January 10, 2018
Employer and sponsors, fiduciaries, administrators and insurers of employee benefitplansof any type covered by the Employee Retirement Income Security Act (ERISA) making any disability based determinations now have until April 1, 2018 to bring their plans’ claims and appeals procedures for disability-based decisions and related notices and communications into compliance with substantially more complicated requirements in new Department of Labor Employee Benefit Security Administration (EBSA) regulations.
The EBSA announced on January 5, 2018 the extension of the effective date of new requirements for benefit plan processing and providing notification about claims or appeals involving disability determinations from their originally scheduled effective date of January 1, 2018 to April 1, 2018.
While the extension gives employer and other sponsors, fiduciaries, administrators and insurers of employee benefit plans making disability-based benefit determinations a few extra months to review and update their plan documents, summary plan descriptions, procedures, processes and claims and appeals notices to meet tightened new federal rules on disability-based benefit determinations applicable to all post December 31, 2017 claims under the restated Final Rule on Claims Procedure for Plans Providing Disability Benefits (“Disability Claims Rule”), the nature and scope of these new requirements will require updates to virtually all ERISA-covered benefit plans with any disability dependent provisions. These updates are likely to include changes to plan documents, summary plan descriptions, notices, contracts, processes and procedures for a broad range of plans. Consequently, employer and other plan sponsors, fiduciaries, administrators, insurers and others responsible for any benefit plan not already reviewed and updated to comply should get moving to complete the necessary review and update to meet the April 1, 2018 deadline.
Cynthia Marcotte Stamer and others will lead a free telephone study group discussion of “Claims Regulations and Other Developments Affecting Plan Fiduciaries” on January 26, 2018 beginning at 1 PM (Eastern), Noon (Central), 11 AM (Mountain), and 10 AM (Pacific). For more details about the Study Group, see here.
New Disability Claims Rule Overview
Originally published in final form by the EBSA on December 16, 2016, the Disability Claims Rule generally require all ERISA-covered employee benefit plans making any disability benefit or other determination conditioned upon a finding of disability to comply with the new Disability Claims Rule for any claim received after March 31, 2018.
Based on EBSA’s previously adopted Patient Protection and Affordable Care Act (“ACA”) group health plan claims and appeals rules, the new Final Disability Claims Rule will apply to all disability determinations made under any ERISA-covered plan after March 31, 2018, regardless of how the plan characterizes the benefit or whether the plan is a health or other welfare, pension, 401(k) plan or other savings plan.
The new Disability Claims Rule will apply to a broad range of plans, most of which historically have not followed the detailed claims and appeals notification, independent and impartial decision-making, rescission, deemed exhaustion, “culturally and linguistically appropriate” and other procedural protections and safeguards that the Disability Claims Rule extends from the current group health plan rules to all ERISA-covered plans making benefit determinations based on disability. Consequently covered plans making disability-based benefit or other covered determinations are likely to require updates to plan documents, insurance or administrative services contracts, summary plan descriptions and other plan communications, claims and appeals notices, and other related processes, procedures and documentation to meet these new requirements. Since certain requirements of the Disability Claims Rules like the summary plan description advance disclosure requirements are required to be provided before the claim is received, plans and their sponsors, fiduciaries, insurers and administrators risk being accused of violating these requirements by waiting to update plans, their processes and materials until after claim involving a disability based determination arises.
Ensuring that impacted plans are updated before the April 1, 2018 deadline is important because the Disability Claims Rule, like the group health plan claims and appeals rules upon which it is based, also states that noncompliance with any of its requirements empowers a participant to immediately sue the plan for enforcement if his rights without further complying the the plan’s administrative procedures. Moreover, failing to comply with summary plan disclosure or claims or appeal adverse benefit determination notification requirements also may subject the plan administrator to administrative penalties under ERISA section 514(c); fiduciaries to ERISA fiduciary liability, and compromise the ability to defend otherwise defensible decisions. Consequently, employers and other plan sponsors, fiduciaries, administrators and insurers will want to act quickly to ensure that their plans, their summary plan descriptions and other communications, notices, processes, contracts and procedures are updated appropriately before April 1, 218.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation; Former Chair of the RPTE Employee Benefits and Compensation Committee, a current Co-Chair of the Committee, and the former Chair of its Welfare Benefit and its Defined Compensation Plan Committees and former RPTE Joint Committee on Employee Benefits Council (JCEB) Representative, Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent” practicing attorney and management consultant, author, public policy advocate, author and lecturer repeatedly recognized for her 30 plus years’ of work and pragmatic thought leadership, publications and training on health, pension and other employee benefit, insurance, labor and employment, and health care fiduciary responsibility, payment, investment, contracting and other design, administration and compliance concerns as among the “Top Rated Labor & Employment Lawyers in Texas,” a “Legal Leader,” a “Top Woman Lawyer” and with other awards by LexisNexis® Martindale-Hubbell®; as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,” “Tax: ERISA & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, in International Who’s Who of Professionals and with numerous other awards and distinctions.
Highly valued for her ability to meld her extensive legal and industry knowledge and experience with her talents as an insightful innovator and pragmatic problem solver, Ms. Stamer advises, represents and defends employer, union, multi-employer, association and other employee benefit plan sponsors, insurers and managed care organizations, fiduciaries, plan administrators, technology and other service providers, government and community leaders and others about health and other employee benefit and insurance program and policy design and innovation, funding, documentation, administration, communication, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management, compliance and operations matters. Her experience encompasses leading and supporting the development and defense of innovative new policies, programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations; crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, Securities and Exchange Commission, Education and other federal agencies, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, and various other foreign and domestic governmental bodies and agencies. She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness. Alongside her extensive legal and operational experience, Ms. Stamer also is recognized for her work as a public and regulatory policy advocate and community leader with a gift for finding pragmatic solutions and helping to forge the common ground necessary to build consensus. Best known for her domestic public policy and community leadership on health care and insurance reform, Ms. Stamer’s lifelong public policy and community service involvement includes service as a lead consultant to the Government of Bolivia on its pension privatization project, as well as extensive legislative and regulatory reform, advocacy and input workforce, worker classification, employee benefit, public health and healthcare, social security and other disability and aging in place, education, migration reforms domestically and internationally throughout her adult life. In addition to her public and regulatory policy involvement, Ms. Stamer also contributes her service and leadership to a professional and civic organizations and efforts including her involvement as the Founder and Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence; Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; Vice Chair, Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group; current Fiduciary Responsibility Committee Co-Chair and Membership Committee member of the ABA RPTE Section; former RPTE Employee Benefits and Other Compensation Group Chair, former Chair and Co-Chair of its Welfare Plans Committee, and Defined Contribution Plans Committee; former RPTE Representative to ABA Joint Committee on Employee Benefits Council; former RPTE Representative to the ABA Health Law Coordinating Counsel; former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former Board Member, Continuing Education Chair and Treasurer of the Southwest Benefits Association; Vice President of the North Texas Healthcare Compliance Professionals Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; past Dallas World Affairs Council Board Member, and in leadership of many other professional, civic and community organizations. Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other public policy advocacy and other professional and civic organizations and involvements. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
Before founding her current law firm, Cynthia Marcotte Stamer, P.C., Ms. Stamer practiced law as a partner with several prominent national and international law firms for more than 10 years before founding Cynthia Marcotte Stamer, P.C. to practice her unique brand of “Solutions law™” and to devote more time to the pragmatic policy and system reform, community education and innovation, and other health system improvement efforts of her PROJECT COPE: the Coalition on Patient Empowerment initiative.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |
Comments Off on April 1 New Deadline To Update Benefit Plan Disability Determination Claims & Appeals Procesures; Hear More on 1/26 |  401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |
401(k), ACA, Accommodation, Civil Rights, Claims Administration, COBRA, compensation, compliance, Corporate Compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, Disease Management, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Executive Compensation, family leave, fiduciary duty, Fiduciary Responsibility, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Labor Management Relations, medical leave, Mental Health, Patient Empowerment, pension plan, Prescription Drugs, Reporting & Disclosure, Retirement Plans, Retirements, Uncategorized, Union, Wellness Programs |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 7, 2018
Arizona legislators are considering adopting legislation banning and rendering unenforceable agreements by employers or others to keep confidential or otherwise restrict the disclosure of allegations or other information about sexual harassment or sexual assault. If enacted as proposed, the proposed legislation could significantly impact employers, sexual harassment and sexual assault victims and witnesses, persons accused of sexual assault or harassment and others’ ability to negotiate, enforce or comply with provisions in new or preexisting employment policies, and settlement, severance and other agreements requiring confidentiality of or restricting disclosure of information about findings or allegations of sexual harassment or assault and related factual information.
As currently proposed, Arizona House Bill 2020 (HB 2020) would amend Section 1. Title 12, chapter 6, article 12, Arizona Revised Statutes, to include add a new section 12-720 that would read as follows
12-720. Confidentiality agreements; disclosure of information relating to sexual assault or sexual harassment; applicability
A. A CONFIDENTIALITY AGREEMENT THAT RESTRICTS THE DISCLOSURE OF FACTUAL INFORMATION THAT IS RELATED TO A SEXUAL ASSAULT OR SEXUAL HARASSMENT, INCLUDING FACTUAL INFORMATION THAT IS RELATED TO AN ALLEGATION OF OR ATTEMPTED SEXUAL ASSAULT OR SEXUAL HARASSMENT, IS AGAINST THIS STATE’S PUBLIC SAFETY AND POLICY AND IS VOID AND UNENFORCEABLE.
B. A PERSON MAY NOT ENTER INTO A CONFIDENTIALITY AGREEMENT THAT RESTRICTS THE DISCLOSURE OF FACTUAL INFORMATION THAT IS RELATED TO AN ALLEGATION OF OR ATTEMPTED SEXUAL ASSAULT OR SEXUAL HARASSMENT BY AN ELECTED OFFICIAL.
C. THIS SECTION DOES NOT APPLY TO THE DISCLOSURE OF A MINOR CRIME VICTIM’S MEDICAL OR PERSONAL IDENTIFYING INFORMATION OR TO OTHER INFORMATION THAT IS SPECIFICALLY PROTECTED FROM DISCLOSURE BY LAW.
Based on this currently proposed language, enactment of HB 2020’s sexual harassment and assault confidentiality restrictions almost certainly will dramatically impact both the financial, reputation and legal liability exposures of individuals accused of sexual harassment or assault and their employers or others potentially responsible for the investigation, management or liability for the alleged harasser’s behavior, behavior, as well as the privacy, retaliation and other concerns of sexual harassment or assault victims and witnesses. Certainly, HB 2020 would preclude or limit the ability of executives or other individuals accused of sexual harassment or assault from hiding their isolated or recurrent actual or alleged misconduct behind confidentiality or nondisclosure provisions in settlement or other contracts, handbooks, investigation, compliance or other policies. Likewise, HB 2020’s prohibitions against agreements requiring the maintenance of confidentiality of information about alleged or actual sexual harassment or assaults also can be expected to make it more difficult for employers to defend or mitigate their exposure to liability for alleged sexual harassment or assaults by making it much easier for alleged victims, their attorneys and the Equal Employment Opportunity Commission and other government agencies to investigate and obtain evidence about the conduct of the accused and the actions of his or her employer to other events or charges of sexual harassment or assault. Among other things, more free availability of this information is likely to make it easier for sexual harassment or assault victims, their plaintiff’s lawyers and the EEOC or other agencies and advocates to uncover, pursue enforcement and recover damages from employers through individual, class action or serial sexual harassment investigations and lawsuits as well as to rebut efforts of employers and those accused to mitigate damages and other liability.
While many might celebrate these expected effects of HB 2020 in helping to hold harassers and their employers more accountable for misconduct and to safeguard others from becoming future victims, HB 2020 also carries the risk of a number of potentially undesirable side effects for sexual harassment and assault victims and witnesses, employer and other investigators and those wrongfully accused. Because victims and witnesses to sexual harassment often fear embarrassment, retaliation or other adverse consequences from their report or involvement in a charge or investigation, sexual harassment and other policies and the employers and others responsible for administering and enforcing sexual harassment policies typically offer assurances of confidentiality and other nondisclosure to encourage and reassure victims and witnesses to report concerning behavior and to help prevent retaliation against victims and witnesses reporting or cooperating in sexual harassment and assault investigations. While HB 2020 includes a provision that appears intended to preserve the confidentiality of the identity and medical information of victims, the technical concealment of names and medical information as a practical matter generally provides an inadequate shield for victims or witnesses when other information otherwise remains discoverable. Consequently, confidentiality restrictions like those proposed in HB 2020 could backfire against these victims and witnesses and employers legitimately working to protect them by enhancing victim and witness reluctance to report or cooperate in sexual harassment investigations as well as inflict substantial and irreversible injury upon the personal and professional reputations of individuals wrongfully accused. The confidentiality prohibitions of HB 2020 are likely to undermine the ability of employers, victims and witnesses to use confidentiality requirements legitimately to prevent unjustified retaliation, loss of privacy and other adverse consequences to victims, witnesses and those wrongfully accused. Likewise, restrictions on confidentiality also can be expected to undermine the ability of victims to secure compensation from guilty parties and their employers without litigation as accused parties and their employer as the inability to enforce confidentiality will undermine the settlement value of questionable charges by enhancing the potential need to dispute and defend such charges to avoid becoming targeted by other accusations concurrently or in the future.
Obviously, these and other potential implications of HB 2020 make it highly advisable that businesses, management, individuals, insurers and others potentially subject to HB 2020 will want to carefully assess the implications of HB 2020 and provide input to the Arizona legislature. Given the wave of recent publicity triggered over the past year from widespread reporting of sexual harassment and related charges and resulting resignations and lawsuits and settlements involving sexual harassment charges levied against high profile entertainers, business leaders and others, employers, management and business leaders, victims, witnesses, insurers and other operating outside the jurisdiction of Arizona law can anticipate that they also may face similar legislative, regulatory or other challenges to confidentiality and nondisclosure policies and agreements concerning sexual harassment and assault allegations, investigations and settlements. Because of these and other concerns, employers, victims, witnesses, investigators, insurers and others with responsibility for or involvement with sexual harassment and assault concerns across the nation should both carefully monitor these developments as well as the reliability and effectiveness of their past and existing sexual harassment, investigations, anti-retaliation, confidentiality and other related policies, confidentiality and nondisclosure provisions in settlement agreements, and other potentially impacted agreements, policies and practices. Employers and other individuals or organizations in the scope of potential liability for sexual harassment or assault charges also may wish to consider strengthening existing anti-harassment policies, investigation practices, insurance coverage and other prevention and risk management arrangements to mitigate their sexual harassment risks.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes including extensive involvement for more than providing training for management and others and helping management, liability insurers and others to develop, administer, enforce, defend and mitigate sexual harassment and other related employment risks.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on sexual harassment and other human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns, who has received high praise for workshops and training programs she conducts on “What To Do When Your Employee’s Personal Life Becomes Your Business,” “Sex, Drugs & Rock ‘N Role in the Workplace,” and other sexual harassment, investigations, privacy and related programs for SHRM, the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2018 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author. directly. All other rights reserved
 Comments Off on Arizona Proposal To Ban Sexual Harassment Confidentiality Agreements Sign Of Growing Employer Risks |
Comments Off on Arizona Proposal To Ban Sexual Harassment Confidentiality Agreements Sign Of Growing Employer Risks |  directors, EEOC, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Discrimination, Employment Policies, ERISA, Excise Taxes, Executive Compensation, Exempt, Human Resources, OFCCP, Rehabilitation Act, Retaliation, Safety, Sexual Harassment, Uncategorized |
directors, EEOC, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Discrimination, Employment Policies, ERISA, Excise Taxes, Executive Compensation, Exempt, Human Resources, OFCCP, Rehabilitation Act, Retaliation, Safety, Sexual Harassment, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 5, 2018
Continuing Fallout of 2015 Data Breach Provides Many Lessons For Other Businesses & Their Health Plans
Read the rest of this entry »
 Comments Off on $23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses |
Comments Off on $23M Penalty Small Part of 21st Century’s Data Breach Fallout; Offers Data Breach Lessons For Other Businesses |  ADA, Association Health Plan, Banking, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Claims Administration, compensation, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Excise Taxes, FACTA, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Breach, HIPAA, Identity Theft, Privacy, Technology |
ADA, Association Health Plan, Banking, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Claims Administration, compensation, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, ERISA, Excise Taxes, FACTA, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Breach, HIPAA, Identity Theft, Privacy, Technology |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 18, 2017
Want to know what tax changes are included in the Tax Cuts and Jobs Act (H.R. 1) (Act”) and expected to pass Congress tomorrow (December 20, 2017)? Check out the House Conference Committee Report, H. Rept. 115-466 (the “Conference Report”) released on Friday, December 15, 2017.
The House Conference Committee Report details the negotiated reconciliation of House Bill (H.R. 1) as passed by the House of Representatives on November 16, 2017 and the provisions of H.R. 1 with amendments passed by the Senate on December 2, 2017. Over the past few weeks, a joint committee made up of key representatives from the House and Senate have engaged in highly publicized negotiations to reconcile differences in the House and Senate versions of the Act. The House Conference Committee Report signed off by the Conference Committee and filed in the House of Representatives of December 15, 2017 documents the agreements reached by House and Senate Conferees reconciling the House and Senate versions of H.R. 1, which Congress will vote upon this week. Solutions Law Press, Inc. will publish analysis of various provisions of these reforms over the next few days. In the meantime, taxpayers interested in learning about the Act may use the links in this article to begin familiarizing themselves with its provisions.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses work with domestic and international businesses of all types and sizes as well as extensive work with Congress and U.S. federal and state regulatory agencies on workforce, compensation and benefits, and performance and operational compliance challenges. A primary drafter of the Bolivian Pension Privitization law who also has worked on workforce, tax, employee benefits, health care, insurance, safety, immigration, privacy and data security and other federal and state legal reforms domestically and internationally throughout her adult life, Ms. Stamer also has been extensively involved in various aspects of Congressional considerations of the current Act and other legislation considered by the current Congress.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations, for clients and others.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source |
Comments Off on Read Tax Cuts and Jobs Act Conference Report For Tax Reform From Source |  105(h), 401(k), 5000, Cafeteria Plans, church plan, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Agreement, Employment Tax, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Income Tax, Insurance, insurers, IRC, Management, Obamacare, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, pension plan, Premium Subsidies, retirement plan, Retirement Plans, Risk Management, Social Security, Tax, Tax Credit, Tax Qualification, Uncategorized | Tagged: tax reform, Taxes |
105(h), 401(k), 5000, Cafeteria Plans, church plan, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Agreement, Employment Tax, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HR, Human Resources, Income Tax, Insurance, insurers, IRC, Management, Obamacare, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, pension plan, Premium Subsidies, retirement plan, Retirement Plans, Risk Management, Social Security, Tax, Tax Credit, Tax Qualification, Uncategorized | Tagged: tax reform, Taxes |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 18, 2017
Employers, employee benefit plan sponsors and administrators, vendors and their advisors and service providers should re-evaluate their existing payroll and other settings and elections, planning, testing and related strategies and assumptions in light of the 2018 annual cost-of-living adjustments (COLAs) to the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits announced by the Internal Revenue Service (IRS) in Notice 2017-64, IRB 2017-45 on November 6, 2017.
H.R. 1, Tax Cuts and Jobs Act (Tax Refirm Bill) reported out of the Conference Committee last week and scheduled for a vote before Congress tomorrow leaves these limits substantially unchanged.
Notice 2017-64 adjusts the dollar limitations applicable to the Internal Revenue Code Section 415 qualified retirement plans benefit and contribution limits. The Section 415 limitations COLAs are made and published annually to comply with Section 415(d)’s requirement that the Treasury Security annually adjust these limits for cost-of-living increases. Other limitations applicable to deferred compensation plans are also affected by these adjustments under § 415. Under § 415(d), the adjustments are to be made under adjustment procedures similar to those used to adjust benefit amounts under § 215(i)(2)(A) of the Social Security Act.
In addition to impacting contribution limits permitted to defined benefit, 401(k) and other defined contribution and other plans, the changes can impact the definition of highly compensated employees, discrimination testing, plan funding and a broad range of employee benefit, compensation, tax, payroll, union or other contracting and other concerns for employers, employee benefit plan sponsors, fiduciaries, administrators, payroll, plan and other vendors, participants and beneficiaries and others.
The following is a chart of the adjusted limits compared to the currently applicable 2017 limitations. (Download chart)
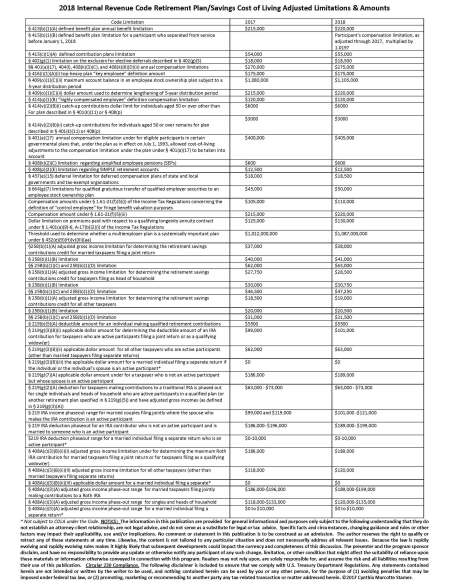
Employers, employee benefit plan sponsors, fiduciaries, administrators and other vendors, participants and beneficiaries and others working with employee benefit plans or compensation contributed to these arrangements should review these new 2018 COLA limitations to assess their potential impact and make appropriate adjustments to avoid compliance challenges or other unfortunate surprises in 2018. If they already have not already done so, reviewing the 2018 Social Security Act COLAs also would be wise. See 2018 Social Security COLAs Set.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |
Comments Off on Check How IRS 2018 Retirement & Saving Plan Limits and Amounts Cost Of Living Adjustments Impact Your HR & Retirement Plan Administration & Planning |  401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |
401(k), Association Health Plan, Brokers, compensation, compliance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, Disability, Disability Plans, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Taxes, Form 5500, Health Plans, HR, Human Resources, Internal Revenue Code, IRC, Labor Management Relations, Management, Pay, pension plan, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Salaried, Tax, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 13, 2017
 Teamwork is a valuable and necessary to organizational performance in most workplaces. However management undermines team performance and effectiveness by giving participation trophies to team members that don’t give their best when working on teams.
Teamwork is a valuable and necessary to organizational performance in most workplaces. However management undermines team performance and effectiveness by giving participation trophies to team members that don’t give their best when working on teams.
Managements goal at all-time should be to maximize the effectiveness of the team by encouraging and require each individual team member to contribute their best on the team.
Overemphasizing team work at the expense of individual performance accountability, however, undermines team performance by disincentivizing optimal performance by every team member. Optimal management and performance rewards ensure that each individual member of the team remains accountable for optimizing his or her individual performance while encouraging effective participation on the team. To maintain individual performance within the team, ensure your expectations and performance measures track not only team performance but also individual performance on the team. Measure and award teamwork by individual members of the team as one of the performance measures rather than making teamwork itself at the expense of the performance goals the basis of the reward.
Check out this coach’s perspective for more food for thought.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪DOL Proposes Changing FLSA Tipped Employee Pay Rules
▪Consider Internal Investigation & Defense Costs When Administering Compliance Programs
▪Recruiting Qualified Workers Biggest Challenge US Manufacturers See In Otherwise Optimistic 3rd Quarter 2017
▪Government Retirees Get New Thrift Plan Distributing Choices
▪Jennifer A. Abruzzo Named NLRB Acting General Counsel
▪Bill Mandating E-Verify, Raising Employer I-9 Penalties Approved By House Judiciary Committee
▪Address Workplace Harassment During October Stop Bullying Month
▪NIOSH Proposed Updated Occupational Safety Chemical Monitoring Rules
▪2018 Social Security COLAs Set
▪IRS Updates Defined Benefit Plan Guidance
▪Read Trump Health Care Executive Order
▪Dealing With HR, Benefits & Other Headaches From Equifax and Other Data Breach
▪Employers Should Manage Potential Unfair Labor Practice Risks From Recording, Acceptable Use, Fighting, Integrity & Other Employment Policies
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved
 Comments Off on Individual Accountability For Performance Matters |
Comments Off on Individual Accountability For Performance Matters |  compensation, compliance, Corporate Compliance, corporate governance, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, Executive Compensation, Hiring, HR, Human Resources, Internal Controls, Management, Pay, Uncategorized |
compensation, compliance, Corporate Compliance, corporate governance, employee, Employee Benefits, Employee Handbook, Employer, Employers, Employment, Employment Policies, Executive Compensation, Hiring, HR, Human Resources, Internal Controls, Management, Pay, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 13, 2017
The National Labor Relations Board is inviting employers to another interested person’s to provide input to the NLRB about it’s union representation election rules By responding by February 12, 2018 to a Request for Information the NLRB will publish in the Federal Register today (12:13/17).
The Request for Information in will ask for public input regarding three questions about the Board’s 2014 Election Rule, which modified the Board’s representation-election procedures published at at 29 CFR parts 101 and 102:
1. Should the 2014 Election Rule be retained without change?
2. Should the 2014 Election Rule be retained with modifications? If so, what should be modified?
3. Should the 2014 Election Rule be rescinded? If so, should the Board revert to the Representation Election Regulations that were in effect prior to the 2014 Election Rule’s adoption, or should the Board make changes to the prior Representation Election Regulations? If the Board should make changes to the prior Representation Election Regulations, what should be changed?
The Request for Information was approved by Board Chairman Philip A. Miscimarra and Board Members Marvin E. Kaplan and William J. Emanuel. Board Members Mark Gaston Pearce and Lauren McFerran dissented.
The election rules published during the Obama administration highly controversial to most employers. The Obama Administration’s publication of the prounion rules was part of a broader series of legislative and regulatory actions by that administration that sought to expand union organizing and other powers. While courts overruled many of these regulatory efforts, the fast track election rules adopted during the Obama Administration have not been struck down and therefore remain in force. Many employers view these rules as giving union organizers unfair advantage in union organizing elections.
Tomorrow’s invitation for public input on the Obama Administration election rule comes after President Trump filled vacancies on the NLRB after he took office. Many NLRB watchers expect these Trump appointees will cause the NLRB to modify or reverse the Obama Administration election and other rules .
The official Request for Information as approved by the Board, including the dissenting views, may be found here.
Responses to these questions will be accepted from Wednesday, December 13, 2017 to Monday, February 12, 2018 (within 60 days after publication in the Federal Register). Employers and others interested in seeking changes to the election rule should submit comments with this period.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Give NLRB Your Input On Union Representation Election Regulations |
Comments Off on Give NLRB Your Input On Union Representation Election Regulations |  board of directors, Corporate Compliance, corporate governance, Employment, HR, Human Resources, Internal Controls, Labor Management Relations, Leadership, Management, NLRA, Risk Management, Uncategorized, Unfair Labor Practice, Union, Union certification, Union elections, Worker Classification | Tagged: Employer, Labor, Union, union election |
board of directors, Corporate Compliance, corporate governance, Employment, HR, Human Resources, Internal Controls, Labor Management Relations, Leadership, Management, NLRA, Risk Management, Uncategorized, Unfair Labor Practice, Union, Union certification, Union elections, Worker Classification | Tagged: Employer, Labor, Union, union election |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 12, 2017
The Internal Revenue Service (“IRS”) is acting to help Patient Protection and Affordable Care Act (“Obamacare”) health subsidy-eligible individuals living in regions where exchange insurers do not offer bronze (lowest cost) coverage even as it moves ahead to nail employers failing to comply with Obamacare’s employer shared responsibility rules (commonly referred to as the “employer mandate”). The move comes as House and Senate Conferees are preparing to conference to work out differences in the tax bill which could repeal the Obamacare individual mandate penalty for failing to maintain coverage while leaving intact penalties against employers violating the employer mandate by failing to offer affordable minimum essential coverage as well as other Obamacare penalties on plans and their employers.
IRS New Individual Obamacare Relief
Notice 2017-74 will provide that Individuals who are not eligible for coverage under an eligible employer-sponsored plan and who lack access to affordable coverage should not be denied the use of the affordability exemption under § 5000A(e)(1) of the Code and § 1.5000A-3(e) of the Regulations merely because they reside in an area served by a Marketplace that does not offer a bronze-level plan. Consequently, for purposes of the affordability exemption under § 5000A(e)(1) and § 1.5000A-3(e), if an individual resides in a rating area served by a Marketplace that does not offer a bronze plan, the individual generally should use as his or her applicable plan the lowest cost metal-level plan available in the Marketplace serving the rating area in which the individual resides.
Notice 2017-74 will be in IRB 2017-51, dated December 18, 2017.
Employer’s Still Face Obamacare Penalties
While the IRS has issued limited relief for individuals from the ACA’s individual mandate penalties, so far it has remained steadfast in its refusal to grant employers corresponding relief from the ACA employer shared responsibility penalties or other ACA penalties. Instead, IRS officials continue to make clear that the IRS intends to enforce the ACA employer shared responsibility rules against employers with 50 or more full-time employees (including full-time equivalent employees) (“covered employers”).
Under the Obamacare employer mandate rules, covered employers face significant Federal tax penalties for (1) failing to offer minimal essential coverage to substantially all full-time employees and their dependents (the “A Penalty”), or (2) offering coverage that is either “unaffordable” or does not provide “minimum value” (the “B Penalty”) (referred to collectively as the “ACA Penalties”) if a full-time employee enrolls in the Health Insurance Marketplace (the “Exchange”) and receives a Premium Tax Credit.
While many employers assumed President Trump’s January 20, 2017 Executive Order Executive Order Minimizing the Economic Burden of the Patient Protection and Affordable Care Act Pending Repeal would insulate them against enforcement of the employer mandate and other Obamacare penalties, the IRS doesn’t see the Executive Order as barring its enforcement of Obamacare against sponsoring employers or their group health plans. An April 14, 2017 IRS Chief Counsel letter, for instance, the IRS announced it does not interpret its discretionary authority under Obamacare to allow waiver of the employer mandate tax imposed under Internal Revenue Code Section 4980H against covered employers that fail to provide the affordable minimum essential coverage required by the employer mandate. In keeping with this interpretation, the IRS has announced that it will begin enforcement of the employer mandate tax liability for plan years after 2015 against covered employers that failed to meet the employer mandate.
Of course, the employer mandate is not the only Obama care provision that employers and their health plans need to worry about. In addition to the employer mandate, Obamacare imposed a host of patient protection and other federal mandates upon employer-sponsored plans, most of which apply to plans covering two or more employees. In addition to any benefit and other administrative penalties that otherwise arise under the Employee Retirement Income Security Act and/or the Social Security Act for violating these mandates, employers sponsoring plans that violate any of 40 listed mandates imposed by Obamacare or certain other federal laws also become liable under Internal Revenue Code Section 6039D to self-identify, self-assess, report on Form 8928 and pay an excise tax equal to $100 per person per uncorrected violation. The IRS, Department Of Labor and Department Of Health and Human Services have taken the position the January 20 Executive Order also does not bar enforcement of those Obamacare penalties. Accordingly, employers and their group health plans continue to face potentially substantial liability if their group health plan does not comply with Obamacare.
In the face of these exposures, employers and their group health plan administrators, fiduciaries and advisors should carefully review their plans and their administration for compliance before the end of the plan year so as to be able to take appropriate and timely corrective action before penalties attach and while stop loss or other insurance is available to help mitigate the cost of these corrections. Employers preparing for upcoming health plan renewals also should review their group contracts and conduct due diligence to verify their group health plan terms and operations meet the mandates as they initiate new plan years. Employers also generally will want to review their compliance and take action to address any deficiencies against any vendors or advisers who may have culpability in the defective health plan design or administration. Prompt action against vendors who may be culpable for the design or administration defects is necessary to preserve potential claims for contractual, deceptive trade practices or other causes of action that an employer might have under state contract, tort or other law. Employers and health plan fiduciaries should consider engaging experienced legal counsel to conduct this review on behalf of the employer other plan sponsor within the scope of attorney-client privilege so as to assess and address these potential risks on a timely basis and explore options within the scope of privilege. Brokers, advisors, consultants and insurers whose employer clients also may want to assess compliance risks and/or urge their clients to do so to help minimize their exposure to malfeasance or other claims from clients angry about penalties and other unexpected costs of noncompliance.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediatepast RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, BenefitsMagazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on IRS Prepares To Nail Employers Under Obamacare Mandate While Giving Some Individual Mandate Relief |
Comments Off on IRS Prepares To Nail Employers Under Obamacare Mandate While Giving Some Individual Mandate Relief |  105(h), 5000, ACA, compliance, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, Excise Taxes, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, Human Resources, Premium Subsidies, Uncategorized |
105(h), 5000, ACA, compliance, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, Excise Taxes, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, Human Resources, Premium Subsidies, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
December 5, 2017
The Justice Department’s report Tuesday that the Justice Department spent $3.2 million on Special counsel Robert Mueller’s Russia probe its first four-and-a-half months highlights the importance for leaders accountable for their organizations’s Federal Sentencing Guideline, sexual harassment and other corporate compliance programs to appropriately plan and budget for potential investigation and defense costs as part of their compliance and risk management planning.
Conducting an internal investigation or defending a government or other allegation of wrongdoing often proves surprisingly expensive. While how much an internal investigation costs can vary widely depending on the issue, its potential civil and criminal liability and public relations implications on the organization and its management, it’s timing, the adequacy of the pre-event compliance management and record keeping relating to the issue, and a host of other concerns, investigation and defense costs often become largely irrelevant when an organization is required to investigate or defend against charges of legal or other business misconduct that expose the organization or its leadership to potentially devastating legal or business consequences. When these events happen, organizations and their leaders often see little option to spend whatever is necessary to defend their organization and its reputation.
Compared to the reported internal investigation and defense expenditures of private sector organizations that have faced these these make or break investigations, the Justice Department’s reported expenditures to date on the Russian probe look small.
For instance, Twenty-First Century Fox in March, 2017 Securities and Exchange Commission (SEC) filings disclosed spending $45 million tied to litigation related to harassment allegations in the 9 first three quarters of 2017 and $10 million “related to settlements of pending and potential litigations” during its fiscal third quarter as well as having received investigative inquiries and stockholder demands to inspect the books and records of the company which could lead to future litigation in the aftermath of sexual harassment allegations at Fox News.
In contrast, Avon Products spent nearly $500 million conducting its internal investigation before paying a $135m fine to the US government to settle charges it violated the Foreign Corrupt Practices Act by giving Chinese authorities $8 million in gifts and cash while it sought to obtain the first “direct sell” license in China.
These and other publicly disclosed expenditures make clear that corporate officers and directors need to reassess their investment in compliance both to strengthen the effectiveness of their efforts and to plan to deal with the financial, legal, operational and other costs of investigating and defending potential charges.
Aboaut The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Consider Internal Investigation & Defense Costs When Administering Compliance Programs |
Comments Off on Consider Internal Investigation & Defense Costs When Administering Compliance Programs |  ADA, Affirmative Action, board of directors, Brokers, Child Labor, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, conflict of interest, Corporate Compliance, corporate governance, Data Breach, Data Security, directors, E-Verify, EEOC, Employers, Employment, Employment Discrimination, Employment Policies, Employment Tax, English As A Second Language, ERISA, Executive Compensation, Fair Credit Reporting Act, Fair Labor Standards Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, FINRA, FLSA, GINA, Government Contractors, h-2A Visa, health benefit, health plan, HIPAA, Human Resources, I-9, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Leadership, LEP, LGBT, Management, Managment, Military Leave, Non-Compete, Nonresident aliens, occupational safety, OFCCP, officers, OSHA, Overtime, Pay, Plan Admistrator, Privacy, Professional Liability, Rehabilitation Act, Retaliation, Safety, Uncategorized, USERRA, VEVRRA, visas, Wage & Hour, Whistleblower, Worker Classification |
ADA, Affirmative Action, board of directors, Brokers, Child Labor, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, conflict of interest, Corporate Compliance, corporate governance, Data Breach, Data Security, directors, E-Verify, EEOC, Employers, Employment, Employment Discrimination, Employment Policies, Employment Tax, English As A Second Language, ERISA, Executive Compensation, Fair Credit Reporting Act, Fair Labor Standards Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, FINRA, FLSA, GINA, Government Contractors, h-2A Visa, health benefit, health plan, HIPAA, Human Resources, I-9, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Leadership, LEP, LGBT, Management, Managment, Military Leave, Non-Compete, Nonresident aliens, occupational safety, OFCCP, officers, OSHA, Overtime, Pay, Plan Admistrator, Privacy, Professional Liability, Rehabilitation Act, Retaliation, Safety, Uncategorized, USERRA, VEVRRA, visas, Wage & Hour, Whistleblower, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 20, 2017
Hiring enough qualified workers to fill demand is the key challenges US manufacturing companies face amid an increasingly healthy manufacturing outlook.
The National Association of Manufacturers (NAM) reports that United States manufacturers generally report feeling optimistic about their own business opportunities as well as the US economy generally heading into the fourth quarter of 2017 and 2018
The chart below summarizes the highlights of the most recent survey responses.

Learn more about the survey here.
The upbeat third-quarter survey results coincide with the release of a number of upbeat economic indicators for the third quarter. Among other things, NAM reports manufacturing production has risen by 2.5 percent over the past 12 months, the best year-over-year rate since August 2014. In October:
- Manufacturing production expanded robustly in October, up 1.3 percent, its fastest monthly pace of growth since April;
- Durable goods production rose by 0.4 percent;
- Nondurable goods production rose by 2.3 percent, rebounding from significant declines in activity in August and September in the chemicals and petroleum and coal products segments due to Hurricanes Harvey and Irma;
- Manufacturing capacity utilized soared from 75.5 percent in September to 76.4 percent in October, a reading not seen since May 2008; and
- Housing starts and consumer spending continue to rise.
- While NAM reports manufacturers are optimistic about their business performance and opportunities over the next 12-months, manufacturers also are increasingly concerned about hiring the workers needed to meet demand. The uptick in the economy following the long economic downturn continues to fuel a shortage in qualified, experienced workers as well as competition among employers for experienced and inexperienced workers. Manufacturing and other businesses need to re-evaluate and update their existing hiring, compensation, training and other workforce recruitment and retention practices to recruit additional workers as well as to retain key employees likely to receive overtures to consider changing employment from other employers within and outside the employer’s industry. Business leaders also should re-assess the adequacy of existing noncompete, trade secret and other policies and practices for safeguarding trade secrets and other sensitive systems and data to minimize risks of lost or compromised intellectual property if workers leave as well as maximize the strength of protections for data and systems shared with new recruits.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Recruiting Qualified Workers Biggest Challenge US Manufacturers See In Otherwise Optimistic 3rd Quarter 2017 |
Comments Off on Recruiting Qualified Workers Biggest Challenge US Manufacturers See In Otherwise Optimistic 3rd Quarter 2017 |  Corporate Compliance, corporate governance, Economy, employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Non-Compete, Trade secret, Uncategorized |
Corporate Compliance, corporate governance, Economy, employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Non-Compete, Trade secret, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 1, 2017
The National Labor Relations Board (NLRB) announced today the appointment of Jennifer A. Abruzzo to serve as NLRB’s Acting General Counsel.
Although Ms. Abruzzo original began her legal career as a civil litigation attorney in the medical malpractice division of a South Florida firm, she has spent almost twenty-three years working for the NLRB in various capacities, including as Field Attorney, Supervisory Field Attorney and Deputy Regional Attorney in the Miami, Florida office, as well as Deputy Assistant General Counsel in the Division of Operations-Management in Washington, DC, where she oversaw Regional operations in the Northeast and Midwest.
Prior to becoming Deputy General Counsel, Ms. Abruzzo served as the Executive Assistant to Acting General Counsel Lafe E. Solomon, and detailed in that role for General Counsel Ronald E. Meisburg. In 2011 her involvement at the NLRB drew public attention when an e-mail sent to her by then NLRB Deputy Assistant General Counsel Joseph Baniszewski forwarding a political cartoon mocking the state of South Carolina with regard to Boeing Corporation’s decision to locate its manufacturing facility to South Carolina was made public.
During her career with NLRB, she has participated in the litigation of numerous high profile cases.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 1 Comment |
1 Comment |  board of directors, compliance, directors, employee, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Policies, ERISA, health plan, Human Resources, Internal Controls, Internal Investigations, Loyalty, Management, Managment, NLRA, Non-Compete, Non-Competition Agreement, Uncategorized, Unfair Labor Practice, Union, Workforce | Tagged: Economy, Employer, Hiring, HR, Job Growth, Labor, Labor Management Relations, Labor Pool, Labor Statistics, Management, Recruiting, Workforce |
board of directors, compliance, directors, employee, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Policies, ERISA, health plan, Human Resources, Internal Controls, Internal Investigations, Loyalty, Management, Managment, NLRA, Non-Compete, Non-Competition Agreement, Uncategorized, Unfair Labor Practice, Union, Workforce | Tagged: Economy, Employer, Hiring, HR, Job Growth, Labor, Labor Management Relations, Labor Pool, Labor Statistics, Management, Recruiting, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 21, 2017
This month’s annual October Stop Bullying Month observances are a great time for employers to deter sexual, racial, religious, national Origin, disability discrimination and harassment, retaliation and other illegal or otherwise counterproductive bullying in their workplaces.
Aside from obvious legal exposures that often attend from many versions of workplaces bullying, unfair or heavy handed tactics of workplace bullies often pervasively disrupt workplace productivity and operations by undermining performance, feedback, initiative, employee retention and a host of other ways.
Seize the opportunity to boost your organization’s legal and operational exposures non discrimination, anti-harassment, and other workplace bullying policies by leveraging the visibility and resources of this month’s anti-bullying activities.
Checkout StopBullying.gov for more information and free resources.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪ RAISE Act Immigration Reforms Touted As “Giving Americans A Raise”
▪ Health Clinic At Houston Convention Center, Other HHS Help For Hurricane Harvey Victims
▪ IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties
▪ DB Plan Sponsors Check Out New Bifurcated Distribution Model Amendmentsy
▪ U.S. News Names 2017-2018 “Best” Hospitals; Patient Usefulness Starts With Metholodogy Understanding
▪ Use Lessons Of Past Mistakes or Injustice To Build Better Future
▪ Prepare For Turnover, Other Challenges From Rising Workforce Competition
▪ Employers, Health Plans Should Brace For Tightened Federal Mental Health Coverage Mandate Disclosure And Enforcement
▪ Withholding Calculator Tool Helps Workers Figure Withholding
▪ Better Preparing U.S. Workers To Fill Your Jobs
▪ SCOTUS Ruling Bars Many State Arbitration Agreement Restrictions
▪ $2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Address Workplace Harassment During October Stop Bullying Month |
Comments Off on Address Workplace Harassment During October Stop Bullying Month |  Absenteeism, ADA, Affirmative Action, board of directors, Child Safety, Civil Rights, compliance, conflict of interest, Corporate Compliance, corporate governance, directors, Disability, Disability Discrimination, Discrimination, Drug & Alcohol, EEOC, employee, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Employment Policies, English As A Second Language, Gaming, HR, Human Resources, Immigration, Internal Controls, Internal Investigations, Leadership, LEP, LGBT, Management, Managment, Patient Empowerment, Privacy, Retaliation, Risk Management, Schools, Security, Sexual Harassment, Union, USERRA, veterans, VEVRAA, VEVRRA, Whistleblower, Worker, Workforce | Tagged: ADA, Corporate Compliance, Employer, Employers, Employment, employment law, Human Resources, Insurance, Insurer, Labor Department, Risk Management, Wage & Hour |
Absenteeism, ADA, Affirmative Action, board of directors, Child Safety, Civil Rights, compliance, conflict of interest, Corporate Compliance, corporate governance, directors, Disability, Disability Discrimination, Discrimination, Drug & Alcohol, EEOC, employee, Employee Handbook, Employer, Employers, Employment, Employment Discrimination, Employment Policies, English As A Second Language, Gaming, HR, Human Resources, Immigration, Internal Controls, Internal Investigations, Leadership, LEP, LGBT, Management, Managment, Patient Empowerment, Privacy, Retaliation, Risk Management, Schools, Security, Sexual Harassment, Union, USERRA, veterans, VEVRAA, VEVRRA, Whistleblower, Worker, Workforce | Tagged: ADA, Corporate Compliance, Employer, Employers, Employment, employment law, Human Resources, Insurance, Insurer, Labor Department, Risk Management, Wage & Hour |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 14, 2017
Monthly Social Security and Supplemental Security Income (SSI) benefits for more than 66 million Americans will increase 2.0 percent in 2018.
The Social Security Administration announced the 2.0 cost of living adjustment (COLA) Friday announced a 2% increase in benefits for 2018.
The largest COLA increase since 2012 will increase the benefits payable to more than 61 million Social Security beneficiaries in January 2018. Increased payments to more than 8 million SSI beneficiaries will begin on December 29, 2017. The Social Security Administration deducts $1 from benefits for each $3 earned over $45,360 until the month the worker turns age 66.)
There is no limit on earnings for workers who are “full” retirement age or older for the entire year.
The slight increase in benefits also may result in a corresponding decrease in disability benefits under plans that integrate or otherwise offset plan benefits with Social Security.
Information about Medicare COLAs for 2018, when announced, will be available at www.Medicare.gov.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪ RAISE Act Immigration Reforms Touted As “Giving Americans A Raise”
▪ Health Clinic At Houston Convention Center, Other HHS Help For Hurricane Harvey Victims
▪ IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties
▪ DB Plan Sponsors Check Out New Bifurcated Distribution Model Amendmentsy
▪ U.S. News Names 2017-2018 “Best” Hospitals; Patient Usefulness Starts With Metholodogy Understanding
▪ Use Lessons Of Past Mistakes or Injustice To Build Better Future
▪ Prepare For Turnover, Other Challenges From Rising Workforce Competition
▪ Employers, Health Plans Should Brace For Tightened Federal Mental Health Coverage Mandate Disclosure And Enforcement
▪ Withholding Calculator Tool Helps Workers Figure Withholding
▪ Better Preparing U.S. Workers To Fill Your Jobs
▪ SCOTUS Ruling Bars Many State Arbitration Agreement Restrictions
▪ $2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on 2018 Social Security COLAs Set |
Comments Off on 2018 Social Security COLAs Set |  Claims Administration, defined benefit plan, Defined Benefit Plans, Disability, Disability Plans, Employee Benefits, Employer, Employers, Employment, ERISA, HR, Human Resources, pension plan, retirement plan, Retirement Plans, Retirements, Social Security, Uncategorized | Tagged: Social Security, SSI |
Claims Administration, defined benefit plan, Defined Benefit Plans, Disability, Disability Plans, Employee Benefits, Employer, Employers, Employment, ERISA, HR, Human Resources, pension plan, retirement plan, Retirement Plans, Retirements, Social Security, Uncategorized | Tagged: Social Security, SSI |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 13, 2017
Qualified profit-sharing and pension plan sponsors, fiduciaries, administrators and service providers should check of this recent guidance on various qualified pension and profit sharing plan qualification:
Organizations and service providers involved in defined benefit plans should review their programs and make adjustments as warranted.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment;a member and policy technical adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leaders, and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here including:
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and uhave no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on IRS Updates Defined Benefit Plan Guidance |
Comments Off on IRS Updates Defined Benefit Plan Guidance |  Bankruptcy, board of directors, Brokers, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, directors, employee, Employee Benefits, Employer, Employers, Employment Policies, Employment Tax, ERISA, Excise Tax, Form 5500, Government Contractors, government plan, HR, Human Resources, Insurance, Internal Revenue Code, IRC, Labor Management Relations, Management, retirement plan, Retirement Plans, Retirements, Tax, Tax Qualification, Uncategorized, Worker Classification | Tagged: defined benefit plan, Retirement Plans, tax qualification |
Bankruptcy, board of directors, Brokers, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, directors, employee, Employee Benefits, Employer, Employers, Employment Policies, Employment Tax, ERISA, Excise Tax, Form 5500, Government Contractors, government plan, HR, Human Resources, Insurance, Internal Revenue Code, IRC, Labor Management Relations, Management, retirement plan, Retirement Plans, Retirements, Tax, Tax Qualification, Uncategorized, Worker Classification | Tagged: defined benefit plan, Retirement Plans, tax qualification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 12, 2017
President Trump today (October 12, 2017) issued the following that he promised to be the first in a series of executive orders and other administrative actions that his administration will roll out to provide Obamacare relief for consumers, employers and others by promoting healthcare choice and competition given the continued difficulty by the Republican-led Congress to pass legislation repealing or replacing the health care law.
What actually will result remains to be seen. Like the January 20, 2017 Executive Order Minimizing the Economic Burden of the Patient Protection and Affordable Care Act Pending Repeal that President Trump signed as his first executive order, the new Executive Order doesn’t actually change anything; it merely directs the agencies to review and propose for implementation changes to regulations and other guidance allowed by law.
On the heels of his announcement of the Executive Order, President Trump moved forward on his promise to take other action on Obamacare by announcing that the Administration will not continue funding for individual subsidies that currently are continued under an Obama Administration action in the absence of Congressional action funding those subsidies.
Concerned parties should monitor and inform themselves about proposed changes in the Executive Order and other actions as they are proposed and develop, and provide timely comments and other input to help influence the shape and content of any changes proposed or adopted in response to the Executive Order. Solutions Law Press, Inc. will be monitoring developments. Stay tuned for updates.
Language of Executive Order
By the authority vested in me as President by the Constitution and the laws of the United States of America, it is hereby ordered as follows:
Section 1. Policy.
(a) It shall be the policy of the executive branch, to the extent consistent with law, to facilitate the purchase of insurance across State lines and the development and operation of a healthcare system that provides high-quality care at affordable prices for the American people. The Patient Protection and Affordable Care Act (PPACA), however, has severely limited the choice of healthcare options available to many Americans and has produced large premium increases in many State individual markets for health insurance. The average exchange premium in the 39 States that are using http://www.healthcare.gov in 2017 is more than double the average overall individual market premium recorded in 2013. The PPACA has also largely failed to provide meaningful choice or competition between insurers, resulting in one-third of America’s counties having only one insurer offering coverage on their applicable government-run exchange in 2017.
(b) Among the myriad areas where current regulations limit choice and competition, my Administration will prioritize three areas for improvement in the near term: association health plans (AHPs), short-term, limited-duration insurance (STLDI), and health reimbursement arrangements (HRAs).
(i) Large employers often are able to obtain better terms on health insurance for their employees than small employers because of their larger pools of insurable individuals across which they can spread risk and administrative costs. Expanding access to AHPs can help small businesses overcome this competitive disadvantage by allowing them to group together to self-insure or purchase large group health insurance. Expanding access to AHPs will also allow more small businesses to avoid many of the PPACA’s costly requirements. Expanding access to AHPs would provide more affordable health insurance options to many Americans, including hourly wage earners, farmers, and the employees of small businesses and entrepreneurs that fuel economic growth.
(ii) STLDI is exempt from the onerous and expensive insurance mandates and regulations included in title I of the PPACA. This can make it an appealing and affordable alternative to government-run exchanges for many people without coverage available to them through their workplaces. The previous administration took steps to restrict access to this market by reducing the allowable coverage period from less than 12 months to less than 3 months and by preventing any extensions selected by the policyholder beyond 3 months of total coverage.
(iii) HRAs are tax-advantaged, account-based arrangements that employers can establish for employees to give employees more flexibility and choices regarding their healthcare. Expanding the flexibility and use of HRAs would provide many Americans, including employees who work at small businesses, with more options for financing their healthcare.
(c) My Administration will also continue to focus on promoting competition in healthcare markets and limiting excessive consolidation throughout the healthcare system. To the extent consistent with law, government rules and guidelines affecting the United States healthcare system should:
(i) expand the availability of and access to alternatives to expensive, mandate-laden PPACA insurance, including AHPs, STLDI, and HRAs;
(ii) re-inject competition into healthcare markets by lowering barriers to entry, limiting excessive consolidation, and preventing abuses of market power; and
(iii) improve access to and the quality of information that Americans need to make informed healthcare decisions, including data about healthcare prices and outcomes, while minimizing reporting burdens on affected plans, providers, or payers.
Sec. 2. Expanded Access to Association Health Plans.
Within 60 days of the date of this order, the Secretary of Labor shall consider proposing regulations or revising guidance, consistent with law, to expand access to health coverage by allowing more employers to form AHPs. To the extent permitted by law and supported by sound policy, the Secretary should consider expanding the conditions that satisfy the commonality‑of-interest requirements under current Department of Labor advisory opinions interpreting the definition of an “employer” under section 3(5) of the Employee Retirement Income Security Act of 1974. The Secretary of Labor should also consider ways to promote AHP formation on the basis of common geography or industry.
Sec. 3. Expanded Availability of Short-Term, Limited‑Duration Insurance.
Within 60 days of the date of this order, the Secretaries of the Treasury, Labor, and Health and Human Services shall consider proposing regulations or revising guidance, consistent with law, to expand the availability of STLDI. To the extent permitted by law and supported by sound policy, the Secretaries should consider allowing such insurance to cover longer periods and be renewed by the consumer.
Sec. 4. Expanded Availability and Permitted Use of Health Reimbursement Arrangements.
Within 120 days of the date of this order, the Secretaries of the Treasury, Labor, and Health and Human Services shall consider proposing regulations or revising guidance, to the extent permitted by law and supported by sound policy, to increase the usability of HRAs, to expand employers’ ability to offer HRAs to their employees, and to allow HRAs to be used in conjunction with nongroup coverage.
Sec. 5. Public Comment.
The Secretaries shall consider and evaluate public comments on any regulations proposed under sections 2 through 4 of this order.
Within 180 days of the date of this order, and every 2 years thereafter, the Secretary of Health and Human Services, in consultation with the Secretaries of the Treasury and Labor and the Federal Trade Commission, shall provide a report to the President that:
(a) details the extent to which existing State and Federal laws, regulations, guidance, requirements, and policies fail to conform to the policies set forth in section 1 of this order; and
(b) identifies actions that States or the Federal Government could take in furtherance of the policies set forth in section 1 of this order.
Sec. 7. General Provisions.
(a) Nothing in this order shall be construed to impair or otherwise affect:
(i) the authority granted by law to an executive department or agency, or the head thereof; or
(ii) the functions of the Director of the Office of Management and Budget relating to budgetary, administrative, or legislative proposals.
(b) This order shall be implemented consistent with applicable law and subject to the availability of appropriations.
(c) This order is not intended to, and does not, create any right or benefit, substantive or procedural, enforceable at law or in equity by any party against the United States, its departments, agencies, or entities, its officers, employees, or agents, or any other person.
DONALD J. TRUMP
THE WHITE HOUSE,
October 12, 2017
Implications & Actions
The impact of this and other Executive Orders and other Presidential actions depend upon what actions, if any, the agencies determine they are allowed by law to take and how those changes are implemented. Concerned persons and organizations should begin preparing input to the agencies and monitoring and commenting on proposals and other guidance to help shape the outcome.
Solutions Law Press, Inc. is preparing initial analysis of this Executive Order and will be closely monitoring and updating this analysis. Follow up to learn more and stay abreast of new developments.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes. Author of numerous works on privacy and data security, Ms. Stamer‘s experience includes involvement in cyber security and other data privacy and security matters for more than 20 years.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Read Trump Health Care Executive Order |
Comments Off on Read Trump Health Care Executive Order |  105(h), ACA, Affordable Care Act, Association Health Plan, Brokers, Civil Rights, Claims Administration, Corporate Compliance, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, Excise Tax, Excise Taxes, Fiduciary Responsibility, FLSA, Form 5500, health benefit, Health Benefits, health Care, Health Care Reform, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, MEWA, Payroll Tax, Premium Subsidies, Reporting & Disclosure, Tax Credit, Uncategorized, Union, Wellness, Wellness Programs, Worker Classification, Workforce, zane benefits | Tagged: ACA, Affordable Care Act, Corporate Compliance, Employee Benefits, Employer, Employers, Employment, employment law, ERISA, executive, Health Care, Health Care Reform, Health Insurance, Health Plan, Health Plans, Human Resources, Insurance, Labor, Labor Department, Managed Care, Medical Coverage, Overtime, Tax, wage and hour, Worker Classification |
105(h), ACA, Affordable Care Act, Association Health Plan, Brokers, Civil Rights, Claims Administration, Corporate Compliance, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, Excise Tax, Excise Taxes, Fiduciary Responsibility, FLSA, Form 5500, health benefit, Health Benefits, health Care, Health Care Reform, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, MEWA, Payroll Tax, Premium Subsidies, Reporting & Disclosure, Tax Credit, Uncategorized, Union, Wellness, Wellness Programs, Worker Classification, Workforce, zane benefits | Tagged: ACA, Affordable Care Act, Corporate Compliance, Employee Benefits, Employer, Employers, Employment, employment law, ERISA, executive, Health Care, Health Care Reform, Health Insurance, Health Plan, Health Plans, Human Resources, Insurance, Labor, Labor Department, Managed Care, Medical Coverage, Overtime, Tax, wage and hour, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 6, 2017
As businesses continue to struggle to comply with the growing plethora of federal and state laws mandating data security, the identity theft and cyber security epidemic keeps growing.
As human resources and other business leaders work to guard their own data and respond to employee demands for assistance in responding to breaches of their personal financial and other data, this weeks’ announcement that embattled credit monitoring giant Equifax has been awarded the exclusive contract to provide taxpayer identification and fraud prevention services to the Internal Revenue Service has many questioning whether these investments are futile.
The IRS’ announcement comes despite the September 7, 2017 announcement by Equifax of a data breach of its records impacting sensitive personal information of millions of consumers including:
- The names, Social Security numbers, birth dates, addresses and, in some instances, driver’s license numbers of an estimated 143 million U.S. consumers;
- Credit card numbers for approximately 209,000 U.S. consumers,
- Certain dispute documents with personal identifying information for approximately 182,000 U.S. consumers,and
- Personal information for certain U.K. and Canadian consumers.
The huge breach already was creating many headaches for many businesses and their human resources departments before the IRS announced the award of the contract to Equifax. Due to the massive size of the breach, mist companies have been required to respond to concerns of workers impacted directly by the breach as well as requests of employees and identity theft protection companies that the business consider offering cybersecurity protection for employees or customers.
Beyond helping their workforce understand and cope with the news, many businesses and employee benefit plans also face the added headache of needing to investigate and respond to concerns about their own potential responsibilities to provide breach notification or take other actions. This added headache arises due to their or their plans’ use of Equifax or vendors utilizing Equifax to run employee or vendor background checks or carry out internal employee or employee benefit plan, customer or other business activities. These involvements often give rise to duties to conduct investigations and potentially provide notification or other responses to employees, applicants, benefit plan members, contractors or customers whose data may have been impacted under the Fair and Accurate Credit Transactions Act (FACTA), the Health Insurance Portability and Accountability Act (HIPAA), the Employee Retirement Income Security Act (ERISA) Fiduciary Responsibility rules or various other federal and state laws and regulations, vendor contracts or their own data privacy or security policies.
When notification is recommended or required, human resources and other business leaders also have to consider if modifications should be considered to standard protocols recommended to data breach victims. Notification and registration as an identity theft victim with Equifax long has been a standard part of the federal and state government recommended protocol for recommended to consumers impacted by identity theft or other data breaches. See,e.g., IRS Taxpayer Guide To Identity Theft. Although government agencies as of yet have not changed this recommendation to remove Equifax reporting, many consumers and others view reporting to Equifax as akin to the fox watching the hen house. Consequently, employers and other parties helping consumers respond to the breach often receive push back or questions from consumers about the appropriateness and security reporting to Equifax in light of its breach.
Beyond evaluating and handling their own legal responsibilities to investigate and deal with any breach impacting their data, employers and other business leaders also likely are or should consider what claims against Equifax, other vendors and business partners involved with Equifax and their own liability insurers are available and warranted to help cover the costs and potential liabilities for the business arising from the breach and it’s fall out.
As employers and other businesses work through these issues, They should keep in mind that the fallout is likely to continue for years and be further complicated by past and subsequent breaches impacting other governmental and private organizations. Human resources, employee benefits and other businesses and their leaders can expect to experience challenges dealing with fraudulent uses of misappropriated information as well as demands that they tighten up their background check, data security and usage and other practices and documentation to mitigate risks from the compromised data.
Human resources, employee benefits and other business leaders need to secure the assistance of counsel experienced in guiding their organizations through these and other challenges.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes. Author of numerous works on privacy and data security, Ms. Stamer‘s experience includes involvement in cyber security and other data privacy and security matters for more than 20 years.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
▪RAISE Act Immigration Reforms Touted As “Giving Americans A Raise”
▪Health Clinic At Houston Convention Center, Other HHS Help For Hurricane Harvey Victims
▪IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties
▪DB Plan Sponsors Check Out New Bifurcated Distribution Model Amendmentsy
▪U.S. News Names 2017-2018 “Best” Hospitals; Patient Usefulness Starts With Metholodogy Understanding
▪Use Lessons Of Past Mistakes or Injustice To Build Better Future
▪Prepare For Turnover, Other Challenges From Rising Workforce Competition
▪Employers, Health Plans Should Brace For Tightened Federal Mental Health Coverage Mandate Disclosure And Enforcement
▪Withholding Calculator Tool Helps Workers Figure Withholding
▪Better Preparing U.S. Workers To Fill Your Jobs
▪SCOTUS Ruling Bars Many State Arbitration Agreement Restrictions
▪$2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Dealing With HR, Benefits & Other Headaches From Equifax and Other Data Breach |
Comments Off on Dealing With HR, Benefits & Other Headaches From Equifax and Other Data Breach |  Banking, board of directors, Brokers, Civil Monetary Penalties, Claims, Claims Administration, compliance, conflict of interest, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, E-Verify, EBSA, Educational Privacy, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Tax, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, Form 5500, GINA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, Hiring, HR, Human Resources, I-9, Identity Theft, Income Tax, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, Internet, IRC, Labor Management Relations, Leadership, Management, Managment, Patient Empowerment, Payroll Tax, pension plan, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Risk Management, Security, Tax, Tax Credit, Tax Qualification, Technology, third party administrators, visas, Workforce | Tagged: ADA, Corporate Compliance, Data Breach, Employee Benefits, Employer, Employers, employment law, Equifax, ERISA, Health Care, Health Insurance, HIPAA, Human Resources, Insurance, Insurer, Labor Department, Privacy, Retirement Plans, Risk Management, Tax, Technology, wage and hour, Worker Classification |
Banking, board of directors, Brokers, Civil Monetary Penalties, Claims, Claims Administration, compliance, conflict of interest, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, E-Verify, EBSA, Educational Privacy, employee, Employee Benefits, Employer, Employers, Employment, Employment Policies, Employment Tax, ERISA, ESOP, Excise Tax, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, Fiduciary Responsibility, Financial Security, Form 5500, GINA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, Hiring, HR, Human Resources, I-9, Identity Theft, Income Tax, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, Internet, IRC, Labor Management Relations, Leadership, Management, Managment, Patient Empowerment, Payroll Tax, pension plan, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Reporting & Disclosure, retirement plan, Retirement Plans, Retirements, Risk Management, Security, Tax, Tax Credit, Tax Qualification, Technology, third party administrators, visas, Workforce | Tagged: ADA, Corporate Compliance, Data Breach, Employee Benefits, Employer, Employers, employment law, Equifax, ERISA, Health Care, Health Insurance, HIPAA, Human Resources, Insurance, Insurer, Labor Department, Privacy, Retirement Plans, Risk Management, Tax, Technology, wage and hour, Worker Classification |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
September 13, 2017
Employers beware of potential National Labor Relations Act unfair labor practices risks that may arise from their adoption or enforcement of overly broad or restrictive workplace recording, acceptable use, workplace conduct, commitment-to-integrity or other policies that might be construed to prohibit or deter employees from exercising protected organization or other collective bargaining rights under the National Labor Relations Act (NLRA) in light of the Fifth Circuit’s July 25, 2017 T-Mobile United States, Inc. v. Nat’l Labor Relations Bd. decision.
In T-Mobile v. NLRB, the Fifth Circuit upheld and ordered the enforcement of a National Labor Relations Board (NLRB) ruling that telecommunications industry employers T-Mobile and MetroPCS (T-Mobile) engaged in unfair labor practices in violation of Section 8 of the NLRA by maintaining a policy that prohibited all photography and audio or video recording in its workplace without the employer’s prior permission (“Recording Policy”).
The Fifth Circuit’s ruling arose from an appeal filed by T-Mobile with the Fifth Circuit, challenging a NLRB ruling that the Recording Policy, a workplace conduct policy, a commitment-to-integrity policy and an Acceptable Use Policy included in the T-Mobile employee handbook violated the NLRA because “employees would reasonably construe the language to prohibit Section 7 activity and therefore constituted unfair labor practices prohibited under Section 8 of the NLRA. (Note: T-Mobile did not appeal the NLRB’s findings that 7 other policies also violated the NLRA).
While the Fifth Circuit’s decision only upheld the unfair labor practice determination based on the Recording policy, the decision makes clear that its findings concerning each of the four employment policies subject to the appeal as well as other employment policies could come out differently in other cases based on the contextual evidence reflected in the factual record concerning the particular employment policy and the context in which it is implemented and enforced. Employers maintaining or administering similar workplace rules will want to scrutinize carefully their own policies to assess their potential for exposing the employer to unfair labor practice charges and take appropriate action to minimize these risks.
Policies Chilling Organizational Rights Protected By NLRA § 7 Create Unfair Labor Practice Exposures
Section 7 of the NLRA protects workers’ right “to form, join, or assist labor organizations, to bargain collectively through representatives of their own choosing, and to engage in other concerted activities for the purpose of collective bargaining or other mutual aid or protection.” 29 U.S.C. § 157. NLRA § 8(a)(1) makes it an “unfair labor practice” for an employer to “interfere with, restrain, or coerce employees in the exercise of the rights” protected by NLRA § 7.
According to existing Fifth Circuit precedent, a workplace rule violates Section 8(a)(1) of the NLRA if the rule either:
- “Explicitly restricts activities protected by Section 7″ or
- Employees would reasonably construe the language to prohibit Section 7 activity even if the rule does not explicitly prohibit or has not been enforced to prohibit or restrict Section 7 protected activity.
A careful analysis of the Fifth Circuit’s decision makes clear that its decision about each of the four challenged policies covered by T-Mobile’s appeal turned upon the Court’s careful analysis of the surrounding context under which the applicable policy was implemented and administered reflected in the factual record. While the Fifth Circuit overruled as erroneous the NLRB’s findings that three other challenged policies violated the NLRA under this analysis, it agreed with and ordered enforced the NLRB’s ruling that T-Mobile’s Recording Policy violated the NLRA by impermissibly chilling worker’s exercise of their Section 7 rights. Construing the Acceptable Use Policy as prohibiting all recording in the workplace without the employer’s consent, the Fifth Circuit concluded that the policy would “discourage” a reasonable employee from engaging in protected activity” because a reasonable employee would construe the Policy as prohibiting employee unionizing or other concerted activity protected by the NLRA.
Context Protected Workplace Conduct, Commitment-To-Integrity, No Arguing or Fighting & Acceptable Use Policy
Based upon its review of the contextual facts shown in the record, the Fifth Circuit overruled the NLRB’s unfair labor practice orders with respect to T-Mobile’s workplace conduct, commitment-to- integrity, no argument or fighting and Acceptable Use policies. Employers should note, however, that the Fifth Circuit’s ruling does not give blanket enforcement to the defensibility of these policies in all circumstances. Rather, noting that “context matters” when determining whether a work rule violates the NLRA, the court found the policies read in the context of the workplace established common sense civility guidelines that a reasonable employee would not read as chilling or discouraging organization activities protected under Section 7. Accordingly, the Fifth Circuit declined to enforce the NLRB’s unfair labor practice orders against T-Mobile with respect to those policies in this instance. Employers considering the implications on this decision on their own policies should keep in mind, however, that the Fifth Circuit based its decision on the context reflected by the facts in the record. Accordingly, there remains a risk that these or other policies could be found to violate the NLRB if adopted or administered under circumstances that could chill reasonable workers from exercising their Section 7 organizational rights.
Context Invalidated Recording Policy
The critical significance of the factual context in determining the defensibility of each of these policies under Sections 7 and 8(a) of the NLRA is driven home by the Fifth Circuit’s explanation in the opinion of its decision to enforce the NLRB’s order with respect to the following Recording Policy as well as its explanation of its distinguishability from the Acceptable Use Policy that the Fifth Court found permitted.:
To prevent harassment, maintain individual privacy, encourage open communication, and protect confidential information employees are prohibited from recording people or confidential information using cameras, camera phones/devices, or recording devices (audio or video) in the workplace. Apart from customer calls that are recorded for quality purposes, employees may not tape or otherwise make sound recordings of work-related or workplace discussions. Exceptions may be granted when participating in an authorized [T-Mobile] activity or with permission from an employee’s Manager, HR Business Partner, or the Legal Department. If an exception is granted, employees may not take a picture, audiotape, or videotape others in the workplace without the prior notification of all participants.
In determining this Recording Policy impermissibly deterred employees from exercising their Section 7 rights in violation of the NLRA, the Fifth Circuit’s opinion makes clear that “the broad reach of the recording ban” strongly influenced this determination, stating:
The ban, by its plain language, encompasses any and all photography or recording on corporate premises at any time without permission from a supervisor. This ban is, by its own terms alone, stated so broadly that a reasonable employee, generally aware of employee rights, would interpret it to discourage protected concerted activity, such as even an off-duty employee photographing a wage schedule posted on a corporate bulletin board. …
Unlike the “workplace conduct” policy and the “commitment-to-integrity” policy, the recording policy forbids certain forms of clearly protected activity. We have earlier held that held those two policies would not be interpreted by a reasonable T-Mobile employee as forbidding protected activity. By contrast, a reasonable T-Mobile employee, aware of his legal rights, would read the language of the recording policy as plainly forbidding a means of engaging in protected activity.
In the face of this possibility, the Court similarly considered the factual record before rejecting T-Mobile’s argument that the Policy was defensible to promote its legitimate business interests “[t]o prevent harassment, maintain individual privacy, encourage open communication, and protect confidential information” on the grounds that “merely reciting such justifications does not alter the fact that the operative language of the rule on its face prohibits protected Section 7 activity, including Section 7 activity wholly unrelated to those stated interests.”
In reaching this determination, the Fifth Circuit distinguished these findings from its findings with regard to the Acceptable Use policy. In explaining its finding the Acceptable Use Policy valid, the Fifth Circuit’s opinion explains that the NLRB’s decision concerning the Acceptable Use Policy disregarded the context in which the acceptable use policy is to be read and understood, stating:
The “Scope” section of the acceptable use policy explicitly states that the policy “applies to all non-public T-Mobile information.” Thus the policy only prohibits employees from sharing non-public information.
Where a company policy prohibits the disclosure of non-public information, courts presume that a reasonable employee would not construe the policy to prohibit the disclosure of information that may be properly used in protected activity, such as wage and benefit information, so long as the policy does not explicitly state that it encompasses such information. … Here… the policy does not define “non-public T-Mobile information” in a way that would lead a reasonable worker to believe that it includes protected wage and benefit information. Instead, the policy only applies to the sort of proprietary business information that an employer may properly restrict its employees from sharing outside of the company. …
Thus the NLRB’s finding that a reasonable worker would construe the acceptable use policy to discourage protected activity is unreasonable, and we deny enforcement as to that part of its order.
Accordingly, the Fifth Circuit upheld enforcement of the NLRB’s order striking down the Recording Policy but denied enforcement and overruled the NLRB’s unfair labor practice finding with regard to the other three policies.
Contextual Basis of Decision Requires Employer Tread Carefully, Manage Risks
While the Fifth Circuit only enforced the NLRB’s unfair labor practice finding with respect to T-Mobile’s Recording Policy in T-Mobile, the opinion makes clear that similar or identical policies could be treated differently depending upon whether the contextual evidence reflects that the policy could be reasonably construed by employees as prohibiting or restricting conduct protected by Section 7 of the NLRA. Employers maintaining or administering similar workplace rules will want to scrutinize carefully their own policies to assess their potential for exposing the employer to unfair labor practice charges and take appropriate action to minimize these risks.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as the following:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Employers Should Manage Potential Unfair Labor Practice Risks From Recording, Acceptable Use, Fighting, Integrity & Other Employment Policies |
Comments Off on Employers Should Manage Potential Unfair Labor Practice Risks From Recording, Acceptable Use, Fighting, Integrity & Other Employment Policies |  board of directors, compliance, directors, employee, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Policies, ERISA, health plan, Human Resources, Internal Controls, Internal Investigations, Loyalty, Management, Managment, NLRA, Non-Compete, Non-Competition Agreement, Uncategorized, Unfair Labor Practice, Union, Workforce | Tagged: Economy, Employer, Hiring, HR, Job Growth, Labor, Labor Management Relations, Labor Pool, Labor Statistics, Management, Recruiting, Workforce |
board of directors, compliance, directors, employee, Employee Handbook, Employer, Employers, Employment, Employment Agreement, Employment Policies, ERISA, health plan, Human Resources, Internal Controls, Internal Investigations, Loyalty, Management, Managment, NLRA, Non-Compete, Non-Competition Agreement, Uncategorized, Unfair Labor Practice, Union, Workforce | Tagged: Economy, Employer, Hiring, HR, Job Growth, Labor, Labor Management Relations, Labor Pool, Labor Statistics, Management, Recruiting, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 21, 2017
Individual Americans that don’t maintain their and their dependents’ enrollment in at least minimum essential coverage in a health program meeting the requirements of the Patient Protection & Affordable Care Act commonly referred to as “Obama Care” still generally should expect to pay individual shared responsibility tax penalties imposed by Obamacare.
Despite campaign promises to quickly repeal or reform Obamacare, the Republican controlled Congress has been unable to pass legislation repealing the individual tax penalty or other Obamacare coverage mandate related rules. Moreover, contrary to the impression widely held by many Americans that President Trump’s January 20 Executive Order protects uncovered individuals from the tax imposed under Internal Revenue Code Section 5001A, the Internal Revenue Service still plans to enforce and collect the tax. See here. Consequently, Internal Revenue Code Section 5001A still generally requires uncovered taxpayers to pay the individual shared responsibility payment.
This means that taxpayers not enrolled in minimum essential coverage or otherwise exempt from the individual responsibility payment need to be prepared to pay the tax.
In anticipation of enforcement of the individual shared responsibility tax, the Internal Revenue Service just set the monthly national average premium for qualified health plans that have a bronze level of coverage offered through Exchanges at $272 per individual and the maximum monthly national average premium for qualified health plans with a bronze level of coverage offered through Exchanges at $1,360 for a shared responsibility family with five or more members. The Internal Revenue Service intends that these amounts will be used to calculate individual shared responsibility tax penalties for 2017. The updated amounts are published in Rev. Proc. 2017-48
In general, the individual responsibility tax equals the lesser of (1) the sum of the monthly penalty amounts, or (2) the sum of the monthly national average bronze plan premiums for the shared responsibility family. See § 1.5000A-4(a). The monthly national average bronze plan premium means, for a month for which a shared responsibility payment is imposed, 1/12 of the annual national average premium for qualified health plans that (1) have a bronze level of coverage, (2) would provide coverage for the taxpayer’s shared responsibility family members, and (3) are offered through Exchanges for plan years beginning in a calendar year with or within which the taxable year ends. §§ 5000A(c)(1)(B) and 1.5000A-4(c). For this purpose, “shared responsibility family” means, for a month in a taxable year, all nonexempt individuals for whom the taxpayer and the taxpayer’s spouse, if the taxpayer is married and files a joint return with the spouse, are liable for the shared responsibility payment under § 5000A for that taxable year. See § 1.5000A-1(d)(17).
Taxpayers who are not enrolled in the necessary health coverage to meet the Obamacare health coverage mandate should evaluate their shared responsibility tax penalty exposure and weigh whether it makes more sense to enroll in qualifying health coverage or prepare to pay the tax.
About The Author
Recognized as “Legal Leader™ Texas Top Rated Lawyer” in both Health Care Law and Labor and Employment Law, a “Texas Top Lawyer,” and an “AV-Preeminent” and “Top Rated Lawyer” by Martindale-Hubble, singled out as among the “Best Lawyers In Dallas” in employee benefits by D Magazine; Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely recognized for her nearly 30 years’ of work and pragmatic thought leadership, publications and training on health coverage and health care, health plan and employee benefits, workforce and related regulatory and other compliance, performance management, risk management, product and process development, public policy, operations and other concerns.
Throughout her legal and consulting career, Ms. Stamer has drawn recognition for combining extensive knowledge and experience with her talents as an insightful innovator and problem solver when advising, representing and defending employer and other plan sponsors, insurers, fiduciaries, insurers, electronic and other technology, plan administrators and other service providers, governments and others about health coverage, benefit program design, funding, documentation, administration, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management and operations matters as well as for her work and thought leadership on a broad range of other health, employee benefits, human resources and other workforce, insurance, tax, compliance and other matters. Her experience encompasses leading and supporting the development and defense of innovative new programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares shared her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, Past Group Chair, current Defined Contribution Plan Committee Co-Chair, former Welfare Committee Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Counsel, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email to here or via telephone to (469) 767-8872.
About Solutions Law Press
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.SolutionsLawPress.com.
If you or someone else you know would like to receive future updates and notices about other upcoming Solutions Law Press™ events, please be sure that we have your current contact information – including your preferred e-mail by creating or updating your profile here. For important information concerning this communication, see here.
NOTICE: Any party accessing or using any content obtained from or through Solutions Law Press, Inc.™ acknowledges and agrees that any and all programs, publications, statements and materials presented or published by Solutions Law Press, Inc.™ and any statements or other contents made or contained therein are for general informational and educational purposes only. They are generic in nature and not tailored or intended to be relied upon by any person, business, entity or other party for purposes for determining the legal, financial or other appropriateness, defensibility, suitability, outcome or consequences of any strategy, action, course of action, or any other facts, circumstances, event or conduct. Users of these resources are responsible at all times for independently evluating the suitability of any content, materials, tools or other materials or information accessed from or through Solutions Law Press, Inc. directly or indirectly.
Solutions Law Press, Inc.™ and its authors and contributors do not represent or warrant in any form or manner, and expressly disclaim and deny the appropriateness of the use or reliance of any person or entity on any content, tools or resources accessed or obtained from or through Solutions Law Press, Inc.™ for any general or particular use or purpose by any party under any circumstances.
Likewise, they do not establish an attorney-client relationship or other fiduciary, contractual or other relationship between Solutions Law Press, Inc. and/or any of its authors or contributors and any other party. They are not, and do not serve as a substitute for legal, accounting, tax or other advice. They don’t create or otherwise give rise to any duty, obligation, responsibility on behalf of Solutions Law Press, Inc™ or any provider or offeree of content, tools or services to any party.
Parties accessing or using any of Solutions Law Press, Inc.™ competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The publisher and the author expressly disclaim all liability for this content and any responsibility to provide any update or otherwise notify anyone of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
©2017 Cynthia Marcotte Stamer. Non-Exclusive License To Republish Granted To Solutions Law Press.
 Comments Off on IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties |
Comments Off on IRS Updates Amounts Used To Calculate 2017 Obamacare Individual Individual Shares Responsibility Tax Penalties |  4980D, 4980H, 6039D, ACA, Affordable Care Act, Employee Benefits, Employer, Employers, Excise Tax, health benefit, Health Benefits, health Care, Health Care Reform, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Revenue Code, IRC, Patient Protection & Affordable Care Act, Premium Subsidies, Tax, Uncategorized | Tagged: ACA, Health Insurance, Health Plans, individual shared responsibility tax, Obamacare |
4980D, 4980H, 6039D, ACA, Affordable Care Act, Employee Benefits, Employer, Employers, Excise Tax, health benefit, Health Benefits, health Care, Health Care Reform, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Revenue Code, IRC, Patient Protection & Affordable Care Act, Premium Subsidies, Tax, Uncategorized | Tagged: ACA, Health Insurance, Health Plans, individual shared responsibility tax, Obamacare |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 1, 2017
Employers and employee benefit plan fiduciaries and administrators should consider sharing the free IRS Withholding Calculator resource offered in English, Spanish, and ASL formats with workers in annual employee benefit enrollment packages, new hire paperwork, bonus announcement and other wage related materials and other employee communications to help workers better understand and manage the tax and other effects of their annual employee benefit elections on their take-home pay. Including reminders to re-evaluate withholding and if necessary, change their W-4 withholding elections also helps employees and their families ensure that withholding elections that workers complete as part of new hire documentation are updated in response to changing taxable income and other relevant events.
Communicating the availability of these free government-resource tools to workers during the annual employee benefit plan enrollment period, year-end, raise or bonus time or other strategic times throughout the year could help employees better appreciate the tax-preferred benefit offerings provided by the employer as well as provide significant financial education benefits many workers need for little or no employer cost.
While enrollment packages typically tout the potential “tax savings” that employees can enjoy from participating in tax-favored, employer-sponsored health, group term life, qualified pension or profit-sharing, and other tax-preferred employee benefit or fringe benefit programs offered by their employers, few employees truly understand how to determine properly their necessary wage withholding on taxable wages, much less the specific effects of their employee benefit elections on their income or employment tax liability or withholding.
A better understanding of the relative tax benefits and savings of enrollment in tax-preferred benefits offered by an employer and their potential implications on the income tax withholding elected by the workers can benefit both employees and their employer. Aside from illustrating in real, meaningful terms specific to the worker the tax benefits of his election of employer-offered, tax preferred benefits, proper tax withholding helps employees avoid unnecessary over withholding that can reduce employees’ take-home pay as well as helps protect employees from unexpectedly higher year-end tax bills that often surprise workers when an employee sets his withholding too low.
While few employers or plans want to incur the potential financial costs or liability of estimating savings for individual workers, sharing information about free government-provided resources like the IRS calculator or using vendor-provided solutions that incorporate tools in employee enrollment and other communications can help employees appreciate the benefits of tax-preferred employee benefits and make more informed choices about their benefits and their withholding.
Educating employees about the availability of these free resources also is a low-cost way of providing valuable information to workers whether or not the employer or plan has a vendor offered solution that includes the same or similar tool. However, educating workers about the availability of the withholding calculator and other tools can be a particularly attractive option for an employer when the employer doesn’t have a vendor-provided option that includes that information or can only access the tool for added charges.
While many vendors offer similar tools and materials sold to employers and employee benefit plans, employers or benefit plan fiduciaries generally must pay fees, share promotional materials or meet at the requirements to deliver those resources as part of a vendor-supplied package. Utilizing these vendor supplied resources without fulfilling these preconditions could expose the employer or plan to potential copyright, trademark or other contractual or intellectual property claims from the vendor. In contrast, IRS withholding calculator and many other government tools can be used or shared freely without these concerns. Moreover, employers and plans are less likely to face challenges for sharing an unfiltered government resource than a similar tool packaged within a vendor communication package promoting other options.
Of course, regardless of whether these or other tools or information are shared as a free-standing tool or as part of a broader communication package, employers, plans and others sharing these government tools and other similar resources generally will want to ensure that the materials are distributed along with and subject to general tax advice and other disclaimers of reliance as well as statements encouraging users to consult with their own qualified tax or other qualified professionals about the users’ specific circumstance.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for management work, coaching, teachings, and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality, governmental and other highly regulated employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service as a management consultant, business coach and consultant and policy strategist as well through her leadership participation in professional and civic organizations such her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and policy adviser to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; ABA Real Property Probate and Trust (RPTE) Section former Employee Benefits Group Chair, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative, and Defined Contribution Committee Co-Chair, past Welfare Benefit Committee Chair and current Employee Benefits Group Fiduciary Responsibility Committee Co-Chair, Substantive and Group Committee member, Membership Committee member and RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a widely published author, highly popular lecturer, and serial symposia chair, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other leadership, performance, regulatory and operational risk management, public policy and community service concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ For information about republication, please contact the author directly. All other rights reserved.
 Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |
Comments Off on Withholding Calculator Tool Helps Workers Figure Withholding |  105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |
105(h), 401(k), Affordable Care Act, Brokers, Cafeteria Plans, compensation, compliance, Corporate Compliance, Default enrollment, defined benefit plan, Defined Benefit Plans, Defined Contribution Plans, Disability, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, Executive Compensation, FICA, fiduciary duty, Form 5500, HR, Human Resources, Income Tax, Insurance, Managment, Tax, Tax Qualification, Uncategorized, Worker, Workforce | Tagged: Employee Benefits, employee communications, Health Insurance, Human Resources, Income Tax, onboarding, Tax, Withholding, Workforce |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
July 7, 2017
July 13 is the deadline to comment on a Occupational Safety and Health Administration (OSHA) proposed rule that would delay four months the compliance date of its electronic reporting rule, formally called “Improve Tracking of Workplace Injuries and Illnesses.” The compliance date would be extended from July 1, 2017, to Dec. 1, 2017 to allow OSHA to further review and consider its final rule the Obama Administration previously published on May 12, 2016. The rule requires certain employers to submit their employee injury and illness logs to OSHA electronically.
Employers and others that support the rule should act promptly to express their support in the form of a comment by the July 13 deadline.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, safety and occupational injury, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, occupational health and safety, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality and governmental employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Comment By 7/13 On OSHA Proposed Electronic Reporting Rule Delay To 12/1/17 |
Comments Off on Comment By 7/13 On OSHA Proposed Electronic Reporting Rule Delay To 12/1/17 |  compliance, Corporate Compliance, Employment, HR, Human Resources, Internal Investigations, occupational safety, OSHA, Uncategorized |
compliance, Corporate Compliance, Employment, HR, Human Resources, Internal Investigations, occupational safety, OSHA, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
June 22, 2017
Register Now To Participate In
“2017 Federal Group Health Plan Mental Health Rules Update”
Solutions Law Press, Inc™ Health Plan Update WebEx Briefing
Tuesday, June 27, 2017
10:30 A.M.-11:30 P.M. Eastern | 11:30 A.M.-12:30 P.M. Central
EXPANDING REGULATORY REQUIREMENTS & ENFORCEMENT SPELL TROUBLE FOR HEALTH PLANS AND THEIR SPONSORING EMPLOYERS.
Solutions Law Press, Inc.™ invites employer and other group health plan sponsors, fiduciaries, insurers, administrative service providers, plan brokers and consultants are invited learn critical information about their expanding risks and responsibilities arising from existing and proposed changes to rules and enforcement of federal group health plan mental health and substance abuse (MH/SUB) coverage and privacy rules under the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA), as supplemented by the Patient Protection and Affordable Care Act (ACA) and the 21st Century Cures Act (Cures Act) and the Privacy Rules of the Health Insurance Portability & Accountability Act (HIPAA) conducted by attorney Cynthia Marcotte Stamer, a Fellow in the American College of Employee Benefits recognized as among the “Best Lawyers” in employee benefits for her health and other benefit knowledge, experience, policy advocacy and thought leadership. Register here now!
Tightening Health Plan Mental Health & Substance Abuse Rules & Enforcement Make Group Health Plan Compliance Critical
New and proposed guidance jointly published June 16, 2017 by the Departments of Labor (DOL), Health & Human Services (HHS) and Treasury is the latest in a series of regulatory and enforcement developments over the past year alerting group health plans and their employer and other group health plan sponsors, fiduciaries, insurers, administrative services providers, plan brokers and consultants involved in health plan design, funding, or administration to get serious about their group health plans’ compliance with the MHPAEA federal group health plan mental health and substance abuse coverage and benefit requirements, as supplemented by the ACA and the Cures Act without running afoul of the Privacy Rules of HIPAA.
Building upon federal group health plan mental health parity mandates originally implemented under the Mental Health Parity Act, the MHPAEA generally requires that any financial requirements or treatment limitations group health plans impose on mental health and substance use disorder (MH/SUD) benefits not be restrictive than the predominant financial requirements and treatment limitations that apply to substantially all medical and surgical benefits. MHPAEA also imposes several disclosure requirements on group health plans and health insurance issuers. Not satisfied with the MHPAEA coverage and disclosure protections, however, Congress subsequently broadened federal MH/SUD benefit rights under group health plans through the enactment of the ACA and the Cures Act. Congress also has imposed special requirements and protections for mental health treatment records adds additional responsibilities for group health plans and their service providers when dealing with information and records in connection with the administration of MH/SUD benefits.
After a long period of lax oversight and enforcement of these federal group health plan mental health rules, the Departments of Labor (DOL), Health and Human Services (HHS), and the Treasury (collectively, the Departments) since October, 2016 have begun both tightening the rules and acting to increase oversight and enforcement. The Departments have issued a series of joint guidance clarifying and broadening their interpretations of these MH/SUD benefit and disclosure mandates while simultaneously taking steps to increase awareness and enforcement of these rights. As part of these ongoing efforts, Departments’ on June 16, 2017 expanded this guidance with their publication of new Mental Health Parity Implementation FAQs Part 38 discussing their joint interpretation of the broadening effect of the enactment of the ACA and the Cure Act on these plan requirements. Concurrently, the Departments signaled their intention to add additional responsibilities for group health plans and insurers by publishing along with FAQ Part 38 a Draft MHPAEA Disclosure Template and request for comments. This latest guidance package reaffirms that the Departments are continuing efforts to increase oversight of and enforcement of MH/SUD compliance against group health plans, their sponsors, fiduciaries, insurers, and their administrative and other service providers. In the face of these developments and the reported initiation of enforcement actions by the Departments, the group health plans, their employer and other sponsors, fiduciaries, insurers, and their administrative and other service providers should move quickly to understand and update their plans and practices to comply with these recent developments while bracing for the likely need to deal with further expanded disclosure and other additional responsibilities under the MHPAEA jointly proposed by the Departments on June 16, 2017.
Beyond fulfilling these expanding MHPAEA responsibilities, health plan fiduciaries, administrators, insurers and sponsors also must ensure their health plan and its business associates comply with special rules concerning the protection, use and disclosure of mental health treatment records and information that may impact certain mental health treatment and other records received, used, retained or disclosed in the course of administering mental health, substance abuse or other provisions of their group health plans under the HIPAA Privacy Rules. Keeping in mind that HHS audit and enforcement of compliance by health plans and other HIPAA covered entities with HIPAA’s medical privacy and data security rules, health plan sponsors, fiduciaries, insurers and administrative and other service providers also should take the opportunity to verify that their plans and practices comply with special HIPAA rules impacting authorizations and other dealings with certain mental health and substance abuse health information and records and other HIPAA medical privacy and security requirements.
Given these developments, group health plans, their sponsors, fiduciaries, insurers and administrator must take steps to verify and maintain compliance with these federal MH/SUD requirements. Ensuring proper compliance with these federal rules is particularly important to avoid triggering the substantial liability that health plans, their employer and other sponsors, insurers, and administrators can incur if their health plan violates these mandates. Obviously, plans and their sponsors, insurers and fiduciaries can expect to pay additional plan expenses necessary to pay wrongfully denied benefits and other expenditures these plan or its fiduciaries expend to investigate, defend and resolve claims or compliance audits, investigations, litigation or actions brought by the Departments, state insurance regulators with respect to state governments or insurers, or private litigation by participants or beneficiaries. Many employer or other plan sponsors may be unaware that these violations also generally expose employers and other health plan sponsors to liability to self identify, self-report on Internal Revenue Service Form 8928 and self-pay and excise tax of up to $100 per participant per day per uncorrected violation by the due date for filing of their annual corporate tax return.
With oversight and enforcement already rising and the Departments proposing to expand further both disclosure duties and enforcement, group health plans, their employer and other sponsors, insurers, fiduciaries and administrators clearly need to take prompt action to verify their existing health plan provisions and administrative practices are up-to-date and administered to withstand challenge from the Departments, participants, beneficiaries, health care providers and others. Consequently, employer and other group health plan sponsors, fiduciaries, insurers, administrative services providers, plan brokers and consultants involved in health plan design, funding, or administration should act quickly to verify their plan terms and practices are updated to comply with existing rules and share their input in response to the Departments June 16, 2017 requests for comments.
ABOUT CYNTHIA MARCOTTE STAMER
Recognized as “Legal Leader™ Texas Top Rated Lawyer” in both Health Care Law and Labor and Employment Law, a “Texas Top Lawyer,” and an “AV-Preeminent” and “Top Rated Lawyer” by Martindale-Hubble, singled out as among the “Best Lawyers In Dallas” in employee benefits by D Magazine; Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely recognized for her nearly 30 years’ of work and pragmatic thought leadership, publications and training on health coverage and health care, health plan and employee benefits, workforce and related regulatory and other compliance, performance management, risk management, product and process development, public policy, operations and other concerns.
Throughout her legal and consulting career, Ms. Stamer has drawn recognition for combining extensive knowledge and experience with her talents as an insightful innovator and problem solver when advising, representing and defending employer and other plan sponsors, insurers, fiduciaries, insurers, electronic and other technology, plan administrators and other service providers, governments and others about health coverage, benefit program design, funding, documentation, administration, data security and use, contracting, plan, public and regulatory reforms and enforcement, and other risk management and operations matters as well as for her work and thought leadership on a broad range of other health, employee benefits, human resources and other workforce, insurance, tax, compliance and other matters. Her experience encompasses leading and supporting the development and defense of innovative new programs, practices and solutions; advising and representing clients on routine plan establishment, plan documentation and contract drafting and review, administration, change and other compliance and operations crisis prevention and response, compliance and risk management audits and investigations, enforcement actions and other dealings with the US Congress, Departments of Labor, Treasury, Health & Human Services, Federal Trade Commission, Justice, state legislatures, attorneys general, insurance, labor, worker’s compensation, and other agencies and regulators, She also provides strategic and other supports clients in defending litigation as lead strategy counsel, special counsel and as an expert witness.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares shared her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE; Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, Past Group Chair, current Defined Contribution Plan Committee Co-Chair, former Welfare Committee Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Counsel, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, the Society of Professional Benefits Administrators, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients, serves on the faculty and planning committee of many workshops, seminars, and symposia, and on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email to here or via telephone to (469) 767-8872.
About Solutions Law Press
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.SolutionsLawPress.com.
If you or someone else you know would like to receive future updates and notices about other upcoming Solutions Law Press™ events, please be sure that we have your current contact information – including your preferred e-mail by creating or updating your profile here. For important information concerning this communication, see here.
NOTICE: Any party accessing or using any content obtained from or through Solutions Law Press, Inc.™ acknowledges and agrees that any and all programs, publications, statements and materials presented or published by Solutions Law Press, Inc.™ and any statements or other contents made or contained therein are for general informational and educational purposes only. They are generic in nature and not tailored or intended to be relied upon by any person, business, entity or other party for purposes for determining the legal, financial or other appropriateness, defensibility, suitability, outcome or consequences of any strategy, action, course of action, or any other facts, circumstances, event or conduct. Users of these resources are responsible at all times for independently evluating the suitability of any content, materials, tools or other materials or information accessed from or through Solutions Law Press, Inc. directly or indirectly.
Solutions Law Press, Inc.™ and its authors and contributors do not represent or warrant in any form or manner, and expressly disclaim and deny the appropriateness of the use or reliance of any person or entity on any content, tools or resources accessed or obtained from or through Solutions Law Press, Inc.™ for any general or particular use or purpose by any party under any circumstances.
Likewise, they do not establish an attorney-client relationship or other fiduciary, contractual or other relationship between Solutions Law Press, Inc. and/or any of its authors or contributors and any other party. They are not, and do not serve as a substitute for legal, accounting, tax or other advice. They don’t create or otherwise give rise to any duty, obligation, responsibility on behalf of Solutions Law Press, Inc™ or any provider or offeree of content, tools or services to any party.
Parties accessing or using any of Solutions Law Press, Inc.™ competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The publisher and the author expressly disclaim all liability for this content and any responsibility to provide any update or otherwise notify anyone of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
©2017 Solutions Law Press. All rights reserved.
 Comments Off on Learn About Rising Group Health Plan Mental Health Mandate Risks From 6/27 “2017 Federal Group Health Plan Mental Health Rules Update” |
Comments Off on Learn About Rising Group Health Plan Mental Health Mandate Risks From 6/27 “2017 Federal Group Health Plan Mental Health Rules Update” |  4980D, 6039D, ACA, Affordable Care Act, Appeals, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Claims Administration, compensation, compliance, conflict of interest, Corporate Compliance, corporate governance, Data Breach, Data Security, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, Exempt, fiduciary duty, Fiduciary Responsibility, H.R. 4872, health reform, HIPAA, HR, Human Resources, Identity Theft, Income Tax, Insurance, insurers, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Protection & Affordable Care Act, Pay, Physician, Plan Admistrator, preventive care, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, SBC, Tax Credit, Uncategorized, Union | Tagged: ACA, Brokers, CCIIO, Corporate Compliance, EBSA, Employers, enforcement, Essential health benefits, Fiduciary, Fiduciary Duties, Health Benefits, health coverage, Health Plans, health reform, HHS, Mental Health, Mental Health Parity, mental health records, substance abuse, Third party Administrators |
4980D, 6039D, ACA, Affordable Care Act, Appeals, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Claims Administration, compensation, compliance, conflict of interest, Corporate Compliance, corporate governance, Data Breach, Data Security, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, Exempt, fiduciary duty, Fiduciary Responsibility, H.R. 4872, health reform, HIPAA, HR, Human Resources, Identity Theft, Income Tax, Insurance, insurers, Internal Revenue Code, IRC, Labor Management Relations, Management, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Protection & Affordable Care Act, Pay, Physician, Plan Admistrator, preventive care, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, SBC, Tax Credit, Uncategorized, Union | Tagged: ACA, Brokers, CCIIO, Corporate Compliance, EBSA, Employers, enforcement, Essential health benefits, Fiduciary, Fiduciary Duties, Health Benefits, health coverage, Health Plans, health reform, HHS, Mental Health, Mental Health Parity, mental health records, substance abuse, Third party Administrators |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 12, 2017
Solutions Law Press, Inc. editor and attorney Cynthia Marcotte Stamer will speak and moderate two key panel programs on health care privacy and data security scheduled at the Healthcare Privacy & Security Form hosted on May 19, 2017 by the Information Security Systems Association of Los Angeles County (ISSA-LA) as a component of its 9th Annual ISSA-LA Information Security Summit. The presentations of Ms. Stamer and others at the conference are particularly timely coming on the heels of the May 12 Cyber alerts to U.S. health industry and other businesses about the urgent need to defend against the spread of an epidemic international malware threat targeting U.S. healthcare and other businesses. See Urgent WannaCry Ransomware Cyber Warning Issued; Alert: Guard Health E-Mail, Other IT Against WannaCry Malware Attack.
The Medical Privacy & Security Summit is part of the 9th Annual ISSA-LA Information Security Summit scheduled for May 18-19, 2017 at the Universal City Hilton in Los Angeles. Recognized as a premier information security education and networking event, the Summit is expected to bring together 1000 or more health industry and other IT and InfoSec executives, leaders, analysts, and practitioners to learn from the experts, exchange ideas with their peers, and enjoy conversations with the community.
The Healthcare Privacy & Security Forum offered for the 5th year as a component of the annual Summit on May 19 specifically focuses on leading challenges, issues and opportunities confronted by health industry privacy and security professionals and their organizations. Ms. Stamer has served on the steering committee, moderator and popular faculty member for the 2017 Forum for the 5th consecutive year. During the 2017 Forum, she will moderate and speak on two panels:
- “Finding & Negotiating The Mine Fields: CISO, CIO & Privacy Officer’s Playbook for Promoting Compliance & Security Without Getting Fired,” a luncheon interactive panel discussion with the audience exploring the challenging mission CISOs, CIOs and Privacy Officers face to ensure their healthcare, financial and other critical information, data and systems continue to support the patient care and operating functions of their organizations, while at the same time defending these systems, operations and their sensitive, but mission critical data against malicious or innocent misappropriation, use, access or destruction; and
- The closing panel on “What Initiatives Are on the Horizon in Healthcare, and How Can We Secure Them?”, which will explore likely future emerging privacy and security threats and technologies, regulatory challenges and enforcement, and other trends that Privacy and Security professionals are likely to face and tips and strategies for preparing to leverage these likely new opportunities and manage new challenges.
Register or get the full schedule of programs and other events scheduled at the Healthcare Privacy & Security Forum specifically along with the overall Information Security Summit here.
About Ms. Stamer
Cynthia Marcotte Stamer is a Martindale-Hubble “AV-Preeminent (Top 1%) rated practicing attorney and management consultant, health industry public policy advocate, widely published author and lecturer, recognized for her nearly 30 years’ of work on health industry and other privacy and data security and other health care, health benefit, health policy and regulatory affairs and other health industry legal and operational as a LexisNexis® Martindale-Hubbell® “LEGAL LEADER™ and “Top Rated Lawyer,” in Health Care Law and Labor and Employment Law; a D Magazine “Best Lawyers In Dallas” in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law,” a Fellow in the American Bar Foundation, the Texas Bar Foundation and the American College of Employee Benefit Counsel.
Scribe for ABA JCEB annual agency meeting with OCR for many years, Ms. Stamer is well-known for her extensive work and leadership throughout her career on HIPAA, FACTA, PCI, IRC and other tax, Social Security, GLB, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and concerns. Ms. Stamer has worked extensively throughout her career with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks, insurers and other financial institutions, and others on trade secret confidentiality, privacy, data security and other risk management and compliance including design, establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, drafting and negotiation of business associate, chain of custody, confidentiality, and other contracting; risk assessments, audits and other risk prevention and mitigation; investigation, reporting, mitigation and resolution of known or suspected breaches, violations or other incidents; and defending investigations or other actions by plaintiffs, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others; reporting known or suspected violations; commenting or obtaining other clarification of guidance and other regulatory affairs, training and enforcement, and a host of other related concerns.
Her clients include public and private health care providers, health insurers, health plans, employers, payroll, staffing, recruitment, insurance and financial services, health and other technology and other vendors, and others.
Author of a multitude of highly-regarded works and training programs on HIPAA and other data security, privacy and use published by BNA, the ABA and other premier legal industry publishers In addition to representing and advising these organizations, she also speaks extensively and conducts training on health care and other privacy and data security and many other matters Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
Beyond these involvements, Ms. Stamer also is active in the leadership of a broad range of other professional and civic organizations. Through these and other involvements, she helps develop and build solutions, build consensus, garner funding and other resources, manage compliance and other operations, and take other actions to identify promote tangible improvements in health care and other policy and operational areas.
For additional information about Ms. Stamer, see here or contact Ms. Stamer directly by e-mail here or by telephone at (469) 767-8872. ©2017 Cynthia Marcotte Stamer. Limited, non-exclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Stamer To Moderate, Talk Medical CyberSecurity At 5/19 ISSA-LA IT Security Meedical Privacy Forum |
Comments Off on Stamer To Moderate, Talk Medical CyberSecurity At 5/19 ISSA-LA IT Security Meedical Privacy Forum |  ADA, ARRA, board of directors, Brokers, Child Safety, Civil Monetary Penalties, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, EBSA, Educational Privacy, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, EMR, ERISA, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, FINRA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Internet, Management, Mental Health, officers, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Public Policy, Security, Technology, third party administrators, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Security, Information Security, IT, medical data, Medical Privacy, medical security, Protected Health Information, speech |
ADA, ARRA, board of directors, Brokers, Child Safety, Civil Monetary Penalties, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, EBSA, Educational Privacy, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, EMR, ERISA, FACTA, Fair Credit Reporting Act, FICA, fiduciary duty, FINRA, Government Contractors, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Internet, Management, Mental Health, officers, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Public Policy, Security, Technology, third party administrators, Uncategorized | Tagged: Cyber Security, Cybercrime, Data Security, Information Security, IT, medical data, Medical Privacy, medical security, Protected Health Information, speech |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 10, 2017
Healthcare providers, health plans, healthcare clearinghouses and their business associates (Covered Entities) can’t disclose the name or other protected health care information about a patient in press releases or other announcements without prior authorization from the patient. That’s the clear lesson Covered Entities should learn from the $2.4 million payment to the U.S. Department of Health and Human Services (HHS) that the largest not-for-profit health system in Southeast Texas, Memorial Hermann Health System (MHHS) is paying to settle charges it violated the Health Insurance Portability and Accountability Act (HIPAA) Privacy Rule by issuing a press release with the name and other protected health information (PHI) about a patient without the patient’s prior HIPAA-compliant authorization under a Resolution Agreement and Corrective Action Plan (Resolution Agreement) announced May 10, 2017 by HHS Office of Civil Rights (OCR).
The Resolution Agreement resolves OCR charges the operator of 13 hospitals, eight Cancer Centers, three Heart & Vascular Institutes, and 27 sports medicine and rehabilitation centers violated the Privacy Rule that resulted from an OCR compliance review of MHHS triggered by multiple media reports suggesting that MHHS improperly disclosed the name and other details about a patient arrested and charged with presenting an allegedly fraudulent identification card to office staff at an MHHS’s clinic after MHHS clinic staff alerted law enforcement of suspicions the patient was presenting false identification to the clinic. According to OCR, after law enforcement investigated and arrested the patient, MHHS published a press release concerning the incident in which MHHS senior management approved the impermissible disclosure of the patient’s PHI by adding the patient’s name in the title of the press release without securing prior authorization of the patient.
While OCR concluded the report to law enforcement allowable under the Privacy Rule, OCR found MHHS violated the Privacy Rule by issuing the press release disclosing the patient’s name and other PHI without authorization from the patient and also by failing to timely document the sanctioning of its workforce members for impermissibly disclosing the patient’s information.
To resolve and avoid the potential Civil Monetary Penalties that HIPAA could authorize OCR to impose for the alleged Privacy Rule violation, MHHS agrees in the Resolution Agreement to pay OCR a $2.4 million monetary settlement and implement a corrective action plan that obligates MHHS to update and train its workforce on its policies and procedures on safeguarding PHI from impermissible uses and disclosures including specific instructions and procedures to:
- Address (a) Uses and disclosures for which an authorization is required, including to the media, to public officials, and on the internet; (b) Disclosures for law enforcement purposes; and (c) Uses and disclosures for health oversight activities;
- Identify MHHS personnel or representatives whom workforce members, agents, or business associates may contact in the event of any inquiry or concern regarding compliance with HIPAA in relation to these activities;
- Internal reporting procedures requiring all workforce members to report to the designated person or office at the earliest possible time any potential violations of the Privacy, Security or Breach Notification Rules or of MHHS’ privacy and security policies and procedures and MHHS promptly to investigate and address all received reports in a timely manner; and
- Application and documentation of appropriate sanctions (which may include retraining or other instructive corrective action, depending on the circumstances) against members of MHHS’ workforce, including senior level management, who fail to comply with the Privacy, Security or Breach Notification Rules or MHHS’ privacy and security policies and procedures, including a description of the sanctions; a timeframe in which MHHS will apply and document sanctions for violations of the HIPAA Rules or of MHHS’ privacy, security or breach policies or procedures; the manner in which MHHS will document the sanctions; and where MHHS will store or retain such documentation (e.g., personnel file).
The corrective action plan in the Resolution Agreement also requires all MHHS facilities to attest to their understanding of permissible uses and disclosures of PHI, including disclosures to the media and others.
Covered entities should keep in mind the MHHS Resolution Agreement is the latest in a series of OCR enforcement actions and resolution agreements highlighting the need for Covered Entities to adopt and use appropriate policies and procedures to prevent wrongful disclosures of PHI to the media or public. For instance, in June, 2013, OCR required Shasta Regional Medical Center (SRMC) to pay a $275,000 settlement payment and implement a comprehensive corrective action plan to resolve OCR charges stemming from SRMC’s disclosure of PHI about a patient to members of the media and its workforce in an effort to respond to accusations the patient made that SRMC engaged in fraud and other misconduct. See HIPAA Sanctions Triggered From Covered Entity Statements To Media, Workforce. In contrast, the $2.2 million resolution agreement that OCR required New York Presbyterian Hospital for improperly allowing a film crew to film hospital patients in violation of HIPAA was almost 10 times greater than the SRMC penalty and was accompanied by OCR’s publication OCR of specific additional guidance warning Covered Entities against improper disclosures to the media. See $2 Million+ HIPAA Settlement, FAQ Warn Providers Protect PHI From Media, Other Recording Or Use.
Following on the heels of this previous guidance and prior enforcement actions warning Covered Entities against wrongful disclosure to the media, the MHHS Resolution Agreement sends a strong message to Covered Entities that they should expect little sympathy if their organizations improperly share PHI with the media. OCR’s announcement of the MHHS Resolution Agreement, for instance quotes OCR Director Roger Severino with stating that “Senior management should have known that disclosing a patient’s name on the title of a press release was a clear HIPAA Privacy violation that would induce a swift OCR response.” The announcement goes on to quote Director Severino further as stating, “This case reminds us that organizations can readily cooperate with law enforcement without violating HIPAA, but that they must nevertheless continue to protect patient privacy when making statements to the public and elsewhere.”
Conduct Entity-Wide Risk Assessment & Review & Tighten Media Relations Policies, Processes & Training ASAP
Covered entities should heed the warning by conducting a risk assessment of their organization’s susceptibility to potential improper disclosures to media or others and reviewing and implementing necessary written policies, procedures and training to prevent the improper disclosure of patient PHI to media or others unless the Covered Entity either secures prior HIPAA-compliant authorization from the patient or can prove the disclosure falls squarely under an exception to the Privacy Rule’s prohibition against disclosure of PHI without authorization except as allowed by the Privacy Rule.
Taking these and other needed steps to evaluate, and strengthen and enforce as needed, risk assessments, policies, procedures, and training to prevent wrongful use, access or disclosure of PHI to the media or others is particularly critical in light of the ongoing tightening of expectations, and rising enforcement and sanctions for HIPAA violations since Congress amended HIPAA in 2009. See OCR Audit Program Kickoff Further Heats HIPAA Privacy Risks; HIPAA Heats Up: HITECH Act Changes Take Effect & OCR Begins Posting Names, Other Details Of Unsecured PHI Breach Reports On Website.
Based on experiences reported in the MHHS and other similar resolution agreements, Covered Entities also generally will want to ensure that their policies, procedures and training extend to all potential sources of communications that could involve patient information and make clear that the Privacy Rule restrictions must be followed even if the circumstances involve allegations of misconduct, special performance by healthcare providers or others that it would benefit the organization or certain individuals to have known to the public, or other circumstances likely to be of interest to the media or other parties.
As part of this process, covered entities should ensure they look outside the four corners of their Privacy Policies to ensure that appropriate training and clarification is provided to address media, practice transition, workforce communication and other policies and practices that may be covered by pre-existing or other policies of other departments or operational elements not typically under the direct oversight and management of the Privacy Officer such as media relations. Media relations, physician and patients affairs, outside legal counsel, media relations, marketing and other internal and external departments and consultants dealing with the media, the public or other inquiries or disputes should carefully include and coordinate with the privacy officer both to ensure appropriate policies and procedures are followed and proper documentation created and retained to show authorization, account, or meet other requirements.
In conducting this analysis and risk assessment, it will be important that Covered Entities include, but also look beyond the four corners of their Privacy Policies to ensure that their review and risk assessment identifies and assesses and addresses compliance risks on an entity wide basis. This entity-wide assessment should include both communications and requests for information normally addressed to the Privacy Officer as well as requests and communications that could arise in the course of media or other public relations, practice transition, workforce communication and other operations not typically under the direct oversight and management of the Privacy Officer. For this reason, Covered Entities also generally will not only to adopt and implement specific policies, processes and training in these other departments to prohibit and prevent inappropriate disclosures of PHI in the course of those departments operations. It also may be advisable to pre-established processes for reviewing media or other communications for potential PHI content and require prior review of any proposed public relations and other internal or external communications containing patient PHI or other information by the privacy officer, legal counsel or another suitably qualified party.
Because of the high risk that the preparation or review of media or other public communications reports will involve the use and disclosure of PHI, Covered Entities also generally should verify that all outside media or public relations, legal, or other outside service providers participating in the investigation, response or preparation or review of communications to the media or others both are covered by signed business associate agreements that fulfill the Privacy Rule and other requirements of HIPAA as well as possess detailed knowledge and understanding of the Privacy and Security Rules suitable to participate in and help safeguard the Covered Entity against violations of these and other Privacy Rules. See e.g., Latest HIPAA Resolution Agreement Drives Home Importance Of Maintaining Current, Signed Business Associate Agreements.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to manage and defend compliance, public policy, regulatory, staffing and other operations and risk management concerns. A core focus of this work includes work to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; dealings with JCHO and other accreditation and quality organizations; investigation and defense of private litigation and other federal and state health care industry investigations and enforcement; insurance or other liability management and allocation; process and product development; managed care, physician and other staffing, business associate and other contracting; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.
Author of leading works on HIPAA and other privacy and data security works and the scribe leading the American Bar Association Joint Committee on Employee Benefits Annual Agency Meeting with OCR, her experience includes extensive compliance, risk management and data breach and other crisis event investigation, response and remediation under HIPAA and other data security, privacy and breach laws. Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly regarded works and training programs on trade secret, HIPAA and other medical, consumer, insurance, tax, and other privacy and data security, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns.
In connection with this work, Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA, FACTA, trade secret and other information privacy and data security rules, including the establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and enforcement, and a host of other related concerns. Her clients include public and private health care providers, health insurers, health plans, technology and other vendors, and others.
Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, MGMA, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked closely with a diverse range of physicians, hospitals and healthcare systems, DME, Pharma, clinics, health care providers, managed care, insurance and other health care payers, quality assurance, credentialing, technical, research, public and private social and community organizations, and other health industry organizations and their management deal with governance; credentialing, patient relations and care; staffing, peer review, human resources and workforce performance management; outsourcing; internal controls and regulatory compliance; billing and reimbursement; physician, employment, vendor, managed care, government and other contracting; business transactions; grants; tax-exemption and not-for-profit; licensure and accreditation; vendor selection and management; privacy and data security; training; risk and change management; regulatory affairs and public policy and other concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health plans, health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other “nonpar,” insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
 Comments Off on $2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others |
Comments Off on $2.4M HIPAA Settlement Message Warns Health Plans & Providers Against Sharing Medical Info With Media, Others |  ADA, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Civil Rights, compliance, conflict of interest, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, Disability Discrimination, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, Employment, EMR, ERISA, Fair Credit Reporting Act, fiduciary duty, GINA, HIPAA, HIPAA, Hiring, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Leadership, LGBT, Management, Medicare Part D, Mental Health, Mental Health Parity, MEWA, Physician, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Technology, third party administrators, Uncategorized | Tagged: Health Care Provider, Health Plans, HIPAA, Medical Privacy, PHI, Privacy |
ADA, board of directors, Brokers, Cafeteria Plans, Civil Monetary Penalties, Civil Rights, compliance, conflict of interest, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, Disability Discrimination, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, Employment, EMR, ERISA, Fair Credit Reporting Act, fiduciary duty, GINA, HIPAA, HIPAA, Hiring, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Leadership, LGBT, Management, Medicare Part D, Mental Health, Mental Health Parity, MEWA, Physician, Prescription Drugs, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Technology, third party administrators, Uncategorized | Tagged: Health Care Provider, Health Plans, HIPAA, Medical Privacy, PHI, Privacy |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 10, 2017
While Congress continues to debate the future of the Obamacare health reforms and its exchanges, the Department of Health & Human Services is reminding employers with less than 50 employees that wish to offer group health coverage for their employees to check out their coverage options offered the Small Business Health Options Program (SHOP) Marketplace established as part of the Patient Protection and Affordable Care Act (ACA). Before or when offering health coverage for employees or their dependents, employers and their management should confirm they fully understand and appropriately arrange for fulfillment of all applicable federal, contractual and other requirements to avoid unfortunate and often expensive liabilities.
The SHOP Marketplace is intended to offer an opportunity for for small employers who want to provide health and dental insurance to their employees. Use of the SHOP Marketplace to obtain coverage may be an option for an employer if it is a business or non-profit organization with 50 or fewer full-time equivalent employees (FTEs). An employer that qualifies to get group health coverage through the SHOP doesn’t have to wait for an annual enrollment period; it can start offering SHOP insurance to your employees any time of year by completing the enrollment process by the applicable deadline prior to the first day of the month that the employer wants to start offering coverage through the SHOP.
In addition to the option to buy coverage through the SHOP, employers with 25 or fewer employees also may be eligible to use the Small Employer Health Care Credit created by the ACA to help defray the costs of providing this coverage to their qualifying employees. For instance, Monday, May 15 is the sign up deadline for small employers and nonprofit employees interested in obtaining small group health plan coverage for their employees through the the SHOP Marketplace beginning on June 1. See HealthCare.gov/Small-Business to enroll your small business or non-profit employees or get more details.
While many excellent reasons may exist for a business to offer group health coverage for qualifying employees, all employers regardless of size considering offering group health coverage obtained through the SHOP or other sources should keep in mind that employers that establish and maintain group health coverage, the group health plans they establish and the company or persons with discretionary authority or responsibility for the maintenance, management or administration of these programs or their plans are required to comply with a variety of federal tax, labor and other rules.
Businesses and their owners or management leaders making these decisions should confirm that they fully understand these responsibilities and take appropriate steps to ensure their fulfillment before establishing or maintaining a group health plan to avoid exposing their business, its management or owners or others to unexpected and often substantial liabilities that can result from violation of these requirements. While small employers plans sometimes qualify for some relief from a few of these requirements, depending on their size, the majority of these federal rules apply to most if not all group health plans. Furthermore, businesses sponsoring these programs and their leaders involved in deciding whether and what health coverage to offer for employees and their dependents should not presume that their organization, the resulting plan or its fiduciaries will fulfill these requirements simply by purchasing coverage through the SHOP Marketplace, directly from an insurer, or with the assistance of a broker or consultant. Fulfillment of applicable requirements generally requires that sponsoring employers and individuals within the management responsible for or appointed to oversee the program to take other steps. The scope of responsibility and resulting liability to a sponsoring employer and members of its ownership or management also typically are impacted by the plan design and contracts used to establish and maintain the program, its funding, and various other factors. These factors generally include contractual language in insurance, consulting or brokerage, administrative services and other contracts presented by vendors for use in purchasing and maintaining the program that often shift responsibility for many duties an employer otherwise might assume would be born by the vendor. For these and other reasons, most businesses and their leadership will want to consider arranging for their proposed program and its associated contracts and arrangements to be reviewed by legal counsel experienced in group health plan and associated labor, tax and other laws and arrangements.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality and governmental employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Leave a Comment » |
Leave a Comment » |  employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Leadership, Managment, MSHA, NLRA, Uncategorized | Tagged: Labor Law, labor-management relations, NLRA, Trump Administration |
employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Leadership, Managment, MSHA, NLRA, Uncategorized | Tagged: Labor Law, labor-management relations, NLRA, Trump Administration |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 25, 2017
While Congress and the Trump Administration continue to ponder and debate what if anything to do with the health care reforms of the Patient Protection and Affordable Care Act (ACA), employer and other health plan sponsors, health plan insurers, plan fiduciaries and others responsible for health plan design, administration or funding must take steps to verify their past and continuing compliance with the ACA and other federal mandates while laying the groundwork to respond quickly to any eventual reforms.
Regardless of what, if anything, the existing Congress or the Trump Administration does to repeal or reform the ACA or other federal health plan rules, all health plan sponsors, insurers, fiduciaries and administrators should act to mitigate their substantial and ever-growing health plan exposures by arranging for an independent compliance audit of their health plan terms, materials and operations for potential uncorrected past or current violations of the 40 federal mandates covered by the Form 8928 reporting and associated Internal Revenue Code excise tax liability exposure, as well as other applicable plan liabilities under the Employee Retirement Income Security Act (ERISA), the Social Security Act, the Internal Revenue Code and other federal laws within open statute of limitation periods.
The cost, complexity and riskiness of health plan sponsorship and administration has grown exponentially over the past two decades. Thanks to the ACA and the continuous stream of other federal laws and regulations implemented over the past 20 years, sponsoring employers, as well as their health plans and those responsible as fiduciaries for administering, funding and insuring these programs now face huge costs, responsibilities and liabilities. While the ACA substantially expanded the federal health plan mandates and liabilities, the ACA is not the lone cause and its amendment or repeal alone won’t fully resolve these risks prospectively or retrospectively insulate sponsoring employers, their plans or their fiduciaries and insurers from the liabilities and costs of compliance issues occurring before Congress repeals or amends the ACA.
Of particular note for employer and other sponsors of group health plans are the self-reporting and excise tax self-assessment and payment requirements for employers coupled with the companion responsibilities and liabilities fiduciaries, plan administrators and others face under these federal mandates make it important that employers and others sponsoring group health plans and their management or other leaders overseeing or participating in plan design or vendor selection, plan administration or other plan related activities get advice and help from qualified legal counsel experienced in health plan matters:
- To conduct an independent compliance review and risk assessment of their health plans,
- To recommend and assist in the performance of recommended steps to correct or mitigate risks from any potential past or existing violations or other exposures that have arisen or are likely to arise from existing contractual, plan design or other health plan actions;
- To explore the potential advisability of taking additional steps to prevent or mitigate health plan associated compliance or other risks going forward whether or not health reform happens; and
- To begin preparing to take advantage of any impending health care reforms by evaluating the requirements and procedures that existing plan terms, contracts, vendors and arrangements are likely to require to implement changes necessary to respond to any reforms as quickly and efficiently as possible.
Spring Clean Your Health Plan House
Since any reforms eventually enacted are unlikely to retroactively eliminate liability of employers, their health plans or fiduciaries for violations of federal health plan mandates, health plan terms, or associated contracts occurring before the effective date of reform, employer and other health plan sponsors, fiduciaries, insurers and administrators should begin by identifying, cleaning up any existing, unresolved, and preventing any new health plan compliance problems.
While overall compliance with applicable federal mandates and health terms generally should be the goal, employers or others sponsoring group health plans need to be particularly concerned with their responsibilities and potential liability under the Internal Revenue Code to self-identify, report and pay stiff excise tax penalties of $100 per day per violation of any of 40 federal health plan mandates imposed by the ACA and various other federal laws when the sponsor files its annual tax return.
This employer or other plan sponsor excise tax liability generally arises in addition to the liabilities that plans, their fiduciaries and their insures face for failing to administer and pay benefits under the plans in accordance with the listed 40 federal mandates, whether actually written into or imputed by operation of law into the plan, the costs of which sponsoring employers often will bear responsibility for funding in whole or in part pursuant to their contractual liabilities under the health plan contracts, as plan fiduciaries or both. See, Businesses Must Confirm & Clean Up Health Plan ACA & Other Compliance Following Supreme Court’s King v. Burwell Decision; More Work For Employers, Benefit Plans Following SCOTUS Same-Sex Marriage Ruling; 2016 & 2017 Health Plan Budgets, Workplans Should Anticipate Expected Changes To SBCs.
Sponsors and plan fiduciaries also need to be concerned about other risks beyond sponsoring employers’ excise tax liability exposures for sponsoring a non-compliant group health plan. Among other things, group health plans and their fiduciaries can face audits, litigation and enforcement actions by the Centers for Medicare & Medicaid Services and other health plans for improperly coordinating plan claims with other coverage as well as lawsuits from covered persons, their health care providers or other beneficiaries, the Department of Labor and CMS, or others seeking to enforce rights to benefits, penalties in the case of CMS or the Department of Labor, and attorneys’ fees and other costs of enforcement. Beyond benefit litigation, the employer or representatives of the sponsoring employer, if any, named or acting as fiduciaries, insurer or third-party service providers named or acting as fiduciaries, also could face fiduciary lawsuits seeking damages, equitable relief, and attorneys’ fees and costs of court, for failing to prudently administer the plan in accordance with its terms and the law brought by covered persons or their beneficiaries or the DOL as well as fiduciary breach penalties if the fiduciary breach action is brought by the DOL. If the plan fails to comply with claims and appeals procedures or other ERISA notification requirements, parties named or functioning as the plan administrator for this purpose also could face penalties of up to $125 per violation per day in the case of enforcement actions brought by participants and beneficiaries or $1025 per violation per day in the case of actions brought by the DOL, plus attorneys’ fees and other costs of enforcement. Unless the employer previously took steps to draft its health plan documents and negotiate its vendor contracts to provide otherwise, most vendor provided plans typically assign these liabilities to the sponsoring employer or a member of its management by naming that employer or the management person the “plan administrator” and/or “named fiduciary” responsible for those activities and liabilities, requiring the plan sponsor to indemnify the vendor for costs and liabilities arising from the performance of actions under the plan even when those actions don’t comply with ERISA fiduciary or other legal standards applicable to the performance of those duties under the plan, or both, and other contractual or plan provisions that shift liabilities and costs to the plan sponsor.
To mitigate their exposure to these liabilities and costs, employer or other health plan sponsors should consider arranging for an independent legal compliance and risk assessment of their health plan, its terms, materials and operations to help mitigate the sponsoring employer’s exposure to self-identify, self-report on IRS Form 2848 and pay the $100 per day per violation excise tax liability now generally required under the Internal Revenue Code for any such violation.
Beyond mitigating a plan sponsor’s Form 8928 reporting and associated excise tax exposures, an independent compliance audit also can mitigate other risks and exposures for the sponsoring employer, the plan and its fiduciaries, the cost of which the sponsoring employer often bears financial responsibility for funding pursuant to the contractual indemnification and funding obligations entered into in connection with the establishment and maintenance of the plan, the fiduciary role, if any, of the employer with respect to the plan, or both. Accordingly, a timely and appropriate review is likely to help mitigate other risks and liabilities such as:
- Fiduciary liability that can arising from failing to administer the plan in accordance with these and other federal health plan mandates under ERISA;
- Unanticipated benefit costs and liabilities, which for self-insured plans are likely to be particularly burdensome if compliance issues are not identified and corrected before applicable deadlines to pay and submit claims to the stop-loss or other insurer expire (usually at or shortly after the close of a plan year or if earlier, contract termination);
- Benefit costs and penalties for wrongful coordination of benefits with Medicare, Medicaid, DOD and certain other plans or coverage in violation of Secondary Payer and other mandates; and
- Costs of defending and settling audits, litigation and other government or participant enforcement actions.
Since prompt self-audit and correction can help mitigate all of these liabilities, business leaders of employers sponsoring health plans should act promptly to engage experienced legal counsel experienced with health plan laws and operations to advise the plan sponsor about how to audit their group health plan’s plan documents, materials and operations for compliance with these and other federal health plan rules within the scope of attorney-client privilege while managing tax, financial, benefit and fiduciary liability exposures to deal with potential compliance concerns that the review might discover as well as mitigate risks that could result if the audit is improperly structured or conducted.
Prepare To Respond To Potential Health Reform & Other Health Plan Improvement
Beyond identifying and addressing existing compliance concerns and other risks associated with prior or existing plan design or administration, most employer and other sponsors also will want to review the health plan document and materials and associated insurance, third-party administration and other health plan vendor contracts pursuant to which the health plan is established, maintained and administered to identify requirements and opportunities to respond quickly to make changes when and if health care reform happens as well as for other opportunities to mitigate existing risks and costs.
As most commentators expect some type of regulatory or statutory health plan relief to result from the current health care reform debates in Congress, employer and other health plan sponsors desiring to accelerate their ability to take advantage of any forthcoming relief should familiarize themselves with the procedures required under existing plan terms, contracts and rules to modify their programs in response to these changes. Almost certainly, plan sponsors should anticipate needing to adopt some amendments to plan documents, summary plan descriptions and other materials to take advantage of any legislative or statutory relief. Plan sponsors also need to keep in mind that their vendor contracts with administrators, group, stop-loss or captive insurers, and other vendors likely also will require the plan sponsor to notify and negotiate with its vendors to secure their agreement before adopting these changes to avoid violating those vendor agreements and prudently to arrange for appropriate implementation and administration of the modified plan design and terms. Identification of the contractual and plan requirements and commencement of discussions with the relevant vendors can help expedite the planning and implementation of any desired plan modifications the plan sponsor elects to make in response to any statutory or regulatory reforms.
While preparing for anticipated health care reforms, most plan sponsors also will want to review their plans and vendor contracts for other potential opportunities to mitigate risks or expenses. With respect to existing and future liability mitigation, each plan sponsor generally should carefully assess the allocation of fiduciary responsibility and liability between the sponsoring employer, members of its management or other workforce team, and vendors to identify potential areas where the contract may assign named or other plan administrator or other fiduciary status and liability to the plan sponsor or a member of its workforce for duties outsourced to a vendor. Sponsoring employers or their management may want to initiate negotiations with the vendor to reallocate the fiduciary role and responsibility to the party responsible for performance of the specific duties, enhancement of performance guarantees, indemnifications and insurance coverage for proper performance of the outsourced duties by the vendor in accordance with the plan terms, including any mandates imposed by the ACA and other federal laws in form and operation, and other safeguards or, if the vendor is unwilling to consider these changes, begin searching for a replacement vendor willing to provide better accountability for its actions with respect to the services it is hired to perform.
Except in rare circumstances where the sponsoring employer has carefully contracted to transfer fiduciary liability to its insurer or administrator and otherwise does not exercise or have a fiduciary obligation to exercise discretion or control over these responsibilities, employers sponsoring group health plans that violate federal mandates like the out-of-pocket limit often ultimately bear some or all of these liabilities even if the violation actually was committed by a plan vendor hired to administer the program either because the plan documents name the employer as the “named fiduciary” or “plan administrator” under ERISA, the employer or a member of its management named in the plan generally bears fiduciary responsibility functionally for selection or oversight of the culpable party, the employer signed a contract, resolution or plan document obligating the employer to indemnify the service provider for the liability, or a combination of these reasons.
Since prompt self-audit and correction can help mitigate all of these liabilities as well as help to preserve access to stop-loss or other reinsurance coverage, if any, applicable to help pay for some or all of any additional benefit liabilities resulting from these benefit mandates, business leaders of companies offering group health plan coverage should act quickly to engage experienced legal counsel for their companies for advice about how to audit their group health plan’s compliance with these and other federal health plan rules within the scope of attorney-client privilege while managing tax, financial, benefit and fiduciary liability exposures to deal with potential compliance concerns that the review might discover as well as mitigate risks that could result if the audit is improperly structured or conducted.
While businesses inevitably will need to involve or coordinate with their accounting, broker, and other vendors involved with the plans, businesses generally will want to get legal advice in a manner that preserves their potential to claim attorney-client privilege to protect against discovery in the event of future enforcement or litigation actions sensitive discussions and analysis about compliance audits, plan design choices, and other risk management and liability planning as well as to get help identifying potential plan design, contracting, procedural or other changes that may be needed to fix compliance deficiencies and mitigate other risks, particularly in light of complexity of the exposures and risks.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health and othre employee benefit, financial services, health care and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
Throughout her career, she has helped a diverse array of clients manage, administer and defend employee and other workforce, vendors and suppliers, their recruitment, selection, performance management, contracting, investigation, discipline and termination; health and other employee benefits; compensation; safety; governance; compliance and internal controls; strategic planning, process and quality improvement; change management; trade secret and other privacy, data security and data breach;; crisis preparedness and response; internal, government and third-party reporting relations, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked extensively throughout her career with employers, health and other employee benefit plans, insurers, managed care organizations, health care clearinghouses, health care providers, their business associates, employers, banks and other financial institutions, management services organizations, professional and trade associations, accreditation agencies, auditors, technology and other vendors and service providers, and others on benefit and insurance program legal and operational compliance, risk management, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending plan sponsors, fiduciaries, service providers, managed care organizations, insurers, self-insured health plans and other payers. Her experience includes both leading edge work designing and administering programs, as well as defending clients in connection with audits and enforcement actions by OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC, OSHA, Department of Insurance, Department of Justice and state attorneys’ general and other federal and state agencies; accreditation and quality organizations; private litigation and other federal and state health care industry investigation, enforcement including insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other nonpar insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns. Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
A lead policy advisor to the Government of Bolivia on its pension privitization project and involved in U.S. federal and state as well as cross border workforce, pension, health care, Social Security, immigration, and tax regulatory and statutory reform throughout her adult life, Ms. Stamer also is widely sought out for her thoughtleadership and assistance with domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; a ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
 Leave a Comment » |
Leave a Comment » |  4980D, 4980H, 6039D, ACA, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, Corporate Compliance, corporate governance, directors, employee, Employee Benefits, Employer, Employment, ERISA, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, IRC, Management, Mental Health, Mental Health Parity, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Premium Subsidies, preventive care, Reporting & Disclosure, SBC, Uncategorized, Wellness Programs | Tagged: Americas Health Care Act, Employee Benefits, Employer, Health Benefits, Health Care Reform, Health Plans, Obamacare, Trump Care |
4980D, 4980H, 6039D, ACA, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, Corporate Compliance, corporate governance, directors, employee, Employee Benefits, Employer, Employment, ERISA, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, IRC, Management, Mental Health, Mental Health Parity, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Premium Subsidies, preventive care, Reporting & Disclosure, SBC, Uncategorized, Wellness Programs | Tagged: Americas Health Care Act, Employee Benefits, Employer, Health Benefits, Health Care Reform, Health Plans, Obamacare, Trump Care |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 24, 2017
Health plans, their fiduciaries and sponsors, health insurers, health care providers, health care clearinghouses (“covered entities”) and their business associates must get and keep your business associate (BA) agreements (BAAs) in place, up-to-date, and readily available for inspection in accordance with the Health Insurance Portability & Accountability Act (HIPAA) Privacy Rule, 45 C.F.R. Part 160 and Subparts A and E of Part 164 (Privacy Rule). That’s the clear message to covered entities and their business associates in the April 17, 2017 HIPAA Resolution Agreement just announced by the Department of Health & Human Services (HHS) Office of Civil Rights (OCR) with the Center for Children’s Digestive Health (CCDH).
While the Resolution Agreement relates to breaches of the BAA requirements of a small pediatric practice, all health plans, health care providers and other covered entities and business associates should focus on the adequacy of their BAAs and their BAA record keeping. HIPAA compliance surveys reflect deficiencies with the BAA rules are common throughout the industry. These findings and the involvement of BAs in data breaches or other OCR enforcement activities suggest a high probability that many other covered entities and business associates may be sitting ducks for similar sanctions. See e.g., HIPAA Compliance Survey Churns Up Many Business Associate Problems (January 3, 2017). Consequently, all covered entities and business associates generally should treat the CCDH Resolution Agreement as a message to review and correct as necessary their organizations’ compliance and recordkeeping to minimize their exposure to potential sanctions from violations of the HIPAA business associate rules.
The HIPAA Business Associate Agreement Requirements
OCR’s announcement of the CCDH Resolution Agreement is the latest in a growing series of HIPAA enforcement actions showing the growing risk covered entities and their business associates face for failing to take appropriate steps to comply with the BAA and other Privacy Rule requirements of HIPAA.
As compliance audits and surveys of covered entities and business associates suggest a high level of noncompliance with the business associate agreement requirements among covered entities and business associates, While the ever-growing list of Resolution Agreements and Civil Monetary Penalties announced by OCR cover a variety of categories of HIPAA violations, the CCDH Resolution Agreement highlights the importance of covered entities and their business associates ensuring that before the BA creates, accesses, receives, discloses, retains or destroys any PHI for the covered entity, a BAA meeting the Privacy Rule requirements is signed and retained for at least the six-year period the Privacy Rule requires in a manner easily producible when and if OCR or another agency asks for a copy as part of an investigation or other compliance audit. See Privacy Rule §§ 164.502(e), 164.504(e), 164.532(d) and (e).
The Privacy Rule requires that covered entities and business associates enter into a written and signed business associate agreement that contains the elements specified in Privacy Rule § 164.504(e) before the business associate creates, uses, accesses or discloses PHI of the covered entity. Meanwhile, the Privacy Rule recordkeeping requirements require that covered entities and BAs maintain copies of these BAAs for a minimum of six years.
Violations of the Privacy Rule can carry stiff civil or even criminal penalties Pursuant to amendments to HIPAA enacted as part of the HITECH Act, civil penalties typically do not apply to violations punished under the criminal penalty rules of HIPAA set forth in Social Security Act , 42 U.S.C § 1320d-6 (Section 1177).
Under Section 1177, the criminal enforcement provisions of HIPAA authorize the Justice Department to prosecute a person who knowingly in violation of the Privacy Rule (1) uses or causes to be used a unique health identifier; (2) obtains individually identifiable health information relating to an individual; or (3) discloses individually identifiable health information to another person, punishable by the following criminal sanctions and penalties:
- A fine of up to $50,000, imprisoned not more than 1 year, or both;
- If the offense is committed under false pretenses, a fine of up to $100,000, imprisonment of not more than 5 years, or both; and
- If the offense is committed with intent to sell, transfer, or use individually identifiable health information for commercial advantage, personal gain, or malicious harm, a fine of up to $250,000, imprisoned not more than 10 years, or both.
In contrast, as amended by the HITECH Act, the civil enforcement provisions of HIPAA empower OCR to impose Civil Monetary Penalties on both covered entities and BAs for violations of any of the requirements of the Privacy or Security Rules. The penalty ranges for civil violations depends upon the circumstances associated with the violations and are subject to upward adjustment for inflation. As most recently adjusted here effective September 6, 2016, the following currently are the progressively increasing Civil Monetary Penalty tiers:
- A minimum penalty of $100 and a maximum penalty of $50,000 per violation, for violations which the CE or BA “did not know, and by exercising reasonable diligence would not have known” about using “the business care and prudence expected from a person seeking to satisfy a legal requirement under similar circumstances;”
- A minimum penalty of $1,000 and a maximum penalty of $50,000 per violation, for violations for “reasonable cause” which do not rise to the level of “willful neglect” where “reasonable cause” means the “circumstances that would make it unreasonable for the covered entity, despite the exercise of ordinary business care and prudence, to comply with the violated Privacy Rule requirement;”
- A minimum penalty of $10,000 and a maximum penalty of $50,000 per violation, for violations attributed to “willful neglect,” defined as “the conscious, intentional failure or reckless indifference to the obligation to comply” with the requirement or prohibition; and
- A minimum penalty of $50,000 and a maximum penalty of $1.5 million per violation, for violations attributed to “willful neglect” not remedied within 30 days of the date that the covered entity or BA knew or should have known of the violation.
For continuing violations such as failing to implement a required BAA, OCR can treat each day of noncompliance as a separate violation. However, sanctions under each of these tiers generally are subject to a maximum penalty of $1,500,000 for violations of identical requirements or prohibitions during a calendar year. For violations such as the failure to implement and maintain a required BAA where more than one covered entity bears responsibility for the violation, OCR an impose Civil Monetary Penalties against each culpable party. OCR considers a variety of mitigating and aggravating facts and circumstances when arriving at the amount of the penalty within each of these applicable tiers to impose.
While criminal enforcement of HIPAA remains relatively rare, a review of the OCR enforcement record in recent years makes clear that civil enforcement of HIPAA and the sanctions imposed is growing. See e.g., $400K HIPAA Settlement Shows Need To Conduct Timely & Appropriate Risk Assessments; $5.5M Memorial HIPAA Resolution Agreement Shows Need To Audit. For more examples, also see here.
CCDH Sanctions For Violation Of HIPAA Business Associate Agreement Rules
The CCDH Resolution Agreement arises from violations of this requirement that OCR says it discovered as a result of a compliance review conducted in response to an OCR investigation of a CCDH business associate, FileFax, Inc. According to OCR, OCR found from the compliance review of CCDH triggered by OCR’s investigation of FileFax that while CCDH began disclosing PHI to Filefax in 2003 and that Filefax stored records containing protected health information (PHI) for CCDH, neither CCDH nor Filefax could produce a signed Business Associate Agreement (BAA) covering their relationship for any period before October 12, 2015.
Based on the resulting investigation, OCR concluded:
- CCDH failed to obtain a BAA providing written assurances from Filefax that it would appropriately safeguard the PHI in Filefax’s possession or control satisfactory assurances as required by Privacy Rule §164.502(e); and
- Because CCDH failed to secure the required BAA, it violated the Privacy Rule by impermissibly disclosing the PHI of at least 10,728 individuals to Filefax when CCDH transferred the PHI to Filefax without obtaining the requisite BAA from Filefax (Covered Conduct).
In the Resolution Agreement, CCDH agrees to pay HHS $31,000.00 (Resolution Amount) and enter into and comply with a Corrective Action Plan (CAP) in return for OCR’s release of CCDH from liability for “any actions it may have against CCDH under the HIPAA Rules” for the Covered Conduct. The Resolution Agreement only settles the civil monetary penalty and other OCR enforcement liabilities of CCDH with respect to the Covered Conduct. Its provisions expressly state the Resolution Agreement does not affect any exposures of CCDH to CCDH to OCR civil monetary penalties or other enforcement for any HIPAA violations other than the Covered Conduct.
Perhaps even more noteworthy given the HITECH Act’s provisions coordinating the civil and criminal sanctions of HIPAA, while the Resolution Agreement provides no clear indication that the Justice Department might be considering criminally prosecuting CCDH or any other party in relation to the Covered Conduct, the Resolution Agreement also expressly states that its provisions do not affect CCDH’s potential exposure, if any, to criminal prosecution by the Justice Department for a criminal violation of the Privacy Rules under Section 1177 of the Social Security Act.
Implications For Covered Entities & Business Associates
Covered entities and their business associates should heed the CCDH Resolution Agreement as a strong message from OCR to ensure their organizations are complying with HIPAA’s BAA and other requirements. The Resolution Agreement makes clear that the starting point of this compliance effort must be obtaining and maintaining the requisite BAAs for each BA relationship.
To position their organizations to withstand potential investigation by OCR, covered entities and BAs should start by conducting a well-documented audit within the scope of attorney-client privilege both to verify that an appropriate, signed BAA is in place for each BA relationship as well as adequacy of processes for identifying business associate relationships, ensuring that signed BAAs are in effect before BAs access any PHI, and for investigating, reporting and resolving any breaches of the HIPAA Privacy or Security Rules that may arise in the course of operations.
Conducting this audit as soon as possible is particularly important in light of reported findings of widespread compliance concerns. See HIPAA Compliance Survey Churns Up Many Business Associate Problems (January 3, 2017). As the audit process could identify potential violations or other legally sensitive concerns, covered entities and business associates generally will want to arrange for this audit and evaluation to be conducted under the supervision of legal counsel experienced with HIPAA within or pursuant to processes structured with the assistance of legal counsel within the scope of attorney-client privilege.
Beyond confirming all necessary BAAs are in place, covered entities and business associates also generally will want to evaluate the adequacy of BAs’ processes and procedures for maintaining compliance with the Privacy and Security Rules as well as processes and procedures for responding to audits, investigations and complaints, reporting and addressing breaches of electronic and other PHI and other possible compliance concerns under HIPAA and other related laws. In many instances, parties may n wish to revise and strengthen existing BAAs to more specifically define these policies and procedures more specifically as well as indemnification, cyber or other liability coverage requirements and other contractual provisions for allocating potential costs and liabilities arising from breaches, audits, investigations and other expenses associated with the administration of these provisions.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to manage and defend compliance, public policy, regulatory, staffing and other operations and risk management concerns. A core focus of this work includes work to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; dealings with JCHO and other accreditation and quality organizations; investigation and defense of private litigation and other federal and state health care industry investigations and enforcement; insurance or other liability management and allocation; process and product development; managed care, physician and other staffing, business associate and other contracting; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.
In the course of this work, Ms. Stamer has accumulated extensive experience helping health industry clients manage workforce, medical staff, vendors and suppliers, medical billing, reimbursement, claims and other provider-payer relations, business partners, and their recruitment, performance, discipline, compliance, safety, compensation, benefits, and training, board, medical staff and other governance; compliance and internal controls; strategic planning, process and quality improvement; change management; assess, deter, investigate and address staffing, quality, compliance and other performance; meaningful use, EMR, HIPAA and other data security and breach and other health IT and data; crisis preparedness and response; internal, government and third-party reporting, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
Author of leading works on HIPAA and other privacy and data security works and the scribe leading the American Bar Association Joint Committee on Employee Benefits Annual Agency Meeting with OCR, her experience includes extensive compliance, risk management and data breach and other crisis event investigation, response and remediation under HIPAA and other laws.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked closely with a diverse range of physicians, hospitals and healthcare systems, DME, Pharma, clinics, health care providers, managed care, insurance and other health care payers, quality assurance, credentialing, technical, research, public and private social and community organizations, and other health industry organizations and their management deal with governance; credentialing, patient relations and care; staffing, peer review, human resources and workforce performance management; outsourcing; internal controls and regulatory compliance; billing and reimbursement; physician, employment, vendor, managed care, government and other contracting; business transactions; grants; tax-exemption and not-for-profit; licensure and accreditation; vendor selection and management; privacy and data security; training; risk and change management; regulatory affairs and public policy and other concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other nonpar, insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns.
In connection with this work, Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA, FACTA, trade secret and other information privacy and data security rules, including the establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and and enforcement, and a host of other related concerns. Her clients include public and private health care providers, health insurers, health plans, technology and other vendors, and others.
Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, MGMA, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; a ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
 Leave a Comment » |
Leave a Comment » |  ARRA, Attorney-Client Privilege, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, employee, Employee Benefits, Employer, Employers, Employment, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Patient Empowerment, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Uncategorized | Tagged: Business Associate, Health Care, Health Insurer, Health Plans, HIPAA, HIPAA OCR, HIPAA Privacy, HITECH, Insurer, Technology, tpa |
ARRA, Attorney-Client Privilege, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, employee, Employee Benefits, Employer, Employers, Employment, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Patient Empowerment, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Uncategorized | Tagged: Business Associate, Health Care, Health Insurer, Health Plans, HIPAA, HIPAA OCR, HIPAA Privacy, HITECH, Insurer, Technology, tpa |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 19, 2017
https://videopress.com/embed/3futNZyv?hd=0&autoPlay=0&permalink=0&loop=0
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.©2017. Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Leave a Comment » |
Leave a Comment » |  Uncategorized |
Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 19, 2017
https://videopress.com/embed/MqUiaSs1?hd=0&autoPlay=0&permalink=0&loop=0
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.
©2017. Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Leave a Comment » |
Leave a Comment » |  Uncategorized |
Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
 Comments Off on SHOP Marketplace Still Health Coverage Option For Small Employers; All Employers Should Confirm Health Plan Compliance |
Comments Off on SHOP Marketplace Still Health Coverage Option For Small Employers; All Employers Should Confirm Health Plan Compliance |  105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, COBRA, compensation, compliance, conflict of interest, Contraception, Corporate Compliance, corporate governance, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excise Tax, Excise Taxes, Exempt, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HIPAA, HIPAA, HR, Human Resources, Uncategorized | Tagged: ACA, Employer, Health Benefits, Health Insurance, Health Plan, Obamacare, shop marketplace |
105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Bankruptcy, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, COBRA, compensation, compliance, conflict of interest, Contraception, Corporate Compliance, corporate governance, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excise Tax, Excise Taxes, Exempt, Fiduciary Responsibility, Form 5500, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HIPAA, HIPAA, HR, Human Resources, Uncategorized | Tagged: ACA, Employer, Health Benefits, Health Insurance, Health Plan, Obamacare, shop marketplace |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
May 4, 2017
The US House of Representatives is scheduled to vote again tonight on the revised Majority-leadership lead first step healthcare reform legislation seeking to provide Americans and American business with some initial relief from the soaring premium and health care costs, care access barriers and regulatory and other burdens that have resulted under the ObamaCare law and regulations. Every American should call, e-mail or fax the leaders and their Congressperson as soon as possible today and tell them to pass this legislation and get busy passing the next set of reforms with no further delay, the get and stay II formed and involved until it gets it done starting with the House hearing and vote slated tonight starting at 8:30 Eastern. Get details here.
Health care and its reform is a complex challenge. Americans and American businesses, health payers, and States and their healthcare needs are highly diverse. The ambitious but far from successful Obamacare law shows the dangers of well-meaning but unrealistic To try to fix these challenges with a sweeping, one shot fix.
While passage of this legislative package won’t magically fix these challenges, it will provide quick relief for some of the ObamaCare expense and restrictions and expand the choices that Americans, American business, payers, providers and States while Congress works with American to identify and pursue legislative, regulatory, marketplace and other improvements.
Let’s get things going in the right direction!
 Comments Off on Tell Congress Pass AHCA Today |
Comments Off on Tell Congress Pass AHCA Today |  4980D, 4980H, 6039D, ACA, Affordable Care Act, board of directors, Cafeteria Plans, Claims Administration, Consumer Protection, Contraception, Corporate Compliance, directors, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Revenue Code, IRC, King V. Burwell, Leadership, Management, Managment, MEWA, Non-Exempt, Obamacare, Overtime, Patient Empowerment, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, Physician, Plan Admistrator, Premium Subsidies, preventive care, Provider, Public Policy, Reporting & Disclosure, SBC, Tax, Wellness, Wellness Programs, Worker Classification, Workforce | Tagged: Affordable Care Act, American Health Care Act, Health Plans, health reform, HSA |
4980D, 4980H, 6039D, ACA, Affordable Care Act, board of directors, Cafeteria Plans, Claims Administration, Consumer Protection, Contraception, Corporate Compliance, directors, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Revenue Code, IRC, King V. Burwell, Leadership, Management, Managment, MEWA, Non-Exempt, Obamacare, Overtime, Patient Empowerment, Patient Protection & Affordable Care Act, Patient Protection and Affordabel Care Act, Patient Protection and Affordable Care Act, Pay, Payroll Tax, Physician, Plan Admistrator, Premium Subsidies, preventive care, Provider, Public Policy, Reporting & Disclosure, SBC, Tax, Wellness, Wellness Programs, Worker Classification, Workforce | Tagged: Affordable Care Act, American Health Care Act, Health Plans, health reform, HSA |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 26, 2017
A new Department of Health and Human Services Office of Civil Rights (OCR) CardioNet Resolution Agreement and Corrective Action Plan (Resolution Agreement) settling OCR charges of violations of the Privacy and Security Rules of the Health Insurance Portability & Accountability Act against remote cardiac monitoring provider CardioNet provides important lessons for all health plans, health insurers, telemedicine and other healthcare providers, healthcare clearinghouses (Covered Entities) and their business associates about steps to take to reduce their risk of getting hit with big OCR penalty like the $2.5 million settlement payment CardioNet must pay under the Resolution Agreement.
OCR announced the first OCR HIPAA settlement involving a wireless health services provider Monday, April 24. Under the Resolution Agreement, CardioNet agrees to pay OCR $2.5 million and to implement a corrective action plan to settle potential OCR charges it violated the HIPAA Privacy and Security Rules based on the impermissible disclosure of unsecured electronic protected health information (ePHI).
CardioNet Charges & Settlement
As has become increasingly common in recent years, the CardioNet settlement arose from concerns initially brought to OCR’s attention in connection with a HIPAA breach notification report. On January 10, 2012, OCR received notification from the provider of remote mobile monitoring of and rapid response to patients at risk for cardiac arrhythmias that a workforce member’s laptop with the ePHI of 1,391 individuals was stolen from a parked vehicle outside of the employee’s home. CardioNet subsequently notified OCR of a second breach of ePHI 2,219 individuals, respectively.
Likewise, the HIPAA breaches uncovered by OCR in the course of investigating these CardioNet breaches occur in the operations of many other covered entities. According to the OCR’s investigation in response to these breach reports revealed a series of continuing compliance concerns, including:
- CardioNet failed to conduct an accurate and thorough risk analysis to assess the potential risks and vulnerabilities to the confidentiality, integrity, and availability of ePHI and failed to plan for and implement security measures sufficient to reduce those risks and vulnerabilities;
- CardioNet’s policies and procedures implementing the standards of the HIPAA Security Rule were in draft form and had not been implemented;
- CardioNet was unable to produce any final policies or procedures regarding the implementation of safeguards for ePHI, including those for mobile devices;
- CardioNet failed to implement policies and procedures that govern the receipt and removal of hardware and electronic media that contain electronic protected health information into and out of its facilities, the encryption of such media, and the movement of these items within its facilities until March 2015; and
- CardioNet failed to safeguard against the impermissible disclosure of protected health information by its employees, thereby permitting access to that information by an unauthorized individual, and failed to take sufficient steps to immediately correct the disclosure.
To resolve these OCR charges, CardioNet agrees in the Resolution Agreement to pay $2.5 million to OCR and implement a corrective action plan. Among other things, the corrective action plan requires CardioNet to complete the following actions to the satisfaction of OCR:
- Prepare a current, comprehensive and thorough Risk Analysis of security risks and vulnerabilities that incorporates its current facility or facilities and the electronic equipment, data systems, and applications controlled, currently administered or owned by CardioNet, that contain, store, transmit, or receive electronic protected health information (“ePHI”) and update that Risk Analysis annually or more frequently, if appropriate in response to environmental or operational changes affecting the security of ePHI.
- Assess whether its existing security measures are sufficient to protect its ePHI and revise its Risk Management Plan, Policies and Procedures, and training materials and implement additional security measures, as needed.
- Develop and implement an organization-wide Risk Management Plan to address and mitigate any security risks and vulnerabilities found in the Risk Analysis as required by the Risk Management Plan.
- Review and, to the extent necessary, revise, its current Security Rule Policies and Procedures (“Policies and Procedures”) based on the findings of the Risk Analysis and the implementation of the Risk Management Plan to comply with the HIPAA Security Rule.
- Provide certification to OCR that all laptops, flashdrives, SD cards, and other portable media devices are encrypted, together with a description of the encryption methods used (“Certification”).
- Review, revise its HIPAA Security training to include a focus on security, encryption, and handling of mobile devices and out-of-office transmissions and other policies and practices require to address the issues identified in the Risk Assessment and otherwise comply with the Risk Management Plan and HIPAA train its workforce on these policies and practices.
- Investigate all potential violations of its HIPAA policies and procedures and notify OCR in writing within 30 days of any violation.
- Submit annual reports to OCR, which must be signed by an owner or officer of CardioNet attesting that he or she has reviewed the annual report, has made a reasonable inquiry regarding its content and believes that, upon such inquiry, the information is accurate and truthful.
- Maintain for inspection and copying, and provide to OCR, upon request, all documents and records relating to compliance with the corrective action plan for six years.
Implications For Covered Entities & Business Associates
The latest in a rapidly-growing list of high dollar HIPAA enforcement actions by OCR, the CardioNet Resolution Agreement contains numerous lessons for other Covered entities and their business associates about the importance of appropriate HIPAA privacy and security compliance, including but not limited to the following:
- Like many previous resolution agreements announced by OCR, the Resolution Agreement reiterates the responsibility of covered entities and business associates to properly secure their ePHI and that as part of this process, OCR expects all laptop computers and other mobile devices containing or with access to ePHI be properly encrypted and secured.
- It also reminds covered entities and their business associates to be prepared for, and expect an audit from OCR when OCR receives a report that their organization experienced a large breach of unsecured ePHI.
- The Resolution Agreement’s highlighting of the draft status of CardioNet’s privacy and security policies also reflects OCR expects covered entities to actually final policies, procedures and training in place for maintaining compliance with HIPAA.
- The discussion and requirements in the Corrective Action Plan relating to requirements to conduct comprehensive risk assessments at least annually and in response to other events, and to update policies and procedures in response to findings of these risk assessments also drives home the importance of conducting timely, documented risk analyses of the security of their ePHI, taking prompt action to address known risks and periodically updating the risk assessment and the associated privacy and security policies and procedures in response to the findings of the risk assessment and other changing events.
- The requirement in the Resolution Agreement of leadership attestation and certification on the required annual report reflects OCR’s expectation that leadership within covered entities and business associates will make HIPAA compliance a priority and will take appropriate action to oversee compliance.
- Finally, the $2.5 million settlement payment required by the Resolution Agreement and its implementation against CardioNet makes clear that OCR remains serious about HIPAA enforcement.
Clearly, covered entities, business associates and their management should take steps to promptly review the adequacy of their organizations’ HIPAA compliance policies, practices and documentation in light of the deficiencies listed in the CardioNet and other HIPAA OCR settlements and civil monetary penalty assessments. See e.g., Latest HIPAA Resolution Agreement Drives Home Importance Of Maintaining Current, Signed Business Associate Agreements; $400K HIPAA Penalty Teaches Risk Assessment Importance; $3.2 Children’s HIPAA CMP Teaches Key Lessons.
Of course, covered entities and business associates need to keep in mind that acts, omissions and events that create HIPAA liability risks also carry many other potential legal and business risks. For instance, since PHI records and data involved in such breaches usually incorporates Social Security Numbers, credit card or other debt or payment records or other personal consumer information, and other legally sensitive data, covered entities and business associates generally also may face investigation, notification and other responsibilities and liabilities under confidentiality, privacy or data security rules of the Fair and Accurate Credit Transaction Act (FACTA), the Internal Revenue Code, the Social Security Act, state identity theft, data security, medical confidentiality, privacy and ethics, insurance, consumer privacy, common law or other state privacy claims and a host of other federal or state laws. Depending on the nature of the covered entity or its business associates, the breach or other privacy event also may trigger fiduciary liability exposures for health plan fiduciaries in the case of a health plan, professional ethics or licensing investigations or actions against health care providers, insurance companies, administrative service providers or brokers, shareholder or other investor actions, employment or vendor termination or disputes and a host of other indirect legal consequences.
Beyond, and regardless of if, a covered entity or business ultimately succeeds in defending its actions against a charge of violating any of these or other standards, however, covered entities, business associates and their leaders should keep in mind that the most material and often most intractable consequences of a HIPAA or other data or other privacy breach report or public accusation, investigation, admission also typically are the most inevitable:
- The intangible, but critical loss of trust and reputation covered entities and business associates inevitably incur among their patients, participants, business partners, investors and the community; and
- The substantial financial expenses and administrative and operational disruptions of investigating, defending the actions of the organization and implementation of post-event corrective actions following a data or other privacy breach, audit, investigation, or charge.
In light of these risks, covered entities business associates and their management should use the experiences of CardioNet and other covered entities or business associates caught violating HIPAA or other privacy and security standards to reduce their HIPAA and other privacy and data security exposures. Management of covered entities and their business associates should take steps to ensure that their organizations policies, practices and procedures currently are up-to-date, appropriately administered and monitored, and properly documented. Management should ensure that their organizations carefully evaluate and strengthen as necessary their current HIPAA risk assessments, policies, practices, record keeping and retention and training in light of these and other reports as they are announced in a well-documented manner. The focus of these activities should be both to maintain compliance and position their organizations efficiently and effectively to respond to and defend their actions against a data breach, investigation, audit or accusation of a HIPAA or other privacy or security rule violation with a minimum of liability, cost and reputational and operational damages.
As the conduct of these activities generally will involve the collection and analysis of legally sensitive matters, most covered entities and business associates will want to involve legal counsel experienced with these matters and utilize appropriate procedures to be able to use and assert attorney-client privilege and other evidentiary privileges to mitigate risks associated with these processes. To help plan for and mitigate foreseeable expenses of investigating, responding to or mitigating a known, suspected or asserted breech or other privacy event, most covered entities and business associates also will want to consider the advisability of tightening privacy and data security standards, notification, cooperation and indemnification protections in contracts between covered entities and business associates, acquiring or expanding data breach or other liability coverage, or other options for mitigating the financial costs of responding to a breach notification, investigation or enforcement action.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to manage and defend compliance, public policy, regulatory, staffing and other operations and risk management concerns. A core focus of this work includes work to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; dealings with JCHO and other accreditation and quality organizations; investigation and defense of private litigation and other federal and state health care industry investigations and enforcement; insurance or other liability management and allocation; process and product development; managed care, physician and other staffing, business associate and other contracting; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.
In the course of this work, Ms. Stamer has accumulated extensive experience helping health industry clients manage workforce, medical staff, vendors and suppliers, medical billing, reimbursement, claims and other provider-payer relations, business partners, and their recruitment, performance, discipline, compliance, safety, compensation, benefits, and training, board, medical staff and other governance; compliance and internal controls; strategic planning, process and quality improvement; change management; assess, deter, investigate and address staffing, quality, compliance and other performance; meaningful use, EMR, HIPAA and other data security and breach and other health IT and data; crisis preparedness and response; internal, government and third-party reporting, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
Author of leading works on HIPAA and other privacy and data security works and the scribe leading the American Bar Association Joint Committee on Employee Benefits Annual Agency Meeting with OCR, her experience includes extensive compliance, risk management and data breach and other crisis event investigation, response and remediation under HIPAA and other data security, privacy and breach laws. Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns.
In connection with this work, Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA, FACTA, trade secret and other information privacy and data security rules, including the establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and enforcement, and a host of other related concerns. Her clients include public and private health care providers, health insurers, health plans, technology and other vendors, and others.
Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, MGMA, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked closely with a diverse range of physicians, hospitals and healthcare systems, DME, Pharma, clinics, health care providers, managed care, insurance and other health care payers, quality assurance, credentialing, technical, research, public and private social and community organizations, and other health industry organizations and their management deal with governance; credentialing, patient relations and care; staffing, peer review, human resources and workforce performance management; outsourcing; internal controls and regulatory compliance; billing and reimbursement; physician, employment, vendor, managed care, government and other contracting; business transactions; grants; tax-exemption and not-for-profit; licensure and accreditation; vendor selection and management; privacy and data security; training; risk and change management; regulatory affairs and public policy and other concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other “nonpar,” insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; an ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
 Comments Off on Latest $2.5M HIPAA Settlement Warning To Health Plans, Providers: Get HIPAA Compliant |
Comments Off on Latest $2.5M HIPAA Settlement Warning To Health Plans, Providers: Get HIPAA Compliant |  ARRA, Attorney-Client Privilege, board of directors, Brokers, Civil Monetary Penalties, Civil Rights, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, Electronic Medical Record, Employee Benefits, Employer, fiduciary duty, Fiduciary Responsibility, FINRA, GINA, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Technology, Telecommuting, Uncategorized | Tagged: Breach, Breach Notification, Business Associate, Covered Entity, Health Insurance, Health Plan, HIPAA, HIPAA Privacy, HIPAA Security, Medical Privacy, OCR, Office of Civil Rights, REmote Care, Technology, Telemedicine |
ARRA, Attorney-Client Privilege, board of directors, Brokers, Civil Monetary Penalties, Civil Rights, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, Electronic Medical Record, Employee Benefits, Employer, fiduciary duty, Fiduciary Responsibility, FINRA, GINA, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, Health Plans, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Technology, Telecommuting, Uncategorized | Tagged: Breach, Breach Notification, Business Associate, Covered Entity, Health Insurance, Health Plan, HIPAA, HIPAA Privacy, HIPAA Security, Medical Privacy, OCR, Office of Civil Rights, REmote Care, Technology, Telemedicine |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 26, 2017
President Donald J. Trump has named Philip A. Miscimarra the Chairman of the National Labor Relations Board (NLRB) by President Donald J. Trump.
A Republican and former management lawyer, Miscimarra has served on the NLRB since August 7, 2013, following the Senate’s confirmation of his appointment to the NLRB on July 30, 2013 His current term of appointment to the NLRB is slated to expire on December 16, 2017.
President Trump originally designated Miscimarra to to serve as Acting NLRB Chairman on January 23, 2017. On April 21, 2017, the White House announced the President’s planned to name Miscimarra as the new NLRB Chairman. President Trump’s April 24, 2017 designation of Miscimarra as NLRB Chairman follows through on this plan.
The NLRB also consists of NLRB Member Mark Gaston Pearce (previously NLRB Chairman), whose term expires on August 27, 2018; and NLRB Member Lauren McFerran, whose term expires on December 16, 2019. Two Board member seats are currently vacant.
Before joining the Board, Chairman Miscimarra was a Senior Fellow in the Center for Human Resources at the University of Pennsylvania’s Wharton Business School in the Wharton Center for Human Resources, and a management-side labor and employment law partner with Morgan Lewis & Bockius LLP in Chicago. He also previously worked as a labor and employment attorney with Seyfarth Shaw LLP; Murphy Smith & Polk PC (now the Chicago office of Ogletree, Deakins, Nash, Smoak & Stewart, PC); and Reed Smith Shaw & McClay (now Reed Smith LLP). He is the author or co-author of several books involving labor law issues, including The NLRB and Managerial Discretion: Subcontracting, Relocations, Closings, Sales, Layoffs, and Technological Change (2d ed. 2010) (by Miscimarra, Turner, Friedman, Callahan, Conrad, Lignowski and Scroggins); The NLRB and Secondary Boycotts (3d ed. 2002) (by Miscimarra, Berkowitz, Wiener and Ditelberg); and Government Protection of Employees Involved in Mergers and Acquisitions (1989 and 1997 supp.) (by Northrup and Miscimarra).
Miscimarra received his Juris Doctor from the University of Pennsylvania Law School; a Master of Business Administration from the University of Pennsylvania’s Wharton Business School; and a Bachelor of Arts, summa cum laude, from Duquesne University.
Miscimarra’s appointment as Chair is expected to shift the balance of the NLRB toward a more management friendly perspective. His dissenting opinions during his tenure on the NLRB suggest that under his leadership after the existing vacancies on the NLRB are filled may adopt more management friendly points of view on issues like rolling back “quickie” certification election rules, the NLRB test for determining whether joint employer relationships exist, deciding when handbooks and work rules interfere with employees’ NLRA rights, recognizing collective bargaining units, extending NLRA protections to nontraditional groups such as students, medical professionals and others compared to those pursued by the NLRB during the Obama Administration.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney board certified in labor and employment law by the Texas Board of Legal Specialization and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. Her day-to-day work encompasses both labor and employment issues, as well as independent contractor, outsourcing, employee leasing, management services and other nontraditional service relationships. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with all aspects for workforce and human resources management, including, recruitment, hiring, firing, compensation and benefits, promotion, discipline, compliance, trade secret and confidentiality, noncompetition, privacy and data security, safety, daily performance and operations management, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well-known for her extensive work with health, insurance, financial services, technology, energy, manufacturing, retail, hospitality and governmental employers, her nearly 30 years’ of experience encompasses domestic and international businesses of all types and sizes.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on human resources, labor and employment, employee benefits, compensation, occupational safety and health, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications.
Want to know more? See here for details about the author of this update, attorney Cynthia Marcotte Stamer, e-mail her here or telephone Ms. Stamer at (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Trump Picks Miscimmara As New NLRB Chair |
Comments Off on Trump Picks Miscimmara As New NLRB Chair |  employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Leadership, Managment, MSHA, NLRA, Uncategorized | Tagged: Labor Law, labor-management relations, NLRA, Trump Administration |
employee, Employer, Employers, Employment, HR, Human Resources, Labor Management Relations, Leadership, Managment, MSHA, NLRA, Uncategorized | Tagged: Labor Law, labor-management relations, NLRA, Trump Administration |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 25, 2017
While Congress and the Trump Administration continue to ponder and debate what if anything to do with the health care reforms of the Patient Protection and Affordable Care Act (ACA), employer and other health plan sponsors, health plan insurers, plan fiduciaries and others responsible for health plan design, administration or funding must take steps to verify their past and continuing compliance with the ACA and other federal mandates while laying the groundwork to respond quickly to any eventual reforms.
Regardless of what, if anything, the existing Congress or the Trump Administration does to repeal or reform the ACA or other federal health plan rules, all health plan sponsors, insurers, fiduciaries and administrators should act to mitigate their substantial and ever-growing health plan exposures by arranging for an independent compliance audit of their health plan terms, materials and operations for potential uncorrected past or current violations of the 40 federal mandates covered by the Form 8928 reporting and associated Internal Revenue Code excise tax liability exposure, as well as other applicable plan liabilities under the Employee Retirement Income Security Act (ERISA), the Social Security Act, the Internal Revenue Code and other federal laws within open statute of limitation periods.
The cost, complexity and riskiness of health plan sponsorship and administration has grown exponentially over the past two decades. Thanks to the ACA and the continuous stream of other federal laws and regulations implemented over the past 20 years, sponsoring employers, as well as their health plans and those responsible as fiduciaries for administering, funding and insuring these programs now face huge costs, responsibilities and liabilities. While the ACA substantially expanded the federal health plan mandates and liabilities, the ACA is not the lone cause and its amendment or repeal alone won’t fully resolve these risks prospectively or retrospectively insulate sponsoring employers, their plans or their fiduciaries and insurers from the liabilities and costs of compliance issues occurring before Congress repeals or amends the ACA.
Of particular note for employer and other sponsors of group health plans are the self-reporting and excise tax self-assessment and payment requirements for employers coupled with the companion responsibilities and liabilities fiduciaries, plan administrators and others face under these federal mandates make it important that employers and others sponsoring group health plans and their management or other leaders overseeing or participating in plan design or vendor selection, plan administration or other plan related activities get advice and help from qualified legal counsel experienced in health plan matters:
- To conduct an independent compliance review and risk assessment of their health plans,
- To recommend and assist in the performance of recommended steps to correct or mitigate risks from any potential past or existing violations or other exposures that have arisen or are likely to arise from existing contractual, plan design or other health plan actions;
- To explore the potential advisability of taking additional steps to prevent or mitigate health plan associated compliance or other risks going forward whether or not health reform happens; and
- To begin preparing to take advantage of any impending health care reforms by evaluating the requirements and procedures that existing plan terms, contracts, vendors and arrangements are likely to require to implement changes necessary to respond to any reforms as quickly and efficiently as possible.
Spring Clean Your Health Plan House
Since any reforms eventually enacted are unlikely to retroactively eliminate liability of employers, their health plans or fiduciaries for violations of federal health plan mandates, health plan terms, or associated contracts occurring before the effective date of reform, employer and other health plan sponsors, fiduciaries, insurers and administrators should begin by identifying, cleaning up any existing, unresolved, and preventing any new health plan compliance problems.
While overall compliance with applicable federal mandates and health terms generally should be the goal, employers or others sponsoring group health plans need to be particularly concerned with their responsibilities and potential liability under the Internal Revenue Code to self-identify, report and pay stiff excise tax penalties of $100 per day per violation of any of 40 federal health plan mandates imposed by the ACA and various other federal laws when the sponsor files its annual tax return.
This employer or other plan sponsor excise tax liability generally arises in addition to the liabilities that plans, their fiduciaries and their insures face for failing to administer and pay benefits under the plans in accordance with the listed 40 federal mandates, whether actually written into or imputed by operation of law into the plan, the costs of which sponsoring employers often will bear responsibility for funding in whole or in part pursuant to their contractual liabilities under the health plan contracts, as plan fiduciaries or both. See, Businesses Must Confirm & Clean Up Health Plan ACA & Other Compliance Following Supreme Court’s King v. Burwell Decision; More Work For Employers, Benefit Plans Following SCOTUS Same-Sex Marriage Ruling; 2016 & 2017 Health Plan Budgets, Workplans Should Anticipate Expected Changes To SBCs.
Sponsors and plan fiduciaries also need to be concerned about other risks beyond sponsoring employers’ excise tax liability exposures for sponsoring a non-compliant group health plan. Among other things, group health plans and their fiduciaries can face audits, litigation and enforcement actions by the Centers for Medicare & Medicaid Services and other health plans for improperly coordinating plan claims with other coverage as well as lawsuits from covered persons, their health care providers or other beneficiaries, the Department of Labor and CMS, or others seeking to enforce rights to benefits, penalties in the case of CMS or the Department of Labor, and attorneys’ fees and other costs of enforcement. Beyond benefit litigation, the employer or representatives of the sponsoring employer, if any, named or acting as fiduciaries, insurer or third-party service providers named or acting as fiduciaries, also could face fiduciary lawsuits seeking damages, equitable relief, and attorneys’ fees and costs of court, for failing to prudently administer the plan in accordance with its terms and the law brought by covered persons or their beneficiaries or the DOL as well as fiduciary breach penalties if the fiduciary breach action is brought by the DOL. If the plan fails to comply with claims and appeals procedures or other ERISA notification requirements, parties named or functioning as the plan administrator for this purpose also could face penalties of up to $125 per violation per day in the case of enforcement actions brought by participants and beneficiaries or $1025 per violation per day in the case of actions brought by the DOL, plus attorneys’ fees and other costs of enforcement. Unless the employer previously took steps to draft its health plan documents and negotiate its vendor contracts to provide otherwise, most vendor provided plans typically assign these liabilities to the sponsoring employer or a member of its management by naming that employer or the management person the “plan administrator” and/or “named fiduciary” responsible for those activities and liabilities, requiring the plan sponsor to indemnify the vendor for costs and liabilities arising from the performance of actions under the plan even when those actions don’t comply with ERISA fiduciary or other legal standards applicable to the performance of those duties under the plan, or both, and other contractual or plan provisions that shift liabilities and costs to the plan sponsor.
To mitigate their exposure to these liabilities and costs, employer or other health plan sponsors should consider arranging for an independent legal compliance and risk assessment of their health plan, its terms, materials and operations to help mitigate the sponsoring employer’s exposure to self-identify, self-report on IRS Form 2848 and pay the $100 per day per violation excise tax liability now generally required under the Internal Revenue Code for any such violation.
Beyond mitigating a plan sponsor’s Form 8928 reporting and associated excise tax exposures, an independent compliance audit also can mitigate other risks and exposures for the sponsoring employer, the plan and its fiduciaries, the cost of which the sponsoring employer often bears financial responsibility for funding pursuant to the contractual indemnification and funding obligations entered into in connection with the establishment and maintenance of the plan, the fiduciary role, if any, of the employer with respect to the plan, or both. Accordingly, a timely and appropriate review is likely to help mitigate other risks and liabilities such as:
- Fiduciary liability that can arising from failing to administer the plan in accordance with these and other federal health plan mandates under ERISA;
- Unanticipated benefit costs and liabilities, which for self-insured plans are likely to be particularly burdensome if compliance issues are not identified and corrected before applicable deadlines to pay and submit claims to the stop-loss or other insurer expire (usually at or shortly after the close of a plan year or if earlier, contract termination);
- Benefit costs and penalties for wrongful coordination of benefits with Medicare, Medicaid, DOD and certain other plans or coverage in violation of Secondary Payer and other mandates; and
- Costs of defending and settling audits, litigation and other government or participant enforcement actions.
Since prompt self-audit and correction can help mitigate all of these liabilities, business leaders of employers sponsoring health plans should act promptly to engage experienced legal counsel experienced with health plan laws and operations to advise the plan sponsor about how to audit their group health plan’s plan documents, materials and operations for compliance with these and other federal health plan rules within the scope of attorney-client privilege while managing tax, financial, benefit and fiduciary liability exposures to deal with potential compliance concerns that the review might discover as well as mitigate risks that could result if the audit is improperly structured or conducted.
Prepare To Respond To Potential Health Reform & Other Health Plan Improvement
Beyond identifying and addressing existing compliance concerns and other risks associated with prior or existing plan design or administration, most employer and other sponsors also will want to review the health plan document and materials and associated insurance, third-party administration and other health plan vendor contracts pursuant to which the health plan is established, maintained and administered to identify requirements and opportunities to respond quickly to make changes when and if health care reform happens as well as for other opportunities to mitigate existing risks and costs.
As most commentators expect some type of regulatory or statutory health plan relief to result from the current health care reform debates in Congress, employer and other health plan sponsors desiring to accelerate their ability to take advantage of any forthcoming relief should familiarize themselves with the procedures required under existing plan terms, contracts and rules to modify their programs in response to these changes. Almost certainly, plan sponsors should anticipate needing to adopt some amendments to plan documents, summary plan descriptions and other materials to take advantage of any legislative or statutory relief. Plan sponsors also need to keep in mind that their vendor contracts with administrators, group, stop-loss or captive insurers, and other vendors likely also will require the plan sponsor to notify and negotiate with its vendors to secure their agreement before adopting these changes to avoid violating those vendor agreements and prudently to arrange for appropriate implementation and administration of the modified plan design and terms. Identification of the contractual and plan requirements and commencement of discussions with the relevant vendors can help expedite the planning and implementation of any desired plan modifications the plan sponsor elects to make in response to any statutory or regulatory reforms.
While preparing for anticipated health care reforms, most plan sponsors also will want to review their plans and vendor contracts for other potential opportunities to mitigate risks or expenses. With respect to existing and future liability mitigation, each plan sponsor generally should carefully assess the allocation of fiduciary responsibility and liability between the sponsoring employer, members of its management or other workforce team, and vendors to identify potential areas where the contract may assign named or other plan administrator or other fiduciary status and liability to the plan sponsor or a member of its workforce for duties outsourced to a vendor. Sponsoring employers or their management may want to initiate negotiations with the vendor to reallocate the fiduciary role and responsibility to the party responsible for performance of the specific duties, enhancement of performance guarantees, indemnifications and insurance coverage for proper performance of the outsourced duties by the vendor in accordance with the plan terms, including any mandates imposed by the ACA and other federal laws in form and operation, and other safeguards or, if the vendor is unwilling to consider these changes, begin searching for a replacement vendor willing to provide better accountability for its actions with respect to the services it is hired to perform.
Except in rare circumstances where the sponsoring employer has carefully contracted to transfer fiduciary liability to its insurer or administrator and otherwise does not exercise or have a fiduciary obligation to exercise discretion or control over these responsibilities, employers sponsoring group health plans that violate federal mandates like the out-of-pocket limit often ultimately bear some or all of these liabilities even if the violation actually was committed by a plan vendor hired to administer the program either because the plan documents name the employer as the “named fiduciary” or “plan administrator” under ERISA, the employer or a member of its management named in the plan generally bears fiduciary responsibility functionally for selection or oversight of the culpable party, the employer signed a contract, resolution or plan document obligating the employer to indemnify the service provider for the liability, or a combination of these reasons.
Since prompt self-audit and correction can help mitigate all of these liabilities as well as help to preserve access to stop-loss or other reinsurance coverage, if any, applicable to help pay for some or all of any additional benefit liabilities resulting from these benefit mandates, business leaders of companies offering group health plan coverage should act quickly to engage experienced legal counsel for their companies for advice about how to audit their group health plan’s compliance with these and other federal health plan rules within the scope of attorney-client privilege while managing tax, financial, benefit and fiduciary liability exposures to deal with potential compliance concerns that the review might discover as well as mitigate risks that could result if the audit is improperly structured or conducted.
While businesses inevitably will need to involve or coordinate with their accounting, broker, and other vendors involved with the plans, businesses generally will want to get legal advice in a manner that preserves their potential to claim attorney-client privilege to protect against discovery in the event of future enforcement or litigation actions sensitive discussions and analysis about compliance audits, plan design choices, and other risk management and liability planning as well as to get help identifying potential plan design, contracting, procedural or other changes that may be needed to fix compliance deficiencies and mitigate other risks, particularly in light of complexity of the exposures and risks.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health and othre employee benefit, financial services, health care and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk.
Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
Throughout her career, she has helped a diverse array of clients manage, administer and defend employee and other workforce, vendors and suppliers, their recruitment, selection, performance management, contracting, investigation, discipline and termination; health and other employee benefits; compensation; safety; governance; compliance and internal controls; strategic planning, process and quality improvement; change management; trade secret and other privacy, data security and data breach;; crisis preparedness and response; internal, government and third-party reporting relations, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked extensively throughout her career with employers, health and other employee benefit plans, insurers, managed care organizations, health care clearinghouses, health care providers, their business associates, employers, banks and other financial institutions, management services organizations, professional and trade associations, accreditation agencies, auditors, technology and other vendors and service providers, and others on benefit and insurance program legal and operational compliance, risk management, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending plan sponsors, fiduciaries, service providers, managed care organizations, insurers, self-insured health plans and other payers. Her experience includes both leading edge work designing and administering programs, as well as defending clients in connection with audits and enforcement actions by OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC, OSHA, Department of Insurance, Department of Justice and state attorneys’ general and other federal and state agencies; accreditation and quality organizations; private litigation and other federal and state health care industry investigation, enforcement including insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other nonpar insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns. Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
A lead policy advisor to the Government of Bolivia on its pension privitization project and involved in U.S. federal and state as well as cross border workforce, pension, health care, Social Security, immigration, and tax regulatory and statutory reform throughout her adult life, Ms. Stamer also is widely sought out for her thoughtleadership and assistance with domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; a ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
 Comments Off on Employers Review Health Plans Now To Avoid Excise Taxes & Other Current Law Plan Risks & Ready For Health Reform |
Comments Off on Employers Review Health Plans Now To Avoid Excise Taxes & Other Current Law Plan Risks & Ready For Health Reform |  4980D, 4980H, 6039D, ACA, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, Corporate Compliance, corporate governance, directors, employee, Employee Benefits, Employer, Employment, ERISA, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, IRC, Management, Mental Health, Mental Health Parity, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Premium Subsidies, preventive care, Reporting & Disclosure, SBC, Uncategorized, Wellness Programs | Tagged: Americas Health Care Act, Employee Benefits, Employer, Health Benefits, Health Care Reform, Health Plans, Obamacare, Trump Care |
4980D, 4980H, 6039D, ACA, board of directors, Brokers, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims Administration, compliance, Corporate Compliance, corporate governance, directors, employee, Employee Benefits, Employer, Employment, ERISA, Fair Labor Standards Act, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health Care, health insurance, health insurance marketplace, health plan, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, IRC, Management, Mental Health, Mental Health Parity, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Premium Subsidies, preventive care, Reporting & Disclosure, SBC, Uncategorized, Wellness Programs | Tagged: Americas Health Care Act, Employee Benefits, Employer, Health Benefits, Health Care Reform, Health Plans, Obamacare, Trump Care |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 24, 2017
Health plans, their fiduciaries and sponsors, health insurers, health care providers, health care clearinghouses (“covered entities”) and their business associates must get and keep your business associate (BA) agreements (BAAs) in place, up-to-date, and readily available for inspection in accordance with the Health Insurance Portability & Accountability Act (HIPAA) Privacy Rule, 45 C.F.R. Part 160 and Subparts A and E of Part 164 (Privacy Rule). That’s the clear message to covered entities and their business associates in the April 17, 2017 HIPAA Resolution Agreement just announced by the Department of Health & Human Services (HHS) Office of Civil Rights (OCR) with the Center for Children’s Digestive Health (CCDH).
While the Resolution Agreement relates to breaches of the BAA requirements of a small pediatric practice, all health plans, health care providers and other covered entities and business associates should focus on the adequacy of their BAAs and their BAA record keeping. HIPAA compliance surveys reflect deficiencies with the BAA rules are common throughout the industry. These findings and the involvement of BAs in data breaches or other OCR enforcement activities suggest a high probability that many other covered entities and business associates may be sitting ducks for similar sanctions. See e.g., HIPAA Compliance Survey Churns Up Many Business Associate Problems (January 3, 2017). Consequently, all covered entities and business associates generally should treat the CCDH Resolution Agreement as a message to review and correct as necessary their organizations’ compliance and recordkeeping to minimize their exposure to potential sanctions from violations of the HIPAA business associate rules.
The HIPAA Business Associate Agreement Requirements
OCR’s announcement of the CCDH Resolution Agreement is the latest in a growing series of HIPAA enforcement actions showing the growing risk covered entities and their business associates face for failing to take appropriate steps to comply with the BAA and other Privacy Rule requirements of HIPAA.
As compliance audits and surveys of covered entities and business associates suggest a high level of noncompliance with the business associate agreement requirements among covered entities and business associates, While the ever-growing list of Resolution Agreements and Civil Monetary Penalties announced by OCR cover a variety of categories of HIPAA violations, the CCDH Resolution Agreement highlights the importance of covered entities and their business associates ensuring that before the BA creates, accesses, receives, discloses, retains or destroys any PHI for the covered entity, a BAA meeting the Privacy Rule requirements is signed and retained for at least the six-year period the Privacy Rule requires in a manner easily producible when and if OCR or another agency asks for a copy as part of an investigation or other compliance audit. See Privacy Rule §§ 164.502(e), 164.504(e), 164.532(d) and (e).
The Privacy Rule requires that covered entities and business associates enter into a written and signed business associate agreement that contains the elements specified in Privacy Rule § 164.504(e) before the business associate creates, uses, accesses or discloses PHI of the covered entity. Meanwhile, the Privacy Rule recordkeeping requirements require that covered entities and BAs maintain copies of these BAAs for a minimum of six years.
Violations of the Privacy Rule can carry stiff civil or even criminal penalties Pursuant to amendments to HIPAA enacted as part of the HITECH Act, civil penalties typically do not apply to violations punished under the criminal penalty rules of HIPAA set forth in Social Security Act , 42 U.S.C § 1320d-6 (Section 1177).
Under Section 1177, the criminal enforcement provisions of HIPAA authorize the Justice Department to prosecute a person who knowingly in violation of the Privacy Rule (1) uses or causes to be used a unique health identifier; (2) obtains individually identifiable health information relating to an individual; or (3) discloses individually identifiable health information to another person, punishable by the following criminal sanctions and penalties:
- A fine of up to $50,000, imprisoned not more than 1 year, or both;
- If the offense is committed under false pretenses, a fine of up to $100,000, imprisonment of not more than 5 years, or both; and
- If the offense is committed with intent to sell, transfer, or use individually identifiable health information for commercial advantage, personal gain, or malicious harm, a fine of up to $250,000, imprisoned not more than 10 years, or both.
In contrast, as amended by the HITECH Act, the civil enforcement provisions of HIPAA empower OCR to impose Civil Monetary Penalties on both covered entities and BAs for violations of any of the requirements of the Privacy or Security Rules. The penalty ranges for civil violations depends upon the circumstances associated with the violations and are subject to upward adjustment for inflation. As most recently adjusted here effective September 6, 2016, the following currently are the progressively increasing Civil Monetary Penalty tiers:
- A minimum penalty of $100 and a maximum penalty of $50,000 per violation, for violations which the CE or BA “did not know, and by exercising reasonable diligence would not have known” about using “the business care and prudence expected from a person seeking to satisfy a legal requirement under similar circumstances;”
- A minimum penalty of $1,000 and a maximum penalty of $50,000 per violation, for violations for “reasonable cause” which do not rise to the level of “willful neglect” where “reasonable cause” means the “circumstances that would make it unreasonable for the covered entity, despite the exercise of ordinary business care and prudence, to comply with the violated Privacy Rule requirement;”
- A minimum penalty of $10,000 and a maximum penalty of $50,000 per violation, for violations attributed to “willful neglect,” defined as “the conscious, intentional failure or reckless indifference to the obligation to comply” with the requirement or prohibition; and
- A minimum penalty of $50,000 and a maximum penalty of $1.5 million per violation, for violations attributed to “willful neglect” not remedied within 30 days of the date that the covered entity or BA knew or should have known of the violation.
For continuing violations such as failing to implement a required BAA, OCR can treat each day of noncompliance as a separate violation. However, sanctions under each of these tiers generally are subject to a maximum penalty of $1,500,000 for violations of identical requirements or prohibitions during a calendar year. For violations such as the failure to implement and maintain a required BAA where more than one covered entity bears responsibility for the violation, OCR an impose Civil Monetary Penalties against each culpable party. OCR considers a variety of mitigating and aggravating facts and circumstances when arriving at the amount of the penalty within each of these applicable tiers to impose.
While criminal enforcement of HIPAA remains relatively rare, a review of the OCR enforcement record in recent years makes clear that civil enforcement of HIPAA and the sanctions imposed is growing. See e.g., $400K HIPAA Settlement Shows Need To Conduct Timely & Appropriate Risk Assessments; $5.5M Memorial HIPAA Resolution Agreement Shows Need To Audit. For more examples, also see here.
CCDH Sanctions For Violation Of HIPAA Business Associate Agreement Rules
The CCDH Resolution Agreement arises from violations of this requirement that OCR says it discovered as a result of a compliance review conducted in response to an OCR investigation of a CCDH business associate, FileFax, Inc. According to OCR, OCR found from the compliance review of CCDH triggered by OCR’s investigation of FileFax that while CCDH began disclosing PHI to Filefax in 2003 and that Filefax stored records containing protected health information (PHI) for CCDH, neither CCDH nor Filefax could produce a signed Business Associate Agreement (BAA) covering their relationship for any period before October 12, 2015.
Based on the resulting investigation, OCR concluded:
- CCDH failed to obtain a BAA providing written assurances from Filefax that it would appropriately safeguard the PHI in Filefax’s possession or control satisfactory assurances as required by Privacy Rule §164.502(e); and
- Because CCDH failed to secure the required BAA, it violated the Privacy Rule by impermissibly disclosing the PHI of at least 10,728 individuals to Filefax when CCDH transferred the PHI to Filefax without obtaining the requisite BAA from Filefax (Covered Conduct).
In the Resolution Agreement, CCDH agrees to pay HHS $31,000.00 (Resolution Amount) and enter into and comply with a Corrective Action Plan (CAP) in return for OCR’s release of CCDH from liability for “any actions it may have against CCDH under the HIPAA Rules” for the Covered Conduct. The Resolution Agreement only settles the civil monetary penalty and other OCR enforcement liabilities of CCDH with respect to the Covered Conduct. Its provisions expressly state the Resolution Agreement does not affect any exposures of CCDH to CCDH to OCR civil monetary penalties or other enforcement for any HIPAA violations other than the Covered Conduct.
Perhaps even more noteworthy given the HITECH Act’s provisions coordinating the civil and criminal sanctions of HIPAA, while the Resolution Agreement provides no clear indication that the Justice Department might be considering criminally prosecuting CCDH or any other party in relation to the Covered Conduct, the Resolution Agreement also expressly states that its provisions do not affect CCDH’s potential exposure, if any, to criminal prosecution by the Justice Department for a criminal violation of the Privacy Rules under Section 1177 of the Social Security Act.
Implications For Covered Entities & Business Associates
Covered entities and their business associates should heed the CCDH Resolution Agreement as a strong message from OCR to ensure their organizations are complying with HIPAA’s BAA and other requirements. The Resolution Agreement makes clear that the starting point of this compliance effort must be obtaining and maintaining the requisite BAAs for each BA relationship.
To position their organizations to withstand potential investigation by OCR, covered entities and BAs should start by conducting a well-documented audit within the scope of attorney-client privilege both to verify that an appropriate, signed BAA is in place for each BA relationship as well as adequacy of processes for identifying business associate relationships, ensuring that signed BAAs are in effect before BAs access any PHI, and for investigating, reporting and resolving any breaches of the HIPAA Privacy or Security Rules that may arise in the course of operations.
Conducting this audit as soon as possible is particularly important in light of reported findings of widespread compliance concerns. See HIPAA Compliance Survey Churns Up Many Business Associate Problems (January 3, 2017). As the audit process could identify potential violations or other legally sensitive concerns, covered entities and business associates generally will want to arrange for this audit and evaluation to be conducted under the supervision of legal counsel experienced with HIPAA within or pursuant to processes structured with the assistance of legal counsel within the scope of attorney-client privilege.
Beyond confirming all necessary BAAs are in place, covered entities and business associates also generally will want to evaluate the adequacy of BAs’ processes and procedures for maintaining compliance with the Privacy and Security Rules as well as processes and procedures for responding to audits, investigations and complaints, reporting and addressing breaches of electronic and other PHI and other possible compliance concerns under HIPAA and other related laws. In many instances, parties may n wish to revise and strengthen existing BAAs to more specifically define these policies and procedures more specifically as well as indemnification, cyber or other liability coverage requirements and other contractual provisions for allocating potential costs and liabilities arising from breaches, audits, investigations and other expenses associated with the administration of these provisions.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to manage and defend compliance, public policy, regulatory, staffing and other operations and risk management concerns. A core focus of this work includes work to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; dealings with JCHO and other accreditation and quality organizations; investigation and defense of private litigation and other federal and state health care industry investigations and enforcement; insurance or other liability management and allocation; process and product development; managed care, physician and other staffing, business associate and other contracting; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.
In the course of this work, Ms. Stamer has accumulated extensive experience helping health industry clients manage workforce, medical staff, vendors and suppliers, medical billing, reimbursement, claims and other provider-payer relations, business partners, and their recruitment, performance, discipline, compliance, safety, compensation, benefits, and training, board, medical staff and other governance; compliance and internal controls; strategic planning, process and quality improvement; change management; assess, deter, investigate and address staffing, quality, compliance and other performance; meaningful use, EMR, HIPAA and other data security and breach and other health IT and data; crisis preparedness and response; internal, government and third-party reporting, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
Author of leading works on HIPAA and other privacy and data security works and the scribe leading the American Bar Association Joint Committee on Employee Benefits Annual Agency Meeting with OCR, her experience includes extensive compliance, risk management and data breach and other crisis event investigation, response and remediation under HIPAA and other laws.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked closely with a diverse range of physicians, hospitals and healthcare systems, DME, Pharma, clinics, health care providers, managed care, insurance and other health care payers, quality assurance, credentialing, technical, research, public and private social and community organizations, and other health industry organizations and their management deal with governance; credentialing, patient relations and care; staffing, peer review, human resources and workforce performance management; outsourcing; internal controls and regulatory compliance; billing and reimbursement; physician, employment, vendor, managed care, government and other contracting; business transactions; grants; tax-exemption and not-for-profit; licensure and accreditation; vendor selection and management; privacy and data security; training; risk and change management; regulatory affairs and public policy and other concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other nonpar, insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns.
In connection with this work, Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA, FACTA, trade secret and other information privacy and data security rules, including the establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and and enforcement, and a host of other related concerns. Her clients include public and private health care providers, health insurers, health plans, technology and other vendors, and others.
Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, MGMA, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; a ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
 Comments Off on Latest HIPAA Resolution Agreement Drives Home Importance Of Maintaining Current, Signed Business Associate Agreements |
Comments Off on Latest HIPAA Resolution Agreement Drives Home Importance Of Maintaining Current, Signed Business Associate Agreements |  ARRA, Attorney-Client Privilege, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, employee, Employee Benefits, Employer, Employers, Employment, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Patient Empowerment, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Uncategorized | Tagged: Business Associate, Health Care, Health Insurer, Health Plans, HIPAA, HIPAA OCR, HIPAA Privacy, HITECH, Insurer, Technology, tpa |
ARRA, Attorney-Client Privilege, Cafeteria Plans, church plan, Civil Monetary Penalties, Civil Rights, Claims, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, employee, Employee Benefits, Employer, Employers, Employment, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Patient Empowerment, Physician, Plan Admistrator, Privacy, Professional Liability, Protected Health Information, Provider, Risk Management, Uncategorized | Tagged: Business Associate, Health Care, Health Insurer, Health Plans, HIPAA, HIPAA OCR, HIPAA Privacy, HITECH, Insurer, Technology, tpa |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 12, 2017
Metro Community Provider Network (MCPN), a federally-qualified health center (FQHC), must pay $400,000 and implement a corrective action plan to resolve U.S. Department of Health and Human Services, Office for Civil Rights (OCR) charges it violated the Health Insurance Portability and Accountability Act of 1996 (HIPAA) Security Rule by failing to implement a security management process to safeguard electronic protected health information (ePHI). The latest in a growing series of high-dollar HIPAA settlements and penalty assessments, it reminds health plans and other HIPAA-covered entities of the importance of conducting risk assessments and other actions to prevent and prepare to respond to hacking and other data breach and security events.
The Resolution Agreement and Corrective Action Plan, like most others before it, resulted from an investigation opened in response to a breach report. On January 27, 2012, MCPN filed a breach report with OCR indicating that a hacker accessed employees’ email accounts and obtained 3,200 individuals’ ePHI through a phishing incident. OCR’s investigation revealed that MCPN took necessary corrective action related to the phishing incident. However, the investigation also revealed that MCPN failed to conduct a risk analysis until mid-February 2012 – well after the hacking incident reported in the breach report.Prior to the breach incident, MCPN had not conducted a risk analysis to assess the risks and vulnerabilities in its ePHI environment, and, consequently, had not implemented any corresponding risk management plans to address the risks and vulnerabilities identified in a risk analysis.
When MCPN finally conducted a risk analysis, OCR found that risk analysis, as well as all subsequent risk analyses, were insufficient to meet the requirements of the Security Rule.
OCR made a point in announcing the Resolution Agreement of noting it considered MCPN’s status as a FQHC when balancing the significance of the violation with MCPN’s ability to maintain sufficient financial standing to ensure the provision of ongoing patient care. MCPN provides primary medical care, dental care, pharmacies, social work, and behavioral health care services throughout the greater Denver, Colorado metropolitan area to approximately 43,000 patients per year, a large majority of whom have incomes at or below the poverty level. It is likely that OCR would have imposed a much greater settlement amount had the covered entity not been a FQHC serving the poor.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Health Care,” “Labor & Employment,” “Tax: Erisa & Employee Benefits” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 29 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer supports these organizations and their leaders on both a real-time, “on demand” basis as well as outsourced operations or special counsel on an interim, special project, or ongoing basis with strategic planning and product and services development and innovation; workforce and operations management, crisis preparedness and response as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
Throughout her career, she has helped health industry clients manage workforce, medical staff, vendors and suppliers, medical billing, reimbursement, claims and other provider-payer relations, business partners, and their recruitment, performance, discipline, compliance, safety, compensation, benefits, and training ;board, medical staff and other governance; compliance and internal controls; strategic planning, process and quality improvement; change management; assess, deter, investigate and address staffing, quality, compliance and other performance; meaningful use, EMR, HIPAA and other data security and breach and other health IT and data; crisis preparedness and response; internal, government and third-party reporting, audits, investigations and enforcement; government affairs and public policy; and other compliance and risk management, government and regulatory affairs and operations concerns.
Author of leading works on HIPAA and other privacy and data security works and the scribe leading the American Bar Association Joint Committee on Employee Benefits Annual Agency Meeting with OCR, her experience includes extensive compliance, risk management and data breach and other crisis event investigation, response and remediation under HIPAA and other laws.
The American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, a Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Member and Compliance Chair of the National Kidney Foundation of North Texas, Ms. Stamer has worked closely with a diverse range of physicians, hospitals and healthcare systems, DME, Pharma, clinics, health care providers, managed care, insurance and other health care payers, quality assurance, credentialing, technical, research, public and private social and community organizations, and other health industry organizations and their management deal with governance; credentialing, patient relations and care; staffing, peer review, human resources and workforce performance management; outsourcing; internal controls and regulatory compliance; billing and reimbursement; physician, employment, vendor, managed care, government and other contracting; business transactions; grants; tax-exemption and not-for-profit; licensure and accreditation; vendor selection and management; privacy and data security; training; risk and change management; regulatory affairs and public policy and other concerns.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; JCHO and other accreditation and quality organizations; private litigation and other federal and state health care industry investigation, enforcement including insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns.
Past Chair of the ABA Managed Care & Insurance Interest Group and, a Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also has extensive health care reimbursement and insurance experience advising and defending health care providers, payers, and others about Medicare, Medicaid, Medicare and Medicaid Advantage, Tri-Care, self-insured group, association, individual and group and other health benefit programs and coverages including but not limited to advising public and private payers about coverage and program design and documentation, advising and defending providers, payers and systems and billing services entities about systems and process design, audits, and other processes; provider credentialing, and contracting; providers and payer billing, reimbursement, claims audits, denials and appeals, coverage coordination, reporting, direct contracting, False Claims Act, Medicare & Medicaid, ERISA, state Prompt Pay, out-of-network and other nonpar insured, and other health care claims, prepayment, post-payment and other coverage, claims denials, appeals, billing and fraud investigations and actions and other reimbursement and payment related investigation, enforcement, litigation and actions.
Heavily involved in health care and health information technology, data and related process and systems development, policy and operations innovation and a Scribe for ABA JCEB annual agency meeting with OCR for many years who has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use, Ms. Stamer also is widely recognized for her extensive work and leadership on leading edge health care and benefit policy and operational issues including meaningful use and EMR, billing and reimbursement, quality measurement and reimbursement, HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and many other concerns. Her work includes both regulatory and public policy advocacy and thought leadership, as well as advising and representing a broad range of health industry and other clients about policy design, drafting, administration, business associate and other contracting, risk assessments, audits and other risk prevention and mitigation, investigation, reporting, mitigation and resolution of known or suspected violations or other incidents and responding to and defending investigations or other actions by plaintiffs, DOJ, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others.
Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks and other financial institutions, and others on risk management and compliance with HIPAA, FACTA, trade secret and other information privacy and data security rules, including the establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and and enforcement, and a host of other related concerns. Her clients include public and private health care providers, health insurers, health plans, technology and other vendors, and others. In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, MGMA, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy concerns in Pensions, healthcare, workforce, immigration, tax, education and other areas.
A popular lecturer and widely published author on health industry concerns, Ms. Stamer continuously advises health industry clients about compliance and internal controls, workforce and medical staff performance, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other related concerns by her service in the leadership of the Solutions Law Press, Inc. Coalition for Responsible Health Policy, its PROJECT COPE: Coalition on Patient Empowerment, and a broad range of other professional and civic organizations including North Texas Healthcare Compliance Association, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children (now Warren Center For Children); current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, past Representative and chair of various committees of ABA Joint Committee on Employee Benefits; a ABA Health Law Coordinating Council representative, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved. For information about republication or other use, please contact Ms. Stamer here.
 Comments Off on $400K HIPAA Penalty Teaches Risk Assessment Importance |
Comments Off on $400K HIPAA Penalty Teaches Risk Assessment Importance |  board of directors, Civil Monetary Penalties, compliance, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, Employee Benefits, Employer, Employers, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, HIPAA, HR, Human Resources, Identity Theft, Uncategorized | Tagged: Data Security, HIPAA, Privacy |
board of directors, Civil Monetary Penalties, compliance, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, Employee Benefits, Employer, Employers, health benefit, Health Benefits, health Care, health insurance, health plan, Health Plans, HIPAA, HIPAA, HR, Human Resources, Identity Theft, Uncategorized | Tagged: Data Security, HIPAA, Privacy |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
April 5, 2017
Employers looking for cost-effective opportunities to sweeten the perceived value their compensation and fringe benefit packages periodically should re-examine their policies for reimbursement of employees for ordinary and necessary business expenses an employee incurs in connection with the performance of his duties, such as:
- Required work clothes or uniforms not appropriate for everyday use.
- Supplies and tools for use on the job.
- Business use of a car.
- Business meals and entertainment.
- Business travel away from home.
- Business use of a home.
- Work-related education.
Businesses generally consider a wide range of factors when deciding what expenses to reimburse to employees. In arriving at these decisions, however, many businesses overlook the opportunity to stretch the overall compensation dollars by reimbursing employees for business expenses in lieu of paying cash compensation to the employee but requiring the employee to use after tax dollars to pay business expenses not reimbursed by the employer.
While many employers believe “cash is king” when paying employees, paying employees more cash in lieu of reimbursing employees for business often increases the employment tax liability of the employer while also unwittingly diminishing the value of the cash compensation paid to the employee because of federal tax rules governing individual deductions a business expenses.
While the Internal Revenue Code and associated Internal Revenue Service regulations impose special rules for certain categories of employment, federal tax law generally allows businesses both:
- To deduct from the gross income of the business for purposes of determining its adjusted gross income those amounts the business pays as wages as well as amounts paid to reimburse an employee for ordinary and necessary business expenses expended by the employee in the performance of his duties and to exclude such amounts for calculating the employment tax liabilities of both the employer and the employee; and
- In many, but not all instances, to exclude all or some of the reimbursement amount from the taxable wages of the employee for income tax and/or employment tax purposes.
The income and employment tax treatment of business expenses paid by an employee generally is much less favorable when an employee seeks to deduct or exclude xpenditures made for ordinary and necessary business expenses from taxable income.
While federal income tax rules generally allow businesses to deduct ordinary and business expenses directly from gross income to arrive at their taxable adjusted gross income, federal tax rules are more restrictive concerning the deduction of business expenses by employees for income tax purposes and provides no easy mechanism to claim credit for such amounts for employment tax purposes.
In general, the Internal Revenue Code generally only allows employees who otherwise have sufficient deductible expenses to itemize deductions to claim any business expenses as a deduction when calculating their federal income taxes. Depending on the income of the workforce and particularly in the case of lower income workers, the itemization requirement effectively bars a large percentage of employees from any possibility of deducting business expenses incurred in the performance of their work.
Beyond the requirement to itemize, the Internal Revenue Code also imposes a second hurdle that further restricts the deductibility of business expenses when claimed by an employee versus a business. Specifically, the Internal Revenue Code generally only allows an employee to deduct business expenses paid by the employee to the extent those expenses exceed 2% of the employee’ adjusted gross income. This means that even those employees who qualify to file itemize deductions cannot deduct the initial 2% of the ordinary and necessary business expenses the employee pays and connection of the performance of his job even though the Internal Revenue Code would allow the employer to deduct the full amount of amounts paid to reimburse the employee for those same expenses.
Since most employees understand that the purchasing power of any cash compensation they receive from the employer is reduced by the amount of any expenses that they pay but are not reimbursed for, considering reimbursing employees for expenses in lieu of paying the employee cash, then requiring the employee to pay those expenses out of taxable income.
Of course, when considering whether to pay or reimburse employee expenses, employers also should evaluate and verify that their planned treatment of an expenditure and its reimbursement otherwise complies with any union or other contracts, as well as any applicable federal and state occupational safety, wage and hour and other laws.
Regardless of whether the employer or the employee plans to claim a business expense for tax purposes, an employer should encourage its employees to keep, and if reimbursing the employee, submit good records for proof of income and expenses. Employers reimbursing business expenses may wish to educate employees about both the tax and financial value of these reimbursement benefits as a part of the overall compensation package provided to employees. Even where an employer does not reimburse its employees all or part of an otherwise deductible business expense, however, it also may want to share Internal Revenue Service resources like “IRS Publication 529, Miscellaneous Deductions,” and “Publication 463, Travel, Entertainment, Gift and Car Expenses” with employees to help educate employees about these tax rules and their opportunities and responsibilities.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Periodically Reevaluate Employee Business Expense Reimbursement Practices |
Comments Off on Periodically Reevaluate Employee Business Expense Reimbursement Practices |  employee, Employee Benefits, Employment, Employment Discrimination, Employment Tax, HR, Human Resources, Income Tax, IRC, Tax, Unemployment Benefits, Unemployment Insurance | Tagged: benefits, Compensation, Employee, Employer, Employment Tax, expense reimbursement, Fringe Benefits, Income Tax |
employee, Employee Benefits, Employment, Employment Discrimination, Employment Tax, HR, Human Resources, Income Tax, IRC, Tax, Unemployment Benefits, Unemployment Insurance | Tagged: benefits, Compensation, Employee, Employer, Employment Tax, expense reimbursement, Fringe Benefits, Income Tax |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
March 1, 2017
Heads up tax-exempt and governmental entities, employer and other qualified employee benefit plan sponsor, fiduciaries, administrators, and recordkeepers and their management, accountants, attorneys, and other service providers and advisors. Changes to the procedures that Internal Revenue Service (IRS) Tax Exempt and Government Entities TE/GE examiners use to make and enforce Information Document Request (IDR) in connection with an audit or other examination make it more important than ever that taxpayers use special care to collect, organize and maintain all of the data and documentation that examiners are likely to request in IDR and take other steps to prepare in advance to respond to an IDR.
New procedures announced in the February 27, 2017 Memorandum For All TE/GE Examiners On New Process For All Information Document Requests and scheduled to take effect April 1 seek to expedite the examination process and reduce backlogs. To accomplish this, the new procedures impose specific, tightened timelines for responding to IDRs and IRS follow and enforcement of data and document productions demanded by an IDR. As part of these changes, the new procedures shorten the time that the examiners will issue early subpoena warnings and subpoenas to compel taxpayers to produce requested data.
Taxpayers unable to respond in a timely fashion risk of both triggering these perilous enforcement procedures and an enhanced risk that IRS examiners will view the delay as an indication that the taxpayer may not be using the internal controls and processes expected by the IRS rules. Accordingly, taxpayers should seek advise from experienced legal counsel about the policies, practices, data and information they might be expected to need to respond to a IDR or other government investigation, recommendations for conducting their operations to promote their ability to efficiently assemble and produce the necessary data, records and other information to respond to a IDR or other investigation, audit or enforcement action, and other appropriate steps to position their organizations timely to recognize and produce the often substantial data generally demanded by an IRD and minimize risks of liability likely to arise from an IRS examination or other governmental or private investigation or action.
About The Author
Recognized by LexisNexis® Martindale-Hubbell® as a “AV-Preeminent” (Top 1%/ the highest) and “Top Rated Lawyer,” with special recognition as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, the author of this update is widely known for her 28 plus years’ of work in health care, health benefit, health policy and regulatory affairs and other health industry concerns as a practicing attorney and management consultant, thought leader, author, public policy advocate and lecturer.
Throughout her adult life and nearly 30-year legal career, Ms. Stamer’s legal, management and governmental affairs work has focused on helping health industry, health benefit and other employee benefit, insurance, technology and other highly regulated organizations and their management use the law, performance and risk management tools and process to manage people, performance, quality, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps these and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup legal and operational crises large and small that arise in the course of operations.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, current American Bar Association (ABA) International Section Life Sciences Committee Vice Chair, Scribe for the ABA Joint Committee on Employee Benefits (JCEB) Annual OCR Agency Meeting, former Vice President of the North Texas Health Care Compliance Professionals Association, past Chair of the ABA Health Law Section Managed Care & Insurance Section, past ABA JCEB Council Representative, past Board President of Richardson Development Center (now Warren Center) for Children Early Childhood Intervention Agency, past North Texas United Way Long Range Planning Committee Member, and past Board Compliance Chair of the National Kidney Foundation of North Texas, and Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, Ms. Stamer’s includes nearly 30 years’ of work with a diverse range of health industry clients on an extensive range of matters.
Ms. Stamer has worked closely with health industry, managed care and insurance, employee benefit, financial services, technology, restructuring, retail, hospitality, manufacturing, consulting, sales, energy, import-export, staffing and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of staffing, human resources and workforce performance management, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans and insurers, managed care organizations, health care clearinghouses, their business associates, employers, banks and other financial institutions, management services organizations, professional associations, medical staffs, accreditation agencies, auditors, technology and other vendors and service providers, and others on legal and operational compliance, risk management and compliance, public policies and regulatory affairs, contracting, payer-provider, provider-provider, vendor, patient, governmental and community relations and matters including extensive involvement advising, representing and defending public and private hospitals and health care systems; physicians, physician organizations and medical staffs; specialty clinics and pharmacies; skilled nursing, home health, rehabilitation and other health care providers and facilities; medical staff, accreditation, peer review and quality committees and organizations; billing and management services organizations; consultants; investors; technology, billing and reimbursement and other services and product vendors; products and solutions consultants and developers; investors; managed care organizations, insurers, self-insured health plans and other payers; and other health industry clients to establish and administer compliance and risk management policies; comply with requirements, investigate and respond to Board of Medicine, Health, Nursing, Pharmacy, Chiropractic, and other licensing agencies, Department of Aging & Disability, FDA, Drug Enforcement Agency, OCR Privacy and Civil Rights, Department of Labor, IRS, HHS, DOD, FTC, SEC, CDC and other public health, Department of Justice and state attorneys’ general and other federal and state agencies; JCHO and other accreditation and quality organizations; private litigation and other federal and state health care industry investigation, enforcement including insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others, and other compliance, public policy, regulatory, staffing, and other operations and risk management concerns.
Best known for her thoughleadership and experience on health benefit and other health and insurance industy matters, Ms. Stamer has worked throughout her career health care, health benefit and insurance and health information technology, data and related process and systems development, policy and operations design, management, product development, innovation, administration, public policy, regulatory compliance, enforcement, contracting, privacy and data security and related matter. Ms. Stamer continuously advises health and insurance industry clients about licensing, regulatory compliance and internal controls, workforce, agent and broker and medical staff performance, claims and reimbursement, quality, governance, reimbursement, privacy and data security, and other risk management and operational matters. Scribe for ABA JCEB annual agency meeting with OCR for many years, Ms. Stamer also is widely recognized for her extensive work and leadership on HIPAA, FACTA, PCI, IRC and other tax, Social Security, GLB, rade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and concerns including policy design, drafting, administration and training; business associate and other contracting; risk assessments, audits and other risk prevention and mitigation; investigation, reporting, mitigation and resolution of known or suspected breaches, violations or other incidents; and defending investigations or other actions by plaintiffs, OCR, FTC, state attorneys’ general and other federal or state agencies, other business partners, patients and others. Ms. Stamer has worked extensively with health care providers, health plans, health care clearinghouses, their business associates, employers and other plan sponsors, banks, insurers and other financial institutions, and others on trade secret confidentiality, privacy, data security and other risk management and compliance including the design, establishment, documentation, implementation, audit and enforcement of policies, procedures, systems and safeguards, investigating and responding to known or suspected breaches, defending investigations or other actions by plaintiffs, OCR, FTC and other federal or state agencies, reporting known or suspected violations, business associate and other contracting, commenting or obtaining other clarification of guidance, training and enforcement, and a host of other related concerns.
Her clients include public and private health care providers, health insurers, health plans, employers, payroll, staffing, recruitment, insurance and financial services, technology and other vendors, and others. In addition to representing and advising these organizations, she also has conducted training on Privacy & The Pandemic for the Association of State & Territorial Health Plans, as well as HIPAA, FACTA, PCI, medical confidentiality, insurance confidentiality and other privacy and data security compliance and risk management for Los Angeles County Health Department, ISSA, HIMMS, the ABA, SHRM, schools, medical societies, government and private health care and health plan organizations, their business associates, trade associations and others. Ms. Stamer also has authored numerous highly-regarded works and training programs on HIPAA and other data security, privacy and use published by BNA, the ABA and other premier legal industy publishers.
Ms. Stamer also has extensive experience with a diverse array of other human resources and other staffing, services, outsourcing and other workforce, qualified and nonqualified employee benefit, compensation, and related matters, their design, documentation, administration, modification, enforcement and defense and other related operational, compliance and risk management. Her experience includes advising andassisting employer and other plan sponsors, fiduciaries, administrators, vendors and others with and program design, documentation and ongoing administration administration for compliance and defensibility under IRS and other federal and state tax, OFCCP, CAS, SCA, Davis Bacon, SEC and other corporate, ERISA and other federal and state labor and employment, SEC and other corporate, Department of Insurance and other laws and regulations; advising and assisting buyers, sellers, investors, debtors, creditors, trustees, plan fiduciaries and service providers and others in relation to business transactions, restructurings, bankruptcies and other substantial corporate and business events and transactions including significant work involving amendment, termination, windup and restructuring of employee benefit plans and workforce concerns in highly publicized fiduciary, securities or other misconduct investigation and enforcement, bankruptcy, restructuring or other distress situations.
A former lead consultant to the Government of Bolivia on its Pension Privatization Project with extensive domestic and international public policy and governmental and regulatory affairs experience, Ms. Stamer also is widely recognized for regulatory and policy work, advocacy and outreach on healthcare, education, aging, disability, savings and retirement, workforce, ethics, and other policies. Throughout her adult life and career, Ms. Stamer has provided thought leadership; policy and program design, statutory and regulatory development design and analysis; drafted legislation, proposed regulations and other guidance, position statements and briefs, comments and other critical policy documents; advised, assisted and represented health care providers, health plans and insurers, employers, professional. and trade associations, community and government leaders and others on health care, health, pension and retirement, workers’ compensation, Social Security and other benefit, insurance and financial services, tax, workforce, aging and disability, immigration, privacy and data security and a host of other international and domestic federal, state and local public policy and regulatory reforms through her involvement and participation in numerous client engagements, founder and Executive Director of the Coalition for Responsible Health Policy and its PROJECT COPE: the Coalition on Patient Empowerment, adviser to the National Physicians Congress for Healthcare Policy, leadership involvement with the US-Mexico Chamber of Commerce, the Texas Association of Business, the ABA JCEB, Health Law, RPTE, Tax, Labor, TIPS, International Life Sciences, and other Sections and Committees, SHRM Governmental Affairs Committee and a host of other involvements and activities.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also publishes and speaks extensively on health and managed care industry regulatory, staffing and human resources, compensation and benefits, technology, public policy, reimbursement and other operations and risk management concerns. Her insights on these and other related matters appear in the Health Care Compliance Association, Atlantic Information Service, Bureau of National Affairs, The Wall Street Journal, Business Insurance, the Dallas Morning News, Modern Health Care, Managed Healthcare, Health Leaders, and a many other national and local publications. In addition to her many years of service as a scrivener for the ABA JCEB’s meeting with OCR, for instance, she also serves as Chair the Southern California ISSA Health Care Privacy & Security Summit, and an editorial advisory board member, author, program chair or steering committee member, and faculties for a multitude of other programs and publications regarding privacy, data security, technology and other compliance, risk management and operational concerns in the health care, health and other insurance, employee benefits and human resources, retail, financial services and other arenas.Ms. Stamer also shares her thought leadership, experience and advocacy on HIPAA and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association, Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Board Compliance Chair and Board member of the National Kidney Foundation of North Texas, current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposium and chair, faculty member and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, Insurance Thought Leadership and many other prominent publications and speaks and conducts training for a broad range of professional organizations.
For more information about Ms. Stamer or her health industry and other experience and involvements, see here or contact Ms. Stamer via telephone at (469) 767-8872 or via e-mail here.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources here such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or your profile here.
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Employers, Benefit Plans & Exempt Org: Prepare For Shortened Deadlines & Other Changes To IRS Employee Plan & Exempt Organization Exam Documentation Request Procedures |
Comments Off on Employers, Benefit Plans & Exempt Org: Prepare For Shortened Deadlines & Other Changes To IRS Employee Plan & Exempt Organization Exam Documentation Request Procedures |  401(k), Attorney-Client Privilege, board of directors, church plan, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, Employee Benefits, Employer, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Form 5500, HR, Human Resources, Internal Revenue Code, IRC, Pay, pension plan, Plan Admistrator, Retirements, Tax, Tax Qualification, third party administrators, Workforce | Tagged: 401(k), 457 plan, Employee Benefits, Exempt Organizations, IRS, retirement plan, tax exempt, tax qualification, TEGE |
401(k), Attorney-Client Privilege, board of directors, church plan, compensation, compliance, Corporate Compliance, corporate governance, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, Employee Benefits, Employer, Employers, Employment Tax, ERISA, Executive Compensation, Fiduciary Responsibility, Form 5500, HR, Human Resources, Internal Revenue Code, IRC, Pay, pension plan, Plan Admistrator, Retirements, Tax, Tax Qualification, third party administrators, Workforce | Tagged: 401(k), 457 plan, Employee Benefits, Exempt Organizations, IRS, retirement plan, tax exempt, tax qualification, TEGE |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 23, 2017
Employer and other health plan sponsors, fiduciaries and insurers generally should be prepared to prove that they are maintaining and administering their health plans to comply with many Patient Protection and Affordable Care Act (ACA) mandates pending Congressional repeal or reform of the ACA, despite President Trump’s January 20, 2017 Executive Order on “Minimizing the Economic Burden of the Patient Protection and Affordable Care Act Pending Repeal” (Executive Order) because the Federal agencies responsible for the implementation and interpretation of the ACA generally don’t have authority to bar health plan participants and beneficiaries from bringing benefit denial or breach of fiduciary duty lawsuits against health plans or fiduciaries for violating ACA mandates incorporated into the Employee Retirement Income Security Act (ERISA).
In addition to affirming President Trump’s commitment to seek the prompt repeal of the ACA, the Executive Order seeks to mitigate the burden of the ACA pending Congressional repeal by ordering the Departments Health and Human Services (HHS), Labor (DOL), Treasury (Treasury) and other agencies with ACA authority (Agencies) to exercise all available authority and discretion to the “maximum extent permitted by law:”
- To waive, defer, grant exemptions from, or delay the implementation of any provision or requirement of the ACA that would impose a “cost, fee, tax, penalty, or regulatory burden on individuals, families, healthcare providers, health insurers, patients, recipients of healthcare services, purchasers of health insurance, or makers of medical devices, products, or medications.”
- To provide greater flexibility to States and cooperate with them in implementing healthcare programs and to waive, defer, grant exemptions from, or delay the implementation of any provision or requirement of the Act that would impose a fiscal burden on any State;
- For departments and agencies with responsibilities relating to healthcare or health insurance to encourage the development of a free and open market in interstate commerce for the offering of healthcare services and health insurance, with the goal of achieving and preserving maximum options for patients and consumers.
While applicable Agencies are expected to act as quickly as possible to comply with President Trump’s orders, various statutory and procedural requirements almost certainly will limit both the relief granted and the speed with which the Agencies can grant the relief. One obvious place where statutory limitations on Agencies authority almost certainly will impact the availability of relief arises from the ACA’s incorporation of many of its patient protection act group mandates into ERISA. While the Agencies may possess the authority to lessen the burden of compliance with the regulatory mandates of the ACA by revising regulations, issuing enforcement relief or other certain other actions, these powers do not extend to blocking the authority of participants and beneficiaries to bring suit to enforce the provision of the ACA that the ACA added to ERISA through private benefit denial or breach of fiduciary duty lawsuits brought under ERISA.
In the case of insured health plans, sponsors, insurers and administrators also will need to consider whether their ability to take advantage of the federal relieve available is blocked or restricted by state insurance statutes, regulations or other administrative requirements. The likelihood of state statutory or regulatory restrictions on insured arrangements is particularly likely because of the heavy regulation of these products by states including the widespread incorporation of ACA mandates into state insurance laws and regulations in response to the Market Reform provisions of the ACA.
Even if these federal requirements are met to qualify for, adopt and implement any federally issued regulatory relief, employer and other plan sponsors, insurers, fiduciaries and administrators also should plan for and be prepared to run the necessary traps to properly amend their plan document, summary plan description and other plan notifications, administrative services agreements, stop loss or other insurance contracts and other vendor agreements to implement their desired changes. Beyond knowing what has to be done to adopt and communicate the desired changes, employer and other sponsors and fiduciaries, their consultants, brokers and advisors need to consider the requirements and consequences that the planned changes might have under applicable plan documents and vendor agreements to avoid unanticipated costs or liabilities as well as what actions are needed to ensure that ERISA’s prudence and other fiduciary requirements are met.
Until these and other required actions are completed by the Agencies and the applicable plan sponsors, fiduciaries and other parties, employers and other plan sponsors, their management, their health plans, health plan fiduciaries, administrators and insurers remain legally obligated to continue to comply with the ACA as presently implemented under the existing regulations and judicial and administrative rulings.
Responsible parties should begin preparing to take advantage of the anticipated legislative and regulatory relief both by both carefully monitoring statutory and regulatory health plan developments and positioning themselves to act quickly when relief comes by evaluating their existing heath plan documents, contracts, communications and systems to verify existing compliance and determine requirements for implementing any planned changes, opening up discussion vendors about these possibilities and taking other steps to position themselves to act knowledgeably and efficiently to take advantage of new opportunities if and when they emerge and are warranted.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with health industry and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on ACA-ERISA Lawsuit Risks Likely To Continue Until Congress Acts Despite Trump Executive Order For Agencies To Issue Relief |
Comments Off on ACA-ERISA Lawsuit Risks Likely To Continue Until Congress Acts Despite Trump Executive Order For Agencies To Issue Relief |  105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, COBRA, COBRA Subsidy, compliance, Consumer Protection, Contraception, Corporate Compliance, corporate governance, directors, EBSA, employee, Employee Benefits, Employer, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, fiduciary duty, Fiduciary Responsibility, FLSA, FMLA, Health Care Reform, health reform, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, King V. Burwell, Management, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Physician, Plan Admistrator, Prescription Drugs, preventive care, Provider, SBC, Uncategorized | Tagged: ACA, Executive Order, Health Care, Health Care Reform, Health Care Reimbursement, Health Insurance, Health Plans, health policy, Minimizing the Economic Burden of the Patient Protection and Affordable Act Act Pending Repeal, Obamacare, Patient Protection and Affordable Care Act |
105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims, Claims Administration, COBRA, COBRA Subsidy, compliance, Consumer Protection, Contraception, Corporate Compliance, corporate governance, directors, EBSA, employee, Employee Benefits, Employer, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, fiduciary duty, Fiduciary Responsibility, FLSA, FMLA, Health Care Reform, health reform, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, King V. Burwell, Management, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Physician, Plan Admistrator, Prescription Drugs, preventive care, Provider, SBC, Uncategorized | Tagged: ACA, Executive Order, Health Care, Health Care Reform, Health Care Reimbursement, Health Insurance, Health Plans, health policy, Minimizing the Economic Burden of the Patient Protection and Affordable Act Act Pending Repeal, Obamacare, Patient Protection and Affordable Care Act |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
January 23, 2017
Trump Executive Order Promises But Gives No ACA Health Plan Relief Until Agencies Act
Employer and other health plan sponsors, insurers, plan members and their family, health care providers and others struggling to cope with the costs and burdens of complying with the Patient Protection and Affordable Care Act (ACA) health care reforms are celebrating the promise of impending relief from ACA mandates held out by newly inagurated President Donald Trump January 20, 2017 Executive Order on “Minimizing the Economic Burden of the Patient Protection and Affordable Care Act Pending Repeal” (Executive Order).
In addition to affirming President Trump’s commitment to seek the prompt repeal of the ACA, the Executive Order seeks to mitigate the burden of the ACA pending Congressional repeal by ordering the Departments Health and Human Services (HHS), Labor (DOL), Treasury (Treasury) and other agencies with ACA authority (Agencies) to exercise all available authority and discretion to the “maximum extent permitted by law”:
- To waive, defer, grant exemptions from, or delay the implementation of any provision or requirement of the ACA that would impose a “cost, fee, tax, penalty, or regulatory burden on individuals, families, healthcare providers, health insurers, patients, recipients of healthcare services, purchasers of health insurance, or makers of medical devices, products, or medications.”
- To provide greater flexibility to States and cooperate with them in implementing healthcare programs and to waive, defer, grant exemptions from, or delay the implementation of any provision or requirement of the Act that would impose a fiscal burden on any State;
- For departments and agencies with responsibilities relating to healthcare or health insurance to encourage the development of a free and open market in interstate commerce for the offering of healthcare services and health insurance, with the goal of achieving and preserving maximum options for patients and consumers.
While employer and other health plan sponsors and others struggling to cope with the costs and mandates of ACA unquestionably welcome the promise of relief offered by the Executive Order, it is critical that those looking forward to enjoying this promised relief not jump the gun or overestimate the scope of the relief. Because the Executive Order is not self-executing, the Executive Order provides no legally enforceable relief from applicable ACA compliance obligations unless and until the applicable Agency or Congress adopts that relief consistent with law. While applicable Agencies are expected to act as quickly as possible to comply with President Trump’s orders, various statutory and procedural requirements almost certainly will limit both the relief granted and the speed with which the Agencies can grant the relief.
First, because the Executive Order is not self-executing, it doesn’t actually provide any relief for anyone; rather it just creates the expectation that the Agencies will grant some relief in the future. Those anticipating relief should expect that even regulatory relief will take time since the Agencies by law as well as the terms of the Executive Order will be required to comply with the often time consuming and cumbersome requirements of the Administrative Procedure Act and other applicable statutes in considering and issuing regulatory revisions and relief, including any applicable requirements for submission and approval by the Office of Management and Budget. The often added need for interagency collaboration and negotiation created by the ACA’s grant of multijurisdictional authority over many of its provisions historically has made negotiating these requirements more complicated and time consuming.
Second, relief will not be available for certain exposures because statutory limits on the jurisdiction and authority of the Agencies under the ACA will limit the scope of the relief that an Agency can grant. The Agencies generally do not have the authority to waive certain provisions of the ACA which are not within the discretion of the Agencies, such as the right of participants and beneficiaries in employer or union-sponsored health plan to sue to enforce ACA health plan mandates through a benefits or breach of fiduciary action brought under the Employee Retirement Income Security Act. Likewise, Agencies also will be restricted in their ability to waive penalties or requirements where the statutory mandate is drafted in a manner that denies the Agency discretionary authority to offer that relief.
Third, health plans, their sponsors, insurers, fiduciaries and administrators should anticipate that they may need to take certain action in response to any issued relief before they can take advantage of the relief allowed such as adopting health plan amendments, issuing notices to participants or beneficiaries, making elections or a combination of these actions.
In the case of insured health plans, sponsors, insurers and administrators also will need to consider whether their ability to take advantage of the federal relieve available is blocked or restricted by state insurance statutes, regulations or other administrative requirements. The likelihood of state statutory or regulatory restrictions on insured arrangements is particularly likely because of the heavy regulation of these products by states including the widespread incorporation of ACA mandates into state insurance laws and regulations in response to the Market Reform provisions of the ACA.
Even if these federal requirements are met to qualify for, adopt and implement any federally issued regulatory relief, employer and other plan sponsors, insurers, fiduciaries and administrators also should plan for and be prepared to run the necessary traps to properly amend their plan document, summary plan description and other plan notifications, administrative services agreements, stop loss or other insurance contracts and other vendor agreements to implement their desired changes. Beyond knowing what has to be done to adopt and communicate the desired changes, employer and other sponsors and fiduciaries, their consultants, brokers and advisors need to consider the requirements and consequences that the planned changes might have under applicable plan documents and vendor agreements to avoid unanticipated costs or liabilities as well as what actions are needed to ensure that ERISA’s prudence and other fiduciary requirements are met.
Until these and other required actions are completed by the Agencies and the applicable plan sponsors, fiduciaries and other parties, employers and other plan sponsors, their management, their health plans, health plan fiduciaries, administrators and insurers remain legally obligated to continue to comply with the ACA as presently implemented under the existing regulations and judicial and administrative rulings. While preparing for future changes, health plans, their sponsors, fiduciaries, administrators and insurers also should act to manage their prior and existing liabilities arising out of acts or omissions occurring before Congress or the regulators revise and ease the rules.
While health plans, their sponsors, fiduciaries, administrators and insurers remain legally responsible to comply with existing rules until changed by the regulators or Congress, they still have much to do to get ready for the changes that are coming while acting to manage their health plan costs and liabilities in the meantime. Whether or not the Trump Administration in the future provides relief from Form 8928 self-reporting and excise tax self- assessment penalties for violation of 40 federal group health plans, group health plans and their fiduciaries almost certainly will remain exposed to ERISA lawsuits for violation of ACA or other federal group health plan mandates. In addition, until revoked or revised, employers and health plans remain subject to and risk liability for failing to provide ACA-required tax forms, notices, benefits, coverage, rights or other compliance.
Responsible parties should begin preparing to take advantage of the anticipated legislative and regulatory relief both by both carefully monitoring statutory and regulatory health plan developments and positioning themselves to act quickly when relief comes by evaluating their existing heath plan documents, contracts, communications and systems to verify existing compliance and determine requirements for implementing any planned changes, opening up discussion vendors about these possibilities and taking other steps to position themselves to act knowledgeably and efficiently to take advantage of new opportunities if and when they emerge and are warranted.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with health industry and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein
©2017 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Employers, Plans, Don’t Jump The Gun On ACA Relief |
Comments Off on Employers, Plans, Don’t Jump The Gun On ACA Relief |  105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims Administration, compensation, compliance, Consumer Protection, Contraception, Corporate Compliance, corporate governance, defined contribution plan, Discrimination, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employment, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, fiduciary duty, FLSA, FMLA, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Prescription Drugs, SBC, Uncategorized | Tagged: ACA, Health Care Reform, Health Insurance, Health Plans, Insurance, Insurer, Obama Care, Patient Protection and Affordable Care Act, Plan Sponsors, Trump |
105(h), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Appeals, board of directors, Brokers, Cafeteria Plans, Claims Administration, compensation, compliance, Consumer Protection, Contraception, Corporate Compliance, corporate governance, defined contribution plan, Discrimination, Drug & Alcohol, EBSA, Employee Benefits, Employer, Employment, ERISA, Excepted Benefits, exchange, Excise Tax, Excise Taxes, fiduciary duty, FLSA, FMLA, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Revenue Code, IRC, Mental Health, Mental Health Parity, MEWA, Obamacare, Patient Empowerment, Patient Protection & Affordable Care Act, Prescription Drugs, SBC, Uncategorized | Tagged: ACA, Health Care Reform, Health Insurance, Health Plans, Insurance, Insurer, Obama Care, Patient Protection and Affordable Care Act, Plan Sponsors, Trump |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 21, 2016
Employee benefit plans and tax-exempt organizations facing Internal Revenue Service (IRS) audits or investigations after April, 2016, their leaders and advisors should prepare for some changes in the practices IRS agents will use to issue and enforce document requests (IDRs) after March 31.
The IRS Tax Exempt and Government Entities Division (TEGE) just issued updated internal guidance (Guidance) governing the procedures its agents will use to gather information for employee benefit plan and exempt organization examinations including information requests made in connection with:
- Employee Benefit Form 5500 Examination Procedures
- Exempt Organizations Pre-Audit Procedures
- On-Site Examinations
- Tax Exempt Bonds Examinations
- Indian Tribal Government Examinations and
- Federal, State and Local Governments (FSLG) Examinations
The new Guidance follows other recent announcements of changes of IRS employee plan or exempt organization procedures such as recently announced changes in IRS employee plan correction procedures. See, e.g., IRS Qualified Plan Correction Procedures Changing 1/1/17.
The new procedures defined in the Guidance apply more broadly and take effect April 1, 2017. The Guidance also requires that TEGE update the following IRMs to specifically reflect the new procedures within the next two years:
- IRM 4.71.1, Overview of Form 5500 Examination Procedures;
- IRM 4.75.10, Exempt Organizations Pre-Audit Procedures;
- IRM 4.75.11, On-Site Examination Guidelines;
- IRM 4.81.5, Tax Exempt Bonds Examination Program Procedures – Conducting the Examination;
- IRM 4.86.5, Conducting Indian Tribal Government Examinations; and
- IRM 4.90.9, Federal, State and Local Governments (FSLG) – Procedures, Workpapers and Report Writing.
Among other things, the new Guidance will require “active involvement” by managers of IRS examiners’ early in the process. The Guidance also calls for:
- Taxpayers to be involved in the IDR process.
- Examiners to discuss the issue being examined and the information needed with the taxpayer prior to issuing an IDR.
- Examiners to ensure that the IDR clearly states the issue and the relevant information they are requesting.
- If the taxpayer does not timely provide the information requested in the IDR by the agreed upon date, including extensions, examiners to issue a delinquency notice.
- If the taxpayer fails to respond to the delinquency notice or provides an incomplete response, for the examiner to issue a pre-summons notice to advise the taxpayer that the IRS will issue a summons unless the missing items are fully provided.
- For a summons to be issued if the taxpayer fails to provide a complete response to the pre-summons letter by its response due date.
According to TEGE the new procedures set forth in the Guidance are designed to “ensure” that IRS Counsel is prepared to enforce IDRs through the issuance of a summons when necessary while also reinforcing the IRS’ commitment to the respect of taxpayer rights under the Taxpayer Bill of Rights. TEGE says the updated procedures established in the Guidance will promote these goals by:
- Providing for open and meaningful communication between the IRS and taxpayers;
- Reducing taxpayer burdens
- Providing for consistent treatment of taxpayers;
- Allowing the IRS to secure more complete and timely responses to IDRs;
- Providing consistent timelines for IRS agents to review IDR responses; and
- Promoting timely issue resolution.
While it remains to be seen exactly how well the new procedures will promote these goals in operation, leaders, sponsors, administrators and tax advisors to employee benefit plans and exempt organizations tagged for audits after the Guidelines take effect will want to ensure that they review and fully understand the new procedures as soon as possible after receiving notice of the audit.
A clear understanding of the procedures can help the entities and their representatives to take advantage of all available options for mitigating exposures and liability from the audit as well as to avoid unfortunate missteps that could result in forfeiture of otherwise available tax-related rights and options or otherwise increase the tax and other associated risks and liabilities of the entities or others associated with them arising from the audit.
Along with responding to these tax-related risks, leaders and advisors of employee benefit plan and exempt organizations also need to keep in mind the often substantial non-tax related risks that may arise concurrently or evolve from a TEGE or other tax-related audit or investigation. The often substantial tax and non-tax exposures typically makes it desirable if not necessary to involve experienced legal counsel in the process as soon as possible.
To help respond to the audit and manage its tax and non-tax related risks and, leaders responsible for these entities generally not only will want to seek legal advice within the scope of attorney-client privilege from legal counsel immediately after receiving an IDR or other notice of an audit or investigation, as well as consider periodically consulting experienced legal counsel for assistance in conducting pre-audit assessment of compliance and other compliance and risk management planning.
Early involvement of legal counsel generally is necessary both to understand and manage both the tax and non-tax exposures associated with the audit, as well as to preserve and utilize the potential benefits of attorney-client privilege and other evidentiary privileges that could help to mitigate both the tax and non-tax related risks. While federal tax rules afford some evidentiary privileges to certain accounting professionals when providing tax representation or advice, the protective scope of such privileges generally are more limited than attorney-client privilege and work product evidentiary privileges and typically do not apply to non-tax matters. As a result, most entities and their leaders will want to consider involvement of legal counsel to maximize privilege protections and non-tax related exposures even if the parties plan for a qualified tax professional or other consultant to play a significant role in assisting them to prepare for and respond to the audit.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,” “Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with health industry and other businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association; Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Gulf Coast TEGE Council Exempt Organization Coordinator; a founding Board Member and past President of the Alliance for Healthcare Excellence; former board member and Vice President of the Managed Care Association; past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; a member and advisor to the National Physicians’ Council for Healthcare Policy; current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee; current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section; Past Chair of the ABA Health Law Section Managed Care & Insurance Section; a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group; immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council; past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former member of the Board of Directors, Treasurer, Member and Continuing Education Chair of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at SolutionsLawPress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please provide your current contact information and preferences including your preferred e-mail by creating or updating your profile here.
NOTICE: These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein
©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on IRS Changing Employee Plans & Exempt Organization Audit Procedures |
Comments Off on IRS Changing Employee Plans & Exempt Organization Audit Procedures |  105(h), 401(k), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, COBRA, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health reform, HR, Human Resources, Identity Theft, Income Tax, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Pay, Payroll Tax, pension plan, Plan Admistrator, Tax, Tax Credit, Tax Qualification, Uncategorized |
105(h), 401(k), 4980D, 4980H, 6039D, ACA, Affordable Care Act, Attorney-Client Privilege, board of directors, Brokers, Cafeteria Plans, church plan, COBRA, compensation, compliance, Corporate Compliance, corporate governance, defined benefit plan, Defined Benefit Plans, defined contribution plan, Defined Contribution Plans, directors, Discrimination, EBSA, employee, Employee Benefits, Employer, Employers, Employment, Employment Tax, ERISA, ESOP, Excise Tax, Excise Taxes, Executive Compensation, Exempt, Form 5500, health reform, HR, Human Resources, Identity Theft, Income Tax, Internal Controls, Internal Investigations, Internal Revenue Code, IRC, Pay, Payroll Tax, pension plan, Plan Admistrator, Tax, Tax Credit, Tax Qualification, Uncategorized |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
November 3, 2016
Restaurant employers beware! Restaurants are the target of a highly successful, U.S. Department of Labor Wage and Hour Division (WHD) restaurant enforcement and compliance initiative that WHD already has used to nail a multitude of restaurants across the country for “widespread violations” of Fair Labor Standards Act (FLSA) minimum wage, overtime, child labor and other wage and hour laws (WH Law).
Having reportedly found WH Law violations in “nearly every one” of the WH Law investigations conducted against restaurant employers during 2016 and recovered millions of dollars of back pay and penalties from restaurants caught through investigations conducted under its WHD Restaurant Enforcement Initiative, WHD Administrator Dr. David Weil recently confirmed WHD plans to expand the restaurant employers targeted for investigation and other efforts to punish and correct WH Law violations under the Restaurant Enforcement Initiative through 2017 in an October 5, 2016 WHD News Release: Significant Violations In The Austin Restaurant Industry Raise Concerns For Us Labor Department Officials (News Release).
The News Release quotes Administrator Weil as stating:
The current level of noncompliance found in these investigations is not acceptable …WHD will continue to use every tool we have available to combat this issue. This includes vigorous enforcement as well as outreach to employer associations and worker advocates to ensure that Austin restaurant workers receive a fair day’s pay for a fair day’s work.
Given the substantial back pay, interest, civil or in the case of willful violations, criminal penalties, costs of defense and prosecution and other sanctions that restaurant employers, their owners and management can face if their restaurant is caught violating FLSA or other WH Laws, restaurants and their leaders should arrange for a comprehensive review within the scope of attorney-client privilege of the adequacy and defensibility of their existing policies, practices and documentation for classifying, assigning duties, tracking regular and overtime hours, paying workers and other WH Law compliance responsibilities and opportunities to mitigate risks and liabilities from WH Law claims and investigations.
Many Restaurants Already Nailed Through Restaurant Enforcement Initiative
Even before the planned 2017 expansion of its Restaurant Enforcement Initiative, WHD’s enforcement record shows WHD’s efforts to find and punish restaurants that violate WH Laws are highly successful. Restaurant employers overwhelmingly are the employers targeted by WHD in the vast majority of the WH Law settlements and prosecutions announced in WHD News Releases published over the past two years, including aggregate back pay and penalty awards of more than $11.4 million recovered through the following 31 actions announced by WHD between January 1, 2016 and October 31, 2016:
- US Labor Department Investigation Finds Thundercloud Subs Owes Nearly $128K In Back Wages, Damages To Austin Restaurant Workers (October 20, 2016);
- US Labor Department Announces Hotline To Offer Updates To Capitol Hill Cafeteria Workers Owed Back Wage Payments (October 20, 2016);
- US Labor Department Recovers More Than $570K In Back Wages, Damages For 55 Workers At Johnny Rockets Restaurants In Washington Metro Area (October 11, 2016);
- Portland, Texas, Restaurant Settles Worker Retaliation Allegation After US Labor Department Finds Nine Employees Owed $25K In Back Wages (October 06, 2016);
- Providence Restaurant, Owner To Pay $567K In Back Wages, Damages To 104 Employees Denied Minimum Wage, Overtime Pay (September 23, 2016);
- US Labor Department Investigation Finds Capitol Hill Cafeteria Workers Illegally Denied More Than $1M In Wages By Federal Food Service Contractors (July 26, 2016);
- El Azteca Restaurant Group To Pay $700K In Back Wages, Damages To 129 Workers At Four Wisconsin Eateries (July 26, 2016);
- Historic Oklahoma City Restaurant Pays Workers $52K In Back Wages, Damages After Labor Department Investigation (June 22, 2016);
- Kissimmee, Florida, Restaurant To Pay Nearly $41KIn Back Wages To 15 Employees After US Department Of Labor Investigation (June 15, 2016);
- Court Orders Buffet Restaurant, Owners To Pay $128K In Back Wages, Penalties To Resolve Allegations Of Federal Minimum Wage, Overtime Violations (June 09, 2016);
- Grand Rapids Restaurant, Owners Agree With Court Order To Comply With Federal Record-Keeping Rules After Department’s Wage And Hour Investigation (May 31, 2016);
- Court Judgment Orders Four Phoenix-Area Federico’s Mexican Food Restaurants To Pay Workers $202KIn Overtime Back Wages, Damages (May 24, 2016);
- US Labor Department Investigation Finds Child Labor, Minimum Wage And Other Violations At Street’s Seafood Restaurant (May 17, 2016);
- US Labor Department Initiative Finds 14 Lawrence Restaurants Owe More Than $112K In Back Wages To 130 Workers (May 17, 2016);
- US Labor Department Obtains Order To Stop Arlington Restaurant Owners From Intimidating Workers Who Cooperate With Federal Investigators (May 16, 2016);
- Charleston Restaurants’ Minimum Wage, Overtime Violations Result In Nearly $217K In Back Wages For 26 Employees (May 9, 2016);
- Las Investigaciones Dieron Como Resultado Casi $1.2 Millones En Salarios Retroactivos Y Daños Y Perjuicios Para Más De 100 Trabajadores En 13 Restaurantes En El Área De Charleston and Investigations Result In Nearly $1.2M In Back Wages, Damages For More Than 100 Workers At 13 Charleston Area Restaurants (April 19, 2016);
- Clairmont Diner Will Pay $213K In Back Wages, Damages And Penalties After Federal Wage And Hour Investigation (March 30, 2016);
- Tampico Restaurants Agree To Pay $190K In Back Wages To 67 Workers (March 26, 2016);
- S. Labor Department Lawsuit Seeks Back Wages And Damages For Austintown, Ohio Restaurant Workers (March 16, 2016);
- Popular Cajun Food Enterprise Will Pay More Than $138K In Back Wages, Penalties Following U.S. Labor Department Investigation (March 07, 2016);
- US Labor Department Initiative Finds Ames Restaurants Owe Nearly $100K In Back Wages To More Than 150 Workers (March 02, 2016);
- S. Labor Department Sues To Recover Unpaid Minimum Wage, Overtime Plus Additional Damages For Akron Restaurant Workers (February 25, 2016);
- Paying To Work? Sophia’s House Of Pancakes Resolves Allegations Servers Made To Pay $2 Per Hour To Work At Restaurants (February 16, 2016)($245K);
- Two Hawaii Restaurants Found In Violation Of Overtime Pay Requirements (February 10, 2016)($81,294);
- Labor Department Launches West Coast Sweep To Investigate Pay Practices At Fast Food Establishments To Ensure Fairness, Compliance (February 4, 2016);
- Sushi And Ramen Restaurants Pay $621K In Back Wages, Damages And Penalties After US Labor Department Investigation (January 25, 2016)
- Federal Judge Overturns Jury Verdict, Orders El Tequila Restaurants And Owner Carlos Aguirre To Pay $2.1 Million In Back Wages And Damages To Workers (January 14, 2016);
- Taqueria La Herradura En Pharr, Texas, Paga Más De $33 Mil En Concepto De Salarios Retroactivos Y Daños Al Personal De La Cocina Después De Una Investigación Del Departamento De Trabajo De Ee.Uu.(January 12, 2016);
- Investigations At 10 North Carolina Restaurants Find More Than $510K In Back Wages Owed To 125 Workers (January 12, 2016);
- Restaurant Enforcement Initiative Finds More Than $2.27M In Back Wages, Damages Owed To More Than 3,000 Georgia Workers (January 05, 2016).
Enforcement Actions Highlight Common Restaurant WH Law Compliance Concerns
Restaurant employers, like employers in most other industries, are subject to a host of minimum wage, overtime and other requirements including the FLSA requirement that covered, nonexempt employees earn at least the federal minimum wage of $7.25 per hour for all regular hours worked, plus time and one-half their regular rates, including commissions, bonuses and incentive pay, for hours worked beyond 40 per week. Employers also are required to maintain accurate time and payroll records and must comply with child labor, anti-retaliation and other WH Law requirements.
The News Release identified some of the common violations WHD uncovered in these investigations included employers:
- Requiring employees to work exclusively for tips, with no regard to minimum-wage standards;
- Making illegal deductions from workers’ wages for walkouts, breakages, credit card transaction fees and cash register shortages, which reduce wages below the required minimum wage;
- Paying straight-time wages for overtime hours worked.
- Calculating overtime incorrectly for servers based on their $2.13 per hour base rates before tips, instead of the federal minimum wage of $7.25 per hour.
- Failing to pay proper overtime for salaried non-exempt cooks or other workers;
- Creating illegal tip pools involving kitchen staff;
- Failing to maintain accurate and thorough records of employees’ wages and work hours.
- Committing significant child labor violations, such as allowing minors to operate and clean hazardous equipment, including dough mixers and meat slicers.
Use Care To Verify Tipped Employees Paid Properly
Based on the reported violations, restaurants employing tipped employees generally will want to carefully review their policies, practices and records regarding their payment of tipped employees. Among other things, these common violations reflect a widespread misunderstanding or misapplication of special rules for calculating the minimum hourly wage that a restaurant must pay an employee that qualifies as a tipped employee. While special FLSA rules for tipped employees may permit a restaurant to claim tips (not in excess of $5.12 per hour) actually received and retained by a “tipped employee,” not all workers that receive tips are necessarily covered by this special rule. For purposes of this rule, the definition of “tipped employee” only applies to an employee who customarily and regularly receives more than $30 per month in tips.
Also, contrary to popular perception, the FLSA as construed by the WHD does not set the minimum wage for tipped employees at $2.13 per hour. On the contrary, the FLSA requirement that non-exempt workers be paid at least the minimum wage of $7.25 per hour for each regular hour worked also applies to tipped employees. When applicable, the special rule for tipped employees merely only allows an employer to claim the amount of the tips that the restaurant can prove the tipped employee actually received and retained (not in excess of $5.13 per hour) as a credit against the minimum wage of $7.25 per hour the FLSA otherwise would require the employer to pay the tipped employee. Only tips actually received by the employee may be counted in determining whether the employee is a tipped employee and in applying the tip credit. If a tipped employee earns less than $5.13 per hour in tips, the restaurant must be able to demonstrate that the combined total of the tips retained by the employee and the hourly wage otherwise paid to the tipped employee by the restaurant equaled at least the minimum wage of $7.25 per hour.
Furthermore, restaurant or other employers claiming a tip credit must keep in mind that the FLSA generally provides that tips are the property of the employee. The FLSA generally prohibits an employer from using an employee’s tips for any reason other than as a credit against its minimum wage obligation to the employee (“tip credit”) or in furtherance of a valid tip pool.
Also, whether for purposes of applying the tip credit rules or other applicable requirements of the FLSA and other wage and hour laws, restaurant employers must create and retain appropriate records and other documentation regarding worker age, classification, hours worked, tips and other compensation paid and other evidence necessary to defend their actions with respect to tipped or other employees under the FLSA and other WH Law rules. Beyond accurately and reliably capturing all of the documentation required to show proper payment in accordance with the FLSA, restaurants also should use care to appropriately document leave, discipline and other related activities as necessary to show compliance with anti-retaliation, equal pay, family and medical leave, and other mandates, as applicable. Since state law also may impose additional minimum leave, break time or other requirements, restaurants also generally will want to review their policies, practices and records to verify their ability to defend their actions under those rules as well.
Child Labor Rules Require Special Care When Employing Minors
While hiring workers under the age of 18 (minors) can help a restaurant fulfill its staffing needs while providing young workers valuable first time or other work experience, restaurants that hire minors must understand and properly comply with any restrictions on the duties, work hours or other requirements for employment of the minor imposed by federal or state child labor laws.
As a starting point, the legal requirements for employing minors generally greater, not less, than those applicable to the employment of an adult in the same position. Employers employing workers who are less than 18 years of age (minors) should not assume that the employer can pay the minor less than minimum wage or skip complying with other legal requirements that normally apply to the employment of an adult in that position by employing the minor in an “internship” or other special capacity. The same federal and state minimum wage, overtime, safety and health and nondiscrimination rules that generally apply to the employment of an adult generally will apply to its employment of a worker who is a minor.
Beyond complying with the rules for employment of adults, restaurants employing minors also must ensure that they fully comply with all applicable requirements for the employment of minors imposed under the FLSA child labor rules and applicable state law enacted to ensure that when young people work, the work is safe and does not jeopardize their health, well-being or educational opportunities. Depending on the age of the minor, the FLSA or state child labor rules may necessitate that a restaurant tailor the duties and hours of work of an employee who is a minor to avoid the substantial liability that can result when an employer violates one of these child labor rules.
The FLSA child labor rules, for instance, impose various special requirements for the employment of youth 14 to 17 years old. See here. As a starting point, the FLSA child labor rules prohibit the any worker less than 18 years of age from operating or cleaning dough mixers, meat slicers or other hazardous equipment. Depending on the age of the minor worker, the FLSA child labor rules or state child labor laws also may impose other restrictions on the duties that the restaurant can assign or allow the minor to perform. Restaurants hiring any worker that is a minor must evaluate the duties identified as hazardous “occupations” that the FLSA child labor rules prohibit a minor of that age to perform here as an “occupation” and take the necessary steps to ensure the minor is not assigned and does not perform any of those prohibited activities in the course of his employment.
In addition to ensuring that minors don’t perform prohibited duties, restaurants employing minors also comply with all applicable restrictions on the hours that the minor is permitted to work based on the age of the minor worker. For instance, the FLSA and state child labor rules typically prohibit scheduling a minor less than 16 years of age to work during school hours and restrict the hours outside school hours the minor can work based on his age. Additional restrictions on the types of jobs and hours 14- and 15-year-olds may work also may apply.
Compliance with the FLSA child labor rules is critically important for any restaurant or other employer that employs a minor, particularly since the penalties for violation of these requirements were substantially increased in 2010, as Streets Seafood Restaurant learned earlier this year.
According to a WHD News Release, Street’s Seafood Restaurant paid $14,288 in minimum wage and overtime back wages and an equal amount in liquidated damages totaling $28,577 to eight employees, and also was assessed a civil money penalty of $14,125 for FLSA child labor violations committed in the course of its employment of four minors ages 15 to 17. Specifically, investigators found Street’s Seafood Restaurant:
WHD’s announcement of the settlement resolving these child labor laws quotes Kenneth Stripling, director of the division’s Birmingham District Office as stating:
Employing young people provides valuable experience, but that experience must never come at the expense of their safety …Additionally, employers have an obligation to pay employees what they have legally earned. All workers deserve a fair day’s pay for a fair day’s work. Unfortunately, Street’s Seafood violated not only child labor laws, but has also shorted workers’ pay. The resolution of this case sends a strong message that we will not tolerate either of those behaviors.
Restaurants Must Act To Minimize Risks
Beyond WHD’s direct enforcement actions, WHD also is seeking to encourage private enforcement of WH Law violations by conducting an aggressive outreach to employees, their union and private plaintiff representatives, states and others. Successful plaintiffs in private actions typically recover actual back pay, double damage penalties plus attorneys’ fees and costs. The availability of these often lucrative private damages makes FLSA and other WH Law claims highly popular to disgruntled or terminated workers and their lawyers. When contemplating options to settle claims WH Law claims made by a worker, employers need to keep in mind that WHD takes the position that settlements with workers do not bar the WHD from taking action unless the WHD joins in the settlement and in fact, past settlements may provide evidence of knowingness or willfulness by the employer in the event of a WHD prosecution. The substantial private recoveries coupled with these and other WHD enforcement and other compliance actions mean bad news for restaurant employers that fail to manage their FLSA and other WH Law compliance. Restaurant employers should act within the scope of attorney-client privilege to review and verify their compliance and consult with legal counsel about other options to minimize their risk and streamline and strengthen their ability to respond to and defend against audits, investigations and litigation.
Beyond verifying the appropriateness of their timekeeping and compensation activities and documentation, restaurants and staffing or management organizations working with them also should use care to mitigate exposures that often arise from missteps or overly aggressive conduct by others providing or receiving management services or staffing services. All parties to these arrangements and their management should keep in mind that both parties participating in such arrangements bear significant risk if responsibilities are not properly performed. Both service and staffing providers and restaurants using their services should insist on carefully crafted commitments from the other party to properly classify, track hours, calculate and pay workers, keep records, and otherwise comply with WH Laws and other legal requirements. Parties to these arrangements both generally also will want to insist that these contractual reassurances are backed up with meaningful audit and indemnification rights and carefully monitor the actions of service providers rendering these services.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,”“Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real-time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares shared her thought leadership, experience and advocacy on these and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association, Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Board Compliance Chair and Board member of the National Kidney Foundation of North Texas, current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment, employee benefits, compensation, and other regulatory and operational risk management. Examples of her many highly regarded publications on these matters include the “Texas Payday Law” Chapter of Texas Employment Law, as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clients on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at http://www.solutionslawpress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.
©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on DOL Aggressively Targeting Restaurants For Wage & Hour & Child Labor Law Violations |
Comments Off on DOL Aggressively Targeting Restaurants For Wage & Hour & Child Labor Law Violations |  Attorney-Client Privilege, board of directors, Civil Monetary Penalties, Corporate Compliance, corporate governance, employee, Employer, Employers, Employment, Employment Discrimination, Employment Tax, Fair Labor Standards Act, family leave, FLSA, Government Contractors, Hiring, Hospitality, HR, Human Resources, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Management, Non-Exempt, Pay, Risk Management, Salaried, Uncategorized | Tagged: Child Labor, Employer, Exempt, FLSA, hospitality, Minimum Wage, Non-Exempt, Overtime, pay, Restaurant, wage and hour |
Attorney-Client Privilege, board of directors, Civil Monetary Penalties, Corporate Compliance, corporate governance, employee, Employer, Employers, Employment, Employment Discrimination, Employment Tax, Fair Labor Standards Act, family leave, FLSA, Government Contractors, Hiring, Hospitality, HR, Human Resources, Internal Controls, Internal Investigations, Labor Management Relations, Leave, Management, Non-Exempt, Pay, Risk Management, Salaried, Uncategorized | Tagged: Child Labor, Employer, Exempt, FLSA, hospitality, Minimum Wage, Non-Exempt, Overtime, pay, Restaurant, wage and hour |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 27, 2016
Compliance with the Privacy and Security Rules of the Health Insurance Portability & Accountability Act (HIPAA) is a living process that requires employer and other health plans, health insurers, health care providers and healthcare clearinghouses to recurrently reevaluate their HIPAA enterprise risk and timely act to mitigate security threats to electronic (ePHI) and other protected health information and other HIPAA compliance concerns on an ongoing basis. That’s the clear take away applicable to all HIPAA-Covered Entities and business associates from the St. Joseph Health Resolution Agreement and Corrective Action Plan (SJH Settlement) and the Oregon Health & Science University Resolution Agreement and Corrective Action Plan (OHSU Settlement) announced by the Department of Health & Human Services Office of Civil Rights (OCR) in the past 30 days. Health plans, their sponsors, fiduciaries and vendors, health care providers and health care clearinghouses should carefully heed this message and in response take documented steps to ensure
- Their existing policies, practices and procedures properly are updated in response to changing guidance and events;
- They in place the current, comprehensive enterprise risk assessment along with a mitigation plan documenting actions taken to address these risks;
- Ensure that the organization has and is administering appropriate, documented processes and procedures to ensure that the organization reassesses its enterprise risk assessment and compliance on a timely basis as warranted by changes or other events that could impact ePHI, regulatory developments or other events that might impact its compliance; and
- Have an appropriate, documented process for oversight by C-level management.
OHSU Charges & Settlement
The OHSU Settlement Agreement announced by OCR on September 23, 2016 requires OHSU to pay a $2.7 million settlement payment and adopt and implement a comprehensive three-year corrective action plan to address “widespread and diverse” HIPAA compliance problems OCR reports uncovering while investigating multiple HIPAA breach reports the large public academic health center and research university centered in Portland, Oregon.
OCR began investigating OHSU after the large public academic health center and research university centered in Portland, Oregon, submitted three HIPAA breach reports affecting thousands of individuals, including two reports involving unencrypted laptops and another large breach involving a stolen unencrypted thumb drive:
- On March 23, 2013, HHS received notification from OHSU regarding a breach of its unsecured electronic protected health information (“ePHI”) resulting from a stolen laptop computer;
- On July 28, 2013, HHS received notification from OHSU regarding a breach of its ePHI resulting from storing ePHI at an internet-based service provider without a business associate agreement; and.
These incidents each garnered significant local and national press coverage. OCR’s investigation uncovered evidence of widespread vulnerabilities within OHSU’s HIPAA compliance program, including the storage of the ePHI of more than 3,000 individuals on a cloud-based server without a business associate agreement. OCR found significant risk of harm to 1,361 of these individuals due to the sensitive nature of their diagnoses.
OCR’s investigation showed the reported breaches resulted from widespread, long-term, systematic and unresolved HIPAA violations by OHSU that OCR attributed to an inadequate commitment to and oversight of HIPAA compliance by OHSU C-level management which resulted in the failure by OHSU to appropriately monitor the adequacy of its ongoing compliance and to assess and address changes in its enterprise-wide risk and compliance obligations on an ongoing basis. OHSU performed risk analyses in 2003, 2005, 2006, 2008, 2010, and 2013, but OCR’s investigation found that these analyses did not cover all ePHI in OHSU’s enterprise, as required by the Security Rule. While the analyses identified vulnerabilities and risks to ePHI located in many areas of the organization, OHSU did not act in a timely manner to implement measures to address these documented risks and vulnerabilities to a reasonable and appropriate level. OHSU also lacked policies and procedures to prevent, detect, contain, and correct security violations and failed to implement a mechanism to encrypt and decrypt ePHI or an equivalent alternative measure for ePHI maintained on its workstations, despite having identified this lack of encryption as a risk.
OCR concluded that the reported breaches were the result of long-standing, systematic deficiences in OHSU’s processes and procedures for HIPAA compliance, including the following:
- While OHSU reportedly performed risk analyses in 2003, 2005, 2006, 2008, 2010, and 2013, OCR says its investigation found that these analyses did not cover all ePHI in OHSU’s enterprise, as required by the Security Rule;
- While the analyses identified vulnerabilities and risks to ePHI located in many areas of the organization, OHSU did not act in a timely manner to implement measures to address these documented risks and vulnerabilities to a reasonable and appropriate level;
- OHSU also lacked policies and procedures to prevent, detect, contain, and correct security violations and failed to implement a mechanism to encrypt and decrypt ePHI or an equivalent alternative measure for ePHI maintained on its workstations, despite having identified this lack of encryption as a risk;
- OHSU failed to comply with its duty under HIPAA to enter into a business associate agreement with a vendor before allowing a vendor business associate to store ePHI; and
- The absence of meaningful C-suite leadership oversight and commitment to HIPAA compliance.
Based on these investigations, OCR concluded that while OHSU initially adopted HIPAA Policies, the reported breaches were the result of a series of widespread and ongoing breaches of HIPAA resulted including the following:
- From January 5, 2011, until July 3, 2013, OHSU disclosed the ePHI of 3,044 individuals in violation of Privacy Rules §§160.103 and 164.502(a) when workforce members disclosed the ePHI to a third party internet-based service provider without obtaining a business associate agreement or other satisfactory assurance that the internet-based service provider would safeguard the ePHI;
- From January 5, 2011 until July 3, 2013 OHSU failed to obtain a business associate agreement from an internet-based service provider that was storing ePHI on its behalf as a business associate as required by 45 C.F.R. § 164.308(b);
- From January 5, 2011 until July 3, 2013 OHSU failed to implement policies and procedures to prevent, detect, contain, and correct security violations as required under Privacy Rule § 164.308(a)(1)(i);
- From July 12, 2010 to present, OHSU failed to implement a mechanism to encrypt and decrypt ePHI or an equivalent alternative measure for all ePHI maintained in OHSU’s enterprise as required by Privacy Rules §§ 164.312(a)(2)(iv) and 164.306(d)(3)); and
- From May 29, 2013 until July 3, 2013, OHSU failed to implement policies and procedures to address security incidents in violation of Privacy Rule § 164.308(a)(6)(i).
According to statements made by OCR Director Jocelyn Samuels in OCR’s announcement of the OHSU Settlement, the breaches should not have happened. “From well-publicized large scale breaches and findings in their own risk analyses, OHSU had every opportunity to address security management processes that were insufficient,” said OCR Director Jocelyn Samuels. OCR’s announcement also signals that OCR views inadequate commitment and oversight by OHSU’s senior management to have played a key role in the creation and perpetuation of the OHSU violations. It quotes OCR Director Jocelyn Samuels as stating, “This settlement underscores the importance of leadership engagement and why it is so critical for the C-suite to take HIPAA compliance seriously.”
OCR’s announcement of the OHSU Settlement emphasizes its determination that a lack of commitment and oversight by C-level management resulted in the failure by OHSU to periodically perform a comprehensive enterprise risk analysis and to reevaluate and update that analysis and its policies, practices, procedures and training as warranted by changing events and guidance.
To resolve the HIPAA charges, the OHSU Settlement requires OHSU to pay OCR $2,700,000 as well as take a long series of corrective actions detailed in the Corrective Action Plan incorporated into the Settlement Agreement. The requirements of the Corrective Action Plan both seek to address the specific weaknesses that lead to the breaches of unsecured ePHI reported by OHSU in its breach notifications as well as the broader deficiencies in OHSU’s overall HIPAA compliance practice by requiring among other things that OHSU:
- Conduct an accurate and thorough assessment of the potential risks and vulnerabilities to the confidentiality, integrity, and availability of ePHI at all OHSU facilities and on all systems, networks, and devices that create, receive, maintain, or transmit ePHI;.
- Develop and present to OCR for approval a comprehensive written risk management plan that explains OHSU’s strategy for implementing security measures sufficient to reduce the risks and vulnerabilities identified in the risk analysis to a reasonable and appropriate level based on OHSU’s circumstances as well as a comprehensive, enterprise-wide plan to implement effective oversight of OHSU workforce members to ensure their adherence to HIPAA Rules and OHSU’s internal privacy and security policies and procedures with specific timelines for their expected completion and compensating controls identified in the interim to safeguard OHSU’s ePHI;
- Implement and administer the written risk management plan and other safeguards as approved by OCR;
- Provide updates to OCR about OHSU’s implementation of required encryption including a Mobile Device Management (MDM) solution that ensures all OHSU- owned and personally-owned mobile devices (tablets, smart phones, and other mobile devices) that access ePHI on OHSU’s secure network are encrypted other than mobile devices for which OHSU has granted exceptions based on documented evidence of the implementation of alternative reasonable compensating controls to protect the ePHI on such devices;
- Report to OCR on OHSU’s efforts to a solution to enforce encryption of ePHI on OHSU-owned and personally- owned devices (laptops, desktops, and medical equipment) connecting to OHSU’s secure wired and wireless networks except for any devices for which OHSU has granted exceptions to the encryption requirement;
- Report to OCR about its implementation of policies that prohibit the transfer of data containing ePHI from OHSU-owned and personally-owned devices to unencrypted removable storage devices (USB drives and portable hard drives) and implementation of a technical solution that enforces the policies prohibiting transfers of this type when attached to the OHSU secure network, except for any removable storage devices for which OHSU has granted exceptions based on documented evidence of reasonable compensating controls that have been implemented to protect the ePHI on such devices;
- Send a communication to all members of the OHSU community describing its commitment to enterprise encryption;
- Prepare to the satisfaction of OCR security awareness training materials needed to implement its security management processing including specific privacy and security awareness related to a) use of internet-based information storage services; b) disclosures to third party entities that require a business associate agreement or other reasonable assurance in place to ensure that the business associate will safeguard the protected health information (PHI) and/or ePHI; c) regarding managers, effective oversight of workforce members’ uses and disclosures of PHI, including ePHI, to ensure the workforce members’ compliance with the Privacy and Security Rules and OHSU’s internal policies and procedures; d) security incident reporting; and e) password management;
- Initially train all workforce members with access to PHI and/or ePHI with 120 days of OCR’s approval of the training and thereafter ensure that new workforce members are trained with 15 days of hire and that all workforce members subsequently continue to receive training on an on-going basis;
- Review the security awareness training materials annually, and, where appropriate, update the training to reflect changes in Federal law or HHS guidance, any issues discovered during audits or reviews, and any other relevant developments;
- Management oversight and supervision of the implementation and administration of the corrective actions required by the Corrective Action Plan and HIPAA compliance; and
- Management reporting to OCR on its actions and compliance with the Corrective Action Plan.
SJH Settlement
Similarly, the SJH Settlement OCR announced on October 18, 2016 with St. Joseph Health (SJH) requires SJH to pay a $2.4 million plus settlement payment, conduct an enterprise-wide risk analysis and implement and administer a comprehensive correction plan to settle OCR charges that SJH violated HIPAA by allowing files containing ePHI of 31,800 individuals that SJH created for its participation in the Medicare meaningful use program to be publicly accessible on the internet from February 1, 2011, until February 13, 2012.
A nonprofit integrated Catholic health care delivery system sponsored by the St. Joseph Health Ministry, who through its 24,000 employees and 6,000 physicians provides a range of health care services to more than 137,000 inpatients and 3.6 million outpatients each year at SHS’ 4 acute care hospitals, home health agencies, hospice care, outpatient services, skilled nursing facilities, community clinics and physician organizations located throughout California and in parts of Texas and New Mexico.
OCR’s charges against SJH arose out of OCR’s investigation into a 2012 breach notification report SJS filed with OCR. On February 14, 2012, SJH reported to OCR that files containing electronic protected health information (ePHI) of 31,800 individuals from five of the SJH hospitals-St. Jude Medical Center, Mission Hospital, Queen of the Valley Medical Center, Santa Rosa Memorial Hospital, and Petaluma Valley Hospital that SJH created for its participation in the meaningful use program were publicly accessible on the internet from February 1, 2011, until February 13, 2012, via Google and possibly other internet search engines.
SJH’s report to OCR indicated that this public access resulted from a configuration within its network server in which PDF files containing following patient information were uploaded: patient names; BMI; blood pressure; lab results; smoking status; diagnoses lists; medication allergies; advance directive status and demographic information (language, ethnicity, race, sex, and birth date). The server SJH purchased to store the files included a file sharing application whose default settings allowed anyone with an internet connection to access them. Upon implementation of this server and the file sharing application, SJH did not examine or modify it. As a result, the public had unrestricted access to PDF files containing the ePHI of 31,800 individuals, including patient names, health statuses, diagnoses, and demographic information from February 14, 2012 until SJH blocked external access to the ePHI when it shut down the application February 13, 2012.
OCR’s investigation indicated the following potential violations of the HIPAA Rules:
- From February 1, 2011 to February 13, 2012, SJH potentially disclosed the PHI of 31,800 individuals;
- Evidence indicated that SJH failed to conduct an evaluation in response to the environmental and operational changes presented by implementation of a new server for its meaningful use project, thereby compromising the security of ePHI;
- Although SJH hired a number of contractors to assess the risks and vulnerabilities to the confidentiality, integrity and availability of ePHI held by SJH, evidence indicated that this was conducted in a patchwork fashion and did not result in an enterprise-wide risk analysis, as required by the HIPAA Security Rule.
To resolve charges resulting from these findings, the SJH Resolution Agreement requires SJH to pay OCR a $2,140,500 settlement payment and adopt a comprehensive corrective action plan which among other things, requires SJH to conduct an enterprise-wide risk analysis, develop and implement a risk management plan, revise its policies and procedures, and train its staff on these policies and procedures. SJH’s Chief Executive Officer, Annette M. Walker, is named in the Corrective Action Plan as the SJH authorized representative and contact person responsible for overseeing the CAP implementation.
Among other things, the Corrective Action Plan specifically requires that SJH:
- Within 240 days, conduct an enterprise-wide analysis and provide a report to OCR which includes a complete inventory of all electronic equipment, data systems, and applications that contain or store ePHI, and prepare and deliver to OCR for review an enterprise-wide risk analysis that identifies all security risks and vulnerabilities that incorporates all electronic equipment, data systems, and applications controlled, administered, or owned by SJH, its workforce members, and affiliated staff that contains, stores, transmits, or receives electronic protected health information (ePHJ);
- Revise this risk analysis plan as directed by OCR based on its review of the presented risk analysis;
- Develop and implement to the satisfaction of OCR an organization-wide risk management plan to address and mitigate any security risks and vulnerabilities identified in the risk analysis;
- Distribute the risk management plan as finally approved by OCR to to workforce members involved with implementation of the plan within 30 days of OCR approval;
- Revise to OCR’s satisfaction, adopt and implement within 30 days of OCR’s approval compliant HIPAA policies and procedures;
- Prepare for review of OCR training materials and once approved by OCR, provide initial training to required workforce members, and obtain certification of completion of that training from each required workforce member within 60 days of OCR’s approval of the training and thereafter at least annually as long as the Corrective Action Plan remains in force;
- Promptly conduct a documented investigation of any information indicating a potential workforce member violation of the new HIPAA policies in the manner required by OCR and if the investigation confirms a violation (Reportable Event), notify OCR of the relevant facts, findings, corrective actions and sanctions imposed against the violating workforce member in the manner required by the Corrective Action Plan;
- Submit annual report to OCR signed and attested to by an SJH officer, which contains the information and attestations of compliance with the requirements of the Corrective Action Plan in accordance with the Corrective Action Plan;
- Retain for inspection and copying and provide to OCR upon request all documents and records relating to compliance with this Corrective Action Plan for six (6) years from the Effective Date of the SJH Settlement Agreement.
Take Away For Other Covered Entities & Business Associates
The OHSU and SJH Settlement Agreements send a clear message to all Covered Entities and business associates that they must be prepared to demonstrate not only that their initial adoption and implementation of required HIPAA Privacy and Security policies and safeguards, but also that their organization’s leadership needs to be prepared to demonstrate their commitment to HIPAA compliance by making adequate provision for HIPAA compliance, and appropriately monitoring developments that could impact the adequacy of their existing measures and timely update their systems and security, policies, procedures, training and other relevant safeguards.
The Settlements make clear that Covered Entities and their business associates should ensure that their organization possesses a well-documented current enterprise-wide risk assessment, as well as has in place and is administering as necessary to maintain the currency and adequacy of its risk assessment strong practices for conducting documented evaluations of their own HIPAA security, policies, practices, audits and investigations and other procedures necessary to comply with HIPAA, taking into account recent OCR guidance, its initiation of its Phase II audit program, the insights offered by OCR’s ever growing list of enforcement actions and compliance tools, as well as changes in systems, documentation, software, equipment or other occurrences within the operations of the Covered Entity or business associate’s operations that could impact the currency and adequacy of its risk assessment or otherwise raise compliance risks.
In this respect, Covered Entities and business associates are encouraged to take special note of the advisability of specifically reviewing and updating their HIPAA policies, practices, business associate agreements, training, oversight and documentation to in response to the guidance and insight that OCR provides, including:
- A series of recent OCR Resolution Agreements emphasizing the need for Covered Entities and their Business Associates to verify that have in place, and review and update as necessary business associate agreements e.g. HIPAA Settlement Illustrates The Importance Of Reviewing And Updating, As Necessary, Business Associate Agreements (September 23, 2016); Business Associate’s Failure to Safeguard Nursing Home Residents’ PHI Leads to $650,000 HIPAA Settlement (June 29, 2016);
- Clarification of Permissible Fees for HIPAA Right of Access – Flat Rate Option Up to $6.50 is Not a Cap on All Fees for Copies of PHI (May 23, 2016)
- Guidance On HIPAA & Cloud Computing released October 6, 2016, which provides guidance for Covered Entities and business associates about contracting and other procedures that HIPAA-regulated Covered Entities and their business associates should implement when contracting for and using Cloud Computing Services;
- Joint Guidance published October 21, 2016 by the Federal Trade Commission and OCR reminding Covered Entities and their business associates of the need to ensure that in addition to fulfilling the technical content requirements of HIPAA, their HIPAA authorizations, privacy practices notices and other HIPAA notices and communications are written and presented in plan language, include required specific terms and descriptions and in a manner that does not mislead individuals about their rights or about what is happening with their PHI. Furthermore, where Covered Entities and their business associates contemplate that businesses associates may request that individuals sign HIPAA authorizations, Covered Entities and their business associates should the Covered Entity and business associate have in place a current, signed HIPAA-compliant business associate agreement that that expressly authorizes the business associate to request the HIPAA authorization in light of statements in the Joint Guidance indicating that OCR views the Privacy Rules as prohibiting a business associate from asking a consumer to sign a HIPAA authorization unless its business associate contract expressly permits the business associate to do so; and
- Other OCR enforcement actions, tools and guidance. See, e.g. All Covered Entities Should Learn Lessons From Mississippi Medical Center’s $2.75 Million HIPAA Resolution Agreement; Providers, Health Plans Should Confirm Copy Charges Comply With New OCR HIPAA Guidance; $2 Million+ HIPAA Settlement, FAQ Warn Providers Protect PHI From Media, Other Recording Or Use; Addressing Gaps in Cybersecurity: OCR Releases Crosswalk Between HIPAA Security Rule and NIST Cybersecurity Framework; HIPAA Security Rule Crosswalk to NIST Cybersecurity Framework.
Employer and other health plan sponsors, health plan fiduciaries and business associates, and their service providers also generally will want to consider their responsibilities to provide and enforce employer certifications, as well as the fiduciary obligations health plan fiduciaries under the fiduciary responsibility rules of the Employee Retirement Income Security Act (ERISA). Among other things, wrongful disclosure of PHI to a sponsoring employer or others could violate HIPAA or other plan terms. Furthermore, Department of Labor officials have indicated stated that a fiduciary’s general fiduciary responsibilities can apply to the protection and administration of PHI and other health plan information as well as create a duty by a responsible fiduciary to prudently investigate and take steps to address breaches or other potential concerns that place PHI at risk. See, HIPAA Settlement Warns Health Plans, Sponsoring Employers & Business Associates To Manage HIPAA Risks.
Furthermore, as breaches of PHI and other violations of HIPAA also frequently give rise to responsibilities or risks under a broad range of other federal and state laws medical and financial privacy and data security, Medicare and other terms of federal program participation, medical credentialing, licensure and ethics, insurance and Employee Retirement Income Security Act fiduciary responsibilities in the case of health plans, contractual, tort and other exposures, Covered Entities and their business associates also generally are best served to take into account these other responsibilities and exposures in conjunction with the design and administration of their HIPAA compliance and risk management policies and practices.
Covered Entities and their business associates also should seek advice from legal counsel regarding the adequacy of their compliance, investigatory, training, management oversight, training, reporting, documentation, document retention and other processes and procedures that could reduce risks of HIPAA violations and position the organization to effectively and more efficiently respond to a potential breach, audit, investigation or enforcement action and mitigate the costs and potential liability exposures that increasingly attends these events. In addition, given the typically high financial, operational and legal costs typically incurred to conduct investigations, report and redress breaches, and respond to OCR audits or investigations, much less make any payments and implement any corrective actions required to settle OCR changes, most Covered Entities and their business associations will want to consider the advisability and adequacy of insurance and other sources of funding or indemnification for the often substantial costs that often attend a HIPAA breach, audit or enforcement event. Since HIPAA violations under certain circumstances also can give rise to felony criminal liability, boards of directors and other leaders of Covered Entities and business associates also will want to ensure that their HIPAA compliance policies and practices also are incorporated and monitored by management as part of their organization’s overall Federal Sentencing Guideline Compliance programs and practices.
About The Author
Recognized by her peers as a Martindale-Hubble “AV-Preeminent” (Top 1%) and “Top Rated Lawyer” with special recognition LexisNexis® Martindale-Hubbell® as “LEGAL LEADER™ Texas Top Rated Lawyer” in Health Care Law and Labor and Employment Law; as among the “Best Lawyers In Dallas” for her work in the fields of “Labor & Employment,”“Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine, Cynthia Marcotte Stamer is a practicing attorney and management consultant, author, public policy advocate and lecturer widely known for work, teachings and publications on HIPAA and other privacy and data security concerns earned in connection with her more than 28 years’ of involvement advising and representing business and government clients domestically and internationally about workforce and human resources, employee benefits; health care; insurance and financial; privacy and data security and other performance management, regulatory, internal controls and other compliance, risk management, public policy and operational other key concerns.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Group Chair and current Defined Contribution Plans Committee Co-Chair, Groups and Substantive Committee and Membership Committee Members, past Welfare Plans Committee Chair and Co-Chair, and former Fiduciary Responsibility Vice Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current ABA International Section Life Sciences Committee Vice Chair, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, former ABA Joint Committee on Employee Benefits Council Representative and Marketing Committee Chair and a prolific author and highly popular speaker and consultant, Ms. Stamer helps management manage.
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
As a core component of her work, Ms. Stamer has worked extensively throughout her career with health care providers, health plans, health care clearinghouses, their business associates, employers, banks and other financial institutions, their technology and other vendors and service providers, and others on legal and operational risk management and compliance with HIPAA, FACTA, PCI, trade secret, physician and other medical confidentiality and privacy, federal and state data security and data breach and other information privacy and data security rules and concerns; prevention, investigation, response, mitigation and resolution of known or suspected data or privacy breaches or other incidents; defending investigations or other actions by plaintiffs, OCR, FTC, state attorneys’ general and other federal or state agencies; reporting and redressing known or suspected breaches or other violations; business associate and other contracting; insurance or other liability management and allocation; process and product development, contracting, deployment and defense; evaluation, commenting or seeking modification of regulatory guidance, and other regulatory and public policy advocacy; training and discipline; enforcement, and a host of other related concerns for public and private health care providers, health insurers, health plans, technology and other vendors, employers, and others.
Beyond her extensive involvement advising and representing clients on privacy and data security concerns and other health industry matters, Ms. Stamer also has served for several years as a scrivener for the ABA JCEB’s meeting with OCR, the Chair of the Southern California ISSA Health Care Privacy & Security Summit, and an editorial advisory board member, author, program chair or steering committee member, and faculties for a multitude of other programs and publications regarding privacy, data security, technology and other compliance, risk management and operational concerns in the health care, health and other insurance, employee benefits and human resources, retail, financial services and other arenas.
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Ms. Stamer also shares shared her thought leadership, experience and advocacy on HIPAA and other concerns by her service in the leadership of a broad range of other professional and civic organization including her involvement as the Vice Chair of the North Texas Healthcare Compliance Association, Executive Director of the Coalition on Responsible Health Policy and its PROJECT COPE: Coalition on Patient Empowerment, a founding Board Member and past President of the Alliance for Healthcare Excellence, past Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; former Board President of the early childhood development intervention agency, The Richardson Development Center for Children; former Board Compliance Chair and Board member of the National Kidney Foundation of North Texas, current Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current Vice Chair of Policy for the Life Sciences Committee of the ABA International Section, Past Chair of the ABA Health Law Section Managed Care & Insurance Section, a current Defined Contribution Plan Committee Co-Chair, former Group Chair and Co-Chair of the ABA RPTE Section Employee Benefits Group, immediate past RPTE Representative to ABA Joint Committee on Employee Benefits Council Representative and current RPTE Representative to the ABA Health Law Coordinating Council, former Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division, past Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee, a former member of the Board of Directors of the Southwest Benefits Association and others.
Ms. Stamer also is a highly popular lecturer, symposia chair and author, who publishes and speaks extensively on health and managed care industry, human resources, employment and other privacy, data security and other technology, regulatory and operational risk management. Examples of her many highly regarded publications on these matters include “Protecting & Using Patient Data In Disease Management: Opportunities, Liabilities And Prescriptions,” “Privacy Invasions of Medical Care-An Emerging Perspective,” “Cybercrime and Identity Theft: Health Information Security: Beyond HIPAA,” as well as thousands of other publications, programs and workshops these and other concerns for the American Bar Association, ALI-ABA, American Health Lawyers, Society of Human Resources Professionals, the Southwest Benefits Association, the Society of Employee Benefits Administrators, the American Law Institute, Lexis-Nexis, Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, the HCCA, ISSA, HIMSS, Modern Healthcare, Managed Healthcare, Institute of Internal Auditors, Society of CPAs, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other symposia and publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications and speaks and conducts training for a broad range of professional organizations and for clientson the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and many other publications. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal controls and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at http://www.solutionslawpress.com such as:
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here.
©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™ All other rights reserved.
 Comments Off on Health Plans, Other Covered Entities Have Continuing Duty To Reevaluate HIPAA Enterprise Risk To PHI & Address Security Risks & Other Compliance Concern On Ongoing Basis |
Comments Off on Health Plans, Other Covered Entities Have Continuing Duty To Reevaluate HIPAA Enterprise Risk To PHI & Address Security Risks & Other Compliance Concern On Ongoing Basis |  ARRA, board of directors, Brokers, Cafeteria Plans, CHIP, Civil Monetary Penalties, Civil Rights, Claims, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, EBSA, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, Employment, EMR, fiduciary duty, Fiduciary Responsibility, GINA, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Technology, third party administrators, Uncategorized, Union, Workforce | Tagged: Breach Notification, broker, Covered Entity, Data Breach, Data Security, EPHI, ERISA, health care providers, Health Plans, HIPAA, Medical Privach, Medical Privacy, Personal Health Information, Privacy, Technology |
ARRA, board of directors, Brokers, Cafeteria Plans, CHIP, Civil Monetary Penalties, Civil Rights, Claims, compliance, Consumer Protection, Corporate Compliance, corporate governance, Cybercrime, Data Breach, Data Security, directors, EBSA, Electronic Medical Record, employee, Employee Benefits, Employer, Employers, Employment, EMR, fiduciary duty, Fiduciary Responsibility, GINA, HIPAA, HR, Human Resources, Identity Theft, Insurance, insurers, Internal Controls, Internal Investigations, Technology, third party administrators, Uncategorized, Union, Workforce | Tagged: Breach Notification, broker, Covered Entity, Data Breach, Data Security, EPHI, ERISA, health care providers, Health Plans, HIPAA, Medical Privach, Medical Privacy, Personal Health Information, Privacy, Technology |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
October 21, 2016
Colleges and other institutions of higher education within the meaning of the Higher Education Act of 1965 (schools) may continue until further notice to pay or subsidize student health insurance coverage premiums for students performing work-study or other services for the school as part of their financial aid package without fear of prosecution for violation of the group market reform requirements of the Patient Protection & Affordable Care Act (ACA), according to ACA guidance jointly published by the Departments of Labor (DOL), Health and Human Services (HHS), and the Treasury (collectively, the Tri-Agencies) today.
Many schools have arrangements in place with insurers under which students can purchase individual policies providing health insurance coverage (“student health insurance coverage”), which are individual policies required to comply with the individual market reforms of the ACA other than as provided in the student health insurance guidance issued by HHS. See 45 CFR 147.145.
Of course, the agreement between the college and the student health insurance coverage issuer makes the coverage available for purchase by most if not all students attending the school by paying the specified premium. In some cases, however, the school might include in a student’s financial aid package a reduction to the cost of coverage of the otherwise applicable premium for student health insurance through a credit, offset, reimbursement, stipend, or similar arrangement (a premium reduction arrangement). If the student also performs services under a workstudy or other relationship, however, Tri-Agency guidance interpreting the Group Market Reforms could present a problem unless qualifies for an exemption from the Tri-Agencies’ interpretation of the Group Market Reforms as prohibited employers from paying or reimbursing individual health insurance policy premiums of employees..
The Tri-Agencies’ first announced their interpretation of the Group Market Reforms as prohibiting employer reimbursement of individual health insurance premiums in 2013. Technical Release 2013-03 announced that employers sponsoring arrangements under which the employer directly pays or reimburses premiums for employees’ individual health insurance coverage directly, or through a cafeteria plan pre-tax premium program, health flexible spending account arrangement (health FSA), health reimbursement arrangement (HRA), or other employer arrangement would incur excise taxes liability under section 4980D of the Internal Revenue Code and other penalties and liabilities for violating the ACA Group Market Reform rules. This Tri-Agency Guidance states that because by their very definition, these arrangements promise to reimburse or pay medical expenses on the employee’s behalf only up to a certain dollar amount each year, employer-sponsored arrangements that pay or reimburse employees for individual health insurance premiums generally violate the prohibition on annual dollar limits under Public Health Services (PHS) Act section 2711 and the requirement to provide certain preventive services without cost sharing under PHS Act section 2713 unless properly integrated with a group health plan that otherwise complies with ACA requirements. Furthermore, because the Tri-Agencies also construe the ACA market reforms as preventing the integration of EPPs and individual health insurance coverage, the Tri-Agencies’ guidance also states that an arrangement through which an employer reimburses or directly pays the premium for individual coverage violates the ACA market reform rules. Accordingly, unless otherwise exempted from coverage, this Tri-Agency guidance would prohibit schools from reimbursing students providing services to the school for student health insurance premiums.
Under Tri-Agency guidance published in February, 2016, the Tri-Agencies previously announced they would not that a premium reduction arrangement provided by a school to a student fails to satisfy PHS Act section 2711 or 2713 if the arrangement is offered in connection with other student health coverage (insured or self-insured) for a plan year or policy year beginning before January 1, 2017, but until October 21, 2016, did not address the post-2016 treatment of these arrangements . See Technical Release 2016-01; Notice 2016-17, Insurance Standards Bulletin, Application of the Market Reforms and Other Provisions of the Affordable Care Act to Student Health Coverage.
Under guidance jointly published October 21, 2016, however, the Tri-Agencies extended their policy of non-enforcement with respect to school student health insurance premium reimbursement arrangements beyond its previously announced December 31, 2016 expiration date. FAQs About Affordable Care Act Implementation Part 33 (“FAQ 33”) jointly published by the Tri-Agencies states that “pending further guidance, the Tri-Agencies consider it appropriate to further extend the enforcement relief provided in the February 5, 2016 guidance and will not assert that a premium reduction arrangement offered by an institution of higher education fails to satisfy PHS Act section 2711 or 2713 if the arrangement is offered in connection with student health coverage (insured or self-insured).
About The Author
Cynthia Marcotte Stamer is a noted Texas-based management lawyer and consultant, author, lecture and policy advocate, recognized for her nearly 30-years of cutting edge management work as among the “Top Rated Labor & Employment Lawyers in Texas” by LexisNexis® Martindale-Hubbell® and as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,”“Tax: Erisa & Employee Benefits,” “Health Care” and “Business and Commercial Law” by D Magazine.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Group Chair and current Defined Contribution Plans Committee Co-Chair, Groups and Substantive Committee and Membership Committee Members, past Welfare Plans Committee Chair and Co-Chair, and former Fiduciary Responsibility Vice Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, current ABA International Section Life Sciences Committee Vice Chair, past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, former ABA Joint Committee on Employee Benefits Council Representative and Marketing Committee Chair and a prolific author and highly popular speaker and consultant, Ms. Stamer helps management manage.
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
For additional information about this topic or Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal control and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at http://www.Solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. ©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
IMPORTANT NOTICES
These statements and materials are for general informational and purposes only. They do not establish an attorney-client relationship, are not legal advice, and do not serve as a substitute for legal advice. Readers are urged to engage competent legal counsel for consultation and representation in light of the specific facts and circumstances presented in their unique circumstance at any particular time. No comment or statement in this publication is to be construed as an admission. The author reserves the right to qualify or retract any of these statements at any time. Likewise, the content is not tailored to any particular situation and does not necessarily address all relevant issues. Because the law is rapidly evolving and rapidly evolving rules makes it highly likely that subsequent developments could impact the currency and completeness of this discussion. The presenter and the program sponsor disclaim, and have no responsibility to provide any update or otherwise notify any participant of any such change, limitation, or other condition that might affect the suitability of reliance upon these materials or information otherwise conveyed in connection with this program. Readers may not rely upon, are solely responsible for, and assume the risk and all liabilities resulting from their use of this publication.
Circular 230 Compliance. The following disclaimer is included to ensure that we comply with U.S. Treasury Department Regulations. Any statements contained herein are not intended or written by the writer to be used, and nothing contained herein can be used by you or any other person, for the purpose of (1) avoiding penalties that may be imposed under federal tax law, or (2) promoting, marketing or recommending to another party any tax-related transaction or matter addressed herein
 Comments Off on New ACA Student Health Insurance Guidance Allows College Payment Of Working Students’ Student Health Insurance Premiums Post 2016 |
Comments Off on New ACA Student Health Insurance Guidance Allows College Payment Of Working Students’ Student Health Insurance Premiums Post 2016 |  105(h), 4980D, 6039D, ACA, Affordable Care Act, Cafeteria Plans, compliance, Employee Benefits, Employer, Employers, Employment, ERISA, health benefit, health insurance, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Patient Protection and Affordabel Care Act, Uncategorized | Tagged: ACA, College, employer payment plan, Financial Aid, higher education, HRA, HSA, premium reimbursement, Schools |
105(h), 4980D, 6039D, ACA, Affordable Care Act, Cafeteria Plans, compliance, Employee Benefits, Employer, Employers, Employment, ERISA, health benefit, health insurance, Health Plans, health reform, HR, Human Resources, Insurance, insurers, Internal Controls, Patient Protection and Affordabel Care Act, Uncategorized | Tagged: ACA, College, employer payment plan, Financial Aid, higher education, HRA, HSA, premium reimbursement, Schools |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 31, 2016
U.S. employers, employment agencies, unions, their benefit plans and fiduciaries, and their management and service providers should move quickly to review and strengthen their employment and other practices to guard against a foreseeable surge in employee retaliation claims and judgements likely to follow the August 30, 2016 issuance by the Equal Employment Opportunity Commission (EEOC) of its new final EEOC Enforcement Guidance on Retaliation and Related Issues and concurrently published Question and Answer Guidance(Guidance).
Updating and superceding 2008 guidance previously set forth in the Retaliation Chapter of the EEOC Enforcement Manual, the Guidance details the EEOC’s current policy for investigating and enforcing the retaliation prohibitions under each of the equal employment opportunity (EEO) laws enforced by EEOC, including Title VII of the Civil Rights Act of 1964, the Age Discrimination in Employment Act (ADEA), Title V of the Americans with Disabilities Act (ADA), Section 501 of the Rehabilitation Act, the Equal Pay Act (EPA) and Title II of the Genetic Information Nondiscrimination Act (GINA) as well as the ADA’s separate “interference” prohibitions, which prohibit coercion, threats, or other acts that interfere with the exercise of ADA rights. Among other things, the Guidance discusses :
- What “retaliation means” and the scope of employee activity protected by the prohibitions against retaliation included in all laws enforced by the EEOC as well as the interference prohibitions of the ADA;
- Legal analysis the EEOC will use to determine if evidence supports a claim of retaliation against an employer or other party;
- Detailed examples of employer actions that the EEOC says may constitute prohibited retaliation; and
Remedies available for retaliation.
Understanding and properly responding to the Guidance is critically important for employers and other subject to the EEO laws because in light of the substantial and growing liability exposures retaliation claims present and the likely that the issuance of the Guidance will further fuel these risks.
Even before the EEOC published the Guidance, retaliation and interference exposures were a substantial source of concern for most employers. Employers, employment agencies and unions caught engaging in prohibited retaliation or intimidation in violation of EEO laws can incur compensatory and (except for governmental employers) punitive damage awards, back pay, front pay, reinstatement into a job or other equitable remedies, injunctive or administrative orders requiring changes in employer policies and procedures, managerial training, reporting to the EEOC and other corrective measures, as well as substantial investigation and defense costs.
These substantial liability exposures have become particularly concerning as retaliation and interference claims also have become increasingly common over the past decade. According to the EEOC, for example, EEO law retaliation charges have remained the most frequently alleged basis of charges filed with the EEOC since 2009 and in Fiscal Year 2015 accounted for 44.5 percent of all employment discrimination charges received by EEOC.
Since the EEOC’s issuance of the Retaliation Regs are likely to encourage additional retaliation or interference claims, employers, employment agencies, unions and their management, service providers and agents should quickly to evaluate the updated guidance provided in the Retaliation Reg and act to mitigate their exposure to retaliation retaliation and interference claims under these EEO laws.
Retaliation Risks Under EEO Laws
Federal EEO laws generally prohibit employers, employment agencies, or unions from punishing or taking other adverse actions against job applicants or employees for “asserting their rights” (often referred to as “protected activity”) to be free from harassment or other prohibited employment discrimination as well as certain other conduct. Such claims generally are referred to as “retaliation claims.”
Prohibited retaliation in violation of EEO laws occurs when an employer, employment agency or union takes a materially adverse action because an applicant or employee asserts rights or engages in certain other activities protected by the EEO laws.
To prevail in a retaliation claim, an applicant, employee or other individual generally must show that:
- The individual engaged in prior protected activity;
- The employer, employment agency or union took a materially adverse action; and
- More likely than not, retaliation caused the adverse action by the employer, employment agency or union.
Persons Protected By EEO Retaliation Rules
EEO retaliation prohibitions protect both applicants and current and former employees (full-time, part-time, probationary, seasonal, and temporary) against retaliation under the EEO laws. The retaliation prohibitions bar an employer from refusing to hire or otherwise taking adverse action against any current or former applicant or employee because of his EEO complaint or other protected activity under applicable EEO laws. The EEOC interprets the retaliation rules as prohibiting an employer from giving a false negative job reference to punish a former employee for making an EEO complaint or engaging in other protected activity as well as as prohibiting an employer from refusing to hire or otherwise retaliating or discriminating against an applicant or employee based on a complaint made or other protected activity engaged against any a prior employer. The Guidance also makes clear that the retaliation prohibitions apply regardless of an applicant or employee’s citizenship or work authorization status.
Protected Activity
“Protected activity” generally means either participating in an EEO process or reasonably opposing conduct made unlawful by an EEO law.
The prohibition against an employer retaliating against an individual for “participating” in an EEO process means that an employer cannot punish an applicant or employee for filing an EEO complaint, serving as a witness, or participating in any other way in an EEO matter, even if the underlying discrimination allegation is unsuccessful or untimely. As a part of these prohibitions, the EEOC says that an employer, employment agency or union is not allowed to do anything in response to EEO activity that would discourage someone from resisting or complaining about future discrimination. For example, depending on the facts of the particular case, it could be retaliation because of the employee’s EEO activity for an employer to:
- Reprimand an employee or give a performance evaluation that is lower than it should be;
- Transfer the employee to a less desirable position;
- Engage in verbal or physical abuse;
- Threaten to make, or actually make reports to authorities (such as reporting immigration status or contacting the police);
- Increase scrutiny;
- Spread false rumors, treat a family member negatively (for example, cancel a contract with the person’s spouse); or
-
Take action that makes the person’s work more difficult (for example, punishing an employee for an EEO complaint by purposefully changing his work schedule to conflict with family responsibilities).
The Guidance clearly states that the EEOC views participating in any capacity in a complaint process or other protected equal employment opportunity as protected activity which is protected from retaliation under all circumstances. The EEOC views other acts to oppose discrimination also as protected as long as the employee was acting on a reasonable belief that something in the workplace may violate EEO laws, even if he or she did not use legal terminology to describe the issue. EEOC’s view is that protections against retaliation extend to participation in an employer’s internal EEO complaint process, even if a charge of discrimination has not yet been filed with the EEOC. The EEOC also takes the position that participation in the EEO process is protected whether or not the EEO allegation is based on a reasonable, good faith belief that a violation occurred. While an employer is free to bring these to light in the EEO matter where it may rightly affect the outcome, the Retaliation Regs state it is unlawful retaliation for an employer to take matters into its own hands and impose consequences for participating in an EEO matter.
In addition to prohibition for participation in protected activities, EEO law also prohibits retaliation against an individual for “opposing” a perceived unlawful EEO practice. The EEOC construes prohibition against retaliation for opposition as prohibiting an employer or other covered entity from punishing an applicant or employee for communicating or taking other action in opposition of a perceived EEO violation if the individual acted reasonably and based on a reasonable good faith belief that the conduct opposed is or could become unlawful if repeated.
According to the EEOC, opposition also can be protected even if it is informal or does not include the words “harassment,” “discrimination,” or other legal terminology. A communication or act may be protected opposition as long as the circumstances show that the individual is conveying resistance to a perceived potential EEO violation such as, for example:
- Complaining or threatening to complain about alleged discrimination against oneself or others;
- Taking part in an internal or external investigation of employment discrimination, including harassment;
- Filing or being a witness in a charge, complaint, or lawsuit alleging discrimination;
- Communicating with a supervisor or manager about employment discrimination, including harassment;
- Answering questions during an employer investigation of alleged harassment;
- Refusing to follow orders that would result in discrimination;
- Resisting sexual advances, or intervening to protect others;
- Reporting an instance of harassment to a supervisor;
- Requesting accommodation of a disability or for a religious practice;
- Asking managers or co-workers about salary information to uncover potentially discriminatory wages;
- Providing information in an employer’s internal investigation of an EEO matter;
- Refusing to obey an order reasonably believed to be discriminatory;
- Advising an employer on EEO compliance;
- Resisting sexual advances or intervening to protect others;
- Passive resistance (allowing others to express opposition);
- Requesting reasonable accommodation for disability or religion;
- Complaining to management about EEO-related compensation disparities;
- Talking to coworkers to gather information or evidence in support of a potential EEO claim; or
- Other acts of opposition.
In order for the protection against opposition to apply, however, the individual must act with a reasonable good faith belief that the conduct opposed is unlawful or could become unlawful if repeated. Opposition not based on such a good faith belief is not protected. Employers should note that the EEOC takes the position that opposition by an employee could qualify as reasonable opposition protected against retaliation when an employee or applicant complains about behavior that is not yet legally harassment (i.e., even if the mistreatment has not yet become severe or pervasive) or to complain about conduct the employee believes violates the EEO laws if the EEOC has adopted that interpretation, even if some courts disagree with the EEOC on the issue.
Furthermore, an individual opposing a perceived violation of an EEO law is disqualified for protection against retaliation for his opposition unless the individual behaves in a reasonable manner when expressing his opposition. For example, threats of violence, or badgering a subordinate employee to give a witness statement, are not protected opposition.
Subject to these conditions, however, the Guidance states that retaliation for opposing perceived unlawful EEOC practices need not be applied directly to the employee to qualify for protection. If an employer, employment agency or union takes an action against someone else, such as a family member or close friend, in order to retaliate against an employee, the EEOC says both individuals would have a legal claim against the employer.
Moreover, according to the EEOC, the prohibitions against retaliation for participation and opposition apply regardless of whether the person is suffers the retaliation for acting as a witness or otherwise participating in the investigation of a prohibited practice regarding an EEO complaint brought by others, or for complaining of conduct that directly affects himself.
Materially Adverse Action
To fall within EEO law prohibitions against retaliation, the retaliatory actions must be “materially adverse,” which the Guidance defines to include any action that under the facts and circumstances might deter a reasonable person from engaging in protected activity. This definition of “materially adverse” sweeps broadly to include more than employment actions such as denial of promotion, non-hire, denial of job benefits, demotion, suspension, discharge, or other actions that can be challenged directly as employment discrimination. It also encompasses within the scope of retaliation employer action that is work-related, as well as other actions with no tangible effect on employment, or even an action that takes place exclusively outside of work, as long as it may well dissuade a reasonable person from engaging in protected activity.
Whether an action is materially adverse depends on the facts and circumstances of the particular case. The U.S. Supreme Court has held that transferring a worker to a harder, dirtier job within the same pay grade, and suspending her without pay for more than a month (even though the pay was later reimbursed) were both “materially adverse actions” that could be challenged as retaliation. The Supreme Court has also said that actionable retaliation includes: the FBI’s refusing to investigate death threats against an agent; the filing of false criminal charges against a former employee; changing the work schedule of a parent who has caretaking responsibilities for school-age children; and excluding an employee from a weekly training lunch that contributes to professional advancement.
In contrast, a petty slight, minor annoyance, trivial punishment, or any other action that is not likely to dissuade an employee from engaging in protected activity in the circumstances is not “materially adverse.” For example, courts have concluded on the facts of given cases that temporarily transferring an employee from an office to a cubicle was not a materially adverse action and that occasional brief delays by an employer in issuing refund checks to an employee that involved small amounts of money were not materially adverse.
The facts and circumstances of each case determine whether a particular action is retaliatory in that context. For this reason, the same action may be retaliatory in one case but not in another. Depending on the facts, other examples of “materially adverse” actions may include:
- Work-related threats, warnings, or reprimands;
- Negative or lowered evaluations;
- Transfers to less prestigious or desirable work or work locations;
- Making false reports to government authorities or in the media;
- Filing a civil action;
- Threatening reassignment;
- Scrutinizing work or attendance more closely than that of other employees, without justification;
- Removing supervisory responsibilities;
- Engaging in abusive verbal or physical behavior that is reasonably likely to deter protected activity, even if it is not yet “severe or pervasive” as required for a hostile work environment;
- Requiring re-verification of work status, making threats of deportation, or initiating other action with immigration authorities because of protected activity;
- Terminating a union grievance process or other action to block access to otherwise available remedial mechanisms; or
- Taking (or threatening to take) a materially adverse action against a close family member (who would then also have a retaliation claim, even if not an employee).
ADA Interference Claims
In addition to the need to manage potential exposures for prohibited retaliation, employers, employment agencies and unions also should be careful to manage their exposure to potential liability arising from claims for wrongful interference and individual’s exercise of the disability rights or protections granted under the ADA.
The ADA generally prohibits disability discrimination, limits an employer’s ability to ask for medical information, requires confidentiality of medical information, and gives employees who have disabilities the right to reasonable accommodations at work absent undue hardship and like other EEO laws, prohibits retaliation. In addition to its prohibitions against retaliation, however, the ADA also more broadly prohibits “interference” with statutory rights under the ADA.
Interference is broader than retaliation. The ADA’s interference provision makes it unlawful to coerce, intimidate, threaten, or otherwise interfere with an individual’s exercise of ADA rights, or with an individual who is assisting another to exercise ADA rights.
In addition, the ADA also prohibits employers from interfering with ADA rights by doing anything that makes it more difficult for an applicant or employee to assert any of these rights such as using threats or other actions to discourage someone from asking for, or keeping, a reasonable accommodation; intimidating an applicant or employee into undergoing an unlawful medical examination; or pressuring an applicant or employee not to file a disability discrimination complaint.
Prohibited interference may be actionable under the ADA even if ineffective and even if the person subjected to intimidation goes on to exercise his ADA rights.
- While acknowledging that some employer actions may be both retaliation and interference, or may overlap with unlawful denial of accommodation, the Guidance identifies the following actions as examples of interference prohibited under the ADA:
- Coercing an individual to relinquish or forgo an accommodation to which he or she is otherwise entitled;
- Intimidating an applicant from requesting accommodation for the application process by indicating that such a request will result in the applicant not being hired;
- Threatening an employee with loss of employment or other adverse treatment if he does not “voluntarily” submit to a medical examination or inquiry that is otherwise prohibited under the statute;
- Issuing a policy or requirement that purports to limit an employee’s rights to invoke ADA protections (e.g., a fixed leave policy that states “no exceptions will be made for any reason”);
- Interfering with a former employee’s right to file an ADA lawsuit against the former employer by stating that a negative job reference will be given to prospective employers if the suit is filed; and
- Subjecting an employee to unwarranted discipline, demotion, or other adverse treatment because he assisted a coworker in requesting reasonable accommodation.
According to the EEOC, a threat does not have to be carried out in order to violate the interference provision, and an individual does not actually have to be deterred from exercising or enjoying ADA rights in order for the interference to be actionable.
Strategies To Help Deter Or Rebut Retaliation Charges
Even though individuals claiming retaliation technically bear the burden of proving more likely than not that he suffered an adverse employment action more probably than not as a result of retaliation, an employer, employment agency or union charged with illegal retaliation frequently need to rebut or undermine a claimant’s evidence of retaliation by having and introducing admissible evidence that it a non-retaliatory reason for taking the challenged action such as evidence that:
- The employer was not, in fact, aware of the protected activity;
- There was a legitimate non-retaliatory motive for the challenged action, that the employer can demonstrate, such as poor performance; inadequate qualifications for position sought; qualifications, application, or interview performance inferior to the selectee; negative job references (provided they set forth legitimate reasons for not hiring or promoting an individual); misconduct (e.g., threats, insubordination, unexcused absences, employee dishonesty, abusive or threatening conduct, or theft); or reduction in force or other downsizing;
- Similarly-situated applicants or employees who did not engage in protected activity were similarly treated;
- Where the “but-for” causation standard applies, there is evidence that the challenged adverse action would have occurred anyway, despite the existence of a retaliatory motive; or
- Other credible evidence showing a legitimate, non-discriminatory and non-retalitory motive behind the action.
It is important that employer other other potential defendants in retaliation actions recognize and take appropriate steps to create and retain evidence documenting these or other legitimate business reasons justifying the action prior to taking adverse action. Many employer or other defendants charged with discrimination or retaliation discover too late that a rule of evidence commonly referred to as the “After Acquired Evidence Doctrine” often prevents an employer or other defendant from using documentation or other evidence of motive created after the adverse action occurs. Consequently, employer and other potential targets of retaliation claims before taking the adverse action would be wise to carefully collect, document and retain the evidence and analysis showing their adverse action was taken for a legitimate, nonretalitory, nondiscriminatory reason rather than for any retaliatory purpose.
Other Defensive Actions & Strategies
Beyond taking care to document and retain evidence of its legitimate motivations for taking an adverse employment action, employers, employment agencies and unions interested in avoiding or enhancing their defenses against retaliation or interference claims also may find it helpful to:
- Maintain a written, plain-language anti-retaliation and anti-interference policy that provides practical guidance on the employer’s expectations with user-friendly examples of what to do and not to do;
- Send a message from top management that retaliation and interference are prohibited and will not be tolerated;
- Ensure that top management understands and complies with policies against prohibited discrimination, retaliation and interference;
- Consistently and fairly administer all equal employment opportunity and other policies and procedures in accordance with applicable laws in a documented, defensible manner;
- Post and provide all required posters or other equal employment opportunity notices;
- Timely and accurately complete and file all required EEO reports;
- Clearly communicate orally and in writing the policy against prohibited retaliation and interference, as well as procedures for reporting, investigating and addressing concerns about potential violations of these policies in corporate policies as well as to employees complaining or participating in investigations or other protected activities;
- Conduct documented training for all managers, supervisors and other employees and agents of the employer about policies against prohibited discrimination, retaliation, and interference including, as necessary, specific education about specific behaviors or situations that could raise retaliation or interference concerns, when and how to report or respond to such concerns and other actions to take to prevent or stop potential retaliation and interference;
- Establish and administer clear policies and procedures for reporting and investigating claims or other indicators of potential prohibited employment discrimination, retaliation, interference including appropriate procedures for monitoring and protecting applicants and workers who have made claims of discrimination or have a record of involvement in activities that might qualify for corrective action;
- Review performance, compensation and other criteria for potential evidence of overt or hidden bias or other evidence of potential prohibited retaliation or interference and take documented corrective action as needed to prevent improper bias from adversely corrupting decision-making process;
- Conduct timely, well-documented investigations of all reports or other evidence of suspected discrimination, retaliation, and interference including any disciplinary, remedial or corrective action taken or foregone and the justification underlying these actions;
- Obtain and enforce contractual reassurances from recruiting, staffing and other contractors to adhere to, and cooperate with the employer in its investigation and redress of the nondiscrimination, data collection and reporting, anti-retaliation and anti-interference requirements of equal employment opportunity and other laws;
- Incorporate appropriate inquiries and other procedures for documented evaluating and monitoring that hiring, staffing, performance review, promotion, demotion, discipline, termination and other employment decisions and actions for evidence or other indicators of potential prohibited discrimination, retaliation, interference or other prohibited conduct and take corrective action as necessary based on the evidence developed; and
- Designate appropriately empowered and trained members of the management of the employer to receive and investigate complaints and other potential concerns;
Arrange for an unbiased third party review of the adverse action or the performance or other decision criteria, processes and analysis that the employer or other defendant contemplates relying on to decide and implement employment decisions for indicators of potential discriminatory, retaliatory or other illegal or undesirable biasand take corrective action as needed to address those concerns before undertaking employment actions;
- Evaluate and allocate appropriate funds within the employer’s budget to support the employer’s compliance efforts as well as to provide for the availability of sufficient funds to investigate and defend potential charges or public or private charges of illegal discrimination, retaliation or interference through the purchase of employment practices liablity or other insurance coverages or otherwise;
- If a manager or other party recommends an adverse action in the wake of an employee’s filing of an EEOC charge or participation in other protected activity, conducting or arranging for an another party to ndependently evaluate whether the adverse action is appropriate;
- Proactively seek assistance from qualified legal counsel with the design and review of policies, practices and operations, investigation and analysis of internal or external complaints or other concerns about potential prohibited discrimination, retaliation or interference, review and execution of termination, discipline or other workforce events to mitigate discrimination, retaliation or interference risks as well as the defense of EEOC or private enforcement actions; and
- Be ever diligent in your efforts to prevent, detect and redress actions or situations that could be a basis for retaliation or interference claims.
About The Author
Cynthia Marcotte Stamer is a noted Texas-based management lawyer and consultant, author, lecture and policy advocate, recognized for her nearly 30-years of cutting edge management work as among the “Top Rated Labor & Employment Lawyers in Texas” by LexisNexis® Martindale-Hubbell® and as among the “Best Lawyers In Dallas” for her work in the field of “Labor & Employment,”“Tax: Erisa & Employee Benefits” “Health Care” and “Business and Commercial Law” by D Magazine.
Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, a Fellow in the American College of Employee Benefit Counsel, past Chair and current committee Co-Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, former Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, a former ABA Joint Committee on Employee Benefits Council Representative and , Ms. Stamer helps management manage.
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping organizations and their management use the law and process to manage people, process, compliance, operations and risk. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
Solutions Law Press, Inc.™ provides human resources and employee benefit and other business risk management, legal compliance, management effectiveness and other coaching, tools and other resources, training and education on leadership, governance, human resources, employee benefits, data security and privacy, insurance, health care and other key compliance, risk management, internal control and operational concerns. If you find this of interest, you also be interested reviewing some of our other Solutions Law Press, Inc.™ resources at www.Solutionslawpress.com.
If you or someone else you know would like to receive future updates about developments on these and other concerns, please be sure that we have your current contact information including your preferred e-mail by creating or updating your profile here. ©2016 Cynthia Marcotte Stamer. Non-exclusive right to republish granted to Solutions Law Press, Inc.™. All other rights reserved.
 Comments Off on Manage Retaliation Risks In Response To Updated EEOC Enforcement Guidance, Rising Retaliation Claims |
Comments Off on Manage Retaliation Risks In Response To Updated EEOC Enforcement Guidance, Rising Retaliation Claims |  Accommodation, ADA, Affirmative Action, Civil Rights, compensation, Corporate Compliance, corporate governance, Disability, Disability, Disability Discrimination, Disability Plans, Discrimination, E-Verify, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Government Contractors, Hiring, HR, Human Resources, Internal Controls, Internal Investigations, Leave, LEP, LGBT, Management, Managment, Risk Management, Sexual Harassment, Uncategorized, Workforce | Tagged: Civl Rights, Discrimination, EEOC, Employee, Employer, Employment Agency, employment discrimination, Equal Employment Opportunity, Interference, Retaliation, Union |
Accommodation, ADA, Affirmative Action, Civil Rights, compensation, Corporate Compliance, corporate governance, Disability, Disability, Disability Discrimination, Disability Plans, Discrimination, E-Verify, EEOC, employee, Employee Benefits, Employer, Employers, Employment, Employment Discrimination, Government Contractors, Hiring, HR, Human Resources, Internal Controls, Internal Investigations, Leave, LEP, LGBT, Management, Managment, Risk Management, Sexual Harassment, Uncategorized, Workforce | Tagged: Civl Rights, Discrimination, EEOC, Employee, Employer, Employment Agency, employment discrimination, Equal Employment Opportunity, Interference, Retaliation, Union |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer
August 1, 2016
The U.S. Department of Labor’s just announced successful whistleblower prosecution in Perez v. Scott Brain, et al of an employee benefit plan trustee, and an individual lawyer and her law firm that served as the employee benefit plan’s outside legal counsel of violating the fiduciary responsibility and whistleblower rules of the Employee Retirement Income Security Act of 1974 (ERISA) illustrates why employee benefit plan sponsors, trustees or other fiduciaries, their management, legal counsel, auditors and other service providers must both prudently investigate whistleblower allegations or other evidence of potential wrongdoing involving their employee benefit plans and resist the temptation to retaliate against employees or others for reporting or cooperating in the investigation of alleged improprieties involving an employee benefit plan.
The Brain decision highlights the care that employee benefit plan sponsors, fiduciaries, advisors and service providers and their management must use when responding to allegations or other evidence of wrongdoing relating to an employee benefit plan or its administration, investigating and addressing alleged misconduct or other performance or disciplinary concerns involving parties whose report or involvement in investigations of ERISA or other misconduct could form the basis of a potential ERISA 510 or other retaliation complaint.
The decision also makes clear that outside legal counsel advising an employee benefit plan or its fiduciaries in relation to the investigation or response to charges of ERISA misconduct involving an employee benefit plan must use care to avoid actions that could render them liable for participation in acts of illegal retaliation, violating their duty of loyalty to the plan by allowing themselves to become involved in a conflict of interest when investigating or defending potential wrongdoing involving an employee benefit plan, or engaging in other discretionary actions that could constitute a breach of fiduciary duty in violation of ERISA.
In Perez v. Scott Brain, et al., the U.S. District Court for the Central District of California ruled that Cement Masons Southern California Trust Fund’s trustee and Cement Masons Local 600 business manager, Scott Brain (Brain) and outside trust fund legal counsel, Melissa Cook, violated sections 510 and 404 of ERISA by causing the firing a trust fund employee Cheryle Robbins (Robbins) and an employee of the plan’s third party administrator, Cory Rice (Rice), in retaliation for their involvement in filing an internal complaint about and cooperating with the Labor Department’s Employee Benefit Security Administration’s federal criminal investigation of reports of Brain’s wrongful interference as a trustee with collections and contributions from unionized employers.
In 2011, Robbins, director of the trust funds’ audit and collections department, responded to a federal criminal investigation into Brain’s activities with contractors. The same year, she and Rice, who worked for the third-party administrator to the trust fund, American Benefit Plan Administrators, now, Zenith American Solutions (Zenith), participated in an effort to complain about Brain’s interference with efforts to collect delinquent contributions from contractors. Within weeks of this conduct, Robbins was suspended from her employment with the trust fund. Less than six months later, both Robbins and Rice were fired.
The court’s 71-page decision chronicles the coordinated retaliatory campaign orchestrated by Brain and Cook that led to Robbins’ suspension and firing by the employee benefit plan as well as the termination of Cook by his employer, Zenith..
With respect to Robbins’ suspension, the court found that the evidence showed Brain and Cook “were very upset with Robbins due to her contact with the [Department of Labor],” and that Brain and Cook “used their positions and influence to cause the other trustees to vote in favor of” suspending Robbins. To do so, the court explained, Brain and Cook “took the lead at the . . . [b]oard meeting with respect to the discussion of Robbins’ contact with the [Department of Labor]” and “created an environment that was hostile to her,” which “caused the trustees to vote to place her on leave.” The court noted that the two “‘set in motion’ the decision by the Joint Board to put Robbins on leave [.]”
As for Rice’s firing, the court explained how Brain and Cook retaliated against Rice by pressuring his employer, Zenith, into firing Rice and manipulating the Zenith relationship to deter Zenith from rehiring Rice in retaliation for his involvement in efforts to make an internal complaint about Brain.
Based upon evidence introduced during a five-day trial, the District Court ruled that Brain, Cook and Cook’s law firm violated ERISA section 510 by suspending and then discharging Robbins, and causing Zenith to refuse to hire Robbins and to discharge Rice in retaliation for their participation in reporting Brian’s misconduct to the General President of the Operative Plasterers’ and Cement Masons’ International Association and because Robbins participated in a federal criminal investigation of Brain. Specifically, the District Court ruled:
- Brain, Cook and Cook’s law firm wrongfully retaliated against Robbins in violation of ERISA 510 for her communications with the DOL by placing her on administrative leave; causing the work performed by the department that Robbins previously managed to be outsourced to Zenith and by causing Zenith not to hire Robbins to participate in its work;
- Brain, Cook and Cook’s law firm wrongfully retaliated against Rice in violation of ERISA 510 by causing Zenith to terminate Cook;
- Brain breached his fiduciary duty under ERISA 404 by retaliating against Robbins and causing her to be placed on administrative leave and that Cook knowingly participated in that breach.
The court held that Brain and Cook’s retaliatory conduct violated section 510 of ERISA, which prohibits retaliation against whistleblowers for complaining of ERISA violations or cooperating with a governmental investigation of such violations. The court also held that the couple’s retaliation against Robbins breached Brain’s fiduciary duties under ERISA section 404 to the trust funds and that Cook participated knowingly in that breach.
In reaching its decision, the court rejected attorney Cook’s argument that she was somehow immunized from her unlawful conduct because she was an attorney to the trust funds. Among other things, the court noted the “apparent conflict of interest” Cook had in representing the trust funds while being in an undisclosed “romantic relationship” with Brain, which existed as defendants carried out their retaliatory scheme. Reminding lawyers of their ethical duties in California, the court cited California Rule of Professional Conduct 3-310(B), which the court explained “requires that an attorney disclose to a client any personal relationship or interest that he or she knows, or with the exercise of reasonable diligence should know, could substantially affect her his or her professional judgment in advising the client.”
As punishing for these criminal violations of ERISA, the District Court ordered the permanent removal of Brain as a trustee. It also ordered the permanent barring of Brain, Cook and her law firm from serving the Cement Masons Southern California Trust Funds. In addition, the court ordered Cook and her law firm to repay all attorneys’ fees she billed the trust funds for the actions she took in retaliating against whistleblowers Robbins and Rice. These criminal sanctions were in addition to the $630,000 civil damage award that the Labor Department previously secured in lost wages and damages for Robbins, Rice and another worker victimized by Brain and Cook in August 2015.
In addition to its successful prosecution of Brain, Cook and Cook’s law firm on these charges, the DOL also had sought, but failed to convince the District Court based on the evidence presented at trial to find Brain, Cook, Cook’s law firm and Brain’s fellow trust fund trustee Local 600 business agent and Joint Board of Trustees member Jaime Briceno guilty of wrongful retaliation against another alleged whistleblower or Briceno of breaching his fiduciary duties under ERISA by failing to prudently investigate Robbins’ allegations against Brain; or by voting to use assets of the Trust Funds to pay the cost of the settlement of the civil action brought by Robbins. The District Court also refused to consider a newly raised charge that Brain breached his fiduciary duty by failing to collect all monies owed to the Trust Funds on the grounds that the Labor Department had failed to timely raise the charge. While the court refused to convict Briceno, Brain, Cook or Cook’s law firm on the additional charges, the Labor Department’s prosecution of these claims illustrates that along with abstaining from retaliating against ERISA whistleblowers, employee benefit plan fiduciaries also should position themselves to defend against potential breach of fiduciary duty claims based on alleged inadequacies in their investigation or response to reports or other evidence of misconduct involving the plan by prudently investigating and acting to redress allegations or other evidence of potential wrongdoing in the administration of employee benefit plans or their assets.
About The Author
A Fellow in the American College of Employee Benefit Counsel, the American Bar Foundation and the Texas Bar Foundation, Board Certified in Labor & Employment Law by the Texas Board of Legal Specialization, the author of this update, attorney Cynthia Marcotte Stamer, is AV-Preeminent (the highest) rated attorney repeatedly recognized as a Martindale-Hubble as a “LEGAL LEADER™” and “Texas Top Rated Lawyer” in Health Care Law, Labor and Employment Law, and Business & Commercial Law and among the “Best Lawyers In Dallas” in ERISA, Labor and Employment and Healthcare Law by D Magazine for her nearly 30 years of experience and knowledge representing and advising employers, employee benefit plans, their sponsors, fiduciaries, service providers and vendors and others on these and other planning, business transaction and contracting, administration, compliance, risk management, audits, investigations, government and private litigation and other enforcement and other related matters.
past Chair and current committee Co-Chair of the American Bar Association (ABA) RPTE Section Employee Benefits Group, Vice Chair of the ABA Tort & Insurance Practice Section Employee Benefits Committee, former Chair of the ABA Health Law Section Managed Care & Insurance Interest Group, a former ABA Joint Committee on Employee Benefits Council Representative ,
Ms. Stamer’s legal and management consulting work throughout her nearly 30-year career has focused on helping management manage. Highly valued for her rare ability to find pragmatic client-centric solutions by combining her detailed legal and operational knowledge and experience with her talent for creative problem-solving, she de[;pus jer her extensive legal and operational knowledge and experience to help organizations and their management use the law and process to manage people, process, compliance, operations and risk.
As a key part of this work, Ms. Stamer helps public and private, domestic and international businesses, governments, and other organizations and their leaders manage their employees, vendors and suppliers, and other workforce members, customers and other’ performance, compliance, compensation and benefits, operations, risks and liabilities, as well as to prevent, stabilize and cleanup workforce and other legal and operational crises large and small that arise in the course of operations.
Ms. Stamer works with businesses and their management, employee benefit plans, governments and other organizations deal with all aspects of human resources and workforce, internal controls and regulatory compliance, change management and other performance and operations management and compliance. She supports her clients both on a real time, “on demand” basis and with longer term basis to deal with daily performance management and operations, emerging crises, strategic planning, process improvement and change management, investigations, defending litigation, audits, investigations or other enforcement challenges, government affairs and public policy.
Well known for her extensive work with health care, insurance and other highly regulated entities on corporate compliance, internal controls and risk management, her clients range from highly regulated entities like employers, contractors and their employee benefit plans, their sponsors, management, administrators, insurers, fiduciaries and advisors, technology and data service providers, health care, managed care and insurance, financial services, government contractors and government entities, as well as retail, manufacturing, construction, consulting and a host of other domestic and international businesses of all types and sizes. Common engagements include internal and external workforce hiring, management, training, performance management, compliance and administration, discipline and termination, and other aspects of workforce management including employment and outsourced services contracting and enforcement, sentencing guidelines and other compliance plan, policy and program development, administration, and defense, performance management, wage and hour and other compensation and benefits, reengineering and other change management, internal controls, compliance and risk management, communications and training, worker classification, tax and payroll, investigations, crisis preparedness and response, government relations, safety, government contracting and audits, litigation and other enforcement, and other concerns.
Ms. Stamer uses her deep and highly specialized health, insurance, labor and employment and other knowledge and experience to help employers and other employee benefit plan sponsors; health, pension and other employee benefit plans, their fiduciaries, administrators and service providers, insurers, and others design legally compliant, effective compensation, health and other welfare benefit and insurance, severance, pension and deferred compensation, private exchanges, cafeteria plan and other employee benefit, fringe benefit, salary and hourly compensation, bonus and other incentive compensation and related programs, products and arrangements. She is particularly recognized for her leading edge work, thought leadership and knowledgeable advice and representation on the design, documentation, administration, regulation and defense of a diverse range of self-insured and insured health and welfare benefit plans including private exchange and other health benefit choices, health care reimbursement and other “defined contribution” limited benefit, 24-hour and other occupational and non-occupational injury and accident, expat and medical tourism, onsite medical, wellness and other medical plans and insurance benefit programs as well as a diverse range of other qualified and nonqualified retirement and deferred compensation, severance and other employee benefits and compensation, insurance and savings plans, programs, products, services and activities. As a key element of this work, Ms. Stamer works closely with employer and other plan sponsors, insurance and financial services companies, plan fiduciaries, administrators, and vendors and others to design, administer and defend effective legally defensible employee benefits and compensation practices, programs, products and technology. She also continuously helps employers, insurers, administrative and other service providers, their officers, directors and others to manage fiduciary and other risks of sponsorship or involvement with these and other benefit and compensation arrangements and to defend and mitigate liability and other risks from benefit and liability claims including fiduciary, benefit and other claims, audits, and litigation brought by the Labor Department, IRS, HHS, participants and beneficiaries, service providers, and others. She also assists debtors, creditors, bankruptcy trustees and others assess, manage and resolve labor and employment, employee benefits and insurance, payroll and other compensation related concerns arising from reductions in force or other terminations, mergers, acquisitions, bankruptcies and other business transactions including extensive experience with multiple, high-profile large scale bankruptcies resulting in ERISA, tax, corporate and securities and other litigation or enforcement actions.
A former lead consultant to the Government of Bolivia on its Social Security reform law Ms. Stamer also is well-known for her leadership on U.S. health and pension, wage and hour, tax, workforce, tax, education, insurance and other policies critical to the workforce, benefits, and compensation practices and other key aspects of a broad range of businesses and their operations. She both helps her clients respond to and resolve emerging regulations and laws, government investigations and enforcement actions and helps them shape the rules through dealings with Congress and other legislatures, regulators and government officials domestically and internationally. Ms. Stamer works with U.S. and foreign businesses, governments, trade associations, and others on workforce, social security and severance, health care, immigration, privacy and data security, tax, ethics and other laws and regulations. Founder and Executive Director of the Coalition for Responsible Healthcare Policy and its PROJECT COPE: the Coalition on Patient Empowerment and a Fellow in the American Bar Foundation and State Bar of Texas, Ms. Stamer for many years acted as the scribe responsible for leading the Joint Committee on Employee Benefits (JCEB) HHS Office of Civil Rights annual agency meeting and regularly participates in the OCR and other JCEB annual agency meetings, and participates in the development and submission of comments and other input to the agencies on regulatory, enforcement and other concerns. She also works as a policy advisor and advocate to many business, professional and civic organizations.
Author of the thousands of publications and workshops these and other employment, employee benefits, health care, insurance, workforce and other management matters, Ms. Stamer also is a highly sought out speaker and industry thought leader known for empowering audiences and readers. Ms. Stamer’s insights on employee benefits, insurance, health care and workforce matters in Atlantic Information Services, The Bureau of National Affairs (BNA), InsuranceThoughtLeaders.com, Benefits Magazine, Employee Benefit News, Texas CEO Magazine, HealthLeaders, Modern Healthcare, Business Insurance, Employee Benefits News, World At Work, Benefits Magazine, the Wall Street Journal, the Dallas Morning News, the Dallas Business Journal, the Houston Business Journal, and many other publications. She also has served as an Editorial Advisory Board Member for human resources, employee benefit and other management focused publications of BNA, HR.com, Employee Benefit News, InsuranceThoughtLeadership.com and many other prominent publications. Ms. Stamer also regularly serves on the faculty and planning committees for symposia of LexisNexis, the American Bar Association, ALIABA, the Society of Employee Benefits Administrators, the American Law Institute, ISSA, HIMMs, and many other prominent educational and training organizations and conducts training and speaks on these and other management, compliance and public policy concerns.
Ms. Stamer also is active in the leadership of a broad range of other professional and civic organizations. For instance, Ms. Stamer serves on the Advisory Boards of InsuranceThoughtLeadership.com, HR.com, Employee Benefit News, and as an editorial advisor and contributing author of many other publications. Her leadership involvements with the American Bar Association (ABA) include year’s serving many years as a Joint Committee on Employee Benefits Council representative; ABA RPTE Section current Practice Management Vice Chair and Substantive Groups & Committees Committee Member, RPTE Employee Benefits & Other Compensation Committee Past Group Chair and Diversity Award Recipient, current Defined Contribution Plans Committee Co-Chair, and past Welfare Benefit Plans Committee Chair Co-Chair; Past Chair of the ABA Health Law Section Managed Care & Insurance Interest Group and a current member of its Healthcare Coordinating Council; current Vice Chair of the ABA TIPS Employee Benefit Committee; International Section Life Sciences Committee Policy Vice Chair; and a speaker, contributing author, comment chair and contributor to numerous Labor, Tax, RPTE, Health Law, TIPS, International and other Section publications, programs and task forces. Other selected service involvements of note include Vice President of the North Texas Healthcare Compliance Professionals Association; past EO Coordinator and a Vice-Chair of the Gulf Coast TEGE Council TE Division; founding Board Member and President of the Alliance for Healthcare Excellence, as a Board Member and Board Compliance Committee Chair for the National Kidney Foundation of North Texas; the Board President of the early childhood development intervention agency, The Richardson Development Center for Children; Chair of the Dallas Bar Association Employee Benefits & Executive Compensation Committee; a former Southwest Benefits Association Board of Directors member, Continuing Education Chair and Treasurer; former Texas Association of Business BACPAC Committee Member, Executive Committee member, Regional Chair and Dallas Chapter Chair; former Society of Human Resources Region 4 Chair and Consultants Forum Board Member and Dallas HR Public Policy Committee Chair; former National Board Member and Dallas Chapter President of Web Network of Benefit Professionals; former Dallas Business League President and others. For additional information about Ms. Stamer, see CynthiaStamer.com or contact Ms. Stamer via email here or via telephone to (469) 767-8872.
About Solutions Law Press, Inc.™
If you found these updates of interest, you may be interested in other recent Solutions Law Press, Inc. updates like the following:
Go here to register to receive other Solutions Law Press, Inc. updates and announcements about other upcoming briefings, training or other programs, products, services, and activities or to learn more about Solutions Law Press, Inc., its publications, programs and training, PROJECT COPE: Coalition on Patient Empowerment community service and education projects, event management and other resources and services.
For important information concerning this communication see here. THE FOLLOWING DISCLAIMER IS INCLUDED TO COMPLY WITH AND IN RESPONSE TO U.S. TREASURY DEPARTMENT CIRCULAR 230 REGULATIONS. ANY STATEMENTS CONTAINED HEREIN ARE NOT INTENDED OR WRITTEN BY THE WRITER TO BE USED, AND NOTHING CONTAINED HEREIN CAN BE USED BY YOU OR ANY OTHER PERSON, FOR THE PURPOSE OF (1) AVOIDING PENALTIES THAT MAY BE IMPOSED UNDER FEDERAL TAX LAW, OR (2) PROMOTING, MARKETING OR RECOMMENDING TO ANOTHER PARTY ANY TAX-RELATED TRANSACTION OR MATTER ADDRESSED HEREIN.
©2016 Cynthia Marcotte Stamer, P.C. Non-exclusive license to republish granted to Solutions Law Press, Inc. All other rights reserved.
 Comments Off on Criminal Conviction Of Plan Trustee, Outside Legal Counsel Shows Risks of Retaliating Against Whistleblowers For Reporting ERISA Violations |
Comments Off on Criminal Conviction Of Plan Trustee, Outside Legal Counsel Shows Risks of Retaliating Against Whistleblowers For Reporting ERISA Violations |  401(k), Appeals, Attorney-Client Privilege, Banking, Bankruptcy, board of directors, Brokers, Claims Administration, compensation, compliance, Corporate Compliance, corporate governance, Cybercrime, defined benefit plan, defined contribution plan, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Malpractice, Reporting & Disclosure, Uncategorized | Tagged: defined contribution plan, EBSA, employee benefit plans, Employer, ERISA, ERISA 404, ERISA 510, Fiduciary responsiility, Health Plan, Health Plans, Multiemployer collectively bargained employee benefit plans, Retailiation, Retirement Plans, Union, Whistleblower |
401(k), Appeals, Attorney-Client Privilege, Banking, Bankruptcy, board of directors, Brokers, Claims Administration, compensation, compliance, Corporate Compliance, corporate governance, Cybercrime, defined benefit plan, defined contribution plan, Disability Plans, EBSA, employee, Employee Benefits, Employer, Employers, ERISA, fiduciary duty, Fiduciary Responsibility, health benefit, Health Benefits, health insurance, health plan, Health Plans, HR, Human Resources, Insurance, insurers, Internal Controls, Internal Investigations, Labor Management Relations, Malpractice, Reporting & Disclosure, Uncategorized | Tagged: defined contribution plan, EBSA, employee benefit plans, Employer, ERISA, ERISA 404, ERISA 510, Fiduciary responsiility, Health Plan, Health Plans, Multiemployer collectively bargained employee benefit plans, Retailiation, Retirement Plans, Union, Whistleblower |  Permalink
Permalink
 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer



 Posted by Cynthia Marcotte Stamer
Posted by Cynthia Marcotte Stamer 
 Teamwork is a valuable and necessary to organizational performance in most workplaces. However management undermines team performance and effectiveness by giving participation trophies to team members that don’t give their best when working on teams.
Teamwork is a valuable and necessary to organizational performance in most workplaces. However management undermines team performance and effectiveness by giving participation trophies to team members that don’t give their best when working on teams.

You must be logged in to post a comment.