solutions Law Press. All rights reserved.
 Comments Off on Health Care Reform: What You Need To Know To Build Your Family’s Healthcare Survival Plan |
Comments Off on Health Care Reform: What You Need To Know To Build Your Family’s Healthcare Survival Plan |  Disability Plans, Employers, ERISA, family leave, Health Plans, Human Resources, Insurance, Leave, medical leave, Patient Empowerment, Patient Protection and Affordable Care Act | Tagged: Disability Planning, Employers, Estate Planning, Health Care, Health Care Reform, Health Plans, Patient Centric, Patient Empowerment, Patients |
Disability Plans, Employers, ERISA, family leave, Health Plans, Human Resources, Insurance, Leave, medical leave, Patient Empowerment, Patient Protection and Affordable Care Act | Tagged: Disability Planning, Employers, Estate Planning, Health Care, Health Care Reform, Health Plans, Patient Centric, Patient Empowerment, Patients |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 8, 2010
Register Now For 8/24 Health Plan Update Briefing
Employer and other health plan sponsors, insurers, fiduciaries and administrators should move quickly to review, update and tighten their plan documents, administrative procedures and agreements, decisional criteria, investigation and decision-making documentation, and claims and appeals-related notification and other communications in response to new requirements and guidance in recently proposed Labor Department Regulations and the increased willingness of Federal courts to scrutinize and overturn benefit denials.
New regulations (ACA Appeals Rules) implementing tighter health plan claims and appeals rules enacted under the Patient Protection & Affordable Care Act (Affordable Care Act) are the latest in a wave of new Affordable Care Act and other federal regulations that require quick updates to employment-based health plans.
The new ACA Appeals rules published July 23, 2010 primarily focus on additional claims and appeals standards that group health plans not “grandfathered” under the Affordable Care Act must meet by the first plan year beginning after September 22, 2010. However, clarifications of the Labor Department’s interpretation of existing claims and appeals rules for employment-based group health plans shared with the ACA Appeals Rules make clear grandfathered plans also have work to do. Therefore, group health plan sponsors, insurers, fiduciaries and administrators of all group health plans should review and tighten their claims and appeals procedures in response to the guidance recently published in connection with the ACA Appeals Rules.
Beyond responding to the Labor Department’s ACA Appeals Rules, employer and other health and employee benefit plan sponsors, insurers, fiduciaries and administrators also should consider tightening and strengthening their claims and appeals decision-making, documentation and notice processes and procedures to reduce the risk that the courts will overturn benefit denials to guard against the growing willingness of federal courts to overturn benefit denials based upon their findings of process, documentation, notification, conflict of interest or other deficiencies that make the decision “arbitrary or capricious” or otherwise unsustainable under ERISA. Read more.
For assistance to review and update your health or other employee benefit claims and appeals or other terms, processes, notices and communication or other processes and procedures, please contact the author of this update, attorney Cynthia Marcotte Stamer at (469) 767-8872 or cstamer@solutionslawyer.net.
Many Other Changing Federal Rules Require Other Plan Updates
Changing claims and appeals standards are only a small part of the sweeping range of developments that employer and other plan sponsors, administrators, and fiduciaries of group health plans must deal with as the struggle to design and administer legally defensible plans this year.
The new ACA Appeals Rules are the latest in a wave of new Affordable Care Act and other federal regulations that require quick action by employment based health plans, their employer and other sponsors, fiduciaries, administrators and insurers. Regulations issued in previous weeks define when health plans and health insurance policies qualify as “grandfathered” under the Affordable Care Act and interpret and implement many other federal health plan rule changes enacted by the Affordable Care Act.
All employer and other group health plan sponsors, fiduciaries, insurers and administrators should be prepared to act quickly to update their health plan documents, communications, insurance and vendor agreements and other practices to comply with new federal requirements that become effective under the Affordable Care Act on the first day of the plan year beginning after September 22, 2010 and various other changes in federal health plan rules effective or scheduled to take effect during 2010 or 2011 plan years. Many plan sponsors also may need to act quickly to cancel or revise certain design or vendor changes planned or already implemented since March 23, 2010 to position their health plan to qualify for grandfather status. Quick action also may be needed to preserve options to claim small employer tax credits, retiree medical subsidies or other opportunities.
In addition to responding to these Affordable Care Act changes, most group health plans also will require updates in response to other federal health plan rule changes beyond those enacted under the Affordable Care Act. These Affordable Care Act and other impending federal health plan changes will require employment-based group health plans, their employer and other plan sponsors, plan fiduciaries, plan administrators and other service providers and insurers to make quick decisions and to act quickly to meet impending federal compliance deadlines while preserving flexibility and managing costs.
August 24 “2010 Health Plan Update” Internet Workshop Provides Key Information
Solutions Law Press invites you to catch up on the latest guidance about the new group health plan Affordable Care Act and other federal health plan regulations by participating in a live “2010 Health Plan Update” internet broadcast briefing on Tuesday, August 24 2010. The briefing will be conducted via live video broadcast from 11:00 A.M.-1:30 P.M. Central Time. Register & Get More Details.
Learn the tests that will decide if your group health plan will qualify as “grandfathered” from key Affordable Care Act requirements and assess what updates you should consider making to meet critical 2010/2011 Affordable Care Act & other federal health plan compliance deadlines.
The August 24, 2010 “2010 Health Plan Update” briefing will cover the latest guidance on Affordable Care Act and other federal health plan regulatory changes impacting employment-based group health plans and their sponsors for plan years beginning between September 23, 2010 and September 22, 2011 and other key information to help employers, group health plans, insurers, plan administrators, fiduciaries, broker and others working with these plans to understand and respond to these new requirements including:
- How to qualify your health plan as a grandfathered plan under Affordable Care act
- How to decide if maintaining grandfathered plan status is worthwhile
- Claims & appeals requirements for grandfathered & non-grandfathered plans
- Preventive care coverage mandates & wellness program requirements & rules under Affordable Care Act & other federal regulations
- Updated dependent child eligibility, pre-existing condition & other requirements for grandfathered & non-grandfathered plans
- Special enrollment, preexisting condition & other eligibility mandates for grandfathered & non-grandfathered plans under new Affordable Care Act, new FMLA, COBRA, Michelle’s Law, HIPAA & other federal regulations
- Mental health & substance abuse, provider choice & other benefit mandates under Affordable Care Act, Mental Health Parity & other federal rules
- Update on other recent & pending Affordable Care Act group health plan rule guidance
- Tips to review & update your plans, vendor agreements & processes to meet Affordable Care Act & other federal group health plan dictates
- Expected future Affordable Care Act & other federal rule changes & tips for preparing
- Practical strategies for responding to new requirements & changing rules
- Participant questions
To register or get additional information, see here.
For Assistance or More Information
If your organization needs assistance updating your heath care program documentation, policies or procedures in response to these or other requirements or with other employee benefit, insurance or human resources matters, please contact the author of this update, Board Certified Labor & Employment attorney Cynthia Marcotte Stamer at (469) 767-8872 or via e-mail here.
Current Chair of the American Bar Association (ABA) RPTE Employee Benefit & Other Compensation Group, a Council Member of the ABA Joint Committee on Employee Benefits and Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, Ms. Stamer continuously advises employers, health and other employee benefit plans, plan sponsors, fiduciaries, plan administrators, plan vendors, insurers and others about health program related legal, operational, documentation, public policy, enforcement, privacy, technology, litigation and risk management and other concerns. Ms. Stamer also publishes, conducts client and other training, speaks and consults extensively on these and other health and managed care program concerns and practices. She regularly speaks and conducts training for the ABA, American Health Lawyers Association, Institute of Internal Auditors, Society for Professional Benefits Administrators, Southwest Benefits Association and many other organizations. Her insights on these and related topics have appeared in Atlantic Information Service, Bureau of National Affairs, World At Work, The Wall Street Journal, Business Insurance, Managed Healthcare, Health Leaders, various ABA publications and a many other national and local publications. To contact Ms. Stamer or for additional information about Ms. Stamer, her experience, involvements, programs or Publishers of her many highly regarded writings on health industry and human resources matters include the Bureau of National Affairs, Aspen Publishers, ABA, AHLA, Aspen Publishers, Schneider Publications, Spencer Publications, World At Work, SHRM, HCCA, State Bar of Texas, Business Insurance, James Publishing and many others. You can review other highlights of Ms. Stamer’s experience here.
Other Resources
If you found this information of interest, you also may be interested in reviewing other recent Solutions Law Press updates including:
About Solutions Law Press
Solutions Law Press™ provides business risk management, legal compliance, management effectiveness and other resources, training and education on human resources, employee benefits, compensation, data security and privacy, health care, insurance, and other key compliance, risk management, internal controls and other key operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press resources available for review here. If you or someone else you know would like to receive future updates and notices about other upcoming Solutions Law Press events, please be sure that we have your current contact information – including your preferred e-mail- by creating or updating your profile at here. For important information concerning this communication click here.
©2010 Solutions Law Press. All rights reserved.
 Comments Off on New Regulations & Court Decisions Require Health Plan Claims & Appeal Updates & Strengthening |
Comments Off on New Regulations & Court Decisions Require Health Plan Claims & Appeal Updates & Strengthening |  Affordable Care Act, Claims Administration, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Preemption, Reporting & Disclosure | Tagged: Affordable Care Act, Appeals, Claims, ERISA, Health Plans |
Affordable Care Act, Claims Administration, Disability Plans, Employee Benefits, Employers, ERISA, Fiduciary Responsibility, Health Plans, Human Resources, Insurance, Preemption, Reporting & Disclosure | Tagged: Affordable Care Act, Appeals, Claims, ERISA, Health Plans |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 19, 2010
Employers and employee benefit plan administrators deciding whether to approve the request of an employee for leave or other rights under the Family and Medical Leave Act (FMLA) due to the serious illness, birth, adoption or placement of a child with no legal or biological relationship with the employee should not underestimate the scope of the FMLA’s reach based on recent guidance. Employers and plan administrators also need to be sure that their policies are properly drafted and administered to apply right definition of child based on the class of leave requested as the family-status-relevant definitions under the FMLA and other laws continue to proliferate.
Recent Department of Labor Wage & Hour Division Wage and Hour Division (WHD) guidance reveals the WHD adopts a very broad view of the circumstances under which a when a child with no legal or biological relationship to an employee can qualify as a “son or daughter” for purposes of determining rights of the employee under the FMLA based on the birth , adoption, placement for adoption or need to care for the child during a serious illness and a narrow view of the documentation that an employer may require an employee to provide to prove such a relationship exists.[i]
Background
The FMLA entitles an employee to 12 work weeks of leave for the birth or placement of a son or daughter, to bond with a newborn or newly placed son or daughter, or to care for a son or daughter with a serious health condition.[ii]
The definition of “son or daughter” under the FMLA includes not only a biological or adopted child, but also a “foster child, a stepchild, a legal ward, or a child of a person standing in loco parentis” who is either:
- Under 18 years of age; or
- 18 years of age or older and incapable of self-care because of a mental or physical disability.”[iii]
In Loco Parentis
The FMLA regulations define in loco parentis as including those relationships between an employee and a child where the facts and circumstances show that the employee has undertaken day-to-day responsibilities to care for and financially support a child.[iv]
Administrator’s Interpretation No. 2010-3 (June 22, 2010) (WHD Interpretation) clarifies the definition of “son or daughter” under Section 101(12) of the FMLA as it applies to an employee standing “in loco parentis” to a child taking FMLA-protected leave for the birth or placement of a child, to care for a newborn or newly placed child, or to care for a child with a serious health condition. The WHD Interpretation does not address an employee’s entitlement to take military FMLA leave for a son or daughter, which is determined by separate definitions.
The WHD Interpretation states that the FMLA does not require an employee who intends to assume the responsibilities of a parent to prove that he or she provides both day-to-day care and financial support to be found to stand in loco parentis to a child.
According to the WHD Interpretation, the determination of when an employee has an in loco parentis relationship with a child is fact specific question based on the facts and circumstances with no particular factor being dispositive. . The WHD Interpretation adds that the fact that a child has a biological parent in the home, or has both a mother and a father, does not prevent a finding that the child is the “son or daughter” of an employee who lacks a biological or legal relationship with the child for purposes of taking FMLA leave.
“The key in determining whether the relationship of in loco parentis is established is found in the intention of the person allegedly in loco parentis to assume the status of a parent toward the child. The intent to assume such parental status can be inferred from the acts of the parties” taking into account a variety of factors including the age of the child; the degree to which the child is dependent on the person claiming to stand in loco parentis; the amount of support, if any, provided; and the extent to which duties commonly associated with parenthood are exercised.
Noting Congress intended the phrase “in loco parentis” to ensure that an employee who actually has day-to-day responsibility for caring for a child is entitled to leave even if the employee does not have a biological or legal relationship to that child, the WHD Interpretation states the phrase is commonly understood to refer to “a person who has put himself in the situation of a lawful parent by assuming the obligations incident to the parental relation without going through the formalities necessary to legal adoption. It embodies the two ideas of assuming the parental status and discharging the parental duties.”
Applying these principles, the WHD Interpretation identifies various situations where the WHD perceives that relationship in loco parentis might exist for purposes of the FMLA based on the assumption of the employee of either responsibility to care for a child or financial responsibility for the child in the absence of a biological or legal relationship including:
- Where an employee provides day-to-day care for his or her unmarried partner’s child (with whom there is no legal or biological relationship) but does not financially support the child;
- Where an employee who will share equally in the raising of a newborn or adopted child with the child’s biological parent;
- Where a grandparent takes in a grandchild and assumes ongoing responsibility for raising the child because the parents are incapable of providing care,;
- Where an aunt assumes responsibility for raising a child after the death of the child’s parents.
In contrast, the WHD Interpretation notes that an employee who cares for a child while the child’s parents are on vacation would not be considered to be in loco parentis to the child.
When determining whether to approve a FMLA Leave request of an employee seeking time off due to the birth, adoption, placement for adoption or serious illness of a child with whom the employee has no biological or legal relationship, the WHD Interpretation makes clear that the WHD construes the phrase “in loco parentis” broadly. Furthermore, the WHD Interpretation also signals the need for employers to exercise caution when requiring documentation of the existence of such a claimed relationship. While acknowledging that the FMLA allows an employer to require an employee claiming a relationship in loco parentis with child to require the employee to provide reasonable documentation or statement of the family relationship, the WHD Interpretation raises questions about the degree of documentation that the employer may require. According to the WHD Interpretation, “[a] simple statement asserting that the requisite family relationship exists is all that is needed in situations such as in loco parentis where there is no legal or biological relationship.”[v]
Drafting Policies & Using the Right Standard for the Right Circumstances
When drafting and applying FMLA and other legally mandated policies, it’s important that employers, employee benefit plan sponsors and administrators and others use the correct standard for the circumstance prevented. The FMLA definition of child from the WHD Interpretation applies only to determinations of the status of a person as a son or daughter for purposes of the FMLA’s leave provisions regarding leaves requested due to the serious illness, birth or adoption of a child of an employee and not for military related FMLA leaves. Different standards apply for military related FMLA leaves. Similarly, the standards used to determine who qualifies as a child for purposes of FMLA may not necessarily be the same as legally required to decide when an individual qualifies as a child for other legal purposes. For instance, recent changes to federal health plan rules enacted as part of the Patient Protection & Affordable Care Act may require that group health plans and insurers use different standards to decide when an individual qualifies for enrollment as the child of an employee in dependent coverage beyond those applicable under the FMLA. It is highly advisable that employers and employee benefit plan sponsors and administrators carefully review and update their existing policies, plan documents and practices for compliance with the appropriate and currently applicable standards and exercise care in the administration of these practices to avoid costly mistakes.
About the Author
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, management attorney and consultant Ms. Stamer has more than 23 years experience working with employers, professional employment organizations, employee benefit plan sponsors and administrators and others on a wide range of labor and employment, employee benefits, and other management matters. The Chair of the American Bar Association (ABA) RPTE Employee Benefits & Other Compensation Committee, a Council Representative on the ABA Joint Committee on Employee Benefits, Government Affairs Committee Legislative Chair for the Dallas Human Resources Management Association, the editor of Solutions Law Press HR & Benefits Update and, Ms. Stamer also is recognized for her publications, industry leadership, workshops and presentations on these and other health industry and human resources concerns. She regularly speaks and conducts training for the ABA, Institute of Internal Auditors, Society for Professional Benefits Administrators, Southwest Benefits Association and many other organizations. Publishers of her many highly regarded writings on health industry and human resources matters include the Bureau of National Affairs, Aspen Publishers, ABA, AHLA, Aspen Publishers, Schneider Publications, Spencer Publications, World At Work, SHRM, HCCA, State Bar of Texas, Business Insurance, James Publishing and many others. You can review other highlights of Ms. Stamer’s experience here.
If you need help with human resources or other management, concerns, wish to ask about compliance, risk management or training, or need legal representation on other matters please contact Cynthia Marcotte Stamer here or (469)767-8872.
Other Resources
If you found this information of interest, you also may be interested in reviewing other recent Solutions Law Press updates including:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information – including your preferred e-mail – by creating or updating your profile here or e-mailing this information here or registering to receive our Solutions Law Press distributions here. For important information about this communication click here. If you do not wish to receive these updates in the future, send an e-mail with the word “Remove” in the Subject to here.
©2010 Solutions Law Press. All rights reserved.
[i] See 29 C.F.R. § 825.122(g), (h).
[ii] See 29 U.S.C. § 2612(a)(1)(A) – (C); 29 C.F.R. § 825.200.
[iii] 29 U.S.C. § 2611(12). See also 29 C.F.R. §§ 825.122(c), 825.800.[1].
[iv] 29 C.F.R. § 825.122(c)(3).
[v] See 29 C.F.R. § 825.122(j); 73 Fed. Reg. 67,952 (Nov. 17, 2008).
 Comments Off on Labor Department FMLA Guidance Signals Need For Employer Care Determining Who Qualifies As Child |
Comments Off on Labor Department FMLA Guidance Signals Need For Employer Care Determining Who Qualifies As Child |  Disability Plans, Employee Benefits, Employers, family leave, FMLA, Health Plans, Human Resources, Insurance, Internal Controls, Leave, medical leave | Tagged: adoption, child, Family Leave, FMLA, medical leave, placement for adoption, serious medical condition |
Disability Plans, Employee Benefits, Employers, family leave, FMLA, Health Plans, Human Resources, Insurance, Internal Controls, Leave, medical leave | Tagged: adoption, child, Family Leave, FMLA, medical leave, placement for adoption, serious medical condition |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer



 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer 

You must be logged in to post a comment.